- Control blood sugar and blood pressure tightly to slow kidney damage progression.
- Use proven medications (ACE inhibitors, SGLT2 inhibitors) alongside lifestyle changes.
- Early action in Stage 2 CKD can stabilize or even partially reverse kidney damage. .
It may be difficult to be diagnosed with both diabetes and Stage 2 chronic kidney disease (CKD). Many people start worrying about renal failure or dialysis right away. But in reality, this eGFR 60–89 stage represents a crucial chance. The right strategy can significantly slow or even stabilize kidney damage.
Everything you need to know about a Stage 2 CKD diabetes treatment plan will be covered in this article, including how diabetes affects your kidneys, what goals to pursue, potentially helpful drugs, and useful lifestyle tips. You’ll also learn how to prevent kidney failure, diabetes, and early CKD through structured, science-backed steps.
Read More: Polycystic Kidney Disease: Early Signs and Treatment Options
What Stage 2 CKD Means When You Also Have Diabetes
Understanding eGFR 60–89 with Kidney Damage Markers
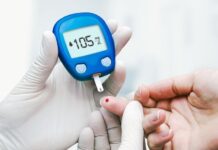
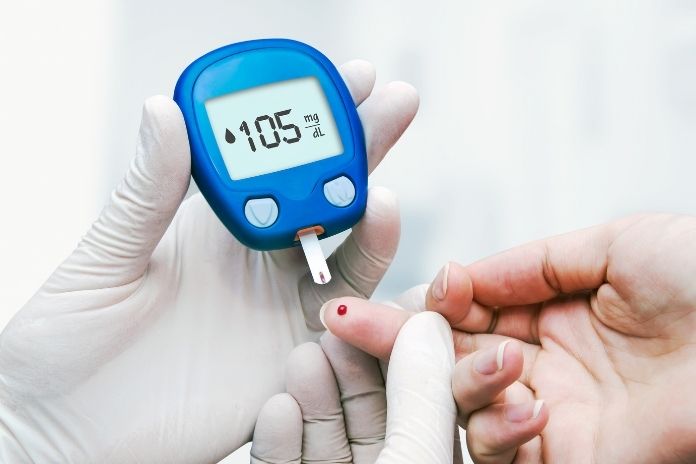
A number derived from blood test results, the estimated glomerular filtration rate (eGFR), helps medical professionals determine whether you have kidney disease (CKD) and how well your kidneys are functioning.
A physician determines your estimated glomerular filtration rate (eGFR) by evaluating your blood levels of a waste product called creatinine in addition to other variables, including your age and biological sex. This figure shows how many milliliters of blood your kidneys are eliminating each minute.
Healthy kidneys normally filter more than 90 milliliters per minute (this amount is adjusted for body size). A decreased rate may indicate chronic kidney disease (CKD).
How Diabetes Affects Kidney Filtering Units
Over 34 million Americans have diabetes, which necessitates lifelong care. Diabetes is a complicated and highly individualized condition. Daily self-management has obstacles, but the rewards are substantial.
Diabetes can harm kidney blood vessels, which can result in kidney damage and a decline in kidney function, which can cause waste materials to accumulate in your blood. Changes in kidney blood circulation are one of the factors linked to other types of kidney disease.
Protein “spills” into the urine as a result of these alterations, which also have an impact on blood vessels and blood pressure (protein shouldn’t ordinarily be present in urine). Another significant risk factor for kidney damage in diabetics is high blood pressure. Maintaining blood pressure at an optimal level can help prevent kidney disease.
Diabetes-related issues can also harm the body’s nerves, making it difficult to urinate. This pressure could lead to renal damage or infection.
Why Early-Stage Intervention Matters Most
Early intervention during diabetes Stage 2 CKD management is crucial because:
- You can still control or partially reverse the damage
- It is possible to slow progress significantly
- Complication risk can be decreased
How Diabetes Leads to Kidney Damage Over Time
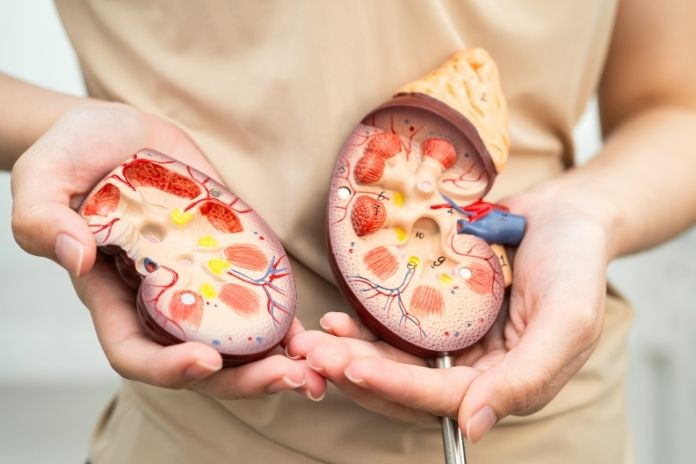
Diabetes affects kidney health in several ways, including:
High Blood Sugar and Glomerular Stress: The kidneys have to work harder when blood glucose levels are consistently high. As a result, the glomeruli’s internal pressure rises, gradually causing damage.
