Days or weeks after recovering from a sore throat, some people experience an unexpected skin eruption. This “random” outbreak may initially appear to be a benign post-infectious rash. Still, in many young adults, it is actually guttate psoriasis associated with a recent case of strep throat.
In this article, we’ll explore the guttate psoriasis after strep throat connection, why it happens, how to recognize guttate psoriasis symptoms, what triggers flare-ups, how long it lasts, and the most effective guttate psoriasis treatment options available today.
- Post-strep trigger: Guttate psoriasis often appears 1–3 weeks after a strep throat infection due to immune system overreaction.
- Distinct appearance: Look for small, drop-shaped red spots that spread across the body, especially the torso and limbs.
- Good outlook: Most cases clear within 3–4 months, but early treatment can ease symptoms and prevent recurrence.
Read More: Can a Newborn Get Strep Throat? Symptoms, Risks, and What Parents Should Know
What Is Guttate Psoriasis?
Psoriasis is a long-term inflammatory skin disease that causes skin discoloration and an uneven texture. Guttate psoriasis is a type of psoriasis characterized by tiny, teardrop-shaped red spots that appear on the skin and are distributed over almost the entire body.
This type of psoriasis typically arises suddenly after a person gets strep throat brought on by Group A Streptococcus or another infection or after taking specific drugs.
Although it can occur in adults, guttate psoriasis is most common in childhood. Papules are tiny, raised patches on the skin that may have a scale covering their surface.
Skin inflammation causes these papules to develop anywhere on the body, including the arms, legs, torso, face, ears, and scalp. Guttate psoriasis does not have stages, unlike other types of psoriasis, because it usually manifests without warning.
Why Strep Throat Can Trigger a Skin Rash
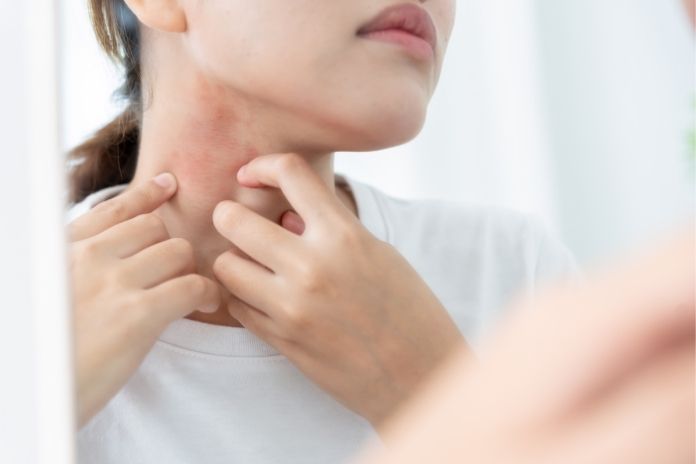
In dermatology, there is ample evidence of a strep throat-psoriasis connection. But not all strep patients go on to acquire psoriasis. Several underlying mechanisms explain why some individuals experience a sudden psoriasis outbreak after infection.
Immune System Cross-Reactivity: When the body fights strep throat, the immune system produces antibodies to combat the infection. In some cases, cross-reactivity occurs, where these immune responses mistakenly target healthy skin cells. This leads to skin inflammation and the development of characteristic drop-like lesions.
Genetic Susceptibility: Post-streptococcal psoriasis is more common in people with a family history of psoriasis. After infection, several genes increase the immune system’s reactivity, which increases the risk of guttate psoriasis triggers.
Inflammatory Reaction Following Infection: Internal inflammation may persist even after throat symptoms resolve. This lingering immune activation can trigger small red spots of psoriasis several days or weeks later.
When the Rash Typically Appears After Strep
Timing is a key clue for identifying a rash after strep throat in young adults.
- The rash usually appears 1–3 weeks after infection.
- It could begin abruptly or spread gradually.
- After their sore throat has already healed, many people become aware of it.
Many people do not initially associate their symptoms with post-streptococcal psoriasis because of this delayed reaction.
