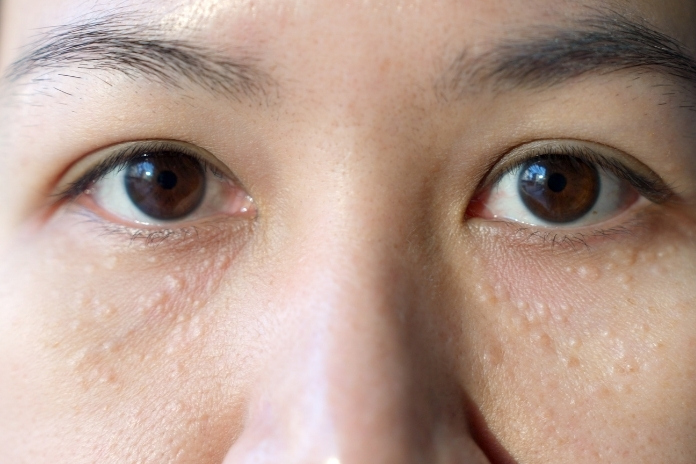
You splurge on a pricey anti-aging eye cream, expecting smoother skin. Weeks later, tiny white bumps appear right under your eyes. These are likely milia from eye cream, a frustrating side effect of rich formulas that trap keratin beneath the surface.
This article uncovers why anti-wrinkle cream white bumps happen, especially from heavy creams that cause milia, and shares safe ways to treat and prevent milia under the eyes without harming delicate skin.
Read More: 16 Effective Cures For Dry Eyes That Work Like Magic
What Exactly Is Milia?
Milia are small, firm, white or yellowish bumps that form under the skin. They occur when keratin, a tough protein produced by skin cells, gets trapped instead of shedding naturally. Unlike acne, milia are not pimples or clogged pores under eyes.
They form cyst-like structures deep in the epidermis, making them harmless but cosmetically bothersome.
These bumps often show up around the eyes in adults who use heavy skincare. While they affect people of all ages, they are common in those over 30 who reach for potent creams in pursuit of youthful skin.
Milia come in two main types worth understanding:
- Primary milia form spontaneously from keratin buildup, typically on the eyelids, cheeks, and nose.
- Secondary milia develop as a direct response to something that damages or clogs the skin’s surface, such as a burn, a blistering rash, sun damage, or, critically, overuse of occlusive skincare products. When your eye cream triggers milia, that is secondary milia at work.
Knowing which type you have matters because secondary milia require addressing the root cause, not just the bumps themselves.
“Milia under the eyes often result from heavy occlusive creams that trap keratin on thin periorbital skin. Switch to lightweight, non-comedogenic gels, incorporate gentle exfoliation like lactic acid, and introduce retinoids slowly to prevent recurrence. For stubborn cases, professional extraction remains the gold standard, safe and effective in expert hands.”
Dr. Mona Gohara, M.D., Clinical Professor of Dermatology at Yale School of Medicine.
How Anti-Wrinkle Creams Can Trigger Milia

Rich eye creams promise miracles, but can backfire on thin under-eye skin. Periorbital milia arise when products disrupt the skin’s natural balance, leading to keratin buildup. Several factors work together here, making prevention key.
The Periorbital Skin Problem
Under-eye skin, the periorbital area, measures just 0.5 millimeters thick, half as thin as the cheeks. It also has fewer oil glands, so it struggles to process heavy textures. Occlusive ingredients like thick emollients create a barrier that blocks keratin shedding, trapping it into bumps.
Not everyone who uses a rich eye cream will develop milia. Skin type plays a real role: people with oily or combination skin tend to be more susceptible because their skin already has a slower natural shedding cycle in the periorbital zone.
Those with drier skin types may tolerate somewhat heavier formulas, though the thinness of under-eye skin makes everyone more vulnerable than they would be elsewhere on the face. If you have developed milia before from skincare, treat that history as a reliable signal to choose lighter formulas going forward.
Ingredient Overload and Barrier Disruption
Layering actives such as retinoids, peptides, and ceramides can overwhelm renewal cycles. Skin responds by overproducing keratin, which gets stuck when the exfoliation barrier function breaks down. This cycle worsens with daily use of non-breathable formulas.
