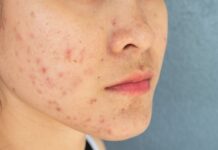
- Running helps improve mood hormones and gut health, even with a poor diet
- Junk food limits benefits; it lowers BDNF and blocks full brain repair from exercise
- Diet and exercise together give the best results for brain and mood health.
A study published in Brain Medicine in October 2025 by researchers at University College Cork offers some of the clearest evidence yet that exercise and brain health are linked through specific, measurable biological pathways.
Running largely undoes the mood-related damage a junk food diet causes. But the study contains a finding that barely made it into any news coverage, and it changes the picture considerably. A Western diet does not just damage the brain. It actively blocks the brain-repair benefit that running normally delivers.
In this article, we examine the science behind how a Western diet affects the brain, how running helps repair that damage, and the biological mechanisms linking the gut and brain. It also explores why diet and exercise interact through BDNF, what the study’s key limitations are, and what the findings mean in practical terms.
Read More: Why You Can’t Stop Craving Junk Food — Your Gut Bacteria May Be to Blame
The Study: Rats, Running Wheels, and a Diet That Looks Familiar

The research was led by Professor Yvonne Nolan at APC Microbiome Ireland, University College Cork, and published in Brain Medicine in October 2025. Four groups of adult male rats were studied: healthy diet plus sedentary, healthy diet plus running, cafeteria diet plus sedentary, and cafeteria diet plus running.
The cafeteria diet, a standard research model for Western dietary patterns, included processed, high-fat, high-sugar foods designed to mirror what a large portion of the human population eats daily. Exercise was voluntary wheel running rather than forced treadmill use, a design choice that more closely resembles self-directed human activity.
The researchers measured 175 gut metabolites across all groups using untargeted metabolomics. In sedentary cafeteria-fed animals, 100 of those 175 metabolites, 57% of the entire profile, were disrupted. That breadth establishes how comprehensively a poor diet reshapes the gut environment before any downstream brain effects are considered.
What a Western Diet Actually Does to Your Brain
Three specific metabolites dropped significantly in cafeteria-fed sedentary animals. Anserine is an anti-inflammatory dipeptide with emerging neuroprotective evidence. Indole-3-carboxylate is a tryptophan metabolite sitting in the serotonin precursor pathway that also supports gut barrier function. Deoxyinosine is a nucleoside involved in managing cellular stress.
All three fell with the cafeteria diet and were partly restored by exercise. Two further metabolites, aminoadipic acid and 5-HIAA, were linked to worse cognitive performance. Insulin and leptin both spiked in sedentary cafeteria-fed animals, and when chronically elevated, both hormones impair the signaling cascades the brain uses to maintain synaptic plasticity.
The Deeper Mechanism: What Junk Food Does to BDNF
Brain-derived neurotrophic factor, BDNF, supports neuron survival, synaptic plasticity, and the generation of new neurons. It is most active in the hippocampus, the region central to memory, learning, and mood. A high-fat, high-sugar diet reduces hippocampal BDNF. The neurotrophic hypothesis of depression identifies hippocampal BDNF depletion as a core mechanism of major depressive illness.
A foundational review in Nature Reviews Neuroscience found that junk food, characterized by high saturated fat and sucrose, produced a decline in cognitive performance and reduced hippocampal BDNF-related synaptic plasticity after only three weeks of dietary exposure in rodent models. The cafeteria diet was depleting the molecular signal the hippocampus depends on to build and maintain itself.
Read More: How to Stop Eating Junk Food: 18 Evidence-Based Strategies for Healthier Living
How Running Repairs the Damage: Three Pathways

Exercise partially restored all three mood-associated metabolites. Anserine, indole-3-carboxylate, and deoxyinosine all recovered toward healthier levels in running animals, suggesting the gut-brain axis responds to physical activity even under dietary stress. Running also sharply reduced the insulin and leptin spikes, removing a key suppressor of BDNF signaling.
One hormonal finding stood out. Peptide YY, a gut hormone involved in appetite and metabolic signaling, increased with exercise only in cafeteria-diet animals. It did not change in healthy-diet runners. The researchers interpreted this as a compensatory response: the body correcting for dietary disruption in a way that healthy animals did not require.
