- Pinky and ring-finger numbness usually results from ulnar nerve irritation. Still, the source can be either the elbow (cubital tunnel) or the neck (C8 nerve root), and they often feel identical.
- The key difference is pattern: neck-related issues radiate from the neck down the arm, while elbow compression stays localized and worsens with elbow bending.
- Getting the diagnosis right matters; treating the wrong site won’t fix the problem and can lead to permanent hand weakness or muscle loss if delayed.
Numbness in the pinky finger and part of the ring finger is one of those symptoms that looks simple until you try to find its source. Most people assume it is coming from the elbow, and sometimes it is. But in a meaningful number of cases, the problem originates much higher up, at the cervical spine, and the two conditions can look nearly identical on the surface. Getting the diagnosis right is what determines whether treatment actually works.
What makes this particular symptom tricky is how common it is and how easy it is to explain away. You lean on your elbow too long at a desk, and your pinky goes numb. You sleep with your arm bent and wake up with tingling in the ring finger. Most of the time, it resolves, and you move on. But when ulnar nerve numbness in the pinky finger keeps coming back or stops going away entirely, that pattern deserves more than reassurance.
The ulnar nerve and the C8 nerve root share almost exactly the same sensory territory in the hand, both supplying the pinky and the inner half of the ring finger. That anatomical overlap is precisely what creates the diagnostic problem. A patient with a pinched nerve in the neck due to a C7-T1 disc herniation can present with symptoms that look and behave almost identically to someone with cubital tunnel syndrome from compression at the elbow.
The stakes of getting it wrong are real. Someone treated for ulnar nerve entrapment symptoms at the elbow when the actual compression is in the cervical spine will not improve, because the nerve is being irritated at a site that was never addressed. Meanwhile, intrinsic hand muscle weakness can quietly progress toward changes that may not fully reverse even after the correct treatment is eventually applied.
Why Pinky Finger Numbness Happens

The Nerve Pathway That Supplies the Ring and Little Fingers
The ulnar nerve is the main highway for sensation in the pinky and the inner half of the ring finger. It originates from the C8 and T1 nerve roots in the lower cervical spine, travels through the brachial plexus, down the inner arm, around the elbow through the cubital tunnel, and into the hand via Guyon’s canal at the wrist. That is a long route with multiple potential compression points, and pinky finger numbness causes can arise at any one of them.
The two most clinically significant sites are the cervical spine, where the C8 nerve root exits between the C7 and T1 vertebrae, and the elbow, where the ulnar nerve passes through the narrow cubital tunnel just behind the medial epicondyle.
Understanding which one is responsible changes everything about how the condition is managed, because C8 radiculopathy vs ulnar neuropathy requires fundamentally different treatment approaches despite producing overlapping symptoms in the hand.
Two Common Sources of Nerve Compression
Cervical radiculopathy occurs when a nerve root is compressed at the spine itself, typically from a herniated disc, bone spur, or degenerative change at the C7-T1 level. The nerve is irritated before it even enters the arm, which is why symptoms from a spinal source can radiate across the entire length of the limb rather than concentrating at one point.
Peripheral nerve compression occurs downstream, most often at the elbow in cubital tunnel syndrome, and less commonly at the wrist in Guyon’s canal. Here, the nerve is structurally intact at the spine but mechanically irritated at a peripheral site.
The distinction matters clinically because a pinched nerve in the neck causing hand numbness requires cervical-focused treatment, while ulnar nerve entrapment symptoms at the elbow respond to entirely different interventions.
Dr. Sophia Strike, MD, hand and upper extremity surgeon at Johns Hopkins Medicine, describes the elbow-level compression plainly: “Cubital tunnel syndrome is a pinching of the large nerve that goes behind your elbow. People often think of it as your funny bone nerve,” she explains, noting that it develops from a combination of irritation and compression that builds gradually over time.
What Is C8 Radiculopathy?
