A lot of people think probiotics are just for gut health, but the truth is, the whole idea of finding “best probiotic for vaginal health” has really taken off lately, both in research and in women’s wellness circles. Vagina has its own little ecosystem – called vaginal microbiome, and it’s usually dominated by Lactobacillus species. When it’s healthy, that microbiome keeps pH low and helps stop bad bacteria from taking over.
But everyday things like antibiotics, stress, hormones, or even intercourse can mess with good bacteria. When Lactobacillus drops, bacterial vaginosis (BV) or yeast can show up.
That’s where vaginal probiotics and probiotics for women come in. Basically, they give your body more of “good” bacteria (mostly different Lactobacillus strains) to help rebuild vaginal flora balance, get pH back to normal, and crowd out stuff that shouldn’t be there.
In this article, we go beyond generic advice with real talk, the raw version.
How Probiotics Support Vaginal Health
To understand why the best probiotic for vaginal health matters, it helps to see how probiotics act in the vaginal environment.
1. Restoring microbiome balance
A healthy vagina is mostly made up of just a few Lactobacillus strains (like 70–90%). When bad bacteria like Gardnerella, Candida, or Prevotella take over, it can lead to BV or yeast issues. Probiotics help restore good bacteria and bring things back into balance.
2. Maintaining vaginal pH (~3.8–4.5)
Lactobacilli break down glycogen (or glucose) in the vaginal lining and turn it into lactic acid. This acidifies the environment, which makes it inhospitable to many pathogens. They may also generate hydrogen peroxide (H₂O₂) or bacteriocins that inhibit pathogens.
3. Competitive exclusion and biofilm disruption
Good strains can compete for adhesion sites, nutrients, and even displace pathogen biofilms. They can reduce vaginal odor, discharge, and irritation, as well as lower the risk of urinary tract infections (UTIs) by stabilizing the urogenital area.
4. Immune modulation
Besides fighting off bad bacteria, probiotics boost the immune defenses right where they matter—in the vaginal and cervical areas. They help keep the mucous layers healthy, support natural antimicrobial processes, and help calm inflammation.
Simply put, best probiotic for vaginal health is one that helps friendly lactobacilli take over again, keeps the pH optimum, and stops harmful bacteria from growing.
Read More: Top Vaginal Health Supplements You Can Buy Online (Probiotics, Prebiotics & More)
Best Probiotic Strains for Vaginal Health (Evidence-Based)
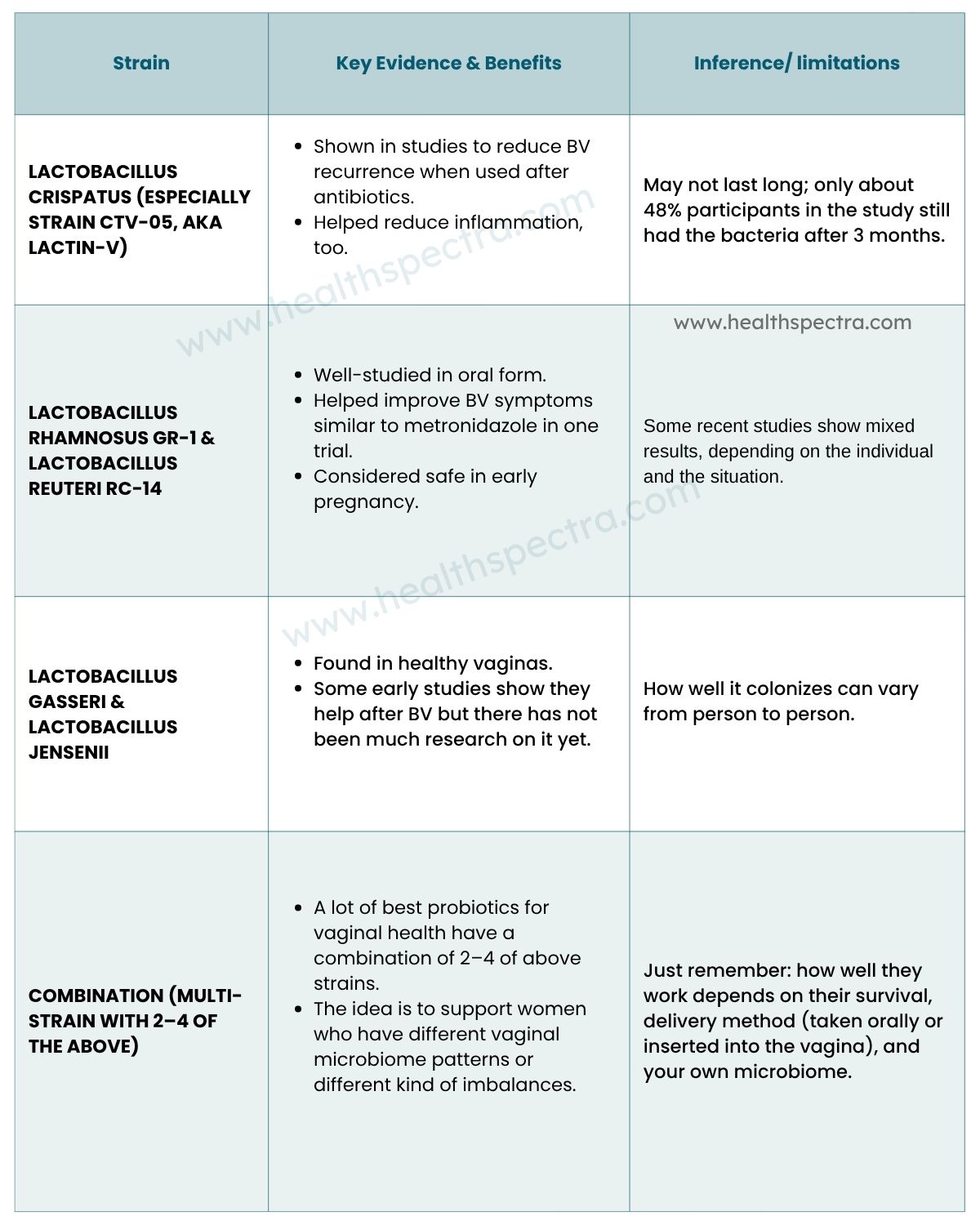 Not all probiotics are the same- strain matters a lot. Below are some good, promising (and researched) strains for vaginal microbiome support – especially probiotics for BV and lactobacillus for vaginal health. More importantly, vaginal microbiomes are diverse for different individuals. Some women’s vaginas are dominated by L. crispatus, others by L. iners, and others are a mix. Researchers now argue that the right bug in the right place matters, i.e., selecting strains that are more “vaginal native,” like crispatus, often yields better outcomes.
