The “gut-brain connection” is a well-known phrase. However, most people aren’t aware of its actual meaning. Your gut has its own nervous system with around 500 million neurons, makes about 95% of the body’s serotonin, and sends most of its signals to the brain.
Such information changes how we think. Your brain isn’t just controlling your gut. Your gut is constantly sending information that can shape how your brain works.
In this article, we’ll explain what the enteric nervous system is, how the gut and brain communicate, what serotonin and “gut feelings” actually mean, how imbalances affect mental health, and what you can do, along with the science behind it.
- The gut is called a “second brain” because it has its own nervous system with ~500 million neurons and communicates constantly with the brain, mostly sending signals upward.
- The gut influences mood and mental health through multiple pathways, including the vagus nerve, immune system, hormones, and gut bacteria.
- Supporting gut health through diet, stress management, and lifestyle can positively impact brain function, but it complements, not replaces, medical care.
What “Second Brain” Actually Means — The Enteric Nervous System
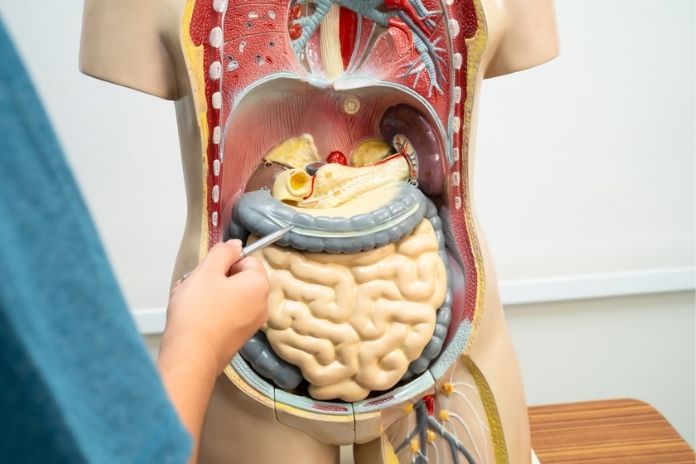
The “second brain” refers to the enteric nervous system (ENS). This is a large network of nerves built into the walls of your digestive tract, running from the esophagus to the rectum. It contains about 500 million neurons, more than the spinal cord.
What makes the ENS special is that it can work on its own. Even if signals from the brain are reduced or blocked, the ENS can still manage digestion. It controls how food moves through the gut, how digestive juices are released, blood flow in the intestines, and even parts of the immune response. It also helps maintain the gut lining, which acts as a protective barrier.
The ENS also produces many of the same chemical messengers as the brain, including serotonin, dopamine, GABA, and acetylcholine. These help the gut function properly and send signals to the brain.
However, it’s important to be clear: the gut doesn’t “think” or create emotions. It’s called a second brain because of its complex structure and independence, not because it can think like the brain.
This independence helps explain why people can have real digestive symptoms, like pain or bloating, even when medical tests don’t show a clear problem.
Read More: How Your Gut Microbiome Secretly Regulates Blood Pressure
How the Gut and Brain Talk — and Who Does Most of the Talking
The Vagus Nerve: The Gut-Brain Superhighway
The vagus nerve is the main connection between the gut and the brain. It runs from the brainstem down to the abdomen.
What’s surprising is the direction of communication. About 80% of the signals travel from the gut to the brain, and only about 20% go from the brain to the gut.
This means your gut is mostly sending updates to your brain. These signals include information about digestion, the state of the gut lining, the activity of gut bacteria, and levels of inflammation. The gut also sends signals from special cells that produce hormones and neurotransmitters like serotonin.
Your brain uses this information to adjust mood, appetite, stress response, and overall body balance. In simple terms, your gut is constantly “reporting” to your brain about what’s happening inside your body.
The Other Communication Routes
The gut and brain don’t rely on just one pathway. They communicate in several ways at the same time.
One important route is the stress system, called the HPA axis. Gut bacteria can influence how much cortisol (the stress hormone) your body produces and how strongly you react to stress.
The immune system is another pathway. The gut plays a significant role in controlling inflammation. It releases chemical signals called cytokines, which can travel through the body and affect the brain, sometimes influencing mood.
There’s also a hormonal pathway. Cells in the gut release hormones such as ghrelin and GLP-1, which circulate in the blood and influence hunger, thinking, and even emotions.
Finally, gut bacteria produce substances called short-chain fatty acids, especially butyrate, when they break down fiber. Some of these can reach the brain and affect its function.
Together, these systems explain why gut health can affect not just digestion, but also mood, sleep, and mental clarity.
Read More: Best Probiotics for Gut Health: Strains That Actually Work and How to Choose
Serotonin Is a Gut Hormone First
Special cells in the intestinal lining produce about 95% of the body’s serotonin. Gut bacteria help stimulate these cells to produce serotonin.
In the gut, serotonin mainly helps control digestion. It regulates how food moves, affects pain sensitivity, and plays a role in nausea.
However, this serotonin does not travel directly to the brain because it cannot cross the blood-brain barrier.
Instead, it works indirectly. When serotonin is released in the gut, it activates the vagus nerve, which sends signals to the brain. These signals can influence how the brain manages its serotonin.
If the gut is out of balance (a condition called dysbiosis), this process can be disrupted. Changes in gut bacteria can affect serotonin production and signaling, which may influence mood through this indirect pathway.
It’s also important to understand that antidepressants like SSRIs work on serotonin in the brain, not the gut. The two systems are separate but closely connected.
