Fiber is one of the few dietary recommendations that has survived virtually every nutritional trend of the past 50 years. Studies supporting its benefits for bowel health, cardiovascular disease, blood sugar regulation, and gut microbiome diversity are numerous and consistent. General practitioners recommend it.
Gastroenterologists and dietitians recommend it. Add more fiber, they all say, and your digestion will improve. Then a significant number of people do exactly that and feel worse.
More bloating, more gas, harder stools, or the uncomfortable feeling that everything has come to a standstill. The advice was correct in principle. Something went wrong in practice. This is what gastroenterologists call the fiber paradox. It is not a contradiction in the research.
There is a gap between the population-level evidence on fiber and constipation and the individual-level reality of how different digestive systems respond to the same dietary change. Understanding what sits inside that gap is what makes the difference between a fiber increase that helps and one that backfires.
Read More: How to Boost Daily Fiber Intake without Feeling Full or Bloated All Day
- Fiber can help with constipation, but adding it incorrectly can actually make symptoms worse.
- The issue often comes from increasing fiber too quickly, not drinking enough water, or choosing the wrong type of fiber.
- Not all fiber works the same; some types can slow things down depending on your gut.
- Fixing this usually means adjusting intake and hydration, not cutting fiber out completely.
Why Fiber Is Usually Recommended for Digestive Health
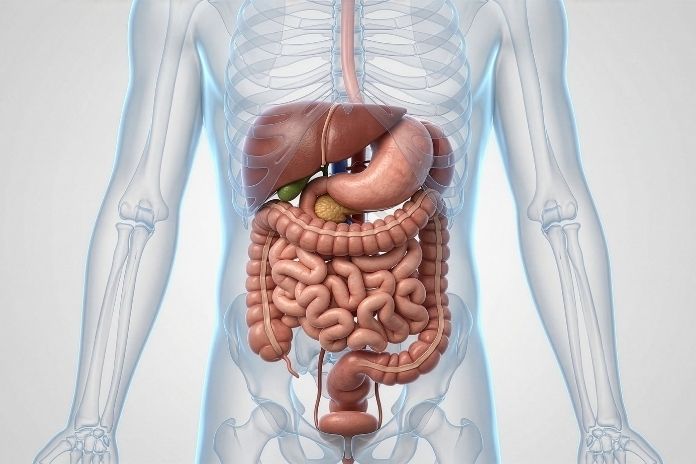
Dietary fiber works on the digestive system through several mechanisms simultaneously. Soluble fiber dissolves in water and forms a gel-like substance in the intestine, softening stool and slowing digestion enough to allow proper water absorption.
Insoluble fiber does not dissolve and adds physical bulk to stool, which stimulates the muscular contractions of the intestinal wall, known as peristalsis, that keep waste moving through the colon toward elimination. Beyond these mechanical functions, fiber also serves as a prebiotic substrate, feeding the beneficial bacteria that live in the large intestine.
These bacteria ferment soluble fiber and resistant starch into short-chain fatty acids, including butyrate, which nourishes the cells lining the colon, reduces inflammation, and supports healthy gut motility. A well-fed gut microbiome is, among other things, a gut that moves well.
A comprehensive PMC review of dietary fiber in irritable bowel syndrome confirmed that supplementation with long-chain, intermediate-viscosity soluble fiber, particularly psyllium, improves overall symptoms in IBS patients compared to placebo, with the strongest evidence for both stool consistency and frequency improvements.
The review also noted that the fiber type determines the outcome, not fiber intake as a category.
Recommended Daily Fiber Intake
Current guidelines from the Academy of Nutrition and Dietetics recommend 25 grams of fiber per day for women and 38 grams for men. Most American adults consume approximately 15 to 17 grams daily, a significant shortfall.
The gap is real and contributes to the high rates of high fiber constipation’s absence, meaning insufficient fiber is a genuine driver of constipation. The solution is more fiber. But the way that fiber is added matters as much as the amount.
The Two Main Types of Fiber and How They Work

Soluble fiber dissolves in water to form a viscous gel in the digestive tract. This gel slows the movement of food through the small intestine, allows more complete nutrient absorption, and reaches the large intestine, where bacteria ferment it into short-chain fatty acids.