Improper Layering and Overuse
Applying thick eye cream over serums or oils hinders proper absorption, leaving excess product on the skin overnight. This residue mixes with dead skin cells, creating an environment where keratin becomes trapped and forms cysts. The fix is moderation: pat products on sparingly and allow each layer enough time to absorb before adding the next.
Read More: How to Remove Bags Under Eyes
Ingredients Most Likely to Cause Milia
Not all ingredients spell trouble, but certain ones found in eye creams formulated for drier skin types can easily clog milia-prone skin.
Heavy occlusive ingredients top the list by sealing everything in. Fragrances and irritants contribute indirectly by sparking inflammation that slows cell turnover. These ingredients work fine on thicker areas like the cheeks, but can be problematic in the delicate periorbital zone.
Based on dermatologist guidance from the American Academy of Dermatology, here are the most common offenders and safer alternatives:
Skin Care Science
Ingredients to Avoid for Periorbital Milia
| Ingredient to Avoid | Why It’s a Problem | Safer Swap |
|---|---|---|
| Petrolatum / Mineral Oil | Creates an impermeable barrier; top association with periorbital milia | Hyaluronic acid Glycerin |
| Lanolin | Highly comedogenic around the eyes despite being “natural” | Squalane |
| Dimethicone (high concentration) | Forms a persistent occlusive film that impedes shedding | Low-weight silicones Niacinamide |
| Shea / Cocoa Butter | Occlusive fats that resist absorption in thin skin | Ceramide-based serums |
| Beeswax / Carnauba Wax | Film-formers with no penetration; trap keratin effectively | Lightweight peptide gels |
| Fragrance / Irritants | Trigger micro-inflammation, slowing turnover | Fragrance-free formulas |
It is worth noting that none of these ingredients is inherently harmful. Petrolatum is a dermatologist-recommended barrier ingredient for dry eczema-prone skin.
Shea butter is deeply nourishing for lips and body. The issue is not the ingredient itself but the mismatch between a heavy formulation and the uniquely thin, low-oil periorbital skin.
If a product leaves a visible waxy sheen 10 to 15 minutes after applying it under your eyes, it is likely too occlusive for that area.
Read More: Dry Eyes: 10 Best Eye Drops 2021; Causes, Symptoms, Treatment
How to Treat and Prevent Milia Around the Eyes
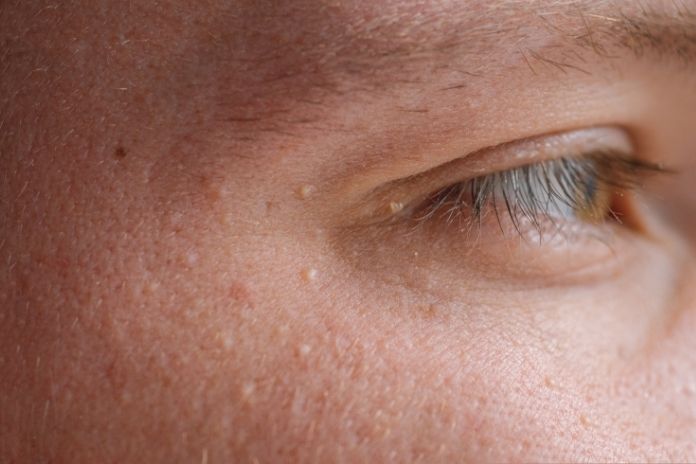
Switching to breathable care routines is the first step. How to treat milia safely starts with prevention. Targeting root causes like product weight can clear bumps and stop them from coming back.
1. Switch to Lightweight, Non-Comedogenic Formulas
Opt for gel serums over thick balms. Choose non-comedogenic moisturizers with humectants like hyaluronic acid or glycerin. These draw moisture into the skin without trapping debris or keratin.
When scanning labels, look for products that list water-based or gel-type bases before any emollient ingredients.
Hyaluronic acid and glycerin are both excellent humectants: they pull water into the skin from the environment without sitting on top of it the way occlusive agents do. These are particularly well-suited to the periorbital area because they deliver hydration without adding the weight that triggers milia.
2. Exfoliate Gently and Consistently
Gentle chemical exfoliants speed cell turnover. Lactic acid or polyhydroxy acids (PHAs) suit sensitive skin around the eyes. Apply two to three times weekly after cleansing for safe results.
