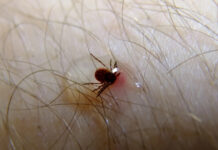
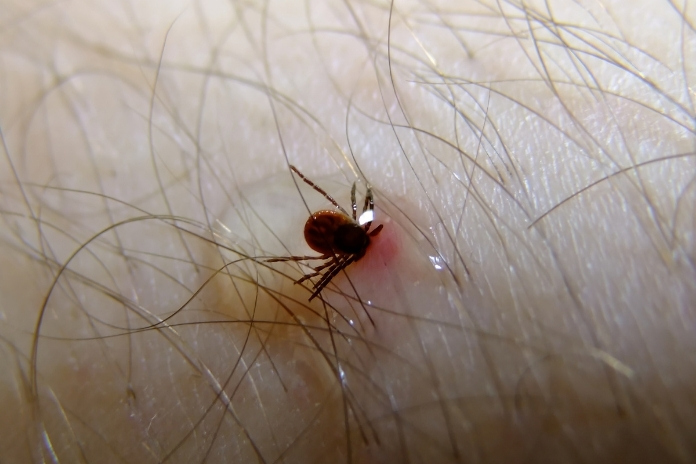
Tick bites are common in the United States, and most do not lead to serious illness. But some can transmit infections like Lyme disease or Rocky Mountain spotted fever if not handled correctly. Knowing how to identify a tick bite, remove the tick promptly, and watch for warning signs over the next several weeks greatly lowers the chance of complications.
What Is A Tick Bite And Why It Can Be Risky
Ticks are small, blood-feeding arachnids that grasp the skin with their mouthparts and stay attached for hours to days while they feed.
As they feed, infected ticks can pass bacteria, viruses, or parasites into the bloodstream, which is why they are an important source of tick-borne diseases in the United States.
Unlike many other insect bites, tick bites are often painless and may go unnoticed until the tick is seen or symptoms appear.
Risk of transmission generally increases the longer an infected tick remains attached, especially beyond about 24 to 36 hours for Lyme disease-carrying blacklegged (deer) ticks.
How To Identify A Tick Bite

A typical fresh tick bite appears as a small red bump or spot at the site where the tick is attached, sometimes with mild swelling or tenderness.
Common locations include the scalp, hairline, behind the ears, armpits, waistline, groin, and behind the knees, because ticks tend to crawl to warm, hidden areas before attaching.
Many people first notice the bite only after finding an attached tick or seeing a new bump after spending time in grassy, wooded, or brushy areas.
Because the bite itself is usually not painful or itchy at first, it is important to perform a full-body tick check after outdoor activities in tick-heavy regions.
How to do a proper tick check:
After coming indoors, check your entire body systematically, starting at your feet and working upward. Use a hand mirror or full-length mirror to check behind your knees, between your legs, around your waist, and up your back.
Have someone help you check your scalp and hairline. Check children’s hair, behind their ears, and around the neckline. Don’t forget to check your pets and gear, and put outdoor clothing in the dryer on high heat for at least 10 minutes to kill any ticks that haven’t attached.
Showering within two hours of coming indoors also reduces risk.
Read More: Understanding Frostbite: Symptoms, Prevention, and Effective Treatment
Tick Bite Symptoms To Watch For
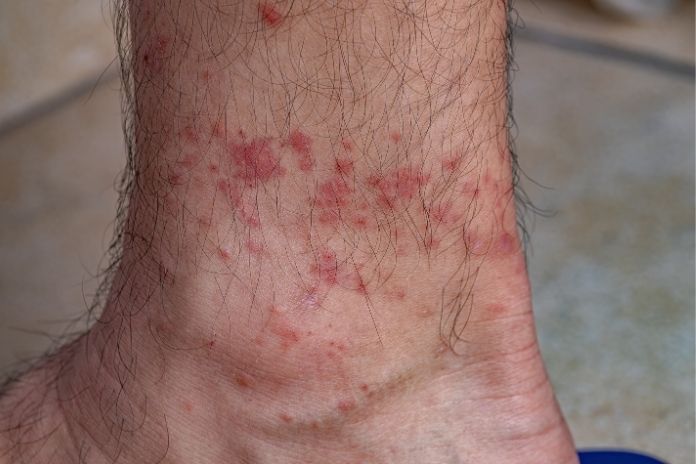
Normal Reaction After A Tick Bite
Many tick bites cause only a mild local reaction. A small, firm bump with limited redness, often less than 1 to 2 inches across, along with slight itching or tenderness that does not spread over 24 to 48 hours, is usually a normal response to the bite rather than a sign of infection.
