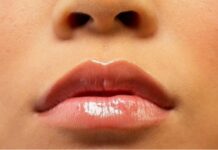
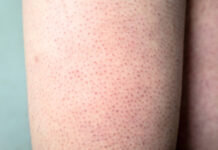
Often referred to as the “chicken skin,” keratosis pilaris is a very common, benign skin condition that results in tiny, rough bumps on the arms, thighs, and, occasionally, the face. Although the condition is not harmful in and of itself, many suffer more from the aftereffects of irritation or picking, particularly dark spots, uneven tone, and persistent blemishes.
Everything you need to know about healing discoloration and texture changes brought on by KP will be covered in this article. You will discover the causes of keratosis pilaris hyperpigmentation, how actual dermatology practice treats chicken skin scars, the safest techniques for KP dark spots, and how to fade them.
To help you understand how to treat KP marks without further harming your skin barrier, we will also cover substances, routines, timetables, and pitfalls to avoid.
- Stop picking KP bumps to prevent worsening of dark spots and delaying healing.
- Use gentle exfoliants (lactic acid, salicylic acid, urea) and moisturize daily to repair skin and fade marks.
- Stay consistent; visible improvement usually takes 4–6 weeks with proper care.
Read More: Eczema Scars: How to Heal Discoloration and Redness Safely
Why Picking Keratosis Pilaris Leads to Dark Spots and Scarring
Because the little bumps act as a stimulus to pick, people with Keratosis Pilaris and obsessive skin picking disorder suffer more. Some suggest that the hump’s appearance and the urge to get rid of it drive picking, while others assert that people pick because they want to eliminate the tactile sensation of the bump.
The problem for those who pick at their skin is that they frequently leave scars, as the lumps are hard to remove and can form rash-like accumulations.
The skin perceives picking or scratching KP bumps as an injury. As a defensive response, this triggers the repair pathways that increase melanin production. Unfortunately, rather than restoring clarity, this defense mechanism produces noticeable discoloration.
When inflammation causes melanocytes, which produce pigment, to release excess melanin, the condition known as post-inflammatory hyperpigmentation can develop. Keratosis pilaris can also develop. Brown, red, or purple marks are left behind as this pigment moves into the top layers of the skin.
According to scientific research, PIH is more prevalent in individuals with medium- to deep-skinned tones due to increased baseline melanin activity. It explains why some people have more noticeable KP dark spots than others.
What “Chicken Skin” Marks Usually Look Like
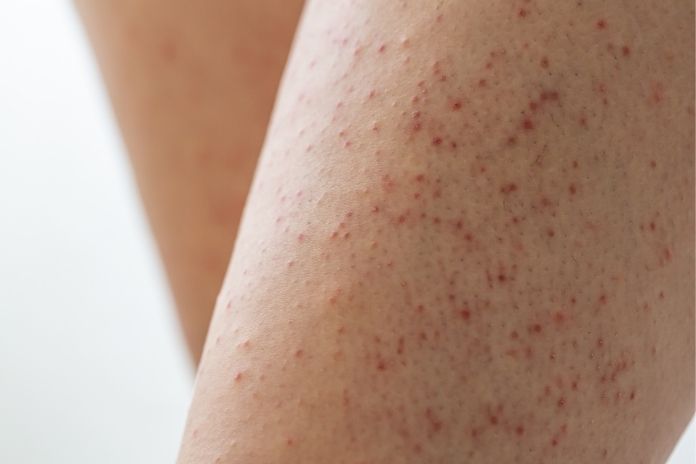
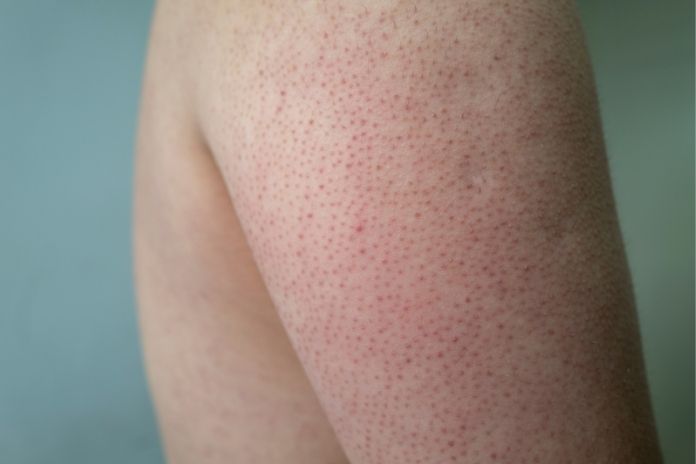
Keratosis pilaris, sometimes abbreviated as KP, is a perfectly benign skin disorder that causes tiny, rough bumps that resemble perpetual goosebumps. Keratosis pilaris is actually a fancy term for follicular bumps, which are little, hard plugs in the hair follicles that cause your skin to feel scratchy.