Inflammation and Microvascular Injury: Diabetes reduces the amount of oxygen that reaches kidney tissues by causing inflammation and damaging small blood vessels.
Protein Leakage (Albuminuria): Proteins such as albumin seep into the urine when the filters deteriorate. It is a sign of early kidney impairment and is known as albuminuria, diabetes, and CKD.
Role of Blood Pressure: By putting more strain on already-damaged renal arteries, high blood pressure exacerbates the issue. That’s why blood pressure goals for CKD and diabetes are critical.
Read More: Does C3 Glomerulopathy Lead to Kidney Failure? What the Data Shows
The Core Goals for Preventing Kidney Failure
If you know what could cause renal failure, you can avoid getting it in the first place. You can do the following things to try to lower the chances of having this problem:
Watch Your Blood Sugar: Eating too many sugary foods and refined sugar can hurt your kidneys. One of the risks of having diabetes, which is a long-term illness, is kidney failure.
Eat a Balanced Diet: A well-balanced diet with few refined foods can help keep your kidneys healthy for a long time. Eating whole grains, fresh fruits and vegetables, and fiber can help your kidneys stay healthy and lower your risk of kidney disease.
Cut Back on Salt: Too much salt, like too much sugar, can harm your kidneys. Eating too much sodium is one of the main causes of high blood pressure, which can harm the kidneys.
Drink a lot of Water: Not drinking enough water can harm the kidneys by reducing the amount of healthy blood that reaches them. Staying well-hydrated can lower your risk of serious health problems.
Limit Your Alcohol Consumption: Drinking too much can hurt your kidneys and other organs very badly. Heavy drinking can also change blood pressure and blood sugar, which makes kidney disease more likely.
Exercise: One more way to keep your kidneys healthy for a long time is to set aside time every day for healthy exercise. Exercise helps the kidneys remove harmful substances and improves blood flow.
Keep an eye on your Blood Pressure: Millions of people worldwide have high blood pressure, which can be very harmful to their health. It can harm the kidneys both immediately and over time.
Blood Sugar Targets That Support Kidney Health
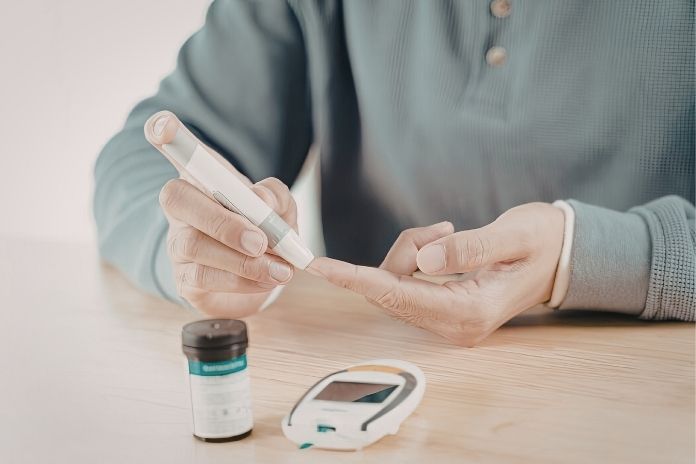
One of the most effective strategies to safeguard your kidneys is to maintain appropriate blood sugar levels. Find out from your doctor what your ideal blood sugar levels should be. Everybody will have a different blood sugar goal.
Generally speaking, the suggested goals for the majority of people are:
- 80–130 mg/dL before meals
- Two hours following the beginning of a meal: less than 180 mg/dL
- About 7% on the A1C test
Preventing Blood Sugar Swings: Stable, slightly increased blood sugar levels are less harmful to blood vessels than large swings.
The Key Is Balance
For glycemic control to be effective:
- Steady blood sugar levels
- Preventing hypoglycemia
- Keeping up regular patterns
Blood Pressure Control: A Key Driver of Kidney Protection
Blood pressure significantly influences kidney health:
Why It Matters: High blood pressure raises internal pressure and accelerates damage to kidney filters.
