- The average diagnostic delay for endometriosis is about 6.8 years, and in some regions it can reach 11.4 years because severe period pain is often dismissed as normal.
- Pain intensity does not reflect disease stage. Mild endometriosis can cause severe pain, while advanced disease may sometimes cause little pain.
- If two or more key symptoms occur consistently, the pain should be medically evaluated rather than dismissed as normal menstrual discomfort..
For generations, women have been told that painful periods are simply part of being a woman. Take an ibuprofen. Use a heating pad. Don’t complain. That cultural script has cost millions of women years of their lives.
A 2024 scoping review published in Health Care for Women International, drawing on studies across four databases covering the period from inception to September 2023, found that the average endometriosis diagnosis delay across studies was 6.8 years, with some countries reporting delays as long as 11.4 years.
Across that entire period, most women had already consulted multiple doctors. Their period cramps and endometriosis pelvic pain were repeatedly minimized. Endometriosis symptoms occur when endometrial tissue, similar to the uterine lining, grows outside the uterus, triggering inflammation, scar tissue formation, and pain that does not behave like normal period cramps.
It is not a new condition, not a rare one, and not one that medicine lacks the vocabulary to identify. What it lacks is the clinical will to take women’s pain seriously.
These are the five endometriosis warning signs that distinguish endometriosis from typical menstrual discomfort, sourced directly from OB-GYNs at Johns Hopkins, Yale, and Loma Linda University Health.
The most important thing to understand before you read the signs: pain severity alone does not determine endometriosis stage. Mild disease can cause severe pain, and advanced disease can sometimes cause none at all.
What is endometriosis? Endometriosis affects an estimated 190 million women of reproductive age worldwide. It occurs when endometrial tissue similar to the uterine lining grows outside the uterus, causing inflammation, scar tissue formation, chronic pelvic pain, heavy bleeding, and, in some cases, infertility. There is currently no cure.
Read More: What Endometriosis Pain Feels Like (And Why It’s Often Misdiagnosed)
Sign 1: Your Pain Is Debilitating, Not Just Uncomfortable

Period cramps and endometriosis presentations are not interchangeable. There is a documented clinical threshold between discomfort and disease, and too many women are being told their pain sits on the normal side of that line when the evidence says otherwise.
Dr. Khara Simpson, MD, draws the clinical line clearly: “Mild discomfort with periods may be normal, but pain that stops a woman from working or going to school or other daily activities is not normal and should be evaluated by a gynecologist.”
The clinical distinction matters. Normal painful periods typically begin one to two days before flow, respond to over-the-counter pain relief, and resolve within 24 to 72 hours. Period cramps: Endometriosis patients describe something categorically different: pain notably worse than typical menstrual cramps, lasting longer, and frequently resisting ibuprofen and other OTC medications.
That painkiller resistance pattern is one of the clearest endometriosis warning signs in the clinical presentation.
“With pain in any other region of the body, doctors immediately investigate to find out what’s wrong; however, this is the only pain that the medical community considers ‘normal.’ Pain with menses is far too frequently dismissed,” says Dr. Hugh Taylor, MD.
Sign 2: Your Pain Exists Outside Your Period

Endometriosis pelvic pain does not confine itself to the days of active bleeding. Cyclical pain that begins a week or more before flow starts, or chronic pelvic pain at other points in the cycle, are patterns that point away from primary dysmenorrhea and toward an underlying lesion-driven process.
If you experience pelvic pain consistently outside of menstruation, endometriosis symptoms should be seriously considered. Johns Hopkins identifies chronic pelvic pain, severe and persistent discomfort even when no period is occurring, as one of the five hallmark endometriosis warning signs, often associated with advanced disease and internal scarring.
A 2021 review published in Cell Press confirmed that cyclical pain can begin earlier in the menstrual cycle, last longer than normal painful periods, and become constant in some women, entirely independent of whether bleeding is occurring.