KP-related pimples are typically flesh-colored, but they can occasionally be redder or darker than the surrounding skin. In certain instances, the area may appear somewhat irritated, and the texture frequently resembles sandpaper. Many people observe that KP improves in the summer and worsens in the winter, when the skin is typically drier.
“The condition is harmless and may eventually resolve on its own,” said Stephanie McNamara, MD, a dermatologist at Riverchase Dermatology. “But if it bothers you, you can reduce the symptoms at home with regular use of an exfoliating product and a good moisturizer.” In extreme cases, she added, if keratosis pilaris self-care measures don’t work, you may want to see a dermatologist for prescription topical medication or perhaps laser treatment.
First Step: Stop the Cycle of Picking
Preventing further damage is the most crucial part of any treatment for chicken skin scars. Even the best goods won’t function properly without it.
Repeated picking irritates the skin, slows down the healing, and exacerbates hyperpigmentation in keratosis pilaris.
To break the cycle of how to stop picking keratosis pilaris, dermatologists recommend the following:
- Keep the skin well hydrated to reduce roughness and the urge to pick
- Cover irritated areas to prevent unconscious scratching
- Keep nails short to minimize damage from unintentional contact
- Treat underlying dryness to reduce the initial sensation that triggers picking
Why this matters:
- Breaking this cycle allows the skin to enter a more stable phase
- In this state, treatments can more effectively help fade keratosis pilaris–related dark spots
Read More: Acne Scars 101: How to Treat Different Types of Scars Effectively
Ingredients That May Help Fade Hyperpigmentation
Using chemicals that gently promote skin renewal without irritation is a key component of maintaining the best treatment for KP dark spots.
Treatment may help reduce the appearance of the characteristic bumps, but it won’t eliminate them right away. Both prescription and over-the-counter drugs are available. For instance:
- Topical formulations containing urea, salicylic acid, lactic acid, ammonium lactate, or a combination of these substances treat the skin directly
- Topical retinoids, including adapalene and tretinoin
- Topical steroids to relieve itching or redness
- Laser treatments
Barrier Repair: Why Moisturizing Matters for Healing
Resolving body hyperpigmentation from KP requires a healthy skin barrier. Prolonged inflammation and heightened sensitivity result from a compromised barrier. Picked keratosis pilaris scars take longer to heal as a result.
Ceramides, fatty acids, and cholesterol are among the substances that help rebuild the barrier. This procedure promotes long-term healing and lowers inflammation.
Because urea moisturizes and gently exfoliates, urea-containing moisturizers are very effective. Dermatology references consistently highlight urea as a gold-standard ingredient in chicken-skin scar treatment routines.
Without proper barrier repair, even advanced KP dark spot treatments will be less effective at fading.
Body Care Routine for KP Marks
When treating keratosis pilaris on the arms, a regular regimen is more crucial than aggressive therapy.
