You finish a meal expecting to feel satisfied. Instead, about an hour later, your hands start shaking. Your heart races. You feel lightheaded, sweaty, irritable, and weirdly anxious. Someone says, “Sounds like low blood sugar.”
So you check. And your glucose is normal. This condition is termed “idiopathic postprandial syndrome.” It seems like a sugar crash. It feels like hypoglycemia. But it isn’t.
Idiopathic postprandial syndrome (IPS) is a recognized condition where hypoglycemia-like symptoms appear after eating, even though blood sugar stays in the normal range. Doctors sometimes call it postprandial adrenergic syndrome because the symptoms are driven more by stress hormones like adrenaline than by an actual drop in glucose.
IPS isn’t dangerous in the way true hypoglycemia is, but it can be disruptive, scary, and deeply confusing if you don’t know what’s happening.
This article breaks it down clearly. What IPS actually is. Why does it happen? How is it different from reactive hypoglycemia? And what actually helps stop the post-meal shakes and adrenaline surges.
The write-up explains the physiology in simple words, so you can finally make sense of what your body is doing after you eat.
What Is Idiopathic Postprandial Syndrome (IPS)?

Idiopathic postprandial syndrome is a condition marked by hypoglycemia-like symptoms after meals, even though blood sugar never actually drops into a true hypoglycemic range.
In medical terms, it’s defined as postprandial adrenergic syndrome, a condition where symptoms occur post-meal without documented hypoglycemia. Symptoms are driven more by stress hormones like adrenaline than by an actual drop in glucose.
“Idiopathic” means the exact root cause isn’t fully understood. “Postprandial” means after eating. And syndrome means it’s a consistent, recognizable cluster of symptoms rather than a one-off reaction. Put together, IPS describes a pattern where the body behaves as if blood sugar were crashing, even when lab values say everything is technically normal.
People with IPS experience the classic signs of low blood sugar, including shakiness, sweating, rapid heartbeat, lightheadedness, irritability, weakness, and anxiety. The key difference is that when glucose is checked during these episodes, it typically stays above 70 mg/dL, which is the clinical cutoff used to define true hypoglycemia.
In other words, the symptoms are real, but they’re not being caused by an actual glucose deficit. IPS is also referred to by a few other names in medical literature, including pseudohypoglycemia and adrenergic postprandial syndrome.
Those alternate terms point to what’s really driving the experience: an exaggerated adrenaline response after meals rather than a dangerous drop in blood sugar.
According to the Cleveland Clinic, IPS is more common than true reactive hypoglycemia in people without diabetes, yet it’s frequently misdiagnosed or brushed off as anxiety.
The symptoms are real. The physiology is real. The difference lies in what’s driving them. In IPS, it’s not low glucose that’s causing the crash feeling. It’s a mismatch between how fast the body handles a meal and how strongly the nervous system reacts to it.
Why You Feel “Low” After Eating, Even With Normal Blood Sugar

After you eat, carbohydrates are broken down into glucose. Blood sugar rises. In response, the pancreas releases insulin, which helps move glucose out of the bloodstream and into cells to be used for energy or stored for later.
In a healthy, well-regulated system, this physiological process is smooth and uneventful. Blood glucose rises modestly after a meal, insulin responds in proportion to that rise, and glucose levels drift back toward baseline without any dramatic swings. Most people never feel these changes.
But here’s the part most people don’t realize: your body doesn’t just monitor how high or low your blood sugar is. It also tracks how fast it’s changing.
Research published in The Journal of Clinical Endocrinology & Metabolism shows that a rapid decline in blood glucose, even when levels stay well within the normal range, can trigger adrenergic symptoms in susceptible individuals. In other words, your nervous system may react to the speed of the drop, not just the final number.
So even if your glucose never falls low enough to meet the clinical definition of hypoglycemia, your brain can still interpret a sharp post-meal dip as a threat. When that happens, it flips on your stress response.
That stress response is what creates the familiar “low blood sugar” feeling: shakiness, sweating, a racing heart, lightheadedness, irritability, and sudden anxiety. Your sugar isn’t actually low. Your body just thinks it is.