Exercise also reduced anxiety across all groups regardless of diet, indicating some of running’s mental health benefits operate through pathways at least partly independent of diet quality.
The Surprising Finding: Junk Food Blocks Exercise’s Brain-Building Benefit
In healthy-diet animals, running boosted hippocampal neurogenesis, the generation of new neurons in the brain’s memory and mood center. This is one of the most replicated findings in exercise neuroscience.
In cafeteria-diet animals, the same exercise produced a significantly blunted neurogenic response. The running happened. The effort was equivalent. The neurogenesis was not. The mechanism runs through BDNF. The cafeteria diet had depleted hippocampal BDNF to the point where the brain could not fully receive exercise’s neurogenic signal.
During aerobic exercise, the body produces a ketone called beta-hydroxybutyrate. It crosses the blood-brain barrier and epigenetically upregulates the BDNF gene, triggering neurogenesis. But that process requires adequate BDNF sensitivity at baseline. A brain chronically depleted by a poor diet is less responsive to the signal when it arrives.
Running partially repairs junk food’s damage through gut metabolite restoration, hormonal normalization, and anxiety reduction. But the deepest repair mechanism, building new neurons, is impaired when the diet continues to work against it. Diet and exercise are not alternatives. They are multipliers, and their interaction is nowhere more visible than in the hippocampus.
BDNF: The Molecule That Explains Why Both Diet and Exercise Matter
BDNF governs neuron survival, synaptic connection formation, and neurogenesis throughout adult life. Dr. Jennifer Heisz, PhD, explains the mechanism: “One key thing that exercise increases is brain-derived neurotrophic factor. This acts as a fertilizer to grow new brain cells and help our existing brain cells function optimally.”
Exercise increases hippocampal BDNF by up to three times baseline through beta-hydroxybutyrate, which crosses the blood-brain barrier and epigenetically activates the BDNF gene. A high-fat, high-sugar diet suppresses that same system.
A foundational 2004 study by Molteni and colleagues showed that exercise could reverse the synaptic and behavioral damage of a high-fat diet, with BDNF as the mediating mechanism, anticipating what the UCC study measured two decades later with far greater metabolomic precision.
The neurotrophic hypothesis of depression holds that hippocampal BDNF depletion is a driving mechanism of depressive illness, not merely a marker. Both antidepressants and aerobic exercise increase hippocampal BDNF through overlapping pathways.
The UCC neurogenesis blockade fits directly into this framework: the cafeteria diet depleted the BDNF machinery, and the exercise signal could not fully land.
Read More: Why Ultra-Processed Foods Are Being Called ‘The Cigarettes of the Future
What This Study Cannot Tell Us, and Why That Matters

The study used adult male rats. Its findings cannot be directly extrapolated to humans, and the absence of female animals is a meaningful limitation given known sex differences in metabolic response and depression prevalence.
One result deserves specific attention. The cafeteria diet did not significantly impair spatial learning or memory in these adult rats, despite disrupting 57% of gut metabolites and blunting neurogenesis. The structural damage was measurable. The behavioral consequence was not, at least in this cohort, over this timeframe.
Developing and aging brains are likely more vulnerable. Voluntary wheel running also cannot be equated to a controlled exercise prescription. What the study does establish is mechanistic direction: specific gut-brain pathways, the nature of the diet-exercise interaction, and the gut metabolome as a plausible mood mediator.
Dr. Heisz’s broader research speaks directly to this: “About one in three people have drug-resistant depression and these individuals often experience greater symptom relief from exercise than medication.” Hence, the brain’s capacity to respond is not fixed. It depends on the conditions you give it.
What the Science Suggests Practically
The evidence does not support the idea that you can fully exercise out of a consistently poor diet, particularly where neurogenesis is concerned. Improving one variable while the other remains poor produces partial benefits. Improving both produces synergistic gains through the BDNF pathway.
For someone sedentary and eating poorly, the practical point is not to wait for a perfect diet before starting to run. Gut metabolite restoration, hormonal normalization, and anxiety reduction still occur even with low diet quality. Those are real benefits even if the neurogenic response is blunted.
