Many women believe urologists are only for men. This is one of the biggest reasons urinary problems in women are often missed or treated late. In reality, understanding the roles of urologists and gynecologists in women’s health is important, as urologists treat the urinary system in all individuals, including women.
Symptoms such as repeated UTIs, bladder pain, leakage, or blood in the urine are common, but they do not always fall under routine gynecologic care. An OB-GYN focuses on reproductive and hormonal health, while a urologist focuses on the bladder, kidneys, and urinary tract.
When these symptoms are treated in the wrong setting, women may go through years of temporary fixes instead of getting a clear diagnosis.
This article explains how care is divided between an OB-GYN, a urologist, and a urogynecologist, highlighting five key symptoms that mean it is time to look beyond routine care.
- Urologists treat the urinary system in women too; many bladder and kidney symptoms fall outside routine gynecologic care.
- Persistent issues such as recurrent UTIs, blood in urine, or bladder pain need specialist evaluation, not repeated short-term treatment.
- Choosing the right specialist matters: OB-GYN (hormones/reproductive), urologist (urinary system), and urogynecologist (bladder + pelvic floor overlap).
Read More: Does C3 Glomerulopathy Lead to Kidney Failure? What the Data Shows
Three Specialists, Three Lanes, and Where They Overlap

Women’s health involves different systems, so different specialists play different roles.
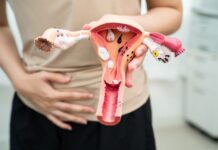
An OB-GYN focuses on reproductive organs and hormones. This includes menstrual cycles, fertility, pregnancy, menopause, and conditions like PCOS. They often treat simple urinary tract infections, especially when symptoms are straightforward, but they usually do not perform advanced testing of the bladder or kidneys.
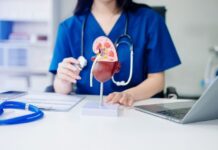
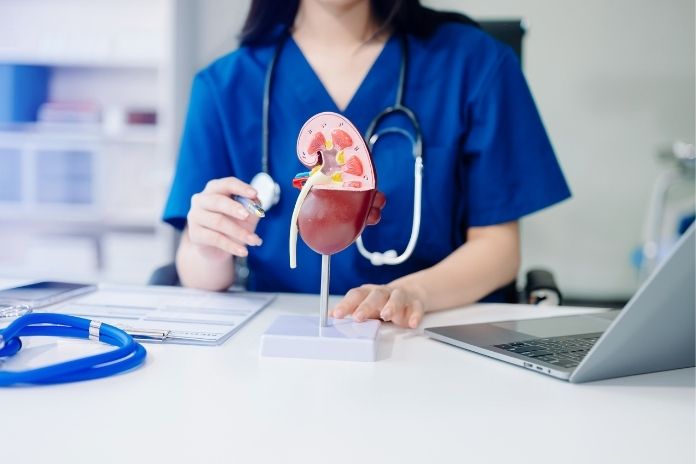
A urologist focuses on the urinary system, which includes the kidneys, ureters, bladder, and urethra. This is important because no other women’s specialist manages the upper urinary tract. Urologists diagnose and treat kidney stones, blood in the urine, bladder disorders, and structural problems.
They also perform procedures such as cystoscopy, where a small camera is used to look inside the bladder, along with imaging studies to evaluate the kidneys.
A urogynecologist is trained in both gynecology and urology. They focus on conditions where the bladder and pelvic floor are connected. This includes bladder leakage, pelvic organ prolapse, childbirth-related pelvic injury, and complex bladder pain conditions. Their approach considers both anatomy and function.
A simple way to think about this:
- For reproductive or hormone-related concerns consult an OB-GYN
- For kidney and upper urinary tract issues, consult a urologist
- For bladder problems linked with pelvic floor changes, consult a urogynecologist
If you are unsure, starting with a primary care doctor or OB-GYN is reasonable, but continuous symptoms should lead to referral rather than repeated short-term treatment.
Quick decision table:
Pelvic & Urinary Health
Symptoms & Specialists
| Symptom(s) or Situation | What It Could Mean | Who to Consult |
|---|---|---|
| Recurrent UTIs 3 or more per year |
Bladder not emptying fully. Bacteria may persist. | Urologist Urogynecologist |
| Blood in urine even once |
It could be stones, an infection, or something serious | Urologist (Urgent) |
| Kidney stones | Mineral buildup in the kidneys | Urologist |
| UTI symptoms but negative tests |
Likely not an infection; could be Interstitial Cystitis (IC) | Urologist |
| Bladder leakage | Weak pelvic floor or bladder issue | Urologist Urogynecologist |
| Pelvic organ prolapse | Weak pelvic support | Urogynecologist |
| Overactive bladder | Bladder signals misfiring | Urologist Urogynecologist |
| Painful bladder or IC | Chronic bladder condition | Urologist Urogynecologist |
| Menstrual/Fertility issues | Hormone or reproductive issue | OB-GYN |
| Mixed pelvic pain | More than one system is involved | OB-GYN + Urologist |
Five Symptoms That Signal It’s Time to See a Urologist
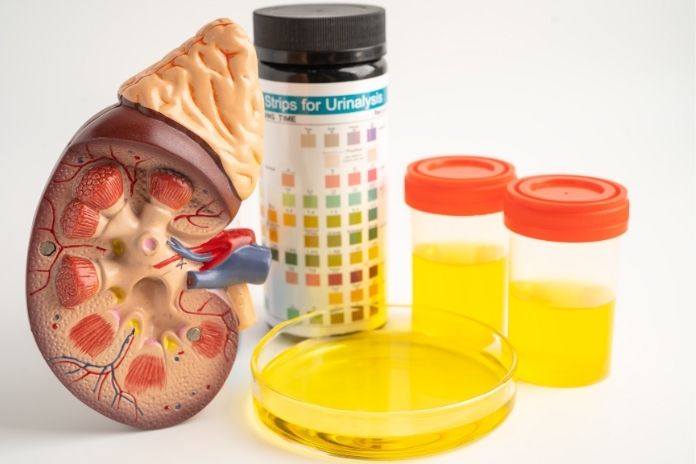
1. Blood In Urine, Even Once
Blood in the urine, called hematuria, should always be taken seriously. If you can see blood, it requires urgent evaluation. Even if it is found only on a lab test, it still needs proper follow-up.
According to American Urological Association guidelines, many women in midlife with microscopic blood in urine should undergo evaluation that includes looking inside the bladder and imaging the kidneys. This helps rule out causes such as stones, infections, and more serious conditions. It should not be assumed to be a simple UTI without confirmation and a follow-up visit.
2. UTIs That Keep Coming Back
Occasional UTIs are common, but frequent urinary tract infections are not. If you have three or more in a year, it is considered recurrent.
At this stage, the goal is to understand why the infections are happening. Possible reasons include incomplete bladder emptying, pelvic organ prolapse, or persistent bacteria that are not fully cleared. A urologist can perform tests to identify these issues and create a long-term plan instead of repeating antibiotics.
3. UTI Symptoms But Negative Cultures
Many women experience burning, urgency, and pelvic discomfort but are told their tests are normal. This pattern is important and should not be ignored.
When urine cultures are negative, but symptoms continue, the cause is often not an infection. One possible condition is interstitial cystitis or bladder pain syndrome. Because it mimics a UTI, it is often misdiagnosed. A urologist is needed to evaluate this properly using specialized tools.
4. Kidney Stones And Lack Of Follow-Up

