It’s a common misconception that severe psoriasis is only a physical ailment, but the reality is far more nuanced. Both pustular and erythrodermic psoriasis can significantly impact everyday functioning, emotional health, and overall quality of life.
These illnesses can have significant impact on mental health since they frequently cause discomfort, observable symptoms, and erratic flare-ups. However, people often neglect the emotional aspects of having these diseases.
In this article, we will explore the mental health challenges due to erythrodermic psoriasis and the emotional impact of pustular psoriasis, understand the psychological effects of severe psoriasis, and discuss practical ways to cope, seek support, and improve overall well-being.
- Severe psoriasis affects both skin and mental health, often causing anxiety, depression, and social isolation.
- Erythrodermic and pustular psoriasis bring added stress due to severity, unpredictability, and frequent flare-ups.
- Lifestyle habits, emotional support, and multidisciplinary care play a key role in improving overall well-being.
Read More: When Should You Change Your Psoriasis Treatment? Signs It’s Not Working Anymore
Why Severe Psoriasis Can Affect Mental Health
Psoriasis is not just a skin ailment. In addition to the dryness, cracking, and itching, millions of people experience emotional distress. The psychological and emotional effects of psoriasis are still poorly understood, even though research is continually revealing new information about its biological underpinnings.
Psoriasis can affect nearly every aspect of a person’s life—from the quiet fatigue caused by disrupted sleep to the emotional strain and social stigma that it can bring. Common companions include anxiety, depression, and feelings of loneliness, which are frequently made worse by delayed diagnosis, misunderstanding, or a lack of any emotional support in healthcare settings.
Psoriasis impacts not only the skin but also relationships, mental health, and self-worth in ways that are frequently undetectable to others. It is also difficult to treat and prone to relapse.
Social Isolation: It can be difficult to conceal psoriasis lesions, which can result in awkward looks, unsolicited advice, and even prejudice.
Anxiety and Depression: Research indicates that people with psoriasis have a markedly higher risk of experiencing anxiety and depression. The chronic nature of the illness causes psychological strain, the unpredictability of flare-ups, and the emotional burden of managing a misdiagnosed ailment.
Sleep Disturbance and General Health: Itching, pain, and discomfort associated with psoriasis frequently disrupt sleep, increasing stress, diminishing coping skills, and weakening the immune system.
Unique Challenges With Erythrodermic Psoriasis
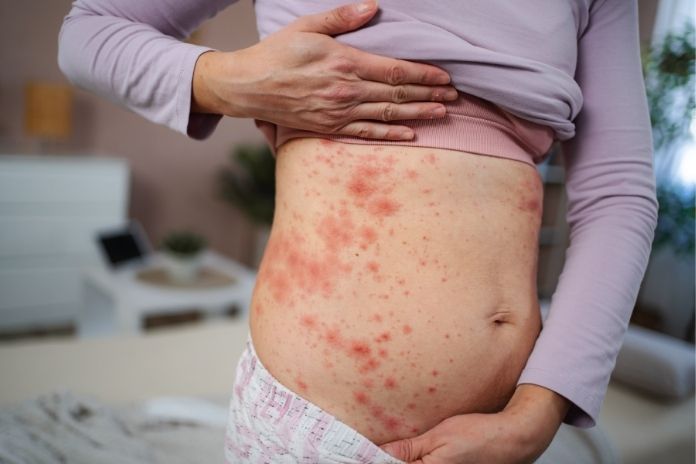
With a prevalence of 1-2.25% among psoriatic patients, erythrodermic psoriasis (EP) is an uncommon and severe variant of psoriasis vulgaris. Significant erythema covers at least 80–90% of the body’s surface, and the condition often causes fever, chills, headaches, and overall discomfort.
Because of the severe inflammation, EP can resemble a burn, and the accompanying systemic symptoms can make it difficult to distinguish it from other serious skin disorders.