This type of reaction may last several days before slowly fading.
Mild tick bite itching around the bite can occur, but intense or spreading redness, drainage, or increasing pain may indicate local skin infection rather than a simple bite reaction.
If the site becomes very swollen, warm, or starts to ooze, medical evaluation is recommended.
Symptoms That May Signal Infection Or Disease
After a tick bite, more concerning symptoms can appear days to weeks later, especially if a tick-borne infection was transmitted. Watch for these warning signs:
- Expanding rash:A rash that continues to grow beyond the initial bite area.
- Flu-like illness (within 3 to 30 days):Fever, chills, fatigue, headache, neck stiffness, and muscle or joint pain.
- Night sweats or general malaise that mimic viral infections.
- Severe or alarming symptoms:
- Shortness of breath
- Confusion or disorientation
- New weakness in limbs
- Intense stomach pain
These symptoms may indicate serious conditions such as Rocky Mountain spotted fever or ehrlichiosis, and they require immediate medical attention.
Anyone experiencing these signs after tick exposure should contact a healthcare provider promptly, even if the tick was removed days earlier.
Read More: 12 Miraculous Remedies For Shoe Bites That Work Wonders
Tick Bite Rash – What Is Normal And What Is Not
A small, non-spreading area of redness at the bite site is commonly due to local irritation and does not necessarily mean infection. This type of rash tends to stay the same size or shrink over 1 to 2 days, and may feel warm or slightly tender, but does not cause systemic symptoms.
In contrast, the classic Lyme disease rash, called the bullseye rash (erythema migrans), typically appears 3 to 30 days after a bite as an expanding red area that can reach several inches across and sometimes clears in the center, creating a target-like appearance.
However, Lyme rashes do not always look like perfect targets. They may be uniformly red, darker at the center, or appear in multiple areas of the body. Any enlarging red patch after a tick bite warrants medical attention.
Here is the content from the image converted into the requested HTML format, maintaining the structure and CSS classes of your template.
“`html
Rash Patterns From Different Tick-Borne Diseases
| Condition | Typical Rash Features | Approximate Onset After Bite |
|---|---|---|
| Lyme disease | Single or multiple expanding red patches; may resemble a bullseye but can be uniformly red. | Usually 3–30 days |
| Rocky Mountain spotted fever | Small pink spots on wrists and ankles that can spread to trunk, palms, and soles; may be absent early on. | Often 3–12 days |
| Ehrlichiosis/Anaplasmosis | Rash is less common and may be faint or absent; flu-like symptoms often dominate. | Typically 5–14 days |
“`
What To Do Immediately After A Tick Bite

How To Remove A Tick Safely
Removing the tick as soon as possible reduces the risk of tick-borne infection, especially Lyme disease. Use fine-tipped tweezers to grasp the tick as close to the skin surface as possible, then pull upward with steady, even pressure until the tick releases. Do not twist, jerk, or crush the body, as this can leave mouthparts in the skin or squeeze infectious material into the bite.
After removal, inspect the area to confirm no visible parts remain embedded. If small fragments are left and cannot be easily removed, the skin often pushes them out over time. Worsening redness or pain, however, should be checked by a clinician.
Common tick removal mistakes to avoid:
In addition to burning the tick or smothering it with petroleum jelly, Americans often try twisting the tick out while pulling, squeezing the tick’s body with their fingers, using essential oils or nail polish to suffocate the tick, or simply yanking quickly with fingernails.
