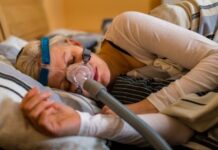
Imagine chasing a spirited toddler while battling the bone-deep exhaustion of early pregnancy. That double fatigue surprises many second-time moms, yet second pregnancy fatigue is incredibly common and rooted in real hormonal and physical changes.
This article unpacks why fatigue intensifies the second time around, explores the key triggers, and shares practical, evidence-based strategies to help you reclaim your energy safely.
What you’re feeling is not weakness, and you are not alone. Research shows that pregnancy fatigue affects the overwhelming majority of expectant mothers, with rates as high as 94% in the first trimester alone, according to UPMC HealthBeat, citing a 2023 Sleep Science study.
When you layer pregnancy fatigue with toddler demands on top of that, the exhaustion can feel relentless in ways your first pregnancy never prepared you for.
While progesterone surges and toddler demands amplify tiredness, targeted tweaks like strategic rest and nutrient-focused eating can make a real difference, helping you thrive through this phase.
Why Fatigue Hits Harder During Your Second Pregnancy

Second pregnancies often bring fatigue that feels unrelenting, striking earlier and lingering longer than the first time. This stems from your body’s intensified physiological demands combined with the realities of active motherhood, leaving less room for recovery.
A commonly searched question sums it up well: Why am I more tired in my second pregnancy? The short answer is that your body is doing two jobs at once, maintaining a pregnancy and keeping up with a young child, and it has less reserve energy to draw on than it did the first time around.
Hormonal Changes and Energy Demands
Progesterone and fatigue are closely linked. Progesterone is a hormone that rises sharply in early pregnancy to support the placenta, and it slows digestion and ramps up metabolism, which can leave you wiped out.
In a second pregnancy, these shifts can hit faster because your body recognizes the process more quickly, sometimes triggering progesterone-driven fatigue effects from as early as week four.
Resting metabolic rate increases during pregnancy as a result of increased body mass, pregnancy-associated physiological changes, and the growing fetus, according to a 2019 review in Nutrients.
One Swiss study published in the European Journal of Clinical Nutrition found that resting metabolic rate during late pregnancy was approximately 21% higher than postpartum baseline, helping explain why first-trimester exhaustion in the second pregnancy feels amplified. This fatigue can persist into the second trimester if unaddressed.
You can also expect some relief. For most women, the worst of first-trimester fatigue lifts around week 13 to 14, once the placenta is fully formed and has taken over hormone production, according to Johns Hopkins Medicine.
The second trimester is often called the “golden trimester” because energy tends to return, though managing pregnancy fatigue with a toddler can make even that window feel less restful than it did during your first pregnancy.
“Fatigue may be one of the most common first symptoms of pregnancy a woman experiences,” said Kelley Saunders, MD, an OBGYN at Banner – University Medicine Women’s Institute in Phoenix, AZ. She adds,
“It is very common and quite significant in the first trimester. For many women, this improves in the second trimester and returns in the late third trimester.”
The Hidden Workload of Motherhood
Beyond biology, the mental and physical load of parenting a toddler erodes rest opportunities. Unlike your first pregnancy, where you could nap freely, you are now managing diaper changes, meals, and playtime in the middle of nausea and exhaustion.
Research shows that new parents consistently experience fragmented sleep and increased fatigue compared to non-parent peers, and mothers carrying a second child are especially vulnerable because they are still in active caregiving mode.
A 2024 study in BMC Psychiatry found that postpartum depression risk factors for second-time mothers include the cumulative physical and emotional demands of overlapping pregnancies and early childhood care. Recovery time shrinks, turning minor tiredness into full exhaustion.
The emotional dimension matters too. Studies show that anxiety and depression rates during a second pregnancy can be just as high as, and in some cases higher than, during a first pregnancy.
Research published in Psychology Research and Behavior Management found that women in their second pregnancies experience meaningful degrees of anxiety and depression, driven by factors like relationship stress, financial pressure, and worries about managing two children.