Kidney stones are not just a one-time problem. After the first episode, the risk of another stone is high.
A urologist evaluates not only the stone itself but also the reason it formed. This may involve 24-hour urine testing, dietary review, and metabolic evaluation. With the right guidance, many future stones can be prevented.
5. Bladder Leakage That Is Not Improving
Bladder leakage is common, especially after childbirth or with aging, but it is not something you have to accept.
There are different types of incontinence, including stress incontinence, urgency incontinence, and mixed forms. Each type has different causes and treatments. A specialist can identify the type and recommend targeted treatments such as pelvic floor therapy, medications, or procedures if needed.
A Note On Overactive Bladder
An overactive bladder is a condition where you feel a sudden and strong urge to urinate that is hard to control. It often comes with frequent urination and waking up at night to go to the bathroom.
It is often misunderstood or ignored because many women think it is normal. In reality, it is treatable. Treatment options include bladder training, pelvic floor exercises, medications, and nerve-based therapies that help control bladder signals. If one treatment does not work, other effective options are available.
Read More: Polycystic Kidney Disease: Early Signs and Treatment Options
Interstitial Cystitis, The Condition That Often Gets Missed

Interstitial cystitis, also called bladder pain syndrome, is one of the most commonly missed conditions in women’s urinary health. It causes long-term bladder pain, urgency, and frequent urination without any infection.
Because the symptoms feel like a UTI, many women are given antibiotics again and again, even when urine tests are negative. This cycle can continue for years, delaying the correct diagnosis and treatment.
The reason for this delay is that diagnosis requires tools like cystoscopy and specialized bladder evaluation, which are only available with a urologist or urogynecologist. These tests help rule out other conditions and confirm the diagnosis.
Treatment is usually a combination approach. It may include pelvic floor physical therapy, dietary changes to avoid bladder irritants, medications, and bladder-specific treatments.
A key takeaway is this: if you have ongoing bladder pain, urgency, or frequency and your urine tests are repeatedly negative, it is important to consider this condition and seek specialist care.
Urologist or Urogynecologist: Which One Should You See
The right specialist depends on your symptoms and where the problem is coming from.
A urologist is the best choice for conditions involving the kidneys or upper urinary tract, blood in the urine, kidney stones, and complex bladder problems that require testing or procedures.
A urogynecologist is better suited for conditions involving both the bladder and pelvic floor. This includes pelvic organ prolapse, leakage after childbirth, and mixed urinary symptoms where both support and function are affected.
If you are unsure, do not delay care while trying to make the right choice. Both specialists are trained to evaluate urinary symptoms and can guide you towards the right treatment. Getting a proper evaluation early is more important than choosing the right specialist in the beginning.
Read More: Hidden Salt Sources That Can Damage Your Kidneys
Conclusion
Your OB-GYN is an important part of your healthcare, but they do not cover every condition related to the urinary system. Some symptoms require a different kind of specialist.
If you have blood in your urine, frequent UTIs, bladder pain without infection, or leakage that is not improving, it may be time to see a urologist or urogynecologist.
Medical Disclaimer: This article is for general information only and does not replace medical advice. Always consult a qualified healthcare provider for diagnosis and treatment tailored to your needs.
References
- National Center for Biotechnology Information. (2023). Interstitial cystitis (bladder pain syndrome). In StatPearls. StatPearls Publishing.
- National Center for Biotechnology Information. (2023). Overactive bladder. In StatPearls. StatPearls Publishing.
- National Center for Biotechnology Information. (2023). Hematuria. In StatPearls. StatPearls Publishing.
- Pella Regional Health Center. (n.d.). Recurrent urinary tract infection.
- National Center for Biotechnology Information. (2023). Hematuria. In StatPearls. StatPearls Publishing.
- American Urological Association. (2020). Microhematuria: AUA/SUFU guideline. The Journal of Urology.
- Max Healthcare. (n.d.). Urologists: Who are they and what can they do for me?
In this Article