Be careful not to apply exfoliating acids directly on the eyelid or too close to the lash line. Apply them to the orbital bone area only, at least a centimeter away from the lash margin. This delivers the cell-turnover benefit where it is needed, right at the under-eye zone, without irritating the sensitive eyelid skin.
3. Introduce Retinoids Slowly
Retinol and milia actually have a helpful long-term relationship. Retinoids boost cell renewal to prevent buildup. Research confirms that topical retinoids actively regulate keratin expression in the epidermis, reducing the likelihood of keratin becoming trapped beneath the skin’s surface.
The retinoid adjustment period can bring initial purging, so ease in carefully.
- Start with one to two applications per week.
- Use a pea-sized dab diluted in moisturizer.
- Buffer with the best skincare for milia-prone skin, such as ceramide serums.
Do not apply retinol directly onto the eyelid. Keep applications to the orbital bone, and use an eye-specific retinol formulation if possible. Standard retinol concentrations for the face can be too strong for this area.
For those who find retinoids too irritating, bakuchiol is a plant-derived retinol alternative with comparable cell-turnover benefits and a gentler tolerance profile.
4. Maintain a Balanced Barrier
Light emollients like squalane or niacinamide restore barrier function without overload. Clinical studies confirm that topical niacinamide improves stratum corneum barrier function, increases ceramide synthesis, and supports healthier keratinocyte turnover. Limit to three to four products maximum around the eyes.
5. Use Sunscreen Daily
UV exposure thickens skin over time, worsening buildup and making it harder for dead cells to shed naturally. Mineral SPFs with zinc oxide clog less than chemical ones. Apply every morning.
Sun protection also helps prevent post-inflammatory hyperpigmentation if you have had milia professionally extracted. Darker skin tones are especially vulnerable to dark spots after extraction procedures, and consistent SPF use significantly reduces that risk.
Read More: 5 Effects of Hurting Your Eyes After Swimming
When to Expect Results
A common question is how long it takes to see improvement once you switch products and start gentle exfoliation. Realistically, give your skin four to eight weeks before expecting visible change.
Milia are structural keratin cysts, not surface buildup, so they respond slowly. New milia should stop forming within two to four weeks of eliminating heavy occlusive products. Existing milia may soften and begin resolving on their own over six to ten weeks.
If bumps have not improved after two to three months of consistent skincare adjustments, that is when professional extraction makes the most sense. Consistency matters more than speed: slow, steady product changes are less likely to cause irritation than abrupt overhauls of your entire routine.
What to Avoid When Treating Milia

Steer clear of DIY fixes that can scar delicate under-eye skin. Milia under the eyes can worsen when you tamper with these deep-seated bumps. Follow expert guidance to avoid setbacks.
Common Mistakes to Skip
Do not pick or squeeze milia. These bumps sit deep beneath the surface. Such actions risk infection, scarring, or lasting pigmentation in the thin periorbital area.
Risky Products and Practices
Avoid occlusive masks and overnight treatments while bumps persist. They trap more keratin and extend recovery time.
Skip undiluted oils like coconut or olive near the eyes. These heavy formulas clog easily and fuel milia under the eyes.
Harsh scrubs inflame sensitive skin. Mechanical exfoliation damages the barrier and slows natural turnover.
It is also worth avoiding topical corticosteroid creams in the eye area unless prescribed and supervised by a dermatologist.
Long-term or unsupervised use of strong topical steroids around the eyes has been documented as a contributing cause of secondary milia, in addition to carrying risks of skin thinning and elevated eye pressure. If you use a steroid cream for another condition and notice milia forming, let your doctor know.
- No home extractions: Tools spread bacteria.
- No strong acids: High concentrations irritate thin skin.
- No heavy balms: They block the natural shedding process.
Read More: Why Your Vision Is Blurry in the Morning (and What It Means for Your Eyes)
When to See a Dermatologist

Milia resolve with skincare adjustments for most people, but seek professional help if bumps linger two to three months. Watch for clusters spreading to the cheeks or eyelids, or for any pain and redness that could signal infection.