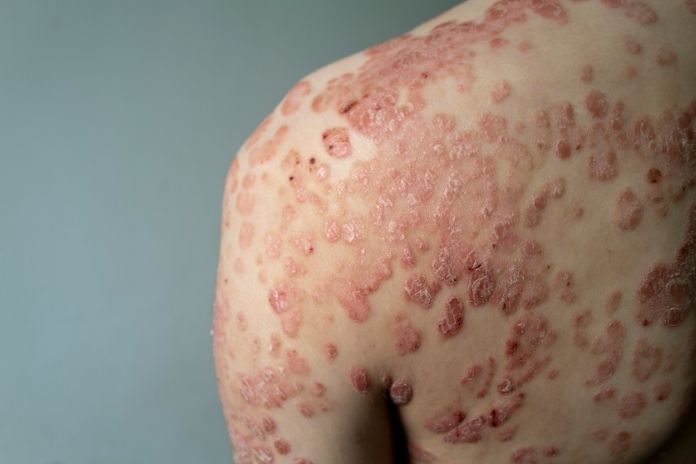
What Guttate Psoriasis Looks Like
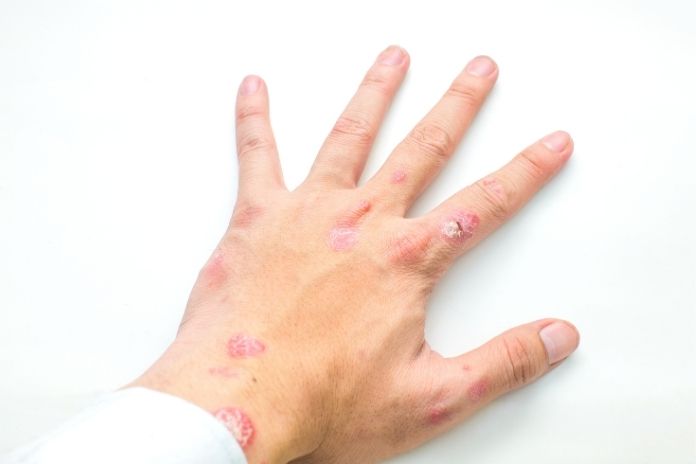
Recognizing guttate psoriasis symptoms can help distinguish it from other skin conditions.
- Two to three weeks after tonsillitis or a streptococcal throat infection, small salmon-pink (or red) papules typically appear suddenly on the skin.
- These drop-like lesions may be itchy.
- The eruption usually begins on the arms, legs, or torso and may spread to the scalp, ears, or face. The palms and soles are typically spared.
- Nail changes, such as pitting or ridging, which are common in chronic psoriasis, are often absent.
Remember that the intensity of guttate psoriasis symptoms varies. While some cases involve massive eruptions, others are more subtle.
Read More: How to Get Rid of Strep Throat Infection
How It Differs From Other Post-Strep Rashes
Not all infection-related rashes are guttate psoriasis after strep throat. Other options consist of:
- Drug responses (such as those caused by strep throat medications)
- Exanthems from viruses
- Allergic rashes
In contrast to these ailments, post-streptococcal psoriasis:
- Shows drop-like lesions
- Persists longer than typical allergic reactions
- May recur with future infections
Who Is Most Likely to Develop Guttate Psoriasis
Certain individuals are more prone to guttate psoriasis triggers:
- Young adults, children, and teens, particularly those under 30.
- People who have a family history of psoriasis.
- Individuals who frequently contract streptococcal infections.
- People who are more sensitive to the immunological system.
Other Triggers Besides Strep Throat
Although guttate psoriasis after strep throat is common, other factors can also trigger outbreaks.
- Certain medications, namely beta blockers and antimalarials
- Infections, including upper respiratory tract infections, sinus infections, or the flu
- Streptococcal infection
- Tonsillitis, or tonsil irritation
- Damage to the skin
- Stress
Read More: Tightness in the Throat: Causes, What It Means & When to Get Help
How Long Does Guttate Psoriasis Usually Last
Guttate psoriasis often resolves spontaneously within three to four months, even without treatment. Patients with streptococcal-associated guttate psoriasis generally have a favorable prognosis. However, recurrence can occur with subsequent streptococcal infections.