Not all probiotics are the same- strain matters a lot. Below are some good, promising (and researched) strains for vaginal microbiome support – especially probiotics for BV and lactobacillus for vaginal health. More importantly, vaginal microbiomes are diverse for different individuals. Some women’s vaginas are dominated by L. crispatus, others by L. iners, and others are a mix. Researchers now argue that the right bug in the right place matters, i.e., selecting strains that are more “vaginal native,” like crispatus, often yields better outcomes.
So, the best probiotic for vaginal health typically includes one or more of these proven Lactobacillus strains with good viability and clearance data behind them.
Read More: 6 Women’s Health Trends to Watch in 2025 (Backed by Data)
How to Choose the Best Vaginal Probiotic
Even with the right strains, many products on the market are underpowered or misleading. Here’s a checklist to help you pick the truly effective best probiotic for vaginal health:
1. Strain specificity/transparency
- Look for full strain names, e.g., Lactobacillus rhamnosus GR-1, Lactobacillus reuteri RC-14, crispatus CTV-05. Avoid labels that just say “Lactobacillus blend” without details.
- Strain-level identity is critical because different strains of the same species exhibit different behaviors.
2. CFU count (colony-forming units)
- Effective ranges in trials often span 1–10+ billion CFU per dose (often daily).
- Watch out for products with super low CFUs (like under 1 billion) unless there’s solid proof they actually stick around and work.
3. Delivery form & route
- Oral capsules: convenient, systemic delivery, supports gut–vagina axis (some strains can translocate).
- Vaginal suppositories, tablets, or gels: direct delivery to the vaginal area, and this may boost colonization for some strains.
- Powders or sachets: less common and may need mixing.
Choose one based on your goal (long-term maintenance, post-antibiotic, symptomatic relief).
4. Viability/survival & formulation quality
- Strains should be stable through shelf life, ideally with data on survival under relevant storage conditions.
- Go for brands with third-party testing or, at least, an independent lab check.
- Packaging should protect against moisture and oxygen (e.g., blister packs, sealed desiccants).
- BPA-free or food-grade capsule shells.
4. Clinical backing & scientific studies
- Prefer brands or formulations that either replicate or cite human clinical trials, especially in BV or yeast infection settings.
- Avoid ones that rely only on in vitro results or animal models.
5. Compatibility & safety
- Should be safe (non-pathogenic, minimal side effects).