It softens stool, which is beneficial for both constipation and diarrhea, depending on the baseline. Food sources include oats, psyllium husk, beans, lentils, apples, pears, flaxseed, and chia seeds.
Soluble fiber is generally better-tolerated by people with sensitive digestion because its fermentation produces less gas than highly fermentable fiber in the short-chain category. Psyllium, in particular, is notable for being soluble but only mildly fermentable, which means it provides bulking and softening benefits without the gas and bloating that more fermentable fibers produce.
Insoluble fiber does not dissolve and is not fermented by gut bacteria. It passes through the digestive system largely intact, adding physical bulk to stool and speeding up digestive transit time by stimulating the intestinal wall. Food sources include wheat bran, whole grain bread and cereals, the skins of fruits and vegetables, and many raw vegetables.
Insoluble fiber is effective at preventing constipation in people with normal gut function and adequate hydration. But it has a specific limitation: it speeds things up mechanically, which requires the gut’s muscular contractions to be functioning well in the first place.
In people with slow gut motility or already-hard stool from dehydration, adding large quantities of insoluble fiber can worsen the backup rather than relieve it. This is one of the primary mechanisms behind why fiber causes constipation in some people.
Most whole foods contain a mix of both fiber types, and the ratio varies by food. This natural blending generally produces better outcomes than supplementing heavily with a single isolated fiber type. Problems arise when someone dramatically increases their intake of a single high-fiber food, particularly a highly insoluble fiber source like wheat bran, without balancing it with soluble fiber sources and adequate hydration.
The Fiber Paradox: Why More Fiber Can Lead to Constipation
The gut microbiome adapts to dietary patterns over time, and the bacteria responsible for fermenting fiber need time to expand their populations when fiber intake increases. When fiber is added rapidly, the existing microbial community is overwhelmed.
The result is often gas, bloating, and paradoxically, slowed transit time as the digestive system struggles to process an unfamiliar substrate load.
Dr. Will Bulsiewicz, MD, MSCI, identified this paradox directly in clinical practice: “Fiber is the nutrient that heals the gut microbiome. But the people who need fiber the most are also the ones who struggle the most when incorporating fiber, because their gut is in a damaged state. We lack the enzymes as humans to process fiber, which means that we are 100% reliant on microbes to do it for us.”
“If you take a person who has a damaged gut microbiome, their capacity to process and digest fiber may be impaired,” he told Forks Over Knives. His solution is not to avoid fiber but to increase it gradually so the microbiome can adapt.
This is the most common and most preventable cause of high fiber constipation. Both soluble and insoluble fiber require water to function correctly. Soluble fiber needs to absorb water to form its gel.
Insoluble fiber needs water in the colon to allow stool to remain soft enough to move through comfortably. When fiber intake increases without a corresponding increase in fluid intake, fiber draws water out of intestinal contents rather than adding it, producing harder, drier stool that is more difficult to pass.
A PMC review of hydration and bowel function confirmed that adequate fluid intake, particularly water, is a prerequisite for fiber to produce its expected laxative effect. The review noted that increased fiber intake without fluid increases was consistently associated with paradoxical constipation rather than relief. The general guidance is to increase fluid intake by at least 500ml per day for every significant increase in dietary fiber.
Gut motility, the speed at which muscular contractions move food and waste through the digestive tract, varies significantly between individuals. People with slow transit constipation, in which waste moves through the colon more slowly than normal, may find that adding more insoluble fiber worsens symptoms by adding bulk to a system that cannot move it efficiently.
A PubMed study examining fiber response in constipation subtypes found that the response to dietary fiber is highly dependent on the underlying mechanism of constipation. Patients with slow transit constipation showed significantly less improvement with fiber supplementation than those with normal transit constipation, and some experienced worsening symptoms.
This finding underscores that eating more fiber but still being constipated is not a signal to add more. It is a signal to investigate the mechanism.
Gut Microbiome Differences
Individual variation in gut microbiome composition directly affects how fiber is processed. Some people have gut bacteria populations that ferment certain fermentable fiber types aggressively, producing excess gas as a byproduct, which causes bloating and abdominal discomfort that can slow stool movement through the discomfort response.
People who have recently taken antibiotics, been ill, or have a history of dietary restriction may have a less diverse microbiome that is less equipped to handle sudden increases in fiber diversity or quantity.