Target Ranges: Typical blood pressure goals for CKD and diabetes are below 130/80 mmHg, though individual recommendations may vary.
Lifestyle Techniques: You can help maintain a healthy blood pressure level by:
- Cutting back on salt consumption
- Maintaining physical activity
- Minimizing tension
- Keeping a healthy weight
When Medication Is Required: A healthy lifestyle might not be sufficient. Medications are often part of the management of diabetes in Stage 2 CKD.
Read More: Kidney Stones: Why They Happen and How to Prevent Them
Medications That May Help Slow CKD Progression in Diabetes

1. Angiotensin-Converting Enzyme Inhibitors, or ACE Inhibitors
ACE inhibitors help preserve kidney health by lowering blood pressure and reducing proteinuria (protein in the urine). Typical names for medications:
- Lotensin, or benazepril
- Lisinopril (Prinivil, Zestril)
- Accupril, or quinapril
- Altace (ramipril)
2. Angiotensin II Receptor Blockers, or ARBs
Like ACE inhibitors, ARBs protect the kidneys by lowering blood pressure and reducing proteinuria. Typical names for medications:
- Losartan (Cozaar) and irbesartan (Avapro)
- Olmesartan (Benicar)
- Valsartan (Diovan)
3. SGLT2 Inhibitors (Sodium-Glucose Co-Transporter-2 Inhibitors)
SGLT2 inhibitors prevent the kidneys from reabsorbing glucose from the blood. Urine is then used to filter away the sugar. Even in those without diabetes, they help protect and lower kidney pressure.
Typical names for medications:
- Brenzavvy, or bexagliflozin
- Canagliflozin (Invokana)
- Farxiga, or dapagliflozin
- Jardiance empagliflozin
- ertugliflozin (Steglatro)
4. GLP-1 Receptor Agonists (Glucagon-Like Peptide-1 Receptor Agonists)
By lowering blood sugar, reducing excess salt intake, and regulating inflammation, GLP-1 RAs may help protect the kidneys. They also aid in weight loss. To fully understand how these drugs directly benefit the kidneys, more research is required.
Typical names for medications:
- Trulicity (dulaglutide)
- exenatide (Bydureon, Byetta)
- Liraglutide (Saxenda, Victoza)
- semaglutide (Ozempic, Wegovy, Rybelsus)
- tirzepatide (Zepbound, Mounjaro)
5. Non-steroidal Mineralocorticoid Receptor Antagonists (nsMRAs)
nsMRAs shield the kidneys’ filters by helping the body eliminate excess water and salt. It lessens the strain on the heart and kidneys, reducing the chance of cardiovascular issues, including strokes and heart attacks. Finerenone (Kerendia) is the only nsMRA approved by the FDA.
6. Statins (HMG-CoA Reductase Inhibitors)
The main purpose of statins is to lower cholesterol levels. By preventing the accumulation of fatty deposits in blood vessels, they also safeguard kidney health in people with diabetes by facilitating easier blood flow to the kidneys and the heart.
Typical names for medications:
- Lipitor, or atorvastatin
- Lescol XL (fluvastatin)
- Altoprev (lovastatin)
- Pitavastatin (Zypitamag, Livalo)
- Pravachol, or pravastatin
- Rosuvastatin (Crestor)
- Simvastatin (Zocor)
Nutrition Strategies for Diabetes With Stage 2 CKD
Diet plays a central role in slowing CKD progression and diabetes:
Balanced Carbs: To help with glycemic control, concentrate on complex carbohydrates with a low glycemic index.
Sodium Awareness: Lowering sodium levels helps achieve blood pressure objectives for diabetes and chronic kidney disease.
Protein Intake: It is advised to consume a moderate amount of protein. While too little protein can lead to malnutrition, too much protein can strain the kidneys.
Fiber-Rich Foods: Whole grains, fruits, and vegetables promote kidney and blood sugar health.
Potassium and Phosphorus: Monitoring may be necessary, but limits are often not severe at Stage 2 CKD.
Read More: Can the Kidneys Repair Themselves? What Science Says
Weight and Physical Activity: Their Role in Slowing Progression

Maintaining a healthy weight lessens kidney strain and increases insulin sensitivity.
Advantages of Exercise
Exercise is beneficial:
- Boost glycemic management
- Reduce your blood pressure
- Decrease inflammation
Exercise Recommendations: For the management of diabetes and Stage 2 CKD, moderate activities such as walking, cycling, and yoga are ideal.