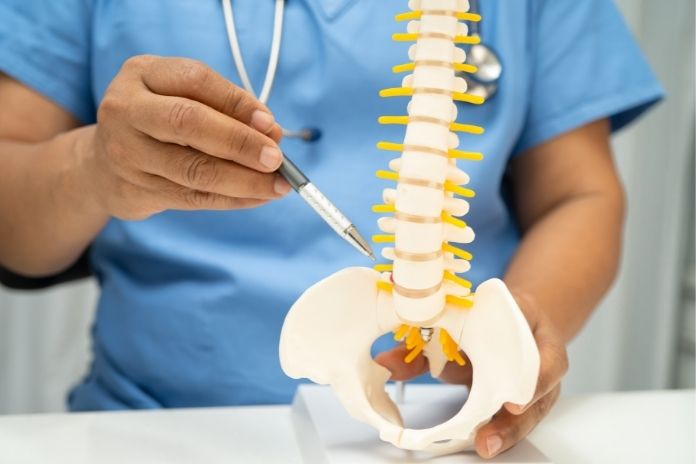
How a Cervical Nerve Root Becomes Compressed
C8 nerve root compression symptoms develop when the nerve root is mechanically irritated at the cervical foramen, the bony opening through which it exits the spine between the C7 and T1 vertebrae.
The most common causes are disc herniation at the C7-T1 level, bone spurs from degenerative spondylosis, or progressive narrowing of the foramen from age-related changes in the vertebral joints.
The C8 nerve root is the least frequently compressed of all cervical roots, which is part of why it gets missed even by experienced clinicians and why pinky finger numbness caused by a spinal source is often attributed to the elbow for months before the correct level is identified.
Unlike compression higher in the cervical spine, which more commonly produces neck and shoulder symptoms, C8 involvement tends to send symptoms distally into the forearm and hand. This distal distribution is what makes it so easy to confuse with a peripheral nerve problem.
Symptoms Often Seen With C8 Radiculopathy
The sensory territory of C8 overlaps almost exactly with the ulnar nerve: numbness in the ring and little finger, the inner forearm, and sometimes into the ulnar palm.
What distinguishes C8 radiculopathy vs ulnar neuropathy at the symptom level is the presence of neck pain or pain radiating from the neck through the shoulder and down the inner arm before reaching the hand. That proximal radiation pattern, starting at the neck and traveling downward, is the clearest indicator that the problem is spinal rather than peripheral.
Muscle weakness in C8 nerve root compression involves the thumb muscles specifically: the abductor pollicis brevis, flexor pollicis brevis, and opponens pollicis.
These muscles are innervated via the median nerve but receive their nerve root input from C8, so they are affected by a cervical lesion at that level but not by ulnar nerve entrapment symptoms at the elbow. This anatomical nuance is one of the most clinically useful differentiators and one of the most commonly overlooked.
What Is Ulnar Nerve Entrapment?
Where the Ulnar Nerve Is Most Commonly Compressed
Ulnar nerve entrapment symptoms most commonly arise at the elbow, where the nerve passes through the cubital tunnel just behind the medial epicondyle. This location is vulnerable because bending the elbow simultaneously stretches and compresses the nerve against the bony groove.
Prolonged elbow flexion, including sleeping with bent arms, resting on the elbow at a desk, or holding a phone to the ear for extended periods, can create enough cumulative irritation to produce elbow nerve compression symptoms that gradually worsen over months.
Less commonly, ulnar neuropathy occurs at the wrist within Guyon’s canal, which tends to produce purely hand symptoms without involving the forearm muscles that are supplied by ulnar nerve branches above the wrist. Distinguishing wrist-level from elbow-level compression matters for surgical planning.
Typical Symptoms of Ulnar Neuropathy
Cubital tunnel syndrome symptoms include intermittent numbness and tingling in the ring and little fingers, often worse with sustained elbow flexion and sometimes partially relieved when the elbow is straightened.
Ulnar nerve numbness in the pinky finger is frequently the first symptom patients notice, often described as the hand “falling asleep” during activities that involve a bent elbow. Grip weakness develops as compression affects the flexor digitorum profundus to the ring and little fingers.