The Science Behind “Gut Feelings”

A “gut feeling” is not just a saying; it has a real biological basis.
Your gut is constantly sensing what’s happening inside it, such as stress, inflammation, or changes in bacteria. When something feels “off,” the gut quickly sends signals through the vagus nerve to the brain. These signals reach areas involved in emotions, like the amygdala, and are experienced as a feeling, such as unease or instinct.
This is also why emotional stress often causes physical symptoms such as nausea, stomach discomfort, or loss of appetite. When the brain senses stress, it directly affects how the gut moves and functions.
The connection operates in both directions. Long-term gut problems, like inflammation or an imbalance in bacteria, can keep sending stress signals to the brain. Over time, these issues can contribute to feelings of anxiety or low mood, even without a clear external reason.
When the Gut-Brain Axis Goes Wrong — Dysbiosis
Dysbiosis means an imbalance in the gut microbiome—the community of bacteria living in your digestive system. This can happen due to antibiotics, poor diet, stress, or illness.
Research shows that changes in gut bacteria can affect the brain. In animal studies, altering the gut microbiome changed behavior and brain chemistry. For instance, after changing their gut bacteria, naturally timid mice became more active and exploratory. When their microbiome returned to normal, their behavior also returned to baseline.
This suggests that gut bacteria can directly influence how the brain works.
In the body, dysbiosis can lead to several changes. It can reduce the production of beneficial substances like butyrate, weaken the gut lining, and allow inflammatory molecules to enter the bloodstream. These can reach the brain and affect its function. Simultaneously, stress hormones may increase, and serotonin signaling may become impaired.
This creates a cycle where stress worsens gut health, and poor gut health feeds back into stress and mood changes. While human research is still growing, the overall pattern is clear.
What You Can Actually Do — With the Mechanism Behind Each Strategy

Supporting your gut becomes more meaningful when you understand how it works. One of the most effective steps is increasing fiber from foods such as garlic, onions, oats, bananas, asparagus, and legumes. These fibers feed gut bacteria, which then produce substances like butyrate. Butyrate helps protect the gut lining, reduces inflammation, and supports brain function by increasing factors linked to mood and learning.
Eating fermented foods such as yogurt, kefir, kimchi, and sauerkraut can also help. These foods provide beneficial bacteria and compounds that support a healthy microbiome. Research suggests they may be more helpful than general probiotic supplements for improving mental well-being.
Managing stress is equally important. Stress can quickly change the balance of gut bacteria by affecting the body’s hormone system. Regular exercise, good sleep, and relaxation practices help keep both the gut and brain stable.
Limiting ultra-processed foods also supports gut health. A high intake of these foods correlates with a decrease in gut bacteria diversity and an uptick in inflammation.
At the same time, it’s important to be cautious with supplements. Strong evidence does not support all probiotics, and many gut health products make unproven claims. Gut health can support mental health, but it should not replace medical treatment when needed.
What the Science Can and Can’t Yet Tell Us
Scientists have now discovered numerous connections between the gut and brain. Researchers have established the basic mechanisms, and more human studies are supporting these findings.
However, there are still gaps. We still don’t know which probiotic strains work best for certain mental health problems or how gut-based treatments stack up against more common treatments like counseling or medication.
Research is growing quickly, but it has not yet reached the stage where highly specific medical recommendations can be made. Currently, we should adopt gut health strategies as supportive tools alongside proper medical care.
Read More: 6 Gut Health Mistakes We Made Before Understanding Digestion
Conclusion
The idea of the gut as a “second brain” reflects real biology. With hundreds of millions of neurons, major production of serotonin, and constant communication with the brain, the gut plays an important role in how we feel.
Systems, including nerves, hormones, the immune system, and gut bacteria, are closely linked to gut health and mental health. Taking care of your gut is not just about digestion; it’s also a way to support your brain.
At the same time, science is still evolving. Understanding this connection can help you make better choices, but it’s important to avoid oversimplifying what gut health alone can do.
References
- Advanced Women’s Health. (n.d.). The gut-brain connection: How anxiety impacts your digestion.
- Ataei, P., Kalantari, H., Bodnar, T. S., & Turner, R. J. (2025). The gut–brain connection: Microbes’ influence on mental health and psychological disorders. Frontiers in Microbiomes, 4, 1701608.
- Carabotti, M., Scirocco, A., Maselli, M. A., & Severi, C. (2015). The gut-brain axis: Interactions between enteric microbiota, central and enteric nervous systems. Annals of Gastroenterology, 28(2), 203–209.
- Cryan, J. F., O’Riordan, K. J., Cowan, C. S. M., Sandhu, K. V., Bastiaanssen, T. F. S., Boehme, M., Codagnone, M. G., Cussotto, S., Fulling, C., Golubeva, A. V., Guzzetta, K. E., Jaggar, M., Long-Smith, C. M., Lyte, J. M., Martin, J. A., Molinero-Perez, A., Moloney, G., Morelli, E., Morillas, E., … Dinan, T. G. (2019). The microbiota-gut-brain axis. Physiological Reviews, 99(4), 1877–2013.
- He, W., Wu, Y., Liu, Y., Wu, Y., & Hua, Y. (2024). Cognitive impairment and the gut-brain axis: A bibliometric analysis. Frontiers in Aging Neuroscience.
- Johns Hopkins Medicine. (n.d.). The brain-gut connection
- Mayer, E. A., Tillisch, K., & Gupta, A. (2015). Gut/brain axis and the microbiota. The Journal of Clinical Investigation, 125(3), 926–938.
In this Article