Possible Mechanisms Behind Idiopathic Postprandial Syndrome
IPS isn’t caused by one single defect or disease. It’s more like a perfect storm of small physiological quirks that stack together and push the body into an exaggerated stress response after meals.
In people with IPS, normal post-meal glucose changes are misread by the nervous system as a threat, which triggers adrenaline-driven symptoms even though blood sugar never actually becomes low.
- Exaggerated insulin response: High-glycemic or refined carbohydrate meals can trigger a fast, oversized insulin release. Blood sugar then falls quickly afterward, even though it stays within the normal range. That rapid drop is often enough to activate the body’s counterregulatory stress response.
- Rapid glucose decline within the normal range: The speed of the fall appears to matter more than the final number. A quick drop from a higher post-meal level to a normal one can feel worse to the brain than a slow, steady return to baseline, even when glucose remains perfectly safe.
- Heightened adrenergic sensitivity: Some people’s sympathetic nervous systems are more reactive than average. When their brains sense a glucose dip, they release adrenaline and noradrenaline more aggressively, which drives symptoms like shaking, palpitations, sweating, and sudden anxiety.
- Gut hormone signaling effects: Incretin hormones such as GLP-1 influence insulin secretion and gastric emptying. In some individuals, these hormones amplify post-meal insulin spikes and glucose swings, making the whole system more volatile after eating.
- Impaired counterregulatory timing: The hormones that normally stabilize blood sugar, like glucagon and cortisol, may fire too early or too strongly, overshooting what the body actually needs and intensifying adrenergic symptoms.
Idiopathic postprandial syndrome isn’t about blood sugar dropping too low. It’s about the body overreacting to normal post-meal glucose shifts. A fast glucose decline, a strong insulin response, and a hypersensitive stress system combine to create symptoms that feel like hypoglycemia without being dangerous.
Once you see IPS as a timing and sensitivity problem rather than a sugar problem, both the confusion and the fear around it start to ease.
Read More: How Digestive Health Impacts Glucose Absorption and Diabetes
Symptoms of Idiopathic Postprandial Syndrome

Idiopathic postprandial syndrome causes sudden, often alarming symptoms after eating, even though blood sugar is normal. Common signs include shakiness, sweating, a racing heart, anxiety, dizziness, sudden hunger, irritability, fatigue, and brain fog.
Symptoms usually appear 1 to 4 hours after meals, especially those high in carbohydrates, and often peak within 15 to 45 minutes. Unlike true hypoglycemia, IPS does not cause seizures, loss of consciousness, or coma, making it uncomfortable but not dangerous.
The episodes feel dramatic because they’re driven by adrenaline, not by an actual drop in glucose, which is why understanding IPS is key to managing it effectively.
IPS vs True Hypoglycemia
At first glance, idiopathic postprandial syndrome (IPS) can feel just like true hypoglycemia. Both involve shakiness, sweating, anxiety, and other dramatic post-meal symptoms. The key difference lies in what’s driving the reaction and whether blood sugar actually drops. Understanding the distinction is crucial for effective management.
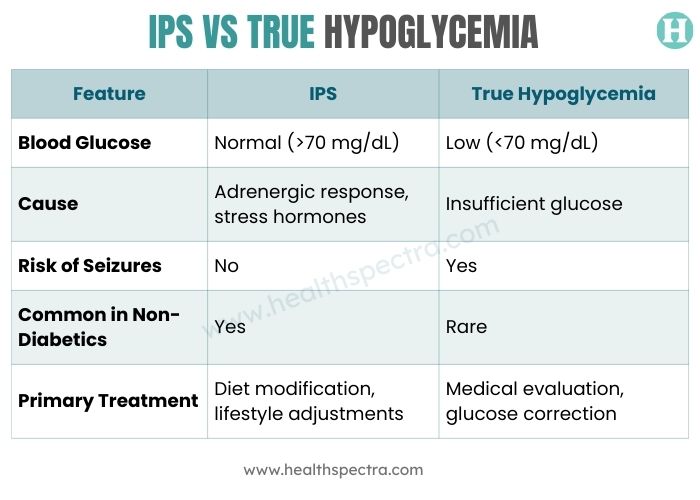 While the symptoms of IPS can feel as intense as a true sugar crash, the absence of actual hypoglycemia makes the approach to management very different.