Mild Cleaning: Instead of using a harsh or drying body wash, use a gentle one. Cleaners with a high sulfate content might remove natural oils and highlight pimples.
Mild Exfoliation: Avoid using loofahs and strong scrubs, as they may irritate the skin. Instead, search for mildly acidic exfoliants such as the following:
- Lactic Acid: Excellent for moisturizing and smoothing tough areas
- Urea: Keeps skin hydrated and aids in the breakdown of keratin plugs
- Salicylic Acid: A beta-hydroxy acid that exfoliates inside the follicle
ABM (always be moisturizing): A thick, fragrance-free moisturizer is your best friend, as dryness can exacerbate KP. To ensure you stay hydrated, apply it immediately after taking a shower.
Be Patient: KP doesn’t get better right away. Before you see smoother skin, you may need to follow steps 1-3 consistently for weeks or even months. Sticking with it is crucial.
Sun protection is important but frequently disregarded. Keratosis pilaris hyperpigmentation can be exacerbated by UV exposure, increasing the persistence of dark patches.
Read More: Top Ways on How to Get Rid of Acne Scars at Home
How Long Does It Take for KP Hyperpigmentation to Fade
The dermatologic healing timeline varies depending on skin type, severity, and consistency of care.
Keratosis pilaris pimples may not go away immediately, even with treatment. You should see results in four to six weeks if you adhere to your treatment plan.
The majority of keratosis pilaris cases begin to clear around the mid-20s and typically resolve entirely by age 30, even without treatment.
What to Avoid While Treating KP Marks
For KP dark spots, avoiding bad habits is just as crucial as applying treatments. Steer clear of coconut oil for treating keratosis pilaris and other skin conditions. It is comedogenic, meaning it clogs pores and tends to exacerbate the issue (since KP already clogs pores, this would be a double-clog).
Don’t waste time with coconut oil; the goal is to clear those pores. Because it is gentler, jojoba oil may help reduce inflammation and redness around KP pimples.
When Dark Spots May Need Professional Treatment

Not every person with KP needs medical attention. However, it may be time to consult a professional if your skin is very dry or itchy, or if you’re just sick of trying every over-the-counter lotion in the store.
Dermatologists who specialize in keratosis pilaris advise seeking expert treatment if:
- You feel self-conscious due to the numerous bumps
- Home remedies have not produced any progress
- You’re feeling irritated, red, or itchy
- You don’t know if what you have is truly KP
Read More: Say Goodbye to Acne and Fade Scars with These 4 Home Remedies
Conclusion
Handle KP-related marks gently, consistently, and patiently. Although keratosis pilaris hyperpigmentation can be annoying, it is typically transient and gets better with the right treatment. The secret is to protect the skin barrier, quit picking, and consistently apply pigment-balancing and mildly exfoliating products.
Focusing on long-term skin health rather than quick fixes will deliver better results. With the right routine, even stubborn discoloration and concerns about chicken skin scars can gradually improve over time.
References
- Loyd Godwin. (September 18, 2025). What is “Chicken Skin”? Understanding and Treating Keratosis Pilaris in Connecticut.
- Trudi Griffin. (May 25th, 2018). Keratosis Pilaris and Skin Picking Disorder.
- Snyder Dermatology. (n.d.). Understanding keratosis pilaris: Causes, symptoms, and treatments.
- Forefront Dermatology. (2025, October 20). Keratosis pilaris: The bumps no one talks about (but everyone Googles).
- American Academy of Dermatology Association. Keratosis pilaris: Diagnosis and treatment.
- Mayo Clinic. (October 23, 2024). Keratosis pilaris.
- Harvard Health. (January 23, 2024). Keratosis pilaris: Treatment and self-care for this common skin condition.
- National Health Service (NHS). (2024, July 4). Keratosis pilaris.
- Soft Services. (2024, October 6). What ingredients should you avoid with keratosis pilaris?
- Schweiger Dermatology Group. Keratosis pilaris.
In this Article