All of these methods can increase the risk of the tick releasing infectious material into the skin or leaving mouthparts behind. The only recommended technique is a slow, steady, upward pull with fine-tipped tweezers, grasped as close to the skin surface as possible.
How To Clean And Care For The Bite Area
Once the tick is removed, wash the bite site and your hands thoroughly with soap and water. After cleaning, apply rubbing alcohol or another antiseptic to the skin and allow it to dry. Consider a simple bandage if the area is irritated or likely to rub against clothing.
Over the next day or two, monitor the site for increasing redness, warmth, swelling, or pus. These signs may suggest local infection and should be evaluated by a healthcare professional.
Many experts also recommend noting the date of the bite and, if possible, how long the tick was attached to help guide later treatment decisions.
Should You Save The Tick For Testing
Saving the tick in a sealed container or plastic bag, ideally with the date and location of the bite, can help identify the species and estimate the risk of certain infections, such as Lyme disease from blacklegged (deer) ticks.
Some labs and local health departments offer tick identification or pathogen testing, which may provide additional information about potential exposures.
However, tick testing has limitations: a positive result does not guarantee that you were infected, and a negative result cannot completely rule out disease, especially if you were bitten by more than one tick or misidentified the species.
Because of these uncertainties, clinicians place more weight on your symptoms, physical exam, and local disease patterns than on tick test results when deciding on treatment.
Disease You Can Get From A Tick Bite
In the United States, ticks can transmit several important infections, and the specific risk varies by tick species and region.
Blacklegged (deer tick) ticks in the Northeast, Mid-Atlantic, and upper Midwest commonly transmit Lyme disease and can also spread anaplasmosis and babesiosis. Lone star ticks in the Southeast and parts of the Midwest may transmit ehrlichiosis.
American dog ticks and Rocky Mountain wood ticks can carry the bacteria that cause Rocky Mountain spotted fever, a potentially life-threatening illness if not treated early.
Geography plays a key role: knowing whether you live in or have visited an area where these infections are common helps clinicians assess your risk and decide whether to test or prescribe antibiotics.
Alpha-gal syndrome (red meat allergy): One lesser-known but increasingly recognized consequence of a tick bite is alpha-gal syndrome (AGS). Primarily associated with lone star tick bites, AGS causes a delayed allergic reaction, typically appearing 2 to 6 hours after eating red meat, dairy, or other mammalian products. Reactions range from hives and stomach pain to, in serious cases, anaphylaxis.
The CDC estimates that as many as 450,000 Americans may be affected, and cases are most common in the South, Southeast, and Central states, where Lone Star ticks are most prevalent. If you develop unexplained allergic reactions after meals following a tick bite, speak with an allergist about testing for alpha-gal antibodies.
Tick paralysis: A separate, non-infectious complication of tick bites is tick paralysis. Caused by a neurotoxin in the saliva of certain attached ticks, it can produce progressive muscle weakness that starts in the legs and may move upward, sometimes resembling Guillain-Barré syndrome or botulism.
Symptoms typically resolve within 24 hours of removing the tick. It is rare but more commonly reported in children. If you or your child develops unexplained weakness or difficulty walking after spending time outdoors in tick-prone areas, seek medical care promptly and perform a thorough tick check
Read More: Say Goodbye to Chigger Bites: 13 Natural Remedies That Work
When To See A Doctor After A Tick Bite

Seek medical care urgently on the same day, or go to the emergency room, if you develop a high fever, severe headache, stiff neck, confusion, difficulty breathing, chest pain, or a rapidly spreading or bruise-like rash after a tick bite. These can signal serious tick-borne illness.
Immediate evaluation is also important for children, pregnant people, older adults, and anyone with a weakened immune system who develops symptoms after a bite.
Pregnancy and tick bites:
Pregnant women who are bitten should contact their healthcare provider even without symptoms, as some tick-borne diseases, including Lyme disease and Rocky Mountain spotted fever, can carry risks to fetal health if untreated.