Intrinsic hand muscle weakness affecting the interossei produces the characteristic difficulty spreading the fingers apart, a finding known as finger abduction weakness, which is one of the most specific signs of ulnar nerve dysfunction at the elbow level.
Dr. Lisa Lattanza, MD, Chair of Orthopedics and Rehabilitation at Yale School of Medicine, describes the typical presentation: “Cubital tunnel syndrome causes an ache in your forearm close to your elbow,” she told WebMD, adding that clinicians typically have patients maintain the elbow in a flexed position during examination to reproduce symptoms before confirming the diagnosis.
Key Symptom Differences Between C8 Radiculopathy and Ulnar Nerve Entrapment
Pattern of Pain and Numbness
With C8 radiculopathy, pinky finger numbness causes typically trace from the neck through the shoulder and down the inner arm before reaching the hand, with the forearm often involved along the way. With ulnar nerve entrapment, symptoms concentrate in the hand and around the elbow without that proximal neck-to-arm radiation pattern.
Ulnar nerve numbness in the pinky finger from cubital tunnel syndrome is characteristically position-dependent: worse with sustained elbow bending and sometimes improving when the elbow is extended.
A pinched nerve in the neck causing hand numbness from C8 radiculopathy typically produces symptoms that are more constant and influenced by neck position. They often worsen with neck extension or rotation, rather than changes in arm position. This difference in symptom triggers is one of the most practical and useful distinctions during history-taking.
Muscle Weakness Patterns
C8 nerve root compression symptoms produce weakness in muscles not innervated by the ulnar nerve, specifically the thumb muscles: abductor pollicis brevis, flexor pollicis brevis, and opponens pollicis. These median-nerve-supplied muscles receive their root-level input from C8, so a cervical lesion weakens them while an elbow compression does not.
Elbow nerve compression symptoms from ulnar nerve entrapment produce intrinsic hand muscle weakness in the interossei and hypothenar muscles, causing finger abduction weakness and difficulty with fine motor tasks like separating the fingers against resistance. The flexor carpi ulnaris and the medial portion of the flexor digitorum profundus are also involved when compression is at the elbow rather than the wrist.
Dr. K. Daniel Riew, MD, Professor of Orthopedic Surgery at Weill Cornell Medicine and one of the world’s foremost cervical spine surgeons, co-authored a Global Spine Journal study testing 24 experienced cervical spine surgeons on their ability to distinguish C8 radiculopathy and ulnar neuropathy. Not one of the 24 correctly identified all the C8-innervated muscles affected by a cervical root lesion but not by elbow compression.
The study concluded this represents “inadequate knowledge regarding the clinical manifestations of C8-T1 radiculopathies and cubital tunnel syndrome” across even experienced practitioners.
Changes in Hand Appearance
Long-standing ulnar nerve entrapment can produce visible structural changes. Clawing of the ring and little fingers develops from the loss of intrinsic muscle balance between the interossei and the long finger flexors.
Intrinsic hand muscle weakness progressing to wasting, particularly in the first dorsal interosseous and the hypothenar eminence, signals advanced and prolonged compression. Finger abduction weakness is often measurable before visible wasting appears. These deformities are not typically seen in C8 radiculopathy alone, and their presence strongly suggests the elbow as the primary compression site.
Physical Tests Doctors Use to Differentiate the Two

Tinel’s Sign at the Elbow
Tapping directly over the cubital tunnel at the medial elbow that produces tingling into the ring and little fingers constitutes a positive Tinel’s sign, suggesting ulnar nerve entrapment at that site. It is among the most reliable and widely used bedside tests for cubital tunnel syndrome symptoms, though sensitivity and specificity vary with technique and the examiner’s experience.
Spurling’s Maneuver
Extension and lateral rotation of the neck toward the symptomatic side, combined with downward axial compression, reproduces radiating arm symptoms in cervical radiculopathy.