While the symptoms of IPS can feel as intense as a true sugar crash, the absence of actual hypoglycemia makes the approach to management very different.
IPS is addressed primarily through dietary and lifestyle strategies to prevent rapid glucose swings and reduce adrenergic reactions, whereas true hypoglycemia requires medical evaluation and careful glucose correction.
Recognizing which condition you’re experiencing is the first step toward stopping post-meal anxiety and shakes without unnecessary medical intervention.
What Triggers IPS Episodes?
Idiopathic postprandial syndrome is often triggered by factors that cause rapid shifts in glucose, insulin, or stress hormones. One of the most common triggers is high-glycemic or refined carbohydrate meals, which digest quickly and spike both glucose and insulin.
Foods like white bread, pastries, sugary cereals, candy, and sweetened beverages can all provoke post-meal shakiness, even when blood sugar remains normal. Research in Nutrients confirms that these meals increase adrenergic symptoms in sensitive individuals.
Irregular eating patterns can also contribute. Skipping meals, going long periods without eating, or relying on one large late meal can make insulin and hormonal responses overshoot, increasing the likelihood of post-meal symptoms.
Alcohol and caffeine may worsen episodes. Alcohol can interfere with normal glucose regulation, while caffeine stimulates adrenaline release, intensifying shakiness, palpitations, and anxiety, especially when combined with sugary mixers.
Finally, individual sensitivity, stress, and sleep quality play a major role. Stress and sleep deprivation elevate baseline adrenaline, lowering the threshold for IPS symptoms. If you’re stressed or overtired, your body is more likely to overreact after meals. The nervous system is already revved up, so even normal blood sugar shifts can trigger symptoms.
In short, IPS is rarely caused by a single factor. Meals that spike glucose, irregular eating, stimulants, and heightened stress all interact to create the adrenaline-driven symptoms that define the condition.
How to Manage Idiopathic Postprandial Syndrome

Managing IPS isn’t about eliminating all carbohydrates or obsessively checking your glucose. It’s about stabilizing blood sugar, preventing rapid insulin spikes, and calming the nervous system so post-meal adrenaline surges don’t take over. Small, practical changes in what, when, and how you eat, along with lifestyle adjustments, can make a significant difference.
The cornerstone of IPS management is balancing your meals. Each meal should include protein, fiber-rich carbohydrates, and healthy fats to slow digestion. Choosing low–glycemic index foods such as vegetables, legumes, whole grains, nuts, and seeds helps prevent rapid glucose swings.
As Cleveland Clinic dietitian Julia Zumpano explains, “Low-glycemic index foods are complex carbohydrates, high in fiber and protein. These foods create a gradual rise and gradual drop in blood sugar levels as opposed to those spikes.” That slower rise-and-fall pattern is exactly what reduces insulin surges and adrenaline-driven symptoms.
It’s equally important to avoid refined carbohydrates on their own. Pairing carbs with protein or fat makes a bigger difference than perfection.
Eating smaller, more frequent meals can also reduce symptoms. Large meals trigger stronger insulin and adrenaline responses, while eating every three to four hours helps stabilize blood sugar, reduce stress-hormone surges, and prevent sudden post-meal dips. This approach aligns with clinical nutrition guidelines and is particularly effective for people prone to postprandial symptoms.
Hydration and alcohol management matter as well. Drinking water consistently throughout the day supports circulation and prevents dizziness and fatigue. Alcohol should be avoided on an empty stomach, and sugary mixers can worsen glucose swings and adrenaline-driven symptoms, so it’s best to skip them entirely.
Stress and sleep are often overlooked contributors. Adrenaline is a major driver of IPS symptoms, so calming the nervous system after meals, through slow breathing, short walks, or light physical activity, can help. Maintaining a consistent sleep schedule and incorporating mind-body practices further reduces sympathetic nervous system overactivity, making post-meal episodes less likely.