During severe flare-ups, patients with erythrodermic psoriasis may need hospital admission. It might result in medical trauma or anxiety related to healthcare settings, which can exacerbate chronic stress and anxiety. Frequent hospital stays can also cause emotional strain by interfering with personal and professional life.
Patients’ quality of life is affected by psoriasis. Sleep difficulties are prevalent among patients with psoriasis, yet most quality-of-life measures do not explicitly assess them. Because sleep disorders affect patients’ physical and mental health; clinicians must evaluate them using specialized scores.
Emotional Impact of Pustular Psoriasis
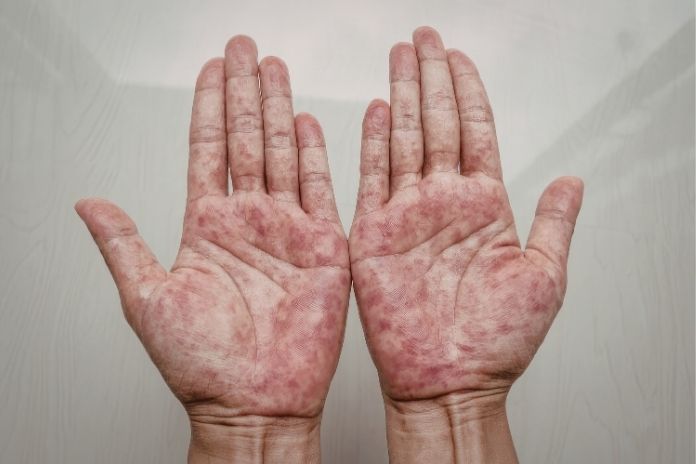
Sterile pustules are the hallmark of a rare, persistent, and potentially fatal neutrophilic skin condition called generalized pustular psoriasis (GPP). GPP and plaque psoriasis can coexist, with or without systemic inflammation, despite their differences. Sterile pustules develop more widely with the episodic deterioration (flares) that characterize the clinical course of GPP. Individual differences in flare intensity exist.
Pustular psoriasis can flare up quickly and severely, unlike some other types. Patients may continuously worry about the next episode as a result of this unpredictability, which exacerbates chronic anxiety.
Relationships and financial stability may be affected by frequent flare-ups that disrupt social obligations and work schedules. This instability contributes to the broader mental health impact of pustular psoriasis.
It’s crucial to remember that experiences differ greatly; some people manage well, while others might have more severe difficulties.
Read More: Top 8 Psoriasis Creams: Soothing Skincare Solutions for Flare-Ups
Common Mental Health Effects Reported by Patients
People living with severe psoriasis frequently experience a variety of emotional difficulties, such as:
- Persistent anxiety about the unpredictability of flare-ups
- Depression symptoms include despondency and low mood
- Psoriasis and social isolation brought on by shame or stigma
- Ongoing body image distress
- Emotional tiredness brought on by fatigue
The Role of Inflammation in Mood Changes
It’s very crucial to realize that, despite its negative connotations, inflammation is a normal and necessary process that the immune system employs to combat infection and heal tissue. However, inflammation can have negative effects on the body and the brain if it persists at low levels over time and becomes chronic.
When it comes to the likelihood of your mental health problems, this persistent, low-level inflammation is the most worrisome kind.
Elevated inflammatory markers were associated with an increased risk of any diagnosed psychiatric disease, according to a compelling 2024 analysis of nearly 585,000 individuals published in JAMA Psychiatry. Psoriasis-related cytokines may potentially affect brain chemistry and exacerbate sadness and anxiety.
Signs the Emotional Impact May Need Attention

Early warning indicators can help stop mental health problems from getting worse. Be mindful of:
Persistent Low Mood: Depression may be indicated by persistently feeling depressed or hopeless.
Loss of Interest in Activities: One of the most typical indicators of emotional pain is a lack of enjoyment in once-loved activities.
Avoidance of Social Situations: Psoriasis and social isolation may be indicated by avoiding social situations out of embarrassment or anxiety.
