You wake up, glance in the mirror, and notice the same crease under your eyes. It doesn’t look like a typical fine line. It’s deeper. More defined. And oddly, it’s been there since your twenties, maybe even earlier. Here’s the thing: not all under-eye lines are caused by aging.
Some are the physical leftovers of chronic allergies, eczema, or years of irritated, itchy eyes. These lines have a name: Dennie-Morgan lines. And once you know what they are, you start seeing them everywhere.
Dermatologists have recognized these folds for decades, especially in people with allergic conditions such as allergic rhinitis, asthma, and atopic dermatitis. Yet most people mistake them for early wrinkles or assume they’re purely genetic. That confusion matters because treating allergy-related under-eye folds is very different from treating age-related wrinkles.
Dennie-Morgan lines aren’t just cosmetic. They’re a visible sign of long-term inflammation, rubbing, swelling, and fluid shifts under the eyes. Over time, that repeated stress changes the structure of the skin, making the fold deeper and more permanent.
This article breaks down what Dennie-Morgan lines really are, why allergies can permanently change the skin under your eyes, how to tell them apart from normal wrinkles, and what actually helps reduce or prevent them. No hype. No skincare myths. Just the science, explained clearly, so you know exactly what you’re dealing with and what actually works.
What Are Dennie-Morgan Lines?

Dennie-Morgan lines are infraorbital creases that form beneath the lower eyelids. They usually show up as one or two distinct horizontal folds running just below the eye, separate from crow’s feet or fine expression lines at the outer corners. In some people, they’re subtle. In others, they’re deep and clearly defined. Either way, once you know what they look like, you start recognizing the same pattern again and again.
Clinically, these lines are most often seen in people with chronic allergic or inflammatory conditions, especially allergic rhinitis, atopic dermatitis (eczema), asthma, and long-standing environmental or seasonal allergies. They’re also common among people who experience persistent eye irritation or allergic conjunctivitis. That connection isn’t a coincidence. It’s central to why these lines form in the first place.
The folds were first described in the 1950s by dermatologists Dr. Charles Dennie and Dr. Donald Morgan while they were studying physical signs associated with atopic disease. What stood out to them was how consistently this under-eye crease appeared in patients with chronic allergies. Since then, Dennie-Morgan lines have been recognized as a cutaneous marker of long-term allergic inflammation, not just a cosmetic flaw or a sign of early aging.
That’s what makes them different from normal wrinkles. Unlike age-related lines, Dennie-Morgan lines can show up in childhood or adolescence, long before collagen loss becomes a factor. They tend to be fairly symmetrical under both eyes and are closely linked to itching, swelling, and repeated eye rubbing.
They often appear alongside allergic shiners, those dark under-eye circles caused by venous congestion, and other eczema-related skin changes, such as dryness, redness, or thickened skin. And unlike typical fine lines, they don’t fade much with moisturizer or disappear when your face relaxes.
The reason allergies can permanently carve these folds into the skin comes down to chronic stress on very delicate tissue. Ongoing inflammation weakens collagen and elastin. Swelling stretches the under-eye skin repeatedly.
Fluid buildup changes how tension is distributed across the area. Add years of rubbing itchy eyes into the mix, and you get repeated micro-trauma followed by imperfect healing. Over time, that cycle reshapes the skin’s structure and locks in a permanent crease.
Dennie-Morgan lines are considered a classic but underrecognized sign of atopic disease, especially in people with long-standing nasal or ocular allergies. They’re not dangerous, but they are a visible clue that allergic inflammation has been shaping the skin for years.
Why Allergies Can Permanently Change Under-Eye Skin
Here’s the part most people miss: allergies don’t just cause temporary puffiness or redness. When they keep flaring year after year, they can physically remodel the skin under your eyes. That area is incredibly thin, delicate, and poorly supported to begin with.
Add chronic inflammation, constant swelling, and habitual rubbing into the mix, and you get a slow, cumulative breakdown of the skin’s structure. Over time, the tissue loses its ability to snap back into place. Instead, it settles into a permanent fold.
This is the biological chain reaction behind Dennie-Morgan lines, and it’s why treating them like ordinary wrinkles completely misses the real cause.
The Inflammatory Cycle
Allergies trigger an immune response. When your body encounters allergens like pollen, dust mites, or pet dander, mast cells release histamine and other inflammatory mediators.
That histamine response causes:
- Itching
- Redness
- Swelling
- Increased blood vessel permeability
The skin under the eyes is among the thinnest on the body, measuring less than 0.5 mm thick. According to research published in Clinical Reviews in Allergy & Immunology and related skin-biology studies, chronic inflammation alters collagen structure and increases the activity of matrix‑degrading enzymes in the skin, accelerating the breakdown of collagen and elastin and making the tissue far more vulnerable to folding and creasing over time.