The clinical distinction is straightforward. Normal cramping is tied to menstruation and resolves when the flow ends. Endometriosis patients describe pain that starts well before a period begins, extends long past its end, and in advanced stages becomes a daily presence that bears no reliable relationship to the menstrual calendar at all.
That progression, from painful periods to persistent chronic pelvic pain, is one of the most important endometriosis symptoms to document and report.
Sign 3: Sex Is Painful, Especially Deep Penetration

Endometriosis and painful sex are one of the most underreported symptom combinations, not because they are uncommon, but because they are the symptoms women feel most reluctant to raise with a doctor.
It is worth being direct: if you experience deep pelvic pain during or after intercourse, tell your gynecologist. It is not embarrassing. It is a clinical data point that belongs in the conversation about your endometriosis symptoms.
Dyspareunia affects more than 50% of women with confirmed endometriosis. Endometrial tissue lesions can develop on the ovaries, vagina, bladder, and colon, making deep internal pain during penetration, along with pain during urination or bowel movements, a clinically significant pattern.
A review in ScienceDirect examining dyspareunia in women with confirmed endometriosis found that deep dyspareunia, pain felt internally rather than superficially, is one of the most diagnostically consistent features of posterior compartment endometriosis and a primary endometriosis warning sign warranting urgent investigation.
The clinical distinction: occasional mild discomfort during sex relating to positioning or dryness is not independently significant. Endometriosis and painful sex present as deep, internal, consistent, and worsening over time. It is not positional or situational. When this pattern accompanies other endometriosis symptoms on this list, gynecological investigation should not be delayed.
Sign 4: Your Gut Gets Involved Around Your Period

Endometriosis and bowel symptoms represent one of the most diagnostically misdirected presentations in women’s health. When endometrial tissue develops on the digestive or urinary tracts, the result is gastrointestinal and urinary symptoms that track the menstrual cycle: diarrhea, constipation, nausea, painful bowel movements, painful urination, and, in some cases, blood in the urine or stool.
These endometriosis symptoms are not random. They are cyclical pain expressions, and their timing is the diagnostic clue most frequently missed.
A Frontiers in Endocrinology review of endometriosis and bowel symptoms confirmed that bowel endometriosis is systematically underidentified in non-gynecological clinical pathways, compounding endometriosis diagnosis delays significantly. The clinical distinction: mild nausea or loose stools accompanying menstruation are not independently concerning.
Endometriosis and bowel symptoms that appear or worsen specifically around your period, particularly when accompanied by endometriosis pelvic pain, point toward a gynecological origin and belong in a conversation with an OB-GYN, not a gastroenterologist.
Read More: Diet for Endometriosis: Foods That Help and Foods to Avoid
Sign 5: You Have Heavy or Prolonged Bleeding

Endometriosis and heavy bleeding frequently occur together. Menorrhagia, the clinical term for abnormally heavy menstrual bleeding, is a common presentation of endometriosis symptoms because the abnormally located endometrial tissue builds up each month but has no adequate exit pathway.
This excessive blood loss can cause iron-deficiency anemia, fatigue, dizziness, and shortness of breath, symptoms frequently attributed to other causes rather than the underlying gynecological disease driving them.
A 2021 review published in PubMed Central examining endometriosis and heavy bleeding in endometriosis cohorts found that menorrhagia alongside endometriosis pelvic pain represents a combination that specifically elevates clinical suspicion for endometriosis.
Neither symptom alone is diagnostic, but together they represent a meaningful pattern that contributes directly to narrowing the endometriosis diagnosis delay. The clinical distinction: losing up to 80 ml of blood per cycle over a period lasting 2 to 7 days is within the normal range.
Endometriosis and heavy bleeding look different: soaking through protection in under an hour, passing large clots consistently, periods lasting longer than 7 days, or bleeding between cycles. Any of these endometriosis warning signs, particularly alongside endometriosis pelvic pain, warrants immediate evaluation.