Dermatologists offer several effective outpatient options:
Professional Skin Care
Common Milia Treatments
| Treatment | How It Works | Best For |
|---|---|---|
| Manual extraction (lancing) | Sterile needle opens the cyst; comedone extractor removes the keratin plug | Most milia, including near the eyelid |
| Cryotherapy | Controlled freezing destroys the cyst | Multiple or clustered milia |
| Laser ablation | Laser energy breaks down trapped keratin | Extensive milia or those near the lid margin |
| Topical retinoid (prescription) | Accelerates cell turnover over weeks to months | Recurring milia as ongoing prevention |
All of these are outpatient procedures with minimal downtime. Do not try to replicate the extraction at home. Milia sit too deep beneath the skin’s surface to squeeze out the way you might a blackhead, and attempting it causes scarring.
The Takeaway
Milia from eye cream most often strike when rich anti-wrinkle products overwhelm thin skin. The heavier the formula, the higher the risk that occlusive ingredients block natural keratin shedding and create those stubborn white bumps.
The good news: smarter choices get faster results than switching to something thicker ever will.
Key fixes: Lightweight gels. Gentle exfoliation. A slow retinol introduction. Daily mineral SPF.
Most people see noticeable improvement within six to eight weeks of making these changes consistently. Smoother under-eyes come from giving the skin room to breathe, not from loading it with more product.
If you have been applying the same heavy cream for months and are not seeing the smoothing effect you hoped for, the cream itself may be part of the problem.
For persistent milia, a dermatologist extraction works quickly and leaves no scarring when done by a professional. You do not need to live with these bumps.
References
- Bailey, C. (2021). What causes milia? Dr. Cynthia Bailey Skin Care.
- Dayal, S., Sahu, P., & Jain, V. K. (2022). Facial milia-like eruption in a patient with alopecia. Cureus, 14(6), Article e26200.
- Del Rosso, J. Q., & Pillai, R. (2017). Efficacy and safety of an anti-aging technology for the periorbital region. Journal of Clinical and Aesthetic Dermatology, 10(12), 28–38.
- Dennis Gross. (2023). What is milia: Causes & treatments.
- EBSCO. (2017). Milia. EBSCO Research Starters.
- Epstein, E., Jr. (1988). Milia induced by corticosteroids. Archives of Dermatology, 124(5), 766.
- Fernández-Quintanilla, E., et al. (2015). Ocular side-effects of topical corticosteroids: A case report and systematic review. Journal of Optometry, 8(3), 201–206.
- Givens, V., & Alexander, J. (n.d.). Milia: A review and classification [PDF]. University of Kentucky.
- Katz, A. G., & Hood, A. F. (1977). Localized milia formation on pinna due to topical steroid application. Archives of Dermatology, 113(8), 1098.
- Menter, A., et al. (2012). Mechanisms of action of topical corticosteroids in psoriasis. International Journal of Dermatology, 51(4), 389–398.
- Millar, J. (2024). Miliaria. In StatPearls. StatPearls Publishing.
- Morales-Callaghan, A. M., Jr., et al. (1998). Multiple eruptive milia: Report of a case, review of the literature, and a classification. Journal of the American Academy of Dermatology, 39(2 Pt 2), 300–304.
- Skin Type Solutions. (2024). Comedogenic acne causing ingredients in skin care.
- Suellyn, S. (n.d.). Pediatric milia. Medscape.
- Thornfeldt, C. R. (2021). A clinician’s guide to topical retinoids. Journal of Clinical and Aesthetic Dermatology, 14(8 Suppl), S4–S12.
- USF Health Dermatology. (2018). What are milia — and how do you get rid of them?
- Yélamos, O., et al. (2021). Topical steroid-induced perioral dermatitis (TOP STRIPED). Journal of Clinical and Aesthetic Dermatology, 14(4), 32–38.
- Berk, D. R., & Bayliss, S. J. (2008). Milia: a review and classification. Journal of the American Academy of Dermatology, 59(6), 1050–1063.
- Millar, J. (2023). Milia. In StatPearls. StatPearls Publishing.
- Törmä, H. (2011). Regulation of keratin expression by retinoids. Dermatoendocrinology, 3(3), 136–140.
- Tanno, O., et al. Nicotinamide increases biosynthesis of ceramides to improve the epidermal permeability barrier. Cited in: Baumann L. How Much Do We Really Know About Our Favorite Cosmeceutical Ingredients? Journal of Clinical and Aesthetic Dermatology
- Amperna. (2024). Milia Dos and Don’ts.
In this Article