With these strategies, balanced meals, regular eating, proper hydration, and stress management, IPS can be effectively controlled. While it may not disappear overnight, most people see a significant reduction in post-meal shakiness, anxiety, and discomfort, allowing daily life to feel calmer and more predictable.
When Diet Changes Aren’t Enough: In rare, persistent cases, medication may be considered. Alpha-glucosidase inhibitors, such as acarbose, slow carbohydrate digestion and can blunt post-meal glucose spikes. Evidence is limited, and these medications should only be used under medical supervision. They are not considered first-line therapy.
When to See a Doctor
You should seek medical evaluation if symptoms of IPS are frequent, worsening, or interfering with your daily life. Episodes that involve confusion, fainting, or severe weakness require prompt attention, as these could indicate a more serious underlying issue.
Testing may be needed to rule out conditions such as reactive hypoglycemia, insulinoma, or thyroid and adrenal disorders. In some cases, a mixed-meal tolerance test is preferred over a standard oral glucose tolerance test, since the latter can exaggerate symptoms and produce misleading results.
Consulting a healthcare professional ensures that any serious causes are addressed and helps guide a safe, effective strategy for managing post-meal episodes.
Read More: Dealing with Hypoglycemia and Hyperglycemia When You Have Type-1 Diabetes
Key Takeaways
Idiopathic postprandial syndrome causes real and often alarming symptoms, even though blood sugar levels remain within the normal range. The root of these episodes isn’t a dangerous glucose crash but rather a combination of insulin dynamics, nervous system sensitivity, and how the body responds to certain meals.
Adrenaline-driven reactions make the symptoms feel dramatic, which is why many people initially mistake IPS for true hypoglycemia or even anxiety. The good news is that IPS is highly manageable. Consistently balanced meals, frequent eating, and pairing carbohydrates with protein and healthy fats help stabilize blood sugar and prevent sudden swings.
Coupled with proper hydration, adequate sleep, and strategies to reduce stress, these lifestyle adjustments can dramatically reduce the frequency and intensity of post-meal episodes. Being aware of personal triggers, like high-glycemic foods, caffeine, alcohol, or irregular eating patterns, also allows for better control and planning.
Persistent or severe symptoms should prompt a medical evaluation. This helps rule out other causes such as reactive hypoglycemia, insulinoma, or hormonal disorders, and provides reassurance that nothing more serious is being overlooked. Understanding IPS as a physiological response rather than a mental or diabetic issue is key.
It’s not “just anxiety,” and it’s not diabetes. Recognizing it as a misunderstood but real condition allows people to take informed, practical steps to prevent episodes, regain confidence after meals, and live without the constant fear of sudden crashes.
References
- Björntorp, P., & Rosmond, R. (1990). Adrenergic responses and postprandial symptoms. Endocrine Abstracts, 81, E532.
- Holt, P. R. (2002). Review of reactive and postprandial hypoglycemia physiology. Journal of Clinical Gastroenterology, 35(4), 260-269.
- Lawler, M. (n.d.). Idiopathic postprandial syndrome. Semantic Scholar.
- Miller, L. L., & Sockett, P. N. (1984). Postprandial adrenergic syndrome and symptomatology. American Journal of Medical Case Reports, 12(14142).
- Service, F. J. (1984). Postprandial hypoglycemia (reactive hypoglycemia). The American Journal of Medicine, 77(1), 37-45.
- Trexler, R. V. (2011). Postprandial hypoglycemia [PDF]. IntechOpen.
- Cleveland Clinic. (2024). How to treat reactive hypoglycemia.
- Cleveland Clinic. (2024). Hypoglycemia (low blood sugar).
- MDPI. (2025). Exploring insulin dynamics during a mixed meal test. Nutrients, 17(3), 479.
- PubMed. (1994). Suspected postprandial hypoglycemia is associated with beta-adrenergic hypersensitivity and emotional distress.
- Grokipedia. (n.d.). Idiopathic postprandial syndrome.
- Wikidoc. (n.d.). Idiopathic postprandial syndrome.
- Gateway Natural Medicine. (n.d.). Postprandial adrenergic syndrome: Post-meal anxiety.
- Diabetes UK Forums. (n.d.). Idiopathic post-prandial syndrome discussion.
In this Article