- Skin icing can reduce puffiness temporarily, but repeated direct ice contact can damage the skin barrier and increase water loss.
- It may also weaken capillaries and trigger flare-ups, especially in conditions like rosacea or sensitive skin.
- Risks vary: healthy skin may tolerate occasional icing with proper technique and a barrier.
- For people with rosacea, eczema, or recent treatments, the risks outweigh the benefits, and safer alternatives are better.
Every few months, a new skincare trend takes over social media, and the appeal of skin icing is easy to understand. Grab an ice cube, run it across your face for a few minutes, and allegedly enjoy tighter pores, reduced puffiness, and a visible glow. It is free, it is fast, and the before-and-after content is convincing enough that millions of people have tried it.
What does not make it onto the TikTok clips is what happens over time, or what happens to the people whose skin does not respond the way the influencer’s did. Because ice facial risks are real and depend heavily on skin type, application method, frequency, and the underlying condition of the skin barrier at the time of contact.
For some people, skin icing is a tolerable occasional ritual with modest short-term results. For others, it is quietly triggering the exact problems they are trying to solve. Dermatologists are not universally opposed to cold therapy for the skin.
But they are clear about the gap between how skin icing is typically practiced on social media and how cold should actually be applied to preserve rather than compromise skin barrier function.
This article breaks down what actually happens to your skin barrier during icing, which conditions make the practice genuinely risky, how to apply cold therapy more safely if you choose to continue, and what alternatives deliver similar results without the compromise.
Read More: Post-Workout Skincare: How to Keep Breakouts and Redness at Bay After a Sweat Session
What Is Skin Icing and Why Has It Become So Popular?
Skin icing refers to the practice of applying ice directly to facial skin, either through ice cubes held in a cloth, ice rollers stored in the freezer, or by submerging the face in ice-cold water, sometimes called a cryo facial or cold plunge for the face.
The trend accelerated significantly on TikTok and Instagram through 2022 and 2023, driven by claims of instant depuffing, temporary pore tightening, reduced redness, and a bright, refreshed complexion. The claimed ice facial benefits are grounded in a real physiological mechanism: vasoconstriction, or the narrowing of surface blood vessels in response to cold.
When vessels constrict, fluid temporarily moves away from the surface, which is why a cold compress reduces swelling around a bruise. Applied to the face, the same response temporarily reduces morning puffiness and gives skin a tighter, more awake appearance.
These results are visible in the short term, which is part of why the trend sustains itself. The problems are subtler, longer-term, and more contingent on individual skin type and application habits. That is where dermatologists want people to pay more attention.
How the Skin Barrier Actually Works, and Why It Matters
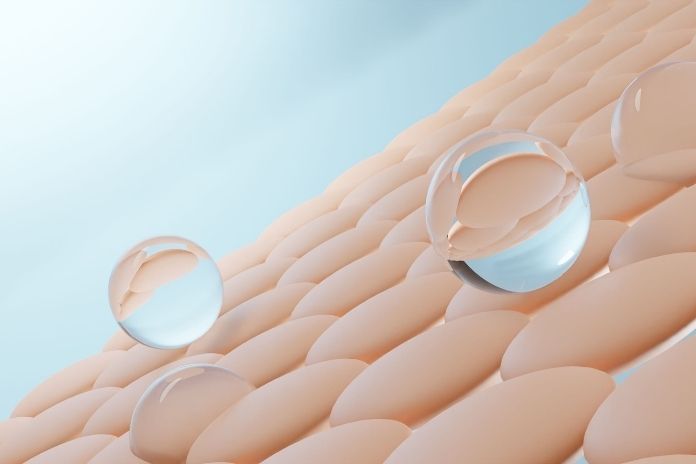
The skin barrier, technically the stratum corneum, is the outermost layer of skin. It is composed of flattened, protein-filled cells called corneocytes embedded in a lipid matrix of ceramides, free fatty acids, and cholesterol.
The arrangement has been compared to bricks and mortar: the cells are the bricks and the lipids are the mortar, together forming a semipermeable membrane that keeps moisture in and irritants, bacteria, and environmental stressors out.