A positive Spurling’s maneuver points clearly toward a spinal source rather than a peripheral one, making it the most useful clinical test when C8 nerve root compression symptoms are suspected. Both tests can be performed at a single clinic visit and together help narrow the differential considerably before ordering electrodiagnostic testing.
Diagnostic Tests That Help Confirm the Cause
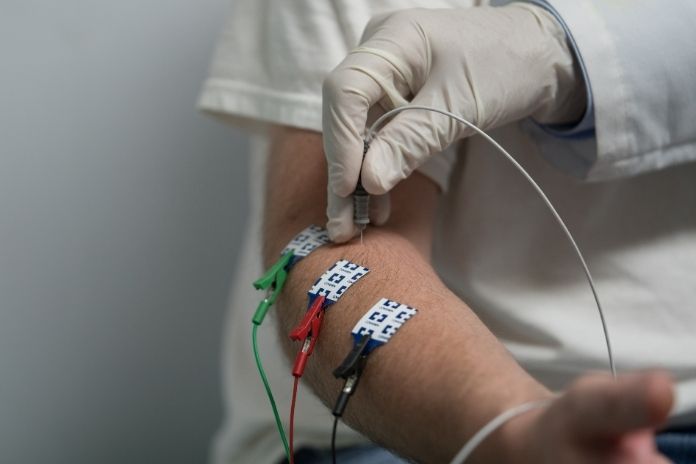
Nerve Conduction Studies and EMG
Nerve conduction studies (EMG/NCS) measure how efficiently electrical signals travel through the nerve at different points along its course. Slowing of conduction velocity across the elbow segment is the electrodiagnostic hallmark of cubital tunnel syndrome. Normal peripheral nerve conduction combined with abnormal findings in the cervical paraspinal muscles on needle EMG points toward cervical radiculopathy as the source.
The important limitation: nerve conduction studies (EMG/NCS) carry a clinically meaningful false-negative rate, particularly early in the disease course or in mild compression. Normal results do not rule out either C8 radiculopathy or ulnar neuropathy, and clinical judgment must inform how much weight to place on a negative study when symptoms are clearly present.
Imaging of the Cervical Spine or Elbow
MRI of the cervical spine is the preferred imaging study when C8 radiculopathy is suspected, identifying disc herniation, foraminal narrowing, or bone spurs at the C7-T1 level. Ultrasound of the elbow can detect ulnar nerve enlargement, flattening, or subluxation at the cubital tunnel, providing structural information that EMG alone cannot.
MRI of the brachial plexus is occasionally needed when neither the cervical spine nor the elbow clearly explains the full clinical picture, particularly in cases of combined or double-crush pathology.
Treatment Approaches Depend on the Source of Compression

Management of C8 Radiculopathy
Conservative management is first-line for most cases of C8 radiculopathy: physical therapy targeting cervical spine mechanics, posture correction, and activity modification to reduce axial loading on the neck. Anti-inflammatory medications address the inflammatory component of nerve root irritation.
Cervical epidural steroid injections are used when conservative measures provide insufficient relief. Surgical intervention, typically anterior cervical discectomy and fusion at C7-T1, is reserved for cases with persistent or progressive neurological deficits, including worsening intrinsic hand muscle weakness or finger abduction weakness that does not respond to conservative care.
Management of Ulnar Nerve Entrapment
The foundational behavioral change for ulnar nerve entrapment symptoms is avoiding prolonged elbow flexion. Night splints holding the elbow at approximately 45 degrees of extension eliminate the nocturnal compression that accumulates during sleep with bent arms. Ergonomic adjustments reduce sustained pressure on the medial elbow during desk work.
When conservative management fails or when elbow nerve compression symptoms have progressed to significant intrinsic hand muscle weakness or finger abduction weakness, surgical decompression or anterior transposition of the ulnar nerve at the elbow is indicated, with outcomes generally better when intervention comes before irreversible muscle wasting has developed.