Sleep Disturbances: Difficulty falling to sleep or frequent waking may exacerbate emotional and physical issues.
Increased Stress During Flares: Exacerbated emotional responses during flares may indicate you need more support.
Read More: Top 7 Psoriasis Shampoos: Gentle Hair Care Products for Scalp Relief
Practical Strategies to Support Mental Well-Being
It matters how you are feeling. Do not be afraid to ask for assistance and support if you feel that you are not handling things as well as you should. Untreated emotional and mental health problems can impact your physical health and almost every other part of your life.
Engage in Physical Activity Three to Five Days a Week: Discuss the appropriate type of exercise with your physician. Exercise releases endorphins, which are feel-good hormones.
Consume a Diet High in Plant-Based Foods, Particularly Fruits and Green Vegetables: Cook with spices like rosemary, turmeric, and ginger. Drink lots of water and consider drinking black or green tea.
Get Seven to Nine Hours of Good Sleep Every Night: To help your body and mind heal and get ready for the next day. When you wake up, consider three things you are thankful for from the day before.
Practice 4-7-8 Breathing: Breathe in for a count of four, hold it for a count of seven, and then exhale for a count of eight. Do this at least four times a day for four breaths. Deep breathing techniques can improve mood, lessen anxiety, and increase focus.
Spend At Least Fifteen Minutes Each Day Outside: Sunlight and fresh air can lift the spirits and strengthen your defenses.
The Importance of Multidisciplinary Care

Dermatological treatment alone is not enough to manage severe psoriasis. A multidisciplinary approach can meet both physical and emotional demands.
Dermatologists, primary care physicians, and mental health professionals can work together to manage chronic skin disease and mental health challenges.
Cognitive-behavioral therapy is a type of therapy that can help patients reframe negative beliefs and develop more constructive coping mechanisms.
Support groups, both online and in-person, offer connection and reduce feelings of isolation, improving the quality of life of people with erythrodermic psoriasis.
Communicating About Mental Health With Your Care Team
Open communication is very crucial, yet many patients are reluctant to talk to their doctors about emotional issues. Think about asking:
- What possible effects might my treatment have on my mood?
- Are there resources available for mental health?
- Should I consult a counselor or therapist?
It’s crucial to talk about the adverse effects of medications because some of them can affect mood.
Read More: Manage Psoriasis With Essential Oils
Social and Practical Coping Approaches
Planning comfortable attire or adjusting schedules in advance of flare days can decrease stress.
Workplace communication, such as informing employers about the disease, can create a supportive environment.
Gradual exposure and confidence-building in secure environments are key components of managing social anxiety. Coping with visible skin disorders can be aided by both online and in-person support groups.
When to Seek Professional Mental Health Support

It might be time to get assistance if:
- Symptoms hamper daily living
- Depression or anxiety becomes chronic
- Treatment becomes too much to handle
- Feelings of loneliness get stronger
Seeking assistance is crucial to managing the psychological effects of pustular psoriasis and other severe types; it is not a sign of weakness.
Read More: Top 5 Foods to Cure Psoriasis
Conclusion
Living with severe psoriasis has a significant impact on one’s emotional and physical well-being. The severe psoriasis psychological effects can include stress, low mood, and difficulty coping with your daily life, especially during unpredictable flare-ups. Recognizing the mental health impact of pustular psoriasis and other severe forms is an essential step toward better overall care.
People can enhance their quality of life with the right support system, including mental health services, lifestyle modifications, and medical care.
References
- Forefront Dermatology. (2025, November 10). The hidden burden: Psoriasis and mental health.
- Vaidya, K., Mukan, K., Sharpe, L., Whittam, L., & Jacobs, C. (December 04, 2024). A rare presentation of erythrodermic psoriasis.
- National Institute of Mental Health. (2024, December). Caring for your mental health.
- National Health Service (NHS). (2022, December 16). Five steps to mental wellbeing.
- Johns Hopkins Health Plans. (2025, September 3). Five tips to improve mental well-being.
In this Article