Doxycycline, the standard antibiotic for many tick-borne infections, is generally avoided during pregnancy, so early contact with your doctor allows time to discuss alternative treatment options, such as amoxicillin for Lyme disease prophylaxis when appropriate.
Children and tick bites: Children are at high risk for tick bites because they spend more time playing outdoors in grassy or wooded areas. Parents should check their children’s hair, scalp, behind the ears, and around the neckline after any outdoor activity.
Tick-borne diseases like Lyme disease and Rocky Mountain spotted fever can progress quickly in children and may present with slightly different features, including a rash that is easy to miss on darker skin.
If a child develops a fever, refuses to walk, has a stiff neck, or seems unusually tired in the weeks after a possible tick exposure, see a doctor promptly.
Doxycycline is safe and approved for treating tick-borne disease in children of all ages, including those under 8, at appropriate doses for short courses.
Even without severe symptoms, it is wise to contact a doctor if a tick was attached for at least 24 to 36 hours in an area where Lyme disease is common, if you notice an expanding rash, or if you feel unexplained flu-like illness within a month of the bite.
Clinicians may recommend preventive antibiotics for certain high-risk bites or arrange follow-up to monitor for evolving symptoms.
Tick Bite Treatment: What Actually
For high-risk bites from identified blacklegged ticks in Lyme-endemic areas, many U.S. guidelines recommend a single dose of doxycycline within 72 hours of tick removal to reduce the chance of Lyme disease.
A bite is considered high risk when the tick is clearly an Ixodes species, the area has significant Lyme activity, and attachment lasted at least about 36 hours.
Not everyone with a tick bite needs antibiotics. For lower-risk exposures, clinicians often recommend close observation instead, since unnecessary antibiotics can cause side effects and contribute to resistance.
If you later develop a compatible rash or symptoms, your doctor may prescribe a full course of antibiotics tailored to the suspected infection, rather than a single preventive dose.
Over-the-counter pain relievers and antihistamines can ease mild discomfort or itching at the bite site, but they do not prevent infection and should not replace medical evaluation when symptoms appear. Always follow package directions or your clinician’s advice when using any medication.
How Long Can Tick Bite Symptoms Take To Appear
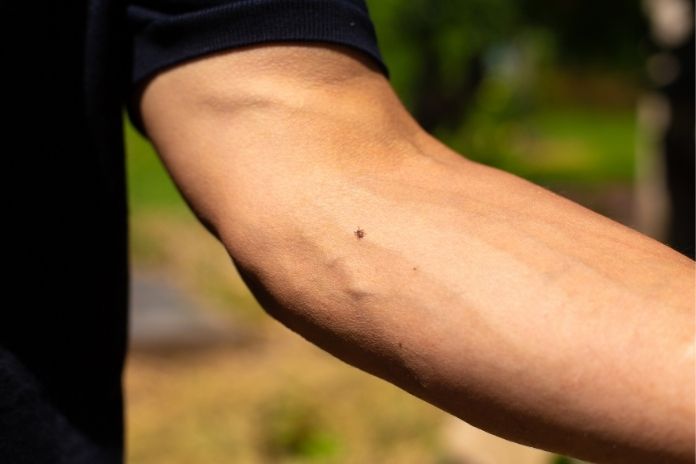
Some reactions to a tick bite, such as localized redness and mild irritation, appear within hours to a day. Infections, however, often develop more slowly. Tick bite symptoms for Lyme disease typically start 3 to 30 days after a bite, while illnesses like Rocky Mountain spotted fever, ehrlichiosis, or anaplasmosis often present within about 3 to 14 days.
Because of this timing, many experts recommend monitoring your health and the bite site for about 30 days after any tick bite, especially if you live in or have visited an area where tick-borne diseases are common.
Keep a note of the bite date, the location on your body, and any evolving rash or symptoms, and share this information with your healthcare provider if you need evaluation.