High-Fiber Foods Most Likely to Trigger Digestive Discomfort

Raw vegetables are significantly higher in insoluble fiber than cooked vegetables, because cooking softens cell walls and partially breaks down fiber structures, making them easier to process.
A large salad of raw kale, cabbage, broccoli, and cruciferous vegetables consumed by someone not accustomed to high fiber intake can produce gas, bloating, and slowed transit, particularly in people with sensitive digestion.
Wheat bran is among the most concentrated sources of insoluble fiber in the food supply. Products like bran cereals, bran muffins, and whole wheat bread with added bran can deliver large amounts of insoluble fiber in a single serving.
For people with adequate gut motility and good hydration, this is beneficial. For people with slower transit, sensitive digestion, or inadequate fluid intake, a sudden increase in wheat bran can significantly worsen high fiber constipation.
Dr. Vu Nguyen, MD, addresses the nuance in fiber recommendations directly: “Eating more fiber has been shown to soften stool and improve stool frequency in patients with constipation. It’s the first-line treatment due to its potential benefits, low cost, and minimal side effects. But increased fiber intake may sometimes worsen constipation. And the role of fiber supplement in IBS or IBD patients is more complex.”
Fiber supplements, including psyllium, inulin, wheat dextrin, and chicory root extract, vary significantly in their fermentability and their effect on gut motility. Psyllium is the most extensively studied and generally the most tolerable because it is soluble but only mildly fermentable.
Inulin and chicory root are highly fermentable, which means they can produce significant gas in people whose microbiomes are not adapted to processing them, even at moderate doses.
Conditions Where Fiber Needs a More Personalized Approach

Irritable bowel syndrome (IBS) is where the fiber and constipation relationship becomes most complex. For people with IBS-C, the evidence strongly supports soluble, low-fermentable fiber, particularly psyllium, as an effective intervention. The same evidence shows that insoluble fiber sources like wheat bran provide no significant benefit for IBS-C and can worsen bloating and discomfort.
A 2024 PMC narrative review of IBS management found that highly fermentable fiber sources, including certain short-chain soluble fiber types, can exacerbate gas and bloating in IBS patients by producing rapid fermentation in the colon. The review concluded that fiber type selection, rather than total fiber quantity, is the critical variable for IBS patients.
People with confirmed slow transit constipation, gastroparesis, or other gut motility disorders should work with a gastroenterologist before significantly increasing fiber intake.
The conveyor belt analogy applies here: if the digestive system is not moving, adding bulk makes the backup worse. In these cases, addressing gut motility through medical management may need to precede dietary fiber optimization.
After a gastrointestinal illness, antibiotic course, or significant dietary disruption, the gut microbiome is less diverse and less equipped to process large amounts of fermentable fiber. Reintroducing fiber gradually from gentle sources during recovery allows the microbial population to rebuild before being given a large fermentable load.
How to Increase Fiber Without Worsening Constipation
How to increase fiber safely means increasing total intake by no more than 5 grams per week, giving the gut microbiome time to adapt at each new level. Starting with soluble fiber sources such as oats, chia seeds, and cooked legumes before adding larger amounts of insoluble fiber is the approach most consistently associated with good tolerance.
Aim for at least 8 cups of water daily when fiber intake is being increased, and add more if physical activity levels are high or the climate is warm. Hydration and digestion are directly linked: every gram of additional dietary fiber requires additional water to function as intended.
Making fiber increase without fluid increases is the single most common reason eating more fiber but still constipated remains the outcome. The best fiber for constipation relief is not a single food but a balance.
Combining soluble fiber from oats, chia, flaxseed, and legumes with moderate insoluble fiber from whole grains and cooked vegetables produces the most consistent and gentle improvement in bowel regularity. Relying heavily on a single fiber supplement or food category reduces the diversity of fermentation substrates available to the gut microbiome.
For how to increase fiber safely in sensitive individuals, the most tolerable starting points are cooked vegetables rather than raw, well-cooked legumes rather than canned or undercooked, oats in porridge form, and chia seeds soaked in liquid. These forms reduce the mechanical demand on the digestive system while still delivering meaningful fiber and resistant starch.
Read More: Too Much Fiber in Your Diet? Tips to Balance Your Intake
Other Lifestyle Factors That Influence Fiber’s Effect
Movement directly stimulates gut motility by increasing blood flow to the digestive organs and triggering the parasympathetic nervous system responses that support peristalsis. Even moderate walking for 20 to 30 minutes after meals has documented effects on digestive transit time.