Read More: The One-Day Gut Reset: How to Recover After Eating Junk Food
The Bottom Line
Running repairs much of what junk food breaks: gut metabolite disruption, hormonal dysregulation, anxiety, and depression-like behavior. The more important finding is the one most coverage missed. The deepest repair mechanism, hippocampal neurogenesis, depends on both diet and exercise simultaneously.
A brain depleted by chronic poor nutrition cannot fully receive the growth signal that running sends. Diet and exercise are interacting variables. Their interaction point is BDNF, and the hippocampus is where that interaction is most visible and most consequential.
These findings come from a preclinical animal study. Results in rats do not automatically translate to humans, and individual responses will vary. Consult a qualified healthcare professional before making significant changes to your diet or exercise routine.
Frequently Asked Questions
1. Can running reverse junk food damage to the brain?
Partially. The UCC 2025 study found that running restored mood-associated gut metabolites, normalized insulin and leptin, and reduced anxiety and depression-like behavior in cafeteria-fed animals. However, hippocampal neurogenesis was significantly blunted by the poor diet, meaning the full brain-building benefit of exercise requires adequate diet quality alongside it.
2. What does junk food do to the brain?
A Western diet disrupts gut metabolites linked to mood and cognition, spikes insulin and leptin in ways that suppress BDNF signaling, and reduces hippocampal BDNF itself. BDNF governs neuron survival, synaptic plasticity, and neurogenesis. Its depletion is considered a core mechanism in the neurotrophic hypothesis of depression.
3. What is BDNF, and why does it matter?
Brain-derived neurotrophic factor is most active in the hippocampus and supports neuron survival, synaptic plasticity, and neurogenesis. Exercise increases it by up to three times through beta-hydroxybutyrate, a ketone that crosses the blood-brain barrier and activates the BDNF gene. A high-fat, high-sugar diet suppresses this same system. Both antidepressants and aerobic exercise increase hippocampal BDNF through overlapping mechanisms.
4. Do I need to fix my diet before exercise helps my brain?
No. Exercise produces meaningful gut, hormonal, and mood benefits even when diet quality is poor. The neurogenic benefit is blunted, but the other pathways still function. Starting to run before achieving a perfect diet still produces real improvements. The goal is to improve both, since their effects on the brain are synergistic.
References
- Nolan, Y. M., et al. (2025). Running fixes what junk food breaks in the brain: gut metabolomics, hippocampal neurogenesis, and the diet-exercise interaction. Brain Medicine.
- Molteni, R., Wu, A., Vaynman, S., Ying, Z., Barnard, R. J., & Gomez-Pinilla, F. (2004). Exercise reverses the harmful effects of consumption of a high-fat diet on synaptic and behavioral plasticity associated to the action of brain-derived neurotrophic factor. Neuroscience, 123(2), 429-440.
- Sleiman, S. F., Henry, J., Al-Haddad, R., El Hayek, L., Abou Haidar, E., Stringer, T., Ulja, D., Karuppagounder, S. S., Holson, E. B., Ratan, R. R., Ninan, I., & Bhide, P. G. (2016). Exercise promotes the expression of brain derived neurotrophic factor through the action of the ketone body beta-hydroxybutyrate. eLife, 5, e15092.
- Duman, R. S., & Monteggia, L. M. (2006). A neurotrophic model for stress-related mood disorders. Biological Psychiatry, 59(12), 1116-1127
- López-Taboada, I., et al. (2020). Western diet: Implications for brain function and behavior.
- Harvard Health Publishing. (2015, November 16). Nutritional psychiatry: Your brain on food.
- Francis, H. M., & Stevenson, R. J. (2013). The longer-term impacts of Western diet on human cognition and the brain. Appetite.
- Yale School of Medicine. (n.d.). How the standard American diet affects your brain.
- World Economic Forum. (2020, February 20). This is what a Western diet is doing to your brain.
- Nutritional Psychology. (n.d.). Western diet impairs memory in rats—Can it do so in humans?
- News-Medical. (2020, February 20). What the Western diet is doing to your brain.
In this Article