- For immunocompromised persons, those with severe pelvic infections, or during pregnancy, always consult a clinician first.
6. Cost vs dose & shelf life
- An expensive product with half of the CFU or no strain data is inferior to a well-priced, transparent one.
- Check “use-by” dates and required storage (room temperature vs refrigeration).
When multiple of these boxes are checked, such as strain transparency, high CFU, good delivery, and clinical backing, you’re closer to selecting the best probiotic for vaginal health for your situation.
Read More: 7 Vaginal Health Myths Doctors Wish Women Would Stop Believing
Best Probiotic Products for Vaginal Health (2025 Update)
Here are some well-known and research-aligned feminine probiotic supplements. Always check labels carefully.
- Love Wellness Good Girl Probiotic — Oral capsule combining GR-1 and RC-14 strains (a common combination in women’s probiotic space).
- O Positive Uro Vaginal Probiotic — Multi-strain formula targeting BV and UTI risk.
- Jarrow Formulas Fem-Dophilus — A classic formula containing GR-1 & RC-14, with clinical backing.
- BAKAKOUL Women’s Vaginal Probiotics — More budget-friendly, multi-strain formulation.
- Culturelle Women’s Healthy Balance — Contains rhamnosus + L. gasseri, relatively accessible.
(Note: Always cross-check strain details in your region; product formulations or strain disclosures can change.)
Here is a recap of what to look for when choosing the best probiotic for vaginal health….See whether they:
- Disclose strain names
- Deliver adequate CFU
- Use stable packaging
- Cite clinical studies
- Provide guidance on usage
These are good starting points, but the true and best probiotic for vaginal health for you depends on your microbiome baseline, whether you have recurrent BV or yeast, and how your body accepts colonization.
Read More: Vaginal Dryness in Your 30s and 40s: Causes and Remedies
Best Ways to Take Probiotics for Vaginal Health
Getting a good product is just half the journey – how you use it matters a lot.
Oral Probiotics
- Dose: Usually 1 capsule a day, or 2 if you’re just starting or dealing with symptoms.
- Duration: Some notice changes in 2–4 weeks, but full results might take 8–12 weeks.
- Timing: Best taken before meals (empty stomach works better for some strains).
- Consistency: missing days can mess with progress.
Vaginal Probiotics (Suppositories / Tablets / Gels)
- Dose: Typically, one suppository or tablet is inserted daily for a few nights to reset your vaginal microbiome balance.
- Duration: Use daily for the first 5–7 days (or as directed), switch to once or twice a week for maintenance (as per product instructions).
- Timing: Insert before bedtime so it stays in place better overnight.
- Consistency: Stick with the schedule; irregular use can reduce how well vaginal probiotics colonize and maintain their results.
Remember, after using, avoid sex, tampons, or douching for a few hours, so it can absorb properly. Really good to use after antibiotics or when symptoms flare up.
Support with Diet / Prebiotics
- Complex carb-based prebiotics, like inulin or resistant starch, can help good bacteria thrive, acting as food for your microbiome. Add them to your diet to obtain optimum benefits from your probiotics.
- Giorgia Soreca, a gynecologist, emphasizes eating a balanced diet (lots of fruits and vegetables), managing stress, and skipping harsh soaps or scented sprays as these can throw off your flora.
Track and Check-in
- Keep an eye on symptoms like discharge, odor, or itching.
- If you’re using probiotics after BV or yeast, then follow-ups with your gynecologist or microbiome tests (if you can do those) are a good idea.
Read More: Ultimate Guide to Feminine Hygiene: Top 7 Intimate Washes for Sensitive Skin
Possible Side Effects and Precautions
Most vaginal probiotics are safe, but few things to watch out for:
- Some people may experience mild bloating or gas initially, but it usually subsides in a few days.
- Rarely, allergies can happen (like from fillers or dairy in the capsule).
- If you feel burning or irritation with vaginal use, stop right away.
- Probiotics alone are not a cure for any disease, and medical therapies are always the first-line treatment for cases of BV, yeast, or STIs.
- If you’re pregnant, have immune issues, or pelvic disease, talk to your doctor first.
- One study said L. crispatus might lower sperm movement in lab tests, so maybe avoid it if you’re trying to get pregnant- just in case.
Broadly speaking, the best probiotics for vaginal health can make a real difference. Just be sure to use them wisely and as part of a bigger self-care routine.