Skin barrier function depends on the integrity of those lipid layers. When they are disrupted, whether by harsh cleansers, over-exfoliation, weather, or extreme temperature exposure, the barrier becomes leaky.
The clinical measurement of barrier disruption is transepidermal water loss (TEWL), the rate at which water passively evaporates through the skin. High TEWL means the barrier is compromised, the skin is losing moisture faster than it should, and it is more vulnerable to irritation from anything it subsequently contacts.
A PMC review of skin barrier function and its clinical relevance confirms that even mild disruptions to the lipid matrix of the stratum corneum produce measurable increases in TEWL and skin sensitivity and that recovery of barrier function after disruption can take days to weeks, depending on the severity of damage and the individual’s skin type.
The review notes that cold exposure specifically reduces the fluidity of skin lipids, which stiffens the barrier and can impair its self-repair mechanisms.
Dr. Muneeb Shah, DO, has made skin barrier protection the central tenet of his clinical and consumer work: the goal of dermatology-grade skincare, he consistently emphasizes, is to break down dirt and makeup “without stripping the skin of its natural oils and disrupting the barrier.”
Skin barrier damage leads downstream to a predictable sequence of problems: increased TEWL, dryness, heightened reactivity to products and environmental triggers, breakouts from impaired immune defense at the skin surface, and, in people with underlying conditions, significantly worsened symptoms.
Anything that disrupts barrier integrity without a compensating benefit, which includes incorrectly applied ice, belongs in the risk column of the ice facial risks ledger.
Can Ice Really Damage Your Skin Barrier?
Cold temperature reduces the fluidity and mobility of skin surface lipids. The ceramides, fatty acids, and cholesterol compounds that form the barrier’s protective matrix become less pliable in cold conditions, reducing their ability to fill gaps in the stratum corneum and maintain its water-holding function.
Repeated cold exposure can, over time, reduce the surface concentration of these lipids, producing dryness, flaking, and tightness that persist after the ice is removed. This effect is more pronounced with direct ice contact than with a cloth-buffered application and more pronounced in people who already have compromised or lipid-depleted skin.
For anyone already dealing with skin barrier damage, dry skin, or seasonal dryness, the skin icing side effects of increased dryness are not theoretical. They are cumulative.
Cold-Induced Vasoconstriction and Rebound Inflammation
The vasoconstriction produced by ice application is real and produces the visible depuffing effect that makes the trend appealing. But vasoconstriction is always followed by vasodilation, the rebound opening of blood vessels as circulation returns to normal temperature.
Research on cold-induced vascular responses published documents this reactive hyperemia response and notes that repeated cycles of constriction and dilation stress the vessel walls.
Dr. Alexander Sobel, MD, explains both sides of the vasoconstriction response: “When you apply ice to your skin, it causes vasoconstriction, the temporary narrowing of blood vessels. This reduces blood flow to the area, which can help decrease inflammation and puffiness.”
The rebound vasodilation can temporarily worsen redness and flushing, which is the opposite of what most people who try skin icing are hoping to achieve. For people with sensitive skin triggers or any tendency toward cold-induced inflammation, the post-icing rebound can be more visible than the pre-icing state.
Frostnip, the precursor to frostbite, can occur with prolonged direct ice contact, particularly on thin-skinned areas like the under-eye. The skin does not need to freeze to sustain surface injury.
Cellular damage begins at temperatures well above freezing when exposure is sustained because the cells lining the skin surface are designed to function within a narrow temperature range. More than five minutes of continuous direct ice contact to the same area can produce persistent redness, stinging, and surface trauma that takes days to resolve.
Read More: Cold Plunges and Workout Recovery: A Game-Changer or Just Another Trend?
Why Skin Icing May Trigger Flare-Ups Instead of Calming Skin
Skin icing rosacea flare-up risk is one of the clearest contraindications in the dermatology literature. Rosacea is characterized by increased capillary fragility, impaired skin barrier function, and a neurovascular reactivity that makes blood vessels on the face hyper-responsive to temperature changes, including cold.
A 2024 narrative review of epidermal skin barrier dysfunction found that rosacea patients have significantly elevated baseline TEWL, altered lipid composition in the stratum corneum, and a compromised barrier that worsens with exposure to temperature extremes.