Safety Advice
- Drink plenty of water
- Steer clear of overdoing it
- Check your blood sugar both before and after working out
Monitoring Markers That Signal Progress or Risk
Tracking your health metrics helps guide your Stage 2 CKD diabetes treatment plan:
Serum Creatinine and Estimated Glomerular Filtration Rate (eGFR): Because creatinine is a waste product of muscle metabolism, blood serum creatinine assays are the primary method for assessing kidney function. When kidney function deteriorates, the human body produces more creatinine. Creatinine analysis does not provide a complete picture of kidney health.
Blood Urea Nitrogen (BUN): By tracking the amount of nitrogen in the blood that is filtered through urea during metabolism, it functions similarly to a kidney function test. High BUN levels indicate impaired kidney function, but other factors, including dietary protein intake and hydration status, can also affect BUN levels.
Proteinuria and Albuminuria: Tests for protein or albumin in the urine are important markers for diagnosing kidney damage. Albuminuria is the first of the antecedent indications of chronic kidney disease (CKD), and it is associated with a higher risk of both progressive disease progression and medical consequences.
Kidney Injury Molecule-1 (KIM-1): Urine samples can be used to assess the KIM-1 protein, which is highly expressed in injured proximal tubules of the kidney. According to studies, KIM-1 can assess the degree of kidney damage and distinguish between acute and chronic renal diseases.
Lifestyle Habits That May Help Protect Kidney Function

Do you want to keep your kidneys as healthy as possible? Consider adding these healthy habits to your daily routine.
Drinking More Water: Your kidneys can remove toxins more effectively if you drink enough water. You probably know the advice to drink “eight glasses of water a day,” but there is no one-size-fits-all way to drink water. How much water you need depends on how much you exercise, where you are, and your overall health.
Eating Foods that are Good for your kidneys: Lean proteins, whole grains, and fresh fruits and vegetables can help relax your kidneys. Because of this, people with kidney disease often eat a lot of these foods. Even if your kidneys are healthy and working well, it’s a good idea to eat a diet that supports them.
Regular Exercise: It can help lower your risk of kidney problems by improving circulation, lowering blood pressure, regulating blood sugar, and helping you keep your weight in check. Every week, try to work out for at least 150 minutes at a moderate intensity.
Keeping an Eye on Important Numbers: Diabetes and high blood pressure are directly linked to chronic renal disease. You can keep your kidneys healthy by regularly checking your blood pressure and blood sugar levels at home.
Read More: How Diabetes Impacts Your Kidneys (and How to Protect Them)
Warning Signs That Kidney Disease May Be Progressing
It’s crucial to keep an eye out for symptoms of deteriorating CKD even with proper management:
- Fluid, exhaustion, and frequent urination
- Breathing difficulties, swelling, and skin changes
- Back pain, blood pressure, and more
- Exhaustion
See your healthcare physician right away if you observe these.
How Often to Follow Up With Your Healthcare Team

Regular follow-ups are key to effective diabetes Stage 2 CKD management.
Normal Timetable:
- Blood tests every three to six months
- Tests for microalbuminuria in the urine
- Checking of blood pressure
Medication Modifications: Depending on test results, treatment may need to be modified.
The Role of a Renal Dietitian: A dietitian can personalize your diet for diabetes with early kidney disease.
Coordinated Care: Managing both diabetes and CKD requires a team approach to prevent kidney failure, diabetes early CKD.
Read More: Kidney Stones: Types, Causes, Symptoms, and Diet
Conclusion
Taking action early and often is the most important part of diabetes Stage 2 CKD management. You have a good chance of stopping, or even reversing, the progression of your illness because your kidneys are still mostly functioning at this point.
By focusing on keeping your blood sugar stable, your blood pressure healthy, and making lifestyle choices that are good for your kidneys, you can avoid problems in the long run. To keep your kidneys healthy, you need to see a doctor on time, eat the right foods for you, and have regular checkups.
When needed, medications can make things safer and less dangerous. Most importantly, small, everyday choices like staying active, eating a healthy diet, and avoiding bad habits can have a big impact on your health.
References
- Kidney Research UK. Estimated glomerular filtration rate (eGFR)
- Nephrological Associates. Diabetes and kidney disease.
- International Diabetes Federation. Diabetes and the kidneys.
- UF Health. Diabetes and kidney disease.
- Kidney Research UK. Kidney disease and diabetes
- Puget Sound Kidney Centers. How to protect your kidneys.
- National Institute of Diabetes and Digestive and Kidney Diseases. Preventing chronic kidney disease.
- American Kidney Fund. (March 4, 2026). Kidney-friendly eating plan.
- Fresenius Medical Care. Common diabetes medication slows CKD progression, study finds.
- Vejthani Hospital. Six signs of kidney disease: How to know your kidneys are in trouble and act fast.
In this Article