According to Dr. Peter A, Lio, MD, a clinical assistant professor of dermatology and pediatrics at Northwestern University Feinberg School of Medicine, “Wherever there is inflammation in the skin, the barrier is in trouble a lot of times.”
This underscores how chronic allergic inflammation, especially when repeated over years, can weaken structural proteins and the skin’s protective layer, making thin, delicate areas like the eyelids more vulnerable to creasing and visible changes.
Once collagen support is compromised, the skin doesn’t bounce back the way it used to. Instead, it settles into folds.
The “Allergic Salute” Effect
If you’ve ever rubbed your eyes during allergy season, you’re not alone. Chronic eye rubbing is so common in patients who are allergic that clinicians have a term for it: the allergic salute. Repeated mechanical stress does real damage.
A study in The Journal of Investigative Dermatology found that chronic friction and stretching of the skin alter fibroblast activity, reducing collagen synthesis while increasing inflammatory signaling. Over the years, that mechanical trauma deepens existing creases and turns temporary folds into permanent lines.
Kids with uncontrolled allergies are particularly vulnerable. Pediatric dermatologists often see Dennie-Morgan lines develop before puberty, long before aging would normally play a role.
Fluid Retention and Circulatory Stasis
Allergies don’t just irritate the skin. They also affect circulation.
Nasal congestion impairs venous and lymphatic drainage around the eyes, leading to:
- Periorbital edema
- Blood pooling under thin skin
- Bluish or purplish discoloration known as allergic shiners
According to clinical literature on allergic inflammation and periocular changes, chronic under‑eye swelling from conditions like allergic rhinitis repeatedly stretches the delicate skin around the eyes.
This repeated edema and inflammation contribute to more prominent folds over time, making temporary creases appear deeper even after swelling subsides, a pattern commonly seen alongside Dennie‑Morgan folds in people with long‑standing allergies.
Think of it like bending paper over and over. Eventually, a crease forms.
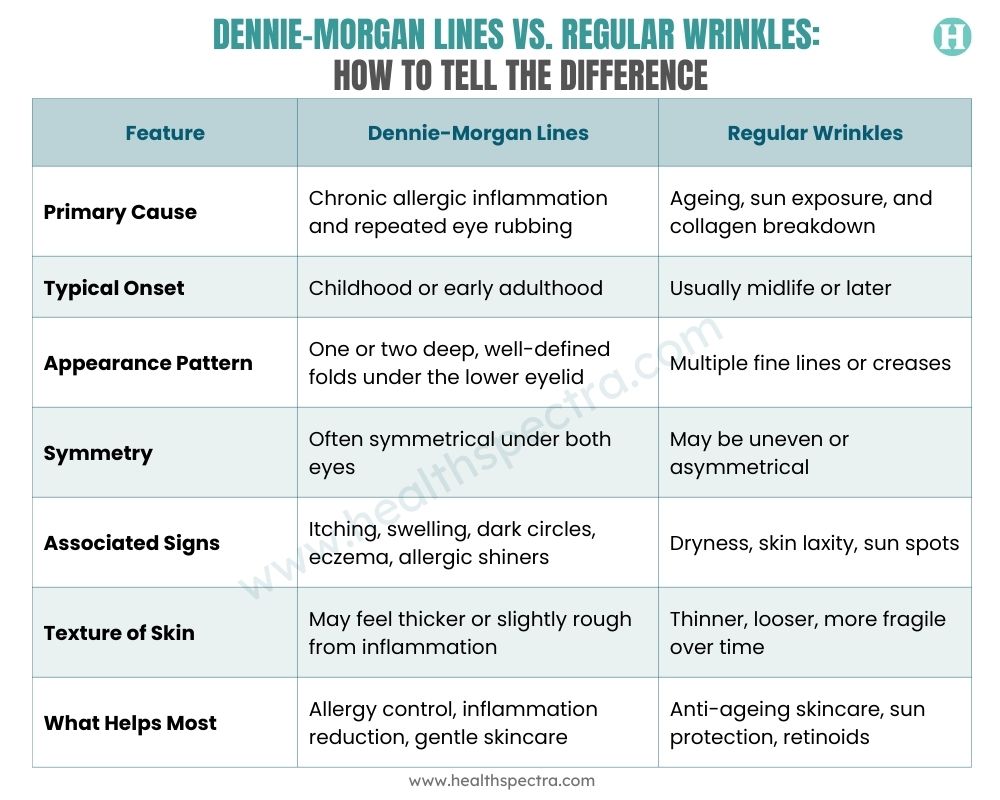
Dennie-Morgan Lines vs. Regular Wrinkles: How to Tell the Difference
At first glance, Dennie-Morgan lines can look like early wrinkles. That’s why so many people treat them with anti-aging creams and get frustrated when nothing changes. But these two types of lines come from completely different biological processes.