Cold exposure that seems mild to healthy skin can trigger a significant inflammatory cascade in rosacea-prone skin, producing flushing, increased telangiectasia, and pain.
The American Academy of Dermatology, in its guidance for rosacea patients, advises washing the face with lukewarm water rather than hot or cold water precisely because temperature extremes are a documented trigger. Skin icing applies cold far more intensely than cold water rinsing.
Eczema and Compromised Skin Barriers
A PMC review of eczema and skin barrier dysfunction confirmed that atopic dermatitis is associated with significantly reduced ceramide content, higher baseline TEWL, and a barrier that is functionally impaired before any external stressor is applied.
Cold exposure adds a stressor to an already compromised system, reducing lipid fluidity and potentially triggering the itch-scratch cycle that drives eczema flares. For eczema patients, ice facial risks include worsening itch, increased dryness, and a barrier disruption that takes significantly longer to repair than it would in healthy skin.
Read More: 10 Everyday Triggers of Atopic Dermatitis (Eczema) Flare-Ups—and How to Avoid Them
Acne-Prone Skin: Temporary Relief vs. Long-Term Irritation
The case for whether skin icing is good or bad for acne is genuinely nuanced. The vasoconstriction produced by ice on an active pimple does temporarily reduce the swelling, redness, and pain of an inflamed lesion, and this is the most clinically defensible application of skin icing for acne. The problem is friction.
Rubbing ice across the face introduces mechanical irritation to the stratum corneum, can transfer bacteria from the ice surface to other areas of the face, and can worsen barrier function in the surrounding skin in ways that promote, rather than prevent, future breakouts.
Dr. Papri Sarkar, MD, recommends a crucial step when icing: “applying a face oil or moisturizer next… there’s less friction and traction, so [you’re] not causing skin damage without meaning to by exfoliating or rubbing.”
She specifically notes this is especially important for deeper skin tones, where friction from rubbing can trigger post-inflammatory hyperpigmentation.
Who Should Avoid Skin Icing Completely?
The populations for whom ice facial risks outweigh benefits are identifiable and consistent across dermatology guidance. People with rosacea or visible telangiectasia should not ice their faces, as cold is a documented skin icing rosacea flare-up trigger.
People with active eczema or chronic dry skin should avoid it because their already-elevated TEWL makes additional barrier stress disproportionately damaging. Anyone with existing broken capillaries or capillary fragility, as Dr. Sobel notes directly, should avoid icing entirely.
People in recovery from chemical peels, laser resurfacing, microneedling, or retinoid-induced peeling have a compromised and actively healing barrier that cannot tolerate temperature extremes. People with Raynaud’s phenomenon or cold urticaria, a condition in which cold triggers hives, should also avoid skin icing entirely.
This is not a universally dangerous practice. It is a selectively dangerous one, and knowing which group you are in determines whether the trend is worth exploring.
Is There Any Safe Way to Try Skin Icing?

How to Minimize Risk
How to use ice on the face safely requires a few non-negotiable steps. Never apply ice directly to bare skin. Always wrap it in a clean, thin cloth or use a properly designed cryo tool designed for facial use. Limit total contact time to one to two minutes per session. Move the ice or tool continuously rather than holding it in one spot.
Avoid applying pressure, which worsens friction damage and increases the force on capillaries. Follow with an immediately applied moisturizer containing ceramides or barrier-supportive ingredients to replace what the cold has temporarily disrupted. Ice facial for puffiness: safe or not, it depends almost entirely on following these steps.
When to Stop Immediately
Any stinging, burning, numbness, or redness that does not resolve within five to ten minutes of stopping is a signal that the skin has been stressed beyond its tolerance.
Persistent redness, a sensation of tightness that feels like a burn rather than refreshment, or increased sensitivity to your usual skincare products in the days following are all indicators that the skin barrier was compromised and that skin icing side effects are outweighing any benefit.
Safer Alternatives That Give Similar Results
Ice facial for puffiness safe or not? It becomes a less urgent question when alternatives are considered. A jade roller or gua sha tool stored in the refrigerator, not the freezer, delivers a mild cold stimulus through a smooth, consistent surface that does not produce the dramatic temperature shock of direct ice.