Why Diagnosis Takes So Long, And Why That Matters
In the UK, 58% of women reported making multiple visits to their care provider before any investigations for endometriosis symptoms were undertaken, with an average global endometriosis diagnosis delay of 7 to 9 years. More than two-thirds of women in the USA report missing school or work as a direct result of undiagnosed or undertreated painful periods, or endometriosis.
The delay is not a quirk of individual clinical judgment. It is a structural, documented failure. The racial dimension compounds it. Black and Hispanic women face barriers to endometriosis diagnosis that extend well beyond the normalization of period cramps.
Dr. Soyini Hawkins, MD, MPH, FACOG, states the disparity plainly: “On average, a diagnosis of endometriosis takes 7 to 10 years. In Black and Hispanic women, it could take twice as long. There’s definitely a disparity on the front end of getting the diagnosis,” she told AJMC.
A later endometriosis diagnosis means more advanced lesions, more scar tissue, more complex surgery, and a higher risk of fertility complications by the time anyone intervenes.
A systematic review and meta-analysis by Bougie et al. examining 18 studies on endometriosis diagnosis across racial and ethnic groups found that Black women were approximately 51% less likely to receive a diagnosis than White women, a disparity rooted in both systemic access barriers and documented racial bias in pain assessment by clinicians.
How Endometriosis Is Actually Diagnosed
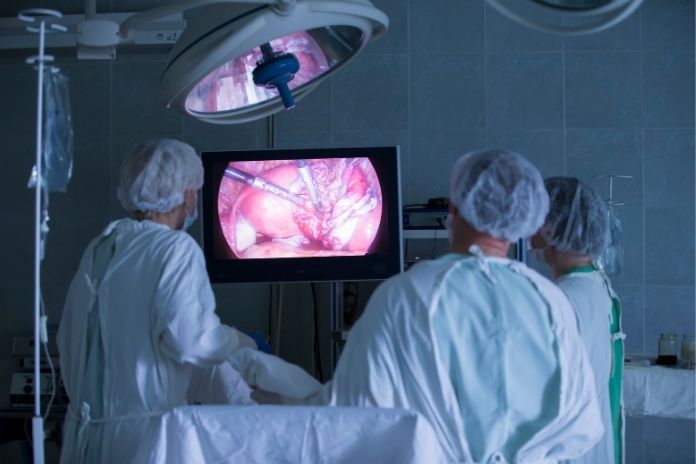
Routine ultrasounds frequently fail to detect endometriosis symptoms unless ovarian cysts are present. The only confirmed diagnostic method is laparoscopy, a minimally invasive surgical procedure performed under general anesthetic that allows direct visualization and biopsy of endometrial tissue lesions outside the uterus.
A clinical diagnosis can be made based on symptom history and MRI in some cases, but laparoscopy remains the gold standard. Laparoscopy is typically a same-day procedure and, when endometriosis is found, can also be used to remove accessible lesions in the same operation.
The prospect of surgical investigation should not delay a referral that is clinically warranted by the endometriosis warning signs above.
Read More: Endometriosis-Symptoms, Causes, Prevention and Treatment
Conclusion: When to See a Doctor
If you recognize two or more of these endometriosis warning signs consistently, your pain deserves medical investigation, not reassurance.
See a gynecologist if you have painful periods or endometriosis patterns, particularly when accompanied by endometriosis and painful sex, endometriosis and bowel symptoms, dyspareunia, menorrhagia, or chronic pelvic pain that persists outside your cycle.
You know your body better than anyone in that consulting room. Persistent endometriosis pelvic pain that disrupts your work, relationships, and quality of life is a signal worth pursuing. The five endometriosis symptoms above are not a checklist for self-diagnosis. They are a framework for a conversation you deserve to have with a doctor who takes the information seriously.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. If you are experiencing the symptoms described, please consult a qualified gynecologist or women’s health specialist.