Sedentary behavior is independently associated with constipation, which means adding fiber without increasing movement provides only a partial solution. Consistent meal timing supports the gastrocolic reflex, the natural wave of increased bowel motility that follows eating.
Eating at irregular times or skipping meals disrupts this reflex and reduces the natural opportunities for stool to move toward elimination. Regular meals, particularly breakfast, support the gut’s natural daily rhythm in ways that directly support fiber and constipation management.
Chronic stress activates the sympathetic nervous system, which slows gut motility as part of the fight-or-flight response. For people already dealing with constipation, high stress levels can significantly blunt the benefit of dietary fiber increases.
The gut-brain axis is a two-way communication system, and stress management is a legitimate component of any high fiber constipation plan that is not producing the expected results.
When to Seek Medical Advice for Constipation
Dr. Vu Nguyen, MD, is clear on the threshold for professional evaluation: “If you have occasional constipation or have chronic constipation but don’t get enough fiber, adding fiber can often help. But if increasing fiber doesn’t work or your constipation is accompanied by other symptoms, it’s important to see a gastroenterologist to diagnose the problem and get the right care.”
Constipation lasting more than three weeks without improvement from dietary and lifestyle changes warrants medical evaluation. Symptoms that should prompt earlier evaluation regardless of duration include blood in the stool, unintentional weight loss, severe or persistent abdominal pain, and a sudden change in bowel habits in someone over 45 who was previously regular.
These can indicate conditions, including colorectal polyps, inflammatory bowel disease, or other structural changes that require diagnosis rather than dietary adjustment.
Fiber supplements and constipation: if a psyllium supplement is used consistently for two to three weeks at the recommended dose with adequate hydration and has not improved symptoms, a gastroenterology assessment is the appropriate next step rather than switching to a different supplement.
Key Takeaway: Fiber Works Best With the Right Balance
Fiber and constipation are not simply opposite ends of the same dial. The relationship is mediated by fiber type, hydration, digestion, gut motility, and gut microbiome composition in ways that vary substantially between individuals.
Why fiber causes constipation in some people is not a mystery once these variables are understood, and the fix is almost always in the approach rather than in abandoning fiber altogether.
How to increase fiber safely means going slowly, drinking more water, starting with soluble fiber sources, and paying attention to which foods the body responds well to. Soluble vs insoluble fiber digestion produces different effects and suits different situations.
The best fiber for constipation relief is psyllium for most people, particularly those with sensitive digestion, because it softens stool without the aggressive fermentation that produces gas and bloating.
And if eating more fiber but still constipated describes your experience after a few consistent weeks of doing it right, that is information worth discussing with a gastroenterologist rather than a reason to conclude that fiber does not work.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare provider or registered dietitian regarding persistent digestive symptoms or before making significant dietary changes.
References
- Bulsiewicz, W. (2022). The fiber paradox. Forks Over Knives.
- Christodoulides, S., et al. (2016). Dietary fiber and IBS: A systematic review. PMC.
- Dupont, C., et al. (2014). Dietary fiber for functional constipation and colonic motility. Journal of Clinical Gastroenterology.
- Gupta, V., & Schecter, M. (2024). Management of irritable bowel syndrome: A narrative review. Translational Gastroenterology and Hepatology.
- Nguyen, V. (2024). Constipated? Why more fiber might not be the answer. University Hospitals Health Essentials.
- Rossi, M. (2025). The Gut Health Doctor: Clinical constipation management protocols. King’s College London / The Gut Health Clinic.
- Stacewicz-Sapuntzakis, M., et al. (2009). Chemical composition and potential health effects of prunes. PMC. Referenced via
- Mayo Clinic Staff. (n.d.). Dietary fiber: Essential for a healthy diet. Mayo Clinic.
- MedlinePlus. (n.d.). Dietary fiber. U.S. National Library of Medicine.
- Harvard T.H. Chan School of Public Health. (n.d.). Fiber.
- WebMD Editorial Contributors. (n.d.). Types of fiber: Soluble and insoluble fiber. WebMD.
- Tata 1mg. (n.d.). Understanding dietary fiber: Soluble vs. insoluble.
In this Article