If you notice persistent sadness, loss of interest in things you normally enjoy, or a sense of hopelessness alongside your physical fatigue, tell your prenatal provider. Prenatal mental health is just as important as physical health, and it is treatable.
Read More: Graves’ Disease in Pregnancy: Risks, Management & What You Should Know
Common Triggers That Make Exhaustion Worse

Several everyday factors compound second-pregnancy fatigue, often sneaking up on busy moms. Poor sleep from toddler night wakings or pregnancy discomfort disrupts deep rest cycles. Skipped meals lead to blood sugar dips, while quick snacks lack sustaining nutrients. Dehydration sneaks in amid constant caregiving, sapping energy further.
Imbalances like iron deficiency in pregnancy or thyroid issues can intensify symptoms. According to Mayo Clinic, iron deficiency anemia during pregnancy causes extreme tiredness, dizziness, and lightheadedness, and women who have had closely spaced pregnancies are at higher risk.
If fatigue feels extreme, request bloodwork from your provider. Here is a quick reference for spotting and addressing these triggers:
- Poor Sleep: Toddler night wakings or hip discomfort fragment rest; aim for consistent bedtimes.
- Skipped Meals: Grabbing crackers instead of balanced bites causes energy crashes.
- Dehydration: Thirst masks as fatigue; track your intake daily.
- Iron or Thyroid Imbalances: Persistent dizziness or breathlessness warrants testing; consult your OB-GYN.
Read More: How Much Choline Do You Need During Pregnancy? Benefits, Sources & Expert Recommendations
Smart Ways to Manage Second Pregnancy Fatigue

Reclaiming energy requires targeted habits that fit a toddler-filled life. Focus on rest, nutrition, movement, and hydration to counteract hormonal dips without overhauling your routine.
Prioritize Rest Strategically
Nap when your toddler does, even if it’s just 20 minutes, to recharge without guilt. First-trimester tiredness tips include sleep hygiene. Keep your room cool (around 65°F), use pregnancy pillows for side-sleeping, and dim screens an hour before bed. Set realistic expectations. Perfection isn’t the goal.
Pregnancy sleep tips from the National Sleep Foundation include creating a consistent wind-down routine, limiting fluid intake in the hour before bed to reduce nighttime bathroom trips, and using white noise or a fan to mask household sounds that might wake you after a light toddler-related disturbance.
Even short naps of 20 minutes, timed before 3 p.m., can restore alertness without disrupting nighttime sleep.
The following practices, backed by the National Sleep Foundation, can add restorative hours of sleep.
Sleep Hygiene Essentials
| Practice | Why It Helps | Quick Tip |
|---|---|---|
| 🌙 Cool, dark room | Regulates body temperature for deeper sleep | Use blackout curtains and a fan |
| 🤰 Pregnancy pillow | Supports belly and back, reducing toss-and-turn | Wedge-style for elevation |
| 📱 No screens pre-bed | Cuts blue light that suppresses melatonin | Read a physical book instead |
| ⏰ Consistent schedule | Aligns circadian rhythm with toddler’s | Bed by 10 PM, wake with sunrise |
Eat for Steady Energy
Fuel yourself with prenatal nutrition for energy: pair lean proteins like eggs or turkey with complex carbs such as oats or sweet potatoes to stabilize blood sugar. Iron-rich foods like spinach and lentils combat deficiency.
Add vitamin C from oranges or tomato juice to boost iron absorption, a tip endorsed by Mayo Clinic. Avoid sugar spikes from pastries, which worsen energy crashes, and limit caffeine to 200 mg daily as recommended by ACOG.
Sample daily plate:
- Breakfast: Greek yogurt with berries and nuts
- Snack: Apple slices with almond butter
- Lunch: Quinoa salad with chickpeas and greens
A note on supplements:
While prenatal vitamins are designed to cover your nutritional bases, they are not a substitute for dietary iron in cases of actual deficiency.