Chilled gel masks provide even, brief cold exposure without friction. Cold water splashing is effective for refreshing the skin and producing a mild vasoconstriction effect without the contact intensity of ice.
Skincare products containing caffeine reduce puffiness through a different mechanism, by improving microcirculation and reducing fluid accumulation, without any cold-related skin barrier damage risk. Green tea extract, aloe vera, and panthenol-containing products provide cold-induced inflammation-calming benefits without temperature extremes.
What Dermatology Evidence Says About Ice Facials
Dr. Jessica Garelik, MD, summarized the clinical picture plainly when asked by National Geographic what harm rubbing an ice cube on the face could cause: “Ice coming into contact with the skin can potentially damage the skin barrier due to its freezing temperature. This can be problematic for patients whose skin is already dry and sensitive.”
The clinical evidence supporting skin icing as a beneficial skincare practice is essentially absent. There are no randomized controlled trials. There are no longitudinal studies of ice facial outcomes. The mechanism for short-term depuffing is real and physiologically sound, but the durability of the effect is zero once circulation normalizes.
The risks, particularly skin barrier damage, TEWL increase, skin icing, rosacea flare-up, and ice causing broken capillaries, are better documented precisely because they are adverse events that bring patients to dermatologists.
Absence of evidence for benefit combined with documented evidence of harm in specific populations is the appropriate framing for an honest assessment of this trend.
Read More: Can Too Many Skincare Actives Damage Your Skin Barrier?
Key Takeaway: Should You Stop Skin Icing?
Skin icing is not inherently dangerous for everyone. On healthy, resilient skin, with a cloth barrier, a two-minute maximum, and moisturizer applied immediately after, occasional icing is unlikely to cause significant harm and may provide a brief, enjoyable depuffing effect.
The problem is that the trend is practiced far beyond those parameters. Direct contact, prolonged sessions, daily use, and application to skin that is already dry, reactive, or condition-affected, is where ice facial risks become genuine skin barrier damage risks.
Skin icing side effects, including increased TEWL, cold-induced inflammation, capillary fragility, and skin icing rosacea flare-ups, are documented and underreported relative to the trend’s reach. If your skin feels better after icing, continue with the safe application guidelines.
If you have rosacea, eczema, broken capillaries, or sensitive skin triggers, skip the ice and reach for a chilled roller or a caffeine serum instead. The goal of any skincare practice should be supporting skin barrier function over time, and that goal is better served by consistent, gentle habits than by a daily cold shock.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical or dermatological advice. Consult a board-certified dermatologist for guidance specific to your skin type and conditions.
References
- Garelik, J. (2024). Ice facials: What dermatologists say. Referenced in: Collins, L. Is an ice facial good for your skin? Deseret News / National Geographic.
- Maden, S. (2024). Epidermal skin barrier and skin care in rosacea: A narrative review. Journal of Dermis.
- Proksch, E., Brandner, J. M., & Jensen, J. M. (2008). The skin: An indispensable barrier. Experimental Dermatology.
- Sarkar, P. (2024). Does icing your skin have real benefits? Kiehl’s.
- Shah, M. (2026). Dr. Shah winter skin care. Good Morning America.
- Sobel, A. (2025). Get the most out of skin icing with these top tips. Anderson Sobel Cosmetic.
- Thyssen, J. P., & Kezic, S. (2014). Causes of epidermal filaggrin reduction and their role in the pathogenesis of atopic dermatitis. Journal of Allergy and Clinical Immunology.
- Wigington, G., Nishi, K., & Wilkinson, J. (2003). Skin blood flow responses to the cold pressor test. Clinical Physiology and Functional Imaging.
- Spranklen, A. (2023, September 5). Skin icing is the new chilly facial trend that instantly tackles spots and redness. Vogue India.
- Meier, C. (2020, November 16). New beauty trend: Skin icing. Mibelle Biochemistry.
- Clinikally. (2022, September 27). How skin icing can transform your beauty routine. Clinikally.
- Inside Beauty Spa. (n.d.). Hyaluronic acid serum home remedy tips. Inside Beauty Spa.
In this Article