Most people think Pelvic Inflammatory Disease (PID) only comes from significant sexually transmitted diseases (STIs) like chlamydia or gonorrhea, as per numerous articles. But in reality, this is not entirely true. Doctors see patients having negative reports; still, infection persists in the upper reproductive organs. This leads to confusion.
Another problem: yeast infection masking symptoms. Early PID symptoms do not always lead to intense pain or fever. Sometimes it’s in the form of white discharge, itching, and little irritation. Many people assume their symptoms are due to a yeast infection and start over-the-counter antifungal treatment.
However, if the underlying issue is bacterial, this delay in appropriate treatment allows the infection to persist and potentially spread upward. The concern is not rapid aggressiveness, but a silent, mixed, or misdiagnosed infection.
- PID is not always caused by STIs. Hidden bacteria like Mycoplasma genitalium, BV-related organisms, and normal vaginal bacteria can also lead to infection.
- Yeast infection symptoms can confuse diagnosis and delay the treatment.
- A negative STI test does not rule out PID, so proper evaluation is important.
Can You Develop PID Without Chlamydia or Gonorrhea?
Yes, and it is also not rare. PID is never always about one bacterium causing the problem. Many times, it is a combination of factors. This is called a polymicrobial infection, which simply means that more than one type of bacteria is working together, leading to PID.
In the lower genital tract, many bacteria are already present. Some are harmless normally. But if the balance changes, they can start behaving differently. They can attach to the lining, irritate tissue, and slowly move upward.
Standard STI testing is limited. It checks only for a few organisms. So when the result comes as negative, the patient feels relaxed. Even some doctors may never go deeper immediately to test more if symptoms are mild.
But infection does not depend on the test panel. If bacteria are not included in the testing panels, then they will not show on the reports too. This is where many PID cases are missed in the early stage.
Hidden Bacteria #1: Mycoplasma Genitalium
1. What it is and how it spreads
Mycoplasma genitalium is a very small bacterium. It does not have a typical cell wall like other bacteria. Because of this, it behaves differently and is also harder to treat. It spreads mainly through sexual contact. But compared to other STIs, it is more silent. “Sometimes doctors might not know about it until a patient comes with pelvic inflammatory disease,” said Dr. Sarah Yamaguchi, OBYGN. Many people carry it without knowing. No strong symptoms are obvious in the beginning.
2. Why it’s often missed in routine STI panels
Most standard STI panels do not include this test. The reasons are cost and availability, and also because it was not widely studied earlier. So even if infection is present, the report shows “negative.” This result gives a false sense of safety. Furthermore, the testing method is different. It needs a specific Nucleic Acid Amplification Test (NAAT). Not all labs include it by default.
3. Link between Mycoplasma genitalium and PID
This bacterium can infect the cervix first. A condition called cervicitis. From there, slowly it can move upward to the uterus and the fallopian tubes. The problem is that the symptoms are not clear. Initially, there is no high fever and no severe pain. So individuals ignore or delay a check-up.
Over time, reproductive tract inflammation builds. That is when a PID diagnosis becomes important, but the infection has already been there for a long time.
4. Treatment challenges and antibiotic resistance considerations
This is where it becomes tricky. Many antibiotics used for PID may not fully work on this bacterium. Antibiotic resistance keeps increasing after long-term treatment. Some patients take treatment, feel a little better, and then their symptoms come back. So, without proper identification, treatment becomes a trial-and-error type. This delays proper recovery.
Hidden Bacteria #2: Bacterial Vaginosis-Associated Organisms
1. How BV disrupts the vaginal microbiome
Bacterial Vaginosis (BV) is not exactly an infection like the others. It is a vaginal microbiome imbalance. Normally, good bacteria maintain an acidic environment and protect. But in BV, harmful bacteria increase, and good ones reduce. This changes the entire environment. This is an important point: the body loses its natural protection. Dr. Horace Fletcher, an OBYGN, notes that pregnant women are more likely to develop bacterial vaginosis because “during pregnancy, they produce large amounts of steroid hormones, like progesterone, which makes them more prone to infection.”
2. How BV-related bacteria can travel upward
When the protective barrier is weak, bacteria get a chance to move upward. This is not a sudden jump. It is a slow process. Small inflammation starts in the cervix. Then, over time, it spreads. Also, BV bacteria produce enzymes that can break down the mucus barrier. So bacterial entry inside reproductive organs becomes easier.
3. Why does BV increase PID risk even without an STI?
Even if no sexually transmitted infection is there, BV itself can create conditions for PID. Many women ignore BV because the symptoms are mild, such as a slight odor and discharge. Not always pain. But internally, the environment has changed. This increases the risk of ascending infection. So, PID in such a case is not from outside bacteria but from an imbalance inside itself.