If you are experiencing fatigue beyond what feels typical, ask your provider to check your ferritin and hemoglobin levels before adding separate iron supplements. Taking unnecessary iron can cause constipation and nausea. Always confirm the need with bloodwork first.
Move Gently to Boost Circulation and Mood
Light activity fights stagnation without draining you. Walking 15 to 20 minutes daily improves circulation, and prenatal yoga eases tension. Gentle prenatal exercise releases endorphins, naturally lifting energy per ACOG guidelines, which recommend at least 150 minutes of moderate-intensity aerobic activity per week for uncomplicated pregnancies.
Start slow: chair stretches, or short walks work well if standing fatigues you.
Hydration and Micronutrients
Sip 10 to 12 cups of water daily. Dehydration mimics tiredness and compounds pregnancy sleep tips that depend on physical comfort. Prenatal vitamins cover the basics, but test for anemia if fatigue remains severe. Low-sugar electrolyte packets can help on hot days or after active toddler outings.
Read More: Cryptic Pregnancy: When You’re Pregnant and Don’t Know It – Causes, Risks & What to Do
Balancing Toddler Care with Pregnancy Rest

Integrating rest means choosing creative engagement over constant activity. Involve your toddler in quiet play like coloring on the floor while you recline, or play audiobooks during couch snuggles. Swap childcare with a friend for guilt-free naps.
Toddler-Friendly Rest Activities
These keep little ones occupied, giving you 30-plus minutes of downtime.
Quiet Play Ideas
- Puzzle sets or magnetic tiles spread on a blanket
- Sensory bins withrice and scoops, supervised from your seat
Audio and Reading
- Kid podcasts like “Wow in the World”
- Picture books read from a propped-up position
Teaching your toddler empathy naturally:
You do not need to make every quiet activity about “the new baby.” Toddlers respond better to routines and modeling than to explanations. Instead, frame rest time as something the two of you do together, reading, listening to music, doing puzzles side by side.
When you say, “Mommy needs to rest her body right now, just like when you need a nap,” you are teaching your child about self-care and body awareness in an age-appropriate way. This approach builds the groundwork for empathy without creating anxiety about an abstract sibling who has not arrived yet.
Research on second-pregnancy psychology, including a 2023 study in the Journal of Family Psychology, confirms that toddlers adapt better when transitions are introduced gradually and positively, rather than framed around displacement.
Lean on support: Ask your partner for evening wind-downs or family for weekly breaks. Set three small daily goals, like one park outing, and let go of perfectionism. Rest is not laziness during pregnancy. It is responsible self-care.
Read More: Dark Chocolate During Pregnancy: Benefits, Risks, and How Much Is Safe
When Fatigue Might Signal Something More Serious
Most tiredness is normal, but watch for red flags that may point to conditions like anemia, thyroid dysfunction, gestational diabetes, or prenatal depression. Extreme exhaustion that is unrelieved by rest, shortness of breath, dizziness, or heart palpitations all demand prompt attention.
Prenatal depression deserves special mention here. It is often mistaken for ordinary pregnancy tiredness, but persistent low mood, lack of interest in activities you usually enjoy, difficulty bonding with your toddler, or intrusive anxious thoughts are signs worth discussing with your provider.
According to research in Psychology Research and Behavior Management, women with a second pregnancy show meaningful rates of both anxiety and depression, and early intervention can significantly improve outcomes for both mother and baby. You do not have to feel this way, and asking for help is a sign of strength, not failure.
Discuss any concerning symptoms with your prenatal provider. Early intervention ensures safety. Routine screenings during prenatal visits are specifically designed to catch these conditions before they escalate.
Read More: Anemia in Pregnancy: 6 Prenatal Vitamins to Support Healthy Iron Levels
Takeaway
This intense tiredness is temporary, not a failure. Your body is building life amid real chaos, and it is doing an extraordinary thing. Embrace grace: seek support, rest proactively, and know that for most women, second pregnancy fatigue eases considerably around week 13 to 14 when the second trimester begins, and the placenta takes over, according to Johns Hopkins Medicine.
Key Takeaways:
- Hormonal surges plus toddler care double fatigue; prioritize naps and protein-rich meals.
- Fuel Smartly:Iron-rich foods, steady hydration, and gentle walks all help.
- Watch Your Mood:Prenatal depression and anxiety are common in second pregnancies and are treatable. Talk to your provider if something feels off emotionally.
- Red Flags:See your doctor promptly for signs of anemia, thyroid dysfunction, or gestational diabetes.
- Rest Strategically:Use your toddler’s nap time, frame rest as a shared activity, and lean on your support network without guilt.
With these steps, joy returns amid the demands. You have got this.
References
- Li, Y., Li, S., Jiang, Y., & Chen, Y. (2022). Psychological status during the second pregnancy and its influencing factors. Psychology Research and Behavior Management, 15, 2263–2273.
- Wuytack, F., Lynch, B., Moran, P., Fitzgerald, A. P., Corcoran, P., Begley, C., & Daly, D. (2025). The prevalence and persistence of maternal morbidities after first vs. second birth: A prospective cohort study in Ireland. PLOS ONE, 20(10), e0332891.
- Wang, X., Zhang, Y., & Li, Q. (2021). Psychological resilience of second-pregnnancy women in China during the COVID-19 pandemic. Asian Nursing Research, 15(2), 93–99.
- Mørkved, S., & Bø, K. (2007). Muscle strengthening exercises during pregnancy are not effective in reducing pelvic girdle pain: A randomized controlled trial. Acta Obstetricia et Gynecologica Scandinavica, 86(1), 71–78.
- Chen, Y., Wang, J., & Liu, H. (2024). Association of the second birth mode of delivery and interval between two births with the risk of postpartum depression. BMC Psychiatry, 24(1), Article 184.
- Handa, V. L., Blomquist, J. L., & Muñoz, A. (2020). Are there differences in pain intensity between two consecutive vaginal births? American Journal of Obstetrics and Gynecology, 222(3), S614.
- Zhang, L., Li, X., & Wang, Y. (2024). Physical activity trajectory during pregnancy and postpartum weight retention: A prospective cohort study. Scientific Reports, 14(1), Article 51648.
- Kwon, E. J., Kim, Y. H., & Lee, Y. J. (2025). The examination of the relationship between the number of pregnancies and postpartum depression. Journal of Affective Disorders.
- Smith, C. A., Levett, K. M., & Dahlen, H. G. (2021). Effectiveness of non-pharmacological interventions for fatigue in pregnancy: A systematic review and meta-analysis. Women and Birth, 34(5), 439–449.
- Li, Q., Wang, Y., & Zhang, X. (2020). Comparisons on perinatal depression between the first- and second-time mothers. Journal of Psychosomatic Obstetrics & Gynecology, 41(3), 179–186.
- Al-Shaikh, G. A., Ibrahim, G. H., & Fayed, A. A. (2013). Effect of grand multiparity on pregnancy outcomes in women younger than 35. Saudi Medical Journal, 34(8), 845–850.
- Collins, M. R., & Habib, A. S. (2015). Pain management in pregnancy: Multimodal approaches. Current Opinion in Anaesthesiology, 28(3), 268–273.
- Vardi, J., & Harlap, S. (2017). Previous pregnancy outcomes and subsequent psychosexual function. Journal of Psychosomatic Research, 94, 1–7.
- Goldfarb, J. (2023). Will I love my second baby as much as my first? Maternal bonding in multiparous women. Journal of Family Psychology.
- Alam, M. S., & Khan, L. A. (2023). Postnatal maternal risks among multiparous women: A comparative study. Journal of Clinical Medicine and Research Open, 5(2), 1–7.
- Handa, V. L., Nygaard, I. E., & Jelovsek, J. E. (2025). Symptoms of pelvic floor dysfunctions during pregnancy and postpartum. Obstetrics & Gynecology.
- Scott, J. R. (1999). Work and pregnancy: The role of fatigue and the “second shift”. American Journal of Obstetrics and Gynecology, 181(5), 1218–1223.
In this Article