Frequently Asked Questions
1. What are the most common endometriosis warning signs to look out for?
The five key endometriosis warning signs are debilitating period cramps, chronic pelvic pain between cycles, endometriosis and painful sex, endometriosis and bowel symptoms timed to your cycle, and endometriosis and heavy bleeding.
These endometriosis symptoms rarely appear in isolation, and if two or more apply to you consistently, see a gynecologist rather than waiting for the pain to worsen.
2. How long does an endometriosis diagnosis delay usually take, and why?
The average endometriosis diagnosis delay is 6.8 years globally, primarily because painful periods and endometriosis presentations are routinely dismissed as normal by clinicians. Women with endometriosis and bowel symptoms face additional delays by being sent to gastroenterologists before anyone considers the OB-GYN pathway.
Tracking your endometriosis symptoms as a pattern rather than isolated complaints can meaningfully shorten your personal diagnostic timeline.
3. Is painful sex always a sign of endometriosis?
Not always, but endometriosis and painful sex, specifically deep internal dyspareunia rather than superficial discomfort, are some of the most diagnostically significant endometriosis warning signs a gynecologist can evaluate.
Over 50% of women with confirmed endometriosis report dyspareunia, making it far more than an incidental complaint. Disclose it directly to your doctor, especially alongside other endometriosis symptoms.
4. What is the difference between normal period cramps and period cramps that endometriosis patients experience?
Normal painful periods respond to over-the-counter pain relief and resolve within 24 to 72 hours without disrupting daily function. Endometriosis patients describe pain that resists ibuprofen, extends beyond the period as chronic pelvic pain, and forces them to miss work or daily activities.
That painkiller resistance combined with functional disruption is the clearest line between normal cramps and endometriosis symptoms requiring evaluation.
5. How is endometriosis actually confirmed, and what does laparoscopy involve?
Endometriosis diagnosis is confirmed through laparoscopy, a minimally invasive, same-day surgical procedure that allows direct visualization of endometrial tissue lesions and can remove them in the same operation.
Routine ultrasounds frequently miss endometriosis symptoms unless ovarian cysts are present. If scans come back clear but endometriosis, pelvic pain, and heavy bleeding persist, a referral for laparoscopy remains clinically warranted.
References
- Bougie, O., Yap, M. I., Sikora, L., Flaxman, T., Singh, S., & Chen, I. (2019). Influence of race/ethnicity on prevalence and presentation of endometriosis: a systematic review and meta-analysis. BJOG.
- Fryer, J., Mason-Jones, A. J., & Woodward, A. (2024). Understanding diagnostic delay for endometriosis: A scoping review. Health Care for Women International.
- Gonzalez, R. (2023). Menstrual cramps or endometriosis? Loma Linda University Health News.
- Hawkins, S. (2023). Racial disparities associated with endometriosis diagnosis. AJMC.
- Simpson, K. (2024). Period pain: Could it be endometriosis? Johns Hopkins Medicine.
- Taylor, H. (2024). Endometriosis is more than just ‘painful periods.’ Yale Medicine.
- Vercellini, P. et al. (2014). Endometriosis: Pathogenesis and treatment. Referenced in PMC heavy menstrual bleeding review.
- WHO. (2023). Endometriosis: Key facts. Referenced in ScienceAlert.
- Cleveland Clinic. (n.d.). Dyspareunia (painful intercourse).
- Flo Health. (n.d.). Painful sex: Symptoms, causes and treatment.
- Healthdirect Australia. (n.d.). Post-menopause.
- Mayo Clinic. (2024, February 16). Painful intercourse (dyspareunia): Symptoms and causes.
- MedicineNet. (n.d.). Why am I having menstrual cramps but no period?
- National Center for Biotechnology Information. (n.d.). Dyspareunia.
- Tender Palm Hospital. (n.d.). Painful intercourse (dyspareunia) treatment in Lucknow, India.
- World Health Organization. (n.d.). Endometriosis.
In this Article