One is driven by inflammation and mechanical stress from allergies. The other is driven by time, sun damage, and collagen loss. Once you understand the differences, it becomes much easier to tell what you’re actually dealing with and why the right treatment approach matters.
 Here’s what this really means. Both can exist at the same time.
Here’s what this really means. Both can exist at the same time.
If you’ve had allergies for decades and also spent years in the sun without sunscreen, you may see a combination of Dennie-Morgan lines and true age-related wrinkles. Treating only one side of the equation won’t fully address the problem.
How to Reduce or Prevent Allergy-Related Under-Eye Folds

Here’s the honest truth: you can’t fix Dennie-Morgan lines by treating them like normal wrinkles. If the inflammation and irritation that created them are still active, no cream, serum, or gadget is going to make a meaningful dent. Real improvement starts by stopping the damage, then helping the skin rebuild what it’s lost.
That means controlling allergies, protecting the fragile skin barrier, reducing chronic swelling, and only then layering in collagen-supporting care. This approach won’t erase the lines overnight, but over time, it can soften their depth and prevent them from getting worse.
1. Control Allergic Triggers
This is non-negotiable. You cannot out-moisturize active inflammation.
Research summarized in clinical allergy reviews shows that controlling allergic inflammation through appropriate therapies (antihistamines, mast‑cell stabilizers, immunotherapy) significantly reduces the signs and symptoms of allergic conjunctivitis, including swelling and irritation around the eyes. These findings are foundational to the recommendations that clinicians make for long‑term allergy management.
Key strategies include:
- Identifying triggers through testing
- Using oral or intranasal antihistamines as directed
- Managing indoor allergens with HEPA filters and frequent washing
According to the Mayo Clinic, untreated allergic rhinitis is a major contributor to chronic under-eye changes, especially in children.
2. Protect and Repair the Skin Barrier
Inflamed skin loses moisture faster and heals more slowly.
Dermatologists recommend:
- Fragrance-free, ceramide-rich moisturizers
- Avoiding harsh activities near the eyes
- Never use topical steroids unless specifically prescribed
According to a randomized controlled trial published in Dermatitis‑related clinical literature, ceramide‑based formulations significantly improved skin barrier function in individuals with atopic dermatitis within four weeks, as measured by reductions in transepidermal water loss and increases in skin hydration, underscoring their role in repairing barrier dysfunction.
Cold compresses can help with itching without the mechanical damage of rubbing. Press gently. Don’t drag.
3. Reduce Inflammation and Swelling
For eczema-related cases, non-steroidal anti-inflammatory options may be used under medical guidance.
Topical calcineurin inhibitors like tacrolimus or pimecrolimus have been shown to:
- Reduce eyelid inflammation
- Improve skin thickness
- Lower flare frequency
According to a review in The British Journal of Dermatology, the overall safety of topical therapies for atopic dermatitis appears good, and systemic complications with non‑steroidal agents are uncommon compared with the documented side effects of topical corticosteroids when used in sensitive areas.
This supports the idea that steroid‑sparing agents (including ceramide‑based or calcineurin‑based formulations) are often preferred for long‑term use on thin or delicate skin such as eyelids.
Lifestyle matters too. Sleeping with your head slightly elevated improves overnight fluid drainage and reduces morning puffiness.
4. Support Collagen and Circulation
Once inflammation is controlled, structural support becomes important.
Dermatologists often recommend:
- Low-strength retinoids formulated for the eye area
- Peptide-based eye creams
- Daily mineral sunscreen around the eyes
According to research in Dermatologic Surgery and related photoaging studies, consistent sun protection helps prevent repeated UV‑induced degradation of collagen and fibroblast dysfunction that drives skin aging and deepening of creases.
By minimizing chronic UV exposure, a major factor in collagen breakdown and extracellular matrix damage, broad‑spectrum photoprotection slows the structural changes that make skin more prone to permanent lines over time.
No product will erase Dennie-Morgan lines overnight. But over months, supportive care can soften their appearance.
Read More: The Dangers of Excessive Eye Rubbing: 7 Hidden Risks You Should Know!
When to See a Dermatologist or Allergist
You should seek medical advice if:
- Under-eye lines worsen despite skincare
- You notice redness, burning, or flaking
- Swelling becomes painful or asymmetric
- There’s discharge or signs of infection
Periorbital dermatitis and cellulitis require prompt evaluation. Ignoring chronic symptoms often leads to deeper, more permanent skin changes.
The upside? Treating the underlying allergy often improves the appearance of these lines over time, especially in younger patients.