Chronic plaque psoriasis can develop from guttate psoriasis if it persists. In a study including more than 190,000 patients with guttate psoriasis, 12.5% went on to develop chronic plaque psoriasis; half of these cases occurred within a year of the patients’ initial presentation with guttate psoriasis.
“For over two-thirds of patients, guttate psoriasis will resolve spontaneously within three to four months,” says Alexandra K. Golant, MD, FAAD, dermatologist and Medical Director, Faculty Practice, Mount Sinai Health System in New York.
Treatment Options Your Doctor May Consider

Guttate psoriasis treatment options are not universally applicable. Individual reaction and intensity determine management.
Topical Therapies: Topical treatments are the primary line of treatment for mild cases involving less than 10% of the body’s surface area. Studies have shown that corticosteroids significantly benefit the majority of patients, making them the most commonly prescribed option. Low-potency corticosteroid formulations are appropriate for facial involvement, while medium-potency formulations are effective for body lesions. Analogs of vitamin D, such as calcipotriol, provide an effective alternative to steroids.
Phototherapy: The best treatment for severe guttate psoriasis. Studies show that narrowband UVB (NB-UVB) significantly improves the condition of about 81% of patients.
Systemic Medication: Systemic intervention may be necessary in severe or resistant cases. Methotrexate successfully manages widespread illness, and research has shown a notable improvement. Combining methotrexate and phototherapy may reduce cumulative UV exposure and accelerate clearance.
Read More: Burning Sensation in Throat – 6 Possible Causes and 10 Remedies
Can Guttate Psoriasis Come Back?
The symptoms of psoriatic disease can go away and come back at any moment during a person’s lifetime. Although there is no known cure for psoriasis, current medications are more effective than ever, and research into both a cure and novel treatments is continuing.
Psoriasis comorbidities, including psoriatic arthritis, heart disease, and depression, may be prevented by treating psoriasis, which can also help alleviate symptoms.
When to Seek Medical Evaluation

Knowing when to seek professional medical attention guarantees the best results and avoids complications. A dermatologist should be consulted right away in certain scenarios, even if minor cases may resolve on their own. Get medical help if you encounter:
- Several tiny red dots suddenly appeared following a recent illness.
- Lesions that occupy more than 10% of your body.
- Severe discomfort or itching that interferes with everyday tasks.
- Areas of the face or genitalia that need extra attention.
- An increase in redness, warmth, and pus are indicators of a skin infection.
- Skin symptoms accompany joint swelling or discomfort.
Practical Tips While the Rash Is Healing
Supportive care can enhance comfort and recuperation throughout treatment.
- Use mild, fragrance-free skincare products.
- Steer clear of irritants and strong soaps.
- Maintain hydrated skin.
- Reduce flare causes by managing your stress.
- Keep an eye out for fresh triggers for guttate psoriasis.
Read More: 20 Home Remedies for Sore Throat That Work Miraculously
Conclusion
After a throat infection, an abrupt skin eruption might not be as coincidental as it first appears. The link between guttate psoriasis after strep throat and the body’s immune response highlights how infections can trigger visible skin changes, especially in younger individuals.
Guttate psoriasis symptoms can be frightening when they first arise, but with the right treatment and prompt assessment, the condition is frequently treatable. Identifying early warning indicators, understanding triggers, and obtaining the right treatment can greatly improve results.
References
- Gainesville Dermatology & Skin Surgery. Guttate psoriasis treatment.
- DermNet New Zealand. (2021, October). Guttate psoriasis.
- Achufusi, T. G. O., Pellegrini, M. V., & Patel, R. K. (July 31, 2023). Milk thistle.
- Centers for Disease Control and Prevention. (2025, August 7). Symptoms of scarlet fever.
- UF Health. Scarlet fever.
- Up to date. (November 21, 2025). Guttate psoriasis.
- National Psoriasis Foundation. (March 31, 2026). Guttate Psoriasis.
- Marc Lallanilla. (22 August, 2024). Guttate Psoriasis: Symptoms, Causes, Treatment, and More.
In this Article