You’re sitting in the doctor’s office. The cuff tightens around your arm. Your pulse quickens. The numbers on the monitor flash higher than you expected, and suddenly your mind races, “Is something wrong?” Then you get home, check your blood pressure again, and everything looks normal. No spikes, no warning signs. Confusing, right?
This scenario is more common than you might think, and it creates a real dilemma. Are those high readings a genuine sign of hypertension, or is anxiety, caused by the very act of being in a medical setting, playing tricks on your body?
Enter white-coat syndrome, also called white-coat hypertension. It’s a well-documented phenomenon where blood pressure temporarily rises in clinical environments but remains normal in daily life. For many, it’s harmless, but for others, it can mask real cardiovascