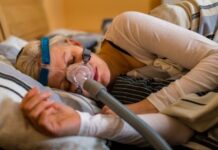
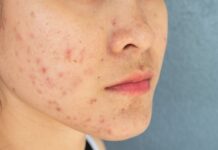
Melanin, the pigment that colours our skin, also protects it against the sun’s rays by acting as a natural sunscreen: it screens off the sun and reduces the risk of any sunburn and longer-term skin damage.
However, the exact protective mechanism reduces the skin’s ability to synthesize vitamin D from sunlight; thus, people with darker skin need more sun exposure to produce the same amount of vitamin D as people with lighter skin.
For many years, lighter-skinned populations have been the primary source of data used to set vitamin D recommendations because they can produce sufficient vitamin D with minimal sun exposure.
This approach has unintentionally overlooked the specific needs of people with darker skin, who may need to be exposed to the sun longer than others and have greater dietary requirements to maintain their vitamin D levels.
In this article, we’ll examine the connection between melanin and vitamin D production, the health risks associated with reduced levels of both substances, and ways to keep vitamin D levels balanced regardless of skin color.
Read More: The Sunlight Diet: Can Eating Seasonally Improve Your Health?
The Melanin–Vitamin D Connection Explained
The quantity of melanin also determines a person’s vitamin D level in their skin; the more melanin, the darker the skin tone. The skin is lighter when there is less melanin.
The amount of melanin in skin impacts vitamin D status because the skin depends on UV rays to produce vitamin D, and darker skin limits its production. It takes around 15 mins in the sun for a person with lighter skin to make enough vitamin D for the day, whereas a person with a darker complexion needs 30 minutes to 3 hours.
Melanin shields cells from sun-induced DNA damage by absorbing harmful UV radiation.
How Melanin Acts as a Natural Sunscreen
Melanin is a biopolymer that principally performs three functions: photoprotection, pigmentation, and redox activity. To put it another way, melanin serves as the body’s first line of defense against the sun’s damaging UV rays, contributes to the pigmentation of our skin, hair, and eyes, and supports a range of physiological processes, including metabolism.
Melanin absorbs UV radiation incident on the skin, converting its energy into heat. It is crucial to shield cells from UV radiation before it can harm them or cause cancer. Melanin is also environmentally favorable because it is biodegradable, unlike commercial sunscreen.
Why People with Higher Melanin Need More Sun Exposure
Darker skin includes more melanin, which means more UVB light is absorbed before it can activate vitamin D production. While vitamin D production is not impossible as a result of this, it also implies a less efficient method of producing it. Due to this limitation, those with higher levels of melanin require more prolonged exposure to produce sufficient vitamin D.
Latitude and Lifestyle Limitations
The production of vitamin D in our body is affected by our lifestyle choices and the geography of the location we reside in. At higher latitudes during some months, the sun’s rays are not powerful enough to produce high levels of UVB.
Life circumstances (living in densely built urban environments, spending the vast majority of the day indoors, and avoiding sun exposure with protective clothing and sunscreen) further limit sun exposure and increase the risk of deficiency across all skin tones.
The Hidden Gap in Traditional Vitamin D Guidelines

In the global conversation on micronutrient shortages, vitamin D has historically been eclipsed by the “Big Three”: iron, iodine, and vitamin A. The dominant notion, fueled by “sunlight paradox,” holds that populations residing in equatorial regions with year-round ultraviolet B (UVB) radiation inherently have adequate vitamin D levels.
Ethiopia is currently facing a silent epidemic of vitamin D deficiency (VDD), according to a comprehensive synthesis of epidemiological data, clinical practice patterns, and health system evaluations. As a result, many individuals may be unwittingly under-supplemented or receive insufficient sun exposure to meet their body’s specific needs.
Narrow Focus on Bone Health
Vitamin D plays a crucial part in protecting your bones. It may also help prevent other illnesses, including some malignancies. Your body requires vitamin D to absorb the calcium. Both adults and children need vitamin D to maintain healthy, strong bones. When people do not obtain enough vitamin D, they can lose bone density.
Research indicates that individuals having low vitamin D levels have reduced bone mass or density. As they get older, they also have a higher risk of breaking bones.
Missed Public Health Opportunity
By failing to account for skin tone, geography, or lifestyle factors, existing vitamin D recommendations contribute to preventable health inequalities. Infections, chronic illnesses, and other health issues may be more common among populations who are more vulnerable to deficiencies.
Read More: 10 Health Benefits Of Sunlight You Definitely Need To Know
Why Vitamin D Deficiency Matters for Respiratory Health
Our bodies are built to thrive when we eat appropriately, exercise, and get the nutrients and vitamins we need. Unfortunately, our busy schedules and junk-food appetites sometimes result in less-than-ideal health. In addition to its well-known function of bone health, vitamin D is essential for immune system regulation.
Vitamin D is like fuel for the immune system. It helps battle inflammation, specifically in the lungs. Some studies even show that increased vitamin D intake reduces the risk of getting the common cold. But it’s not the only strategy for staying healthy and protecting yourself from illness.
Increasing research demonstrates that optimal vitamin D levels, whether from sunlight exposure or supplementation, can reduce any asthma symptoms and severity among individuals with inadequate vitamin D levels.
Vitamin D’s Role in the Immune System
Vitamin D plays a role in immunity through multiple processes and helps regulate both innate and adaptive immune responses. By interacting with vitamin D receptors on innate immune cells throughout the body, vitamin D affects immunological health.
The body’s initial line of non-specific protection against foreign pathogens is the innate immune system. By regulating immune cells that trigger antiviral responses, vitamin D strengthens immunity and supports the fight against infection. Vitamin D binds to receptors on immune cells, like neutrophils, macrophages, and natural killer cells.
Deficiency and Infection Risk
Severe vitamin D insufficiency is associated with a higher risk of hospitalization for respiratory tract infections, such as bronchitis and pneumonia, according to a new study by scientists from the University of Reading.
Scientists found that those with a severe vitamin D deficiency were 33 percent more likely to be admitted to the hospital for their treatment than those with a sufficient level of vitamin D.
Higher Melanin, Higher Risk
Those with higher melanin levels naturally produce vitamin D more slowly, meaning insufficiency is more common in these populations, especially when combined with limited sun exposure or residence at higher latitudes. As a result, these groups may represent modifiable targets for vitamin D interventions aimed at reducing the risk of respiratory infections and their complications.
Read More: What People Who Rarely Get Sick Do Every Morning
Beyond Sunlight — Additional Risk Factors for Low Vitamin D

While sunshine is a primary source for vitamin D for most people, various environmental, dietary, and lifestyle factors can increase the risk of any deficiency, especially among people of color. Even when sun exposure is adequate, other factors may prevent the body from achieving sufficient levels, so vigilance and management are key.
Dietary Patterns and Fortification Gaps
Always remember that although vitamin D occurs naturally in very few food sources, it is found in fatty fish, egg yolks, and liver, and most people thus get their vitamin D from fortified foods (such as milk or cereals) and other sources. However, some people consume smaller amounts of these fortified foods, either due to dietary choices or restricted availability, increasing the chance of insufficiency.
Lactose Intolerance and Nutrient Gaps
Lactose intolerance is more widespread among some ethnic groups, which may limit the intake of fortified dairy products, a significant source of dietary vitamin D. Without alternative sources or supplements, individuals may struggle to maintain optimal levels, even with ample sun exposure.
Cultural and Occupational Influences
Wearing clothing that covers the majority of skin due to any cultural or religious beliefs, working indoors, and regularly using sunscreen can all lower UVB exposure, which further restricts the production of vitamin D.
These lifestyle and cultural factors, together with higher melanin levels, may make achieving optimal vitamin D status more challenging for many people of color.
How to Identify and Address Vitamin D Deficiency

Awareness of and screening for vitamin D deficiency are critical for health, particularly for the immune system and defense against respiratory viruses. Take the appropriate steps, and you can monitor your own health and take action to ensure you’re adequately protected.
When to Test
A straightforward blood test is usually sufficient to detect a deficit. Talk to your doctor about scheduling the vitamin D test. The 25-hydroxy vitamin D blood test is the most precise method of determining your body’s vitamin D levels. Many experts consider the optimal range to be 40-80 ng/mL, with values below 20 ng/mL considered inadequate.
Target Levels and Supplementation
Optimal vitamin D serum levels are generally estimated to be 40–60 ng/mL. Doctors who specialize in this usually use blood test results to guide supplementation safely and correctly, even though the amounts vary widely, so you do not end up over-supplementing.
Nutrition and Safe Sun Habits
Addressing the deficit needs a combination of measures. Dietary sources like fatty fish, eggs, and fortified meals can help improve intake. Additionally, moderate, balanced sun exposure while following skin safety guidelines supports natural vitamin D production.
Read More: Why You Should Take Vitamin K2 With Vitamin D3: The Synergistic Duo for Bone & Heart Health
Rethinking Public Health Recommendations
Current guidelines for vitamin D assume a “one size fits all” approach, but they too do not fully reflect the needs of diverse populations. By taking into account factors such as skin pigmentation, geography, lifestyle, and cultural practices, policies can be better designed to promote equity and eliminate unnecessary burdens of vitamin D deficiency diseases.
Tailoring Vitamin D Policies by Population
Health professionals must personalize vitamin D approaches based on their age, skin pigmentation, location, and pre-existing medical conditions to address the high deficiency rates in the general population. Key components are dietary fortification and supplying at-risk groups with daily supplements and, in some cases, a personalized dose that might elevate, say, heart health.
Education and Awareness
Primary care providers have a very critical role in managing vitamin D insufficiency. Besides informing patients about dietary sources, safe sun exposure, and the use of supplements, routine screening for at-risk populations allows individuals to take proactive steps before developing problems associated with nutrient deficiencies.
The Role of Community Health Campaigns
Public health campaigns help improve engagement and address knowledge gaps. These campaigns increase vitamin D knowledge by adapting their messages to the different types of people they intend to reach based on their lifestyle trends, dietary preferences, and cultural norms.
Read More: Best Light Therapy Lamps for Dementia Patients: What to Look For + Top Picks
Conclusion
Not only strong bones, but also a resilient immune system and protection from infections of the lungs and airways rely on vitamin D. And because melanin decreases the skin’s ability to absorb vitamin D from sunlight, those with darker skin are at heightened risk of deficiency. Traditional vitamin D guidelines may not meet everyone’s needs, as they were primarily developed for people with lighter skin.
The good news is that you can boost vitamin D levels through a mix of safe sun exposure, vitamin D-rich foods, fortified products, and, when needed, supplementation under medical care.
References
- Shi, L., & Lin, H. (2022, May 11). What effect do melanin and sunscreen have on vitamin D levels?
- Fickman, L. (2023, September 2). Study finds low vitamin D levels in young people of color
- Lebron, S. (2023). DIY: Sunscreen — Using melanin in the making of “ultra-protective” sunscreen.
- National Osteoporosis Foundation. (2013). Vitamin D and bone health.
- Minkowitz, B. Vitamin D for good bone health.
- Glen Park Dental. (2020, June 22). This vitamin could improve your respiratory health.
- SOLIUS Medical Light Therapy. The role of vitamin D in the immune system.
- Ropte, M., DO. How to spot a vitamin D deficiency.
In this Article