Hidden Bacteria #3: Opportunistic Vaginal Bacteria
1. When “normal” bacteria become harmful
The body always has some bacteria. Especially in the vagina, many bacterial types exist, which is normal. But the problem starts when they go to places where they should not be. Like the uterus or fallopian tubes. There, the immune system reacts strongly, causing inflammation.
2. Situations that allow bacteria to enter the upper reproductive tract
There are certain times when this movement becomes easier:
- Intrauterine device (IUD) insertion: During insertion, the cervix is slightly open; this acts as an entry gate for bacteria.
- Childbirth or miscarriage: tissues are more sensitive and open and at risk of getting an infection.
- Gynecologic procedures: instruments can push bacteria upward.
These are not wrong procedures, but they temporarily change the barrier.
3. Evidence linking these bacteria to PID
Studies have found mixed bacteria in PID cases. Not just one organism. This shows that even normal vaginal flora can become a cause if conditions allow. So again, PID is not always an “external infection.” Sometimes it is an internal vaginal microbiome imbalance with an opportunity.
Why a Yeast Infection Might Be Hiding These Bacteria
1. Symptom overlap between yeast infection and early PID
A yeast infection causes itching, thick discharge, and irritation. Early PID may also show discharge and mild discomfort. But itching is a more noticeable symptom in a yeast infection. Pain during the early stage of PID is often dull, not sharp. So it’s usually ignored.
2. How itching and discharge can mislead self-diagnosis
Most people diagnose a yeast infection on their own. If the discharge is white, they assume it is fungal. Pharmacy medicines are easily available. So treatment starts without testing. But if bacteria are also present, they continue growing.
3. Delayed testing and missed co-infections
Sometimes both infections are present together: fungal and bacterial. Antifungal treatment stops itching. The person starts feeling normal. But bacterial infection remains hidden. This condition creates a delay of weeks or even months in starting treatment. By the time a proper check happens, the infection has already moved upward.
Signs Your Symptoms May Not Be Just a Yeast Infection

Some signs should not be ignored:
- Dull pelvic pain, not just itching
- Pain during intercourse
- Fever, even low-grade
- Bleeding between cycles
- Symptoms coming back again and again
If antifungal treatment is not giving full relief, then it is an important sign.
Why Standard STI Tests Don’t Always Detect These Infections
1. What routine panels typically include
Routine tests focus on common organisms only. This is a practical approach but limited.
2. Additional tests are sometimes needed
Tests for Mycoplasma genitalium or a detailed bacterial profile are not always done.
3. When doctors consider expanded screening
Usually, when symptoms persist or repeat. But if symptoms are mild, testing may not be extended early. This delay is the main reason hidden infections continue.
How Doctors Evaluate Possible “Hidden” Causes of PID
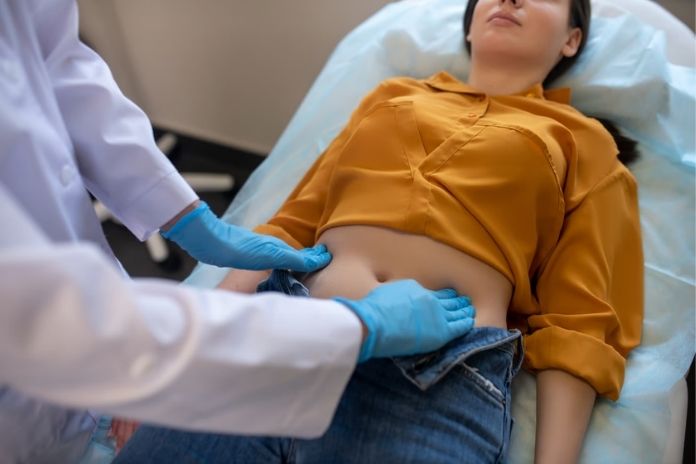
1. Symptom assessment and pelvic exam
The doctor checks the pain location, the discharge type, and tenderness. This gives clues about the disease.
2. Vaginal swabs and cultures
Swabs help understand the bacterial environment, not just a single infection.
3. Nucleic acid amplification tests (NAATs)
These tests detect specific organisms with more accuracy.
4. When imaging may be used
If a complication is suspected, an ultrasound is used, like an abscess or fluid collection.
Read More: Clitoris Itching: Causes, Treatments, and When to See a Doctor
Treatment Considerations for Non-Classic PID Bacteria

Treatment for non-STD causes of pelvic inflammatory disease is usually broad at the start. Because the exact bacteria are not known.
Combination antibiotics are given to cover multiple organisms. Later, if specific bacteria are identified, treatment may be adjusted. Completing the full course is very important. Stopping early can worsen resistance. In some cases, partner treatment is also needed.