Tick season timing: Ticks are active year-round in many parts of the United States, but the highest risk period is typically late spring through early fall, with peak activity in May, June, and July.
The CDC’s Tick Bite Data Tracker allows you to check local tick bite trends in your region. Even in winter, deer ticks remain active when temperatures are above freezing, so tick awareness is not just a summer concern.]
Read More: 10 Best Known Home Remedies For Mosquito Bites
How To Prevent Tick Bites In The Future
Spending time outdoors doesn’t have to lead to tick bites. The key is a layered prevention strategy combining protective clothing, repellents, regular tick checks, and yard care. These practical steps make a big difference in lowering your exposure risk.
- Wear long sleeves and long pants tucked into socks when in grassy or wooded areas.
- Choose light-colored clothing to more easily spot ticks before they attach.
- Apply anEPA-registered insect repellent with DEET, picaridin, or IR3535 to exposed skin.
- Treat clothing, shoes, and gear with permethrin for added protection.
- After spending time outdoors, check your entire body for ticks, especially the scalp, behind the ears, armpits, waist, groin, and behind the knees.
- Shower within two hours of coming indoors to wash off any ticks that haven’t attached yet.
- Keep youryard tick-safe by mowing grass short, removing leaf litter, and placing gravel or woodchip barriers between lawns and wooded areas.
- Use veterinarian-recommended tick control products for pets to prevent them from bringing ticks indoors.
Key Takeaways
- Not Every Tick Bite Leads to Disease:Many bites cause only mild local irritation, but some can transmit serious infections depending on tick type, how long it was attached, and where you live.
- Early Action and Monitoring Reduce Risk:Prompt, proper tick removal, cleaning the bite, and watching for rash or flu-like tick bite symptoms over the next 30 days greatly lowers the chance of complications.
- Know When to Seek Medical Care:Contact a doctor urgently for high fever, spreading or bruise-like rash, severe headache, breathing problems, confusion, or if a deer tick was attached for at least 24 to 36 hours in a Lyme-endemic area. Tick bite treatment is most effective when started early.
References
- Centers for Disease Control and Prevention. (n.d.). Tick bite: What to do.
- Centers for Disease Control and Prevention. (n.d.). Guidance for clinicians: Caring for patients after a tick bite.
- Mayo Clinic. (2024, March 14). Tick bites: First aid.
- Cleveland Clinic. (2025, November 18). Tick bites: Causes, symptoms, treatment & prevention.
- Stone, B. F., & Borsa, M. (2020). Emerging tick-borne diseases. PMC – PubMed Central.
- Nadelman, R. B., et al. (2021). Antibiotic prophylaxis for prevention against Lyme disease following a tick bite. PMC – PubMed Central.
- Lantos, P. M., et al. (2024). Lyme disease prophylaxis by single-dose doxycycline in the emergency department. Open Forum Infectious Diseases.
- U.S. Food and Drug Administration. (2024, July 17). Ticks and Lyme disease: Symptoms, treatment, and prevention.
- U.S. Department of Health and Human Services. (2024). Tick-borne diseases and associated illnesses.
- Centers for Disease Control and Prevention. (2024, June 2). Babesiosis.
- Cleveland Clinic. (2025, November 17). Babesiosis: Causes, symptoms, diagnosis & treatment.
- Centers for Disease Control and Prevention. (n.d.). Clinical signs and symptoms of anaplasmosis.
- Province of Manitoba. (2021, May 19). Anaplasmosis.
- Wikipedia contributors. (2024). Tick paralysis.
- ScienceDirect. (2007). Tick paralysis.
- U.S. Environmental Protection Agency. (2025, December 29). Repellents: Protection against mosquitoes, ticks and other arthropods.
- National Pest Management Association. (2023, November 5). How to safely & easily remove a tick.
- World Health Organization. (2024, September 25). Vector-borne diseases.
- World Health Organization. (2019, November 5). Tick-borne encephalitis.
- Infectious Diseases Society of America. (2020, November 29). Lyme disease.
In this Article