Read More: 8 Innovative Products for Maintaining Eye Health
The Takeaway
Dennie-Morgan lines are not just wrinkles. They’re visible markers of chronic allergic inflammation, mechanical stress, and impaired skin repair. In other words, they’re not a cosmetic accident. They’re the skin’s long-term response to years of itching, swelling, rubbing, and immune activity under one of the thinnest, most fragile areas of the body.
That’s why treating them like ordinary fine lines almost always fails. Eye creams aimed at aging alone can’t undo the damage that’s being actively driven by allergies. If the underlying inflammation isn’t controlled, the skin never gets a real chance to rebuild collagen, restore elasticity, or hold its structure.
The earlier allergies are managed, the better the long-term outcome for under-eye skin. That’s especially true for kids and young adults, where these lines can start forming long before aging would normally play a role.
Gentle care, barrier repair, and medical guidance matter far more than aggressive cosmetic fixes. The goal isn’t to scrub or “resurface” the fold-away. It’s to calm the immune response, stop the mechanical trauma, and support the skin so it can slowly regain strength.
If your under-eye lines showed up long before the rest of your face caught up, allergies may be the real story behind them. And once you see them through that lens, the path forward becomes clearer. Control the inflammation first. Protect the skin second. Then, and only then, worry about softening what’s already there.
Because when you treat the cause rather than just the crease, real improvement finally makes sense.
FAQs: People Also Ask
What are Dennie-Morgan lines?
Dennie-Morgan lines are horizontal folds that form under the lower eyelids and are most commonly seen in people with allergies, eczema, or chronic eye irritation. Unlike typical wrinkles, they’re driven by inflammation and repeated mechanical stress rather than by aging alone. They can appear in childhood or early adulthood and tend to be fairly symmetrical under both eyes.
Are Dennie-Morgan lines permanent?
Dennie-Morgan lines can become permanent if inflammation, swelling, and eye rubbing continue for years without control. Once collagen and elastin are weakened, the skin loses its ability to fully snap back into place. Early allergy management and gentle skin care can soften their appearance and slow their progression, but deeply established folds are difficult to erase completely.
Do Dennie-Morgan lines mean I have allergies?
They’re strongly associated with allergic conditions like hay fever, asthma, and atopic dermatitis, but they’re not a diagnosis by themselves. Some people develop similar folds due to chronic eye irritation, even without classic allergy symptoms. A proper medical evaluation is needed to confirm whether allergies are the underlying cause.
Can skincare alone fix allergy wrinkles under the eyes?
No. Skincare can support healing and improve texture, but it can’t override active allergic inflammation. If the underlying allergy triggers aren’t controlled, creams and serums will have limited impact. Real improvement depends on calming the immune response first, then protecting the skin barrier and supporting collagen over time.
Do children get Dennie-Morgan lines?
Yes. They often appear in children with uncontrolled allergic rhinitis or atopic dermatitis, long before normal aging would play any role. Chronic itching, swelling, and habitual eye rubbing drive their early formation. Managing allergies early can prevent these folds from deepening and becoming permanent later in life.
References
- Clinikally. (n.d.). Dennie-Morgan lines: Understanding and overcoming under-eye concerns.
- Eczema and Inflammatory Skin Disease Center. (n.d.). Additional clinical features. Rady Children’s Hospital San Diego.
- Longevita. (n.d.). Dennie-Morgan lines.
- Oreat EAI. (n.d.). Beyond the rub: Understanding Dennie-Morgan lines and allergic rhinitis in children.
- Patel Plastic Surgery. (n.d.). What are Dennie-Morgan lines and how do you treat them?
- RealSelf. (n.d.). Dennie-Morgan lines.
- The Eczema Store. (n.d.). What are Dennie-Morgan lines?
- Worldwide Journals. (2021, September). Atopic dermatitis – an overview. Indian Journal of Applied Research (IJAR).
- ScienceDirect. (1999). Cutaneous manifestations associated with atopy.
- ScienceDirect. (2025). Multifaceted roles of dermal fibroblasts in skin. Dermatologic Surgery.
- Oxford Academic. (2007). Safety of topical therapies for atopic dermatitis. British Journal of Dermatology, 156(2), 203–215.
- PubMed Central. (2018). Efficacy of ceramide-based formulations in atopic dermatitis.
- PubMed Central. (2005). Allergic shiner: Clinical overview.
- PubMed. (2021). Mechanotransduction in human skin fibroblasts under stress.
- ScienceDirect. (2015). Chronic inflammation accelerates collagen degradation.
- Wikipedia contributors. (n.d.). Allergic shiner.
- Wikipedia contributors. (n.d.). Dennie–Morgan fold.
In this Article