Read More: When to See a Gynecologist for the First Time (A Parent’s Guide)
Key Takeaway
- The best probiotic for vaginal health is never a one-size-fits-all pill. It should include proven Lactobacillus strains, especially crispatus, L. rhamnosus GR-1, L. reuteri RC-14; deliver high viable counts and come in a delivery form that suits your goals.
- Multi-strain formulas with clear labels and actual clinical backing are way more trustworthy.
- Whether you take it orally or vaginal, stick with it as it helps keep vaginal pH balance, supports your vaginal microbiome health, and lowers the chances of BV or yeast coming back.
- Just remember, probiotics are extra support — not a full-on treatment. Always good to check with your doctor.
FAQs About Vaginal Probiotics
Q1. Do probiotics actually help with bacterial vaginosis?
Yes! Certain strains, such as GR-1 + RC-14 or L. crispatus CTV-05, can reduce the risk of BV recurrence and help maintain a balanced vaginal microbiome. But it depends on the strain, the dose, and your body.
Q2. Can you take vaginal probiotics every day?
Yes! Many maintenance protocols use daily dosing initially, then shift to alternate days or a few times per week once colonization is achieved (depending on product instructions).
Q3. What’s better – oral or vaginal probiotic?
It depends on your goal:
- Oral offers systemic support and may be easier to consume daily.
- Vaginal delivery provides direct access —possibly better local colonization.
- Some regimens combine both for a synergistic effect.
Q4. Are probiotics safe during pregnancy?
In low-risk pregnancies, some strains (like GR-1 + RC-14) seem fine, but definitely talk to your doctor first, especially if there’s any risk.
Q5. How long does it take for vaginal probiotics to work?
Some feel better in 2-4 weeks, but full balance can take 8-12 weeks. If nothing’s changing or it gets worse, then check with your doctor.
References
- France MT, Mendes-Soares H, Forney LJ. Genomic Comparisons of Lactobacillus crispatus and Lactobacillus iners Reveal Potential Ecological Drivers of Community Composition in the Vagina. Applied and Environmental Microbiology. 2016;82(24):7063-7073.
- Mei Z, Li D. The role of probiotics in vaginal health. Frontiers in Cellular and Infection Microbiology. 2022;12.
- Wu S, Hugerth LW, Schuppe-Koistinen I, Du J. The right bug in the right place: opportunities for bacterial vaginosis treatment. npj Biofilms and Microbiomes. 2022;8(1).
- Cohen CR, Wierzbicki MR, French AL, et al. Randomized Trial of Lactin-V to Prevent Recurrence of Bacterial Vaginosis. New England Journal of Medicine. 2020;382(20):1906-1915.
- Armstrong E, Hemmerling A, Miller S, et al. Vaginal Lactobacillus crispatus persistence following application of a live biotherapeutic product: colonization phenotypes and genital immune impact. Microbiome. 2024;12(1).
- Anukam KC, Osazuwa E, Osemene GI, Ehigiagbe F, Bruce AW, Reid G. Clinical study comparing probiotic Lactobacillus GR-1 and RC-14 with metronidazole vaginal gel to treat symptomatic bacterial vaginosis. Microbes and Infection. 2006;8(12-13):2772-2776.
- Yang S, Reid G, Challis JRG, et al. Effect of Oral Probiotic Lactobacillus rhamnosus GR-1 and Lactobacillus reuteri RC-14 on the Vaginal Microbiota, Cytokines and Chemokines in Pregnant Women. Nutrients. 2020;12(2):368.
- Zhang Y, Lyu J, Ge L, et al. Probiotic Lacticaseibacillus rhamnosus GR-1 and Limosilactobacillus reuteri RC-14 as an Adjunctive Treatment for Bacterial Vaginosis Do Not Increase the Cure Rate in a Chinese Cohort: A Prospective, Parallel‐Group, Randomized, Controlled Study. Frontiers in Cellular and Infection Microbiology. 2021;11.
- Argentini C, Fontana F, Alessandri G, et al. Evaluation of Modulatory Activities of Lactobacillus crispatus Strains in the Context of the Vaginal Microbiota. Visca P, ed. Microbiology Spectrum. 2022;10(2).
- Qi F, Fan S, Fang C, et al. Orally administrated Lactobacillus gasseri TM13 and Lactobacillus crispatus LG55 can restore the vaginal health of patients recovering from bacterial vaginosis. Frontiers in Immunology. 2023;14:1125239.
- Li P, Wei K, He X, et al. Vaginal Probiotic Lactobacillus crispatus Seems to Inhibit Sperm Activity and Subsequently Reduces Pregnancies in Rat. Frontiers in cell and developmental biology. 2021;9.
In this Article