Read More: Pain After Sex: Common Causes, What’s Normal and When to See a Doctor
Practical Steps to Reduce the Risk of Undetected PID

- Do not repeatedly self-treat a yeast infection without testing
- If symptoms keep coming, get a proper evaluation
- Notice a change in symptom pattern, not just the same discharge
- After procedures, watch for unusual pain or fever
- Do follow up if symptoms are not fully resolved
- Consult a gynecologist if there is recurrent itching or pain
- Test STIs yearly if under 25 or risky
- Follow-up post-IUD procedures
- USPSTF screens chlamydia. Catch it early and save your fallopian tubes.
- Boost lactobacilli via probiotics; use condoms.
For high-risk women (e.g., post-procedure), daily oral/intravaginal use post-antibiotics aids recovery, potentially preventing ascending polymicrobial PID. Combine with condoms (reduces exposure 80-90%), yearly STI screens under 25, and prompt visits to the gynecologist for persistent symptoms. Probiotics aren’t a cure-all, but they can support microbial balance alongside good hygiene, helping catch imbalances early and reduce the risk of longer-term complications.
Read More: What Vaginal Discharge Color Says About Your Health
Final Thoughts: PID Isn’t Always Caused by the Usual Suspects
PID is more complex than what we know generally. It is not just about STIs. Hidden bacteria, imbalance, and timing all play a role. The real danger is often the delay. What seems like a minor, familiar issue can be the early phase of a deeper infection—one that progresses silently if misread or mistreated.
- PID can happen without common STIs due to mixed bacterial involvement.
- PID stems from hidden bacteria like M. genitalium and BV bugs, not just STIs. They scar fallopian tubes, increasing the risk of infertility.
- Mycoplasma genitalium, causing PID, is often missed because it is not routinely tested
- Bacterial vaginosis increases PID risk by weakening natural protection.
- Yeast infection symptoms can hide early bacterial infection signs.
- Testing persistent symptoms early prevents infertility.
- Research gap: Routine testing still does not cover many bacteria linked with PID, so early-stage cases often remain undiagnosed.
- Undergo a pelvic check for odd discharge or pain to prevent long-term complications.
FAQs
1. Can PID occur without any STI?
Yes, due to an internal bacterial vaginal microbiome imbalance and opportunistic infections.
2. Why do tests come back negative, but symptoms are there?
Because many bacteria are not included in standard STI testing panels.
3. Is a yeast infection dangerous like PID?
No, but it can delay detection of bacterial infection.
4. Should I worry if symptoms keep coming back?
Yes, repeated symptoms need proper medical evaluation.
5. Can PID be completely cured?
Yes, if treated early and properly. Delay can cause complications.
References
- BROGDEN, K., GUTHMILLER, J., & TAYLOR, C. (2005). Human polymicrobial infections. The Lancet, 365(9455), 253–255.
- Savaris, R. F., Fuhrich, D. G., Duarte, R. V., Franik, S., & Ross, J. (2017). Antibiotic therapy for pelvic inflammatory disease. Cochrane Database of Systematic Reviews.
- Spencer, T. H. I., Umeh, P. O., Irokanulo, E., Baba, M. M., Spencer, B. B., Umar, A. I., Ardzard, S. A., Oderinde, S., & Onoja, O. (2014). Bacterial Isolates Associated with Pelvic Inflammatory Disease among Female Patients Attending Some Hospitals in Abuja, Nigeria. African Journal of Infectious Diseases, 8(1), 9–13.
- Centers for Disease Control and Prevention. (2021). Pelvic inflammatory disease (PID) – STI treatment guidelines.
- Jenkins, S. M., & Vadakekut, E. S. (2025). Pelvic inflammatory disease. In StatPearls. StatPearls Publishing.
- Blanchard, A. (2021). Mycoplasma genitalium. Journal of Infectious Diseases, 224(Supplement_2), S29–S34.
- Ness, R. B., et al. (2004). Bacterial vaginosis and risk of pelvic inflammatory disease. Obstetrics & Gynecology, 104(5), 761–769.
- Gaydos, C., et al. (2016). Mycoplasma genitalium prevalence, coinfection, and macrolide antibiotic resistance frequency. Journal of Clinical Microbiology, 54(8), 2120–2125.
- Workowski, K. A., et al. (2021). Sexually transmitted infections treatment guidelines. MMWR Recommendations and Reports, 70(4), 1–187.
- Swidsinski, S., et al. (2023). Bacterial vaginosis—Vaginal polymicrobial biofilms and their role as a mediator of reproductive tract infections. Deutsches Ärzteblatt International, 120(20), 335–342.
- Lis, R., et al. (2015). Intrauterine devices & infection: Review of the literature. Contraception, 92(1), 1–8.
- Brunham, R. C., Gottlieb, S. L., & Paavonen, J. (2015). Pelvic inflammatory disease. New England Journal of Medicine, 372(21), 2039–2048.
- Horner, P. J., et al. (2022). Mycoplasma genitalium management in adults. NCBI Bookshelf.
- Cleveland Clinic. (2023). Pelvic inflammatory disease (PID): Symptoms & treatment.
In this Article