Read More: Effective Home Remedies for Rheumatoid Arthritis (RA)
When Pinky Finger Numbness Should Not Be Ignored

Symptoms That Warrant Medical Evaluation
Numbness in the pinky finger lasting more than a few weeks, hand weakness affecting grip or fine motor tasks, visible intrinsic hand muscle weakness or wasting between the knuckles, and finger abduction weakness that affects daily function all warrant prompt evaluation.
Ulnar nerve numbness in the pinky finger that wakes you from sleep, or a pinched nerve in the neck causing hand numbness that changes with head position, are both patterns worth documenting and bringing to a physician rather than waiting to see if they resolve.
Dr. J. Michael Bennett, MD, a board-certified orthopedic and sports medicine surgeon based in Houston, is direct about the stakes of delayed evaluation: “You do not want to let that get out of control because these symptoms can become irreversible if you ignore them.
The muscle wasting can actually become irreversible,” he cautions, emphasizing that elbow nerve compression symptoms caught early respond far better to conservative management than those addressed after structural muscle changes have already set in.
Why Accurate Diagnosis Matters
Treating cubital tunnel syndrome when the actual problem is C8 radiculopathy, or vice versa, leaves the actual compression site unaddressed while potentially adding procedures that carry their own risks.
Nerve conduction studies (EMG/NCS) combined with clinical examination and appropriate imaging are what identify the correct level. Getting that right from the beginning is what makes treatment work.
Key Takeaway: Similar Symptoms, Different Causes
Numbness in the ring and little finger almost always reflects irritation somewhere along the ulnar nerve pathway. The challenge is that this pathway runs from the cervical spine to the hand, with significant compression sites at multiple points along its course.
C8 radiculopathy and ulnar neuropathy share nearly identical sensory symptoms in the hand but differ in their radiation pattern, the specific muscles weakened, and which clinical tests reproduce symptoms. Intrinsic hand muscle weakness and finger abduction weakness point toward the elbow.
Thumb muscle weakness and neck-to-arm radiation point toward the cervical spine. Nerve conduction studies (EMG/NCS) and imaging confirm the location. Treatment for each is fundamentally different, which is exactly why the distinction matters and why persistent pinky finger numbness deserves a thorough clinical workup rather than a reflexive assumption about the elbow.
References
- Bennett, J. M. (2023). How to treat cubital tunnel syndrome. OrthopedicSportsDoctor.com.
- Hopkins Medicine. (2024). Cubital tunnel syndrome. Johns Hopkins Medicine.
- Lattanza, L. (2024). Cubital tunnel syndrome. WebMD
- Stoker, G. E., Kim, H. J., & Riew, K. D. (2014). Differentiating C8-T1 radiculopathy from ulnar neuropathy: A survey of 24 spine surgeons. Global Spine Journal, 4(1), 1-6.
- American Academy of Orthopaedic Surgeons. (2023). Ulnar nerve entrapment at the elbow (cubital tunnel syndrome). OrthoInfo
- Tsao, B. E. (2010). Radiculopathy of the eighth cervical nerve. Journal of Orthopaedic & Sports Physical Therapy.
- Physio-Pedia. (n.d.). Cervical radiculopathy. Retrieved March 23, 2026, from
- Cleveland Clinic. (2022, March 29). Cervical radiculopathy (pinched nerve).
- Orthobullets. (n.d.). Cervical radiculopathy.
- Eubanks, J. D. (2010). Cervical radiculopathy: Nonoperative management of neck pain and radicular symptoms.
- Cervical Disc Institute. (n.d.). Cervical radiculopathy: Causes, symptoms, and treatment.
- Neurosurgeons of New Jersey. (n.d.). Cervical radiculopathy.
- H2 Health. (n.d.). Cervical radiculopathy: Symptoms, causes, and treatment.
- Radhakrishnan, K., et al. (1994). Epidemiology of cervical radiculopathy.
- American Academy of Orthopaedic Surgeons. (n.d.). Cervical radiculopathy (pinched nerve).
- Avant Orthopaedics. (n.d.). Symptoms, causes, and treatments for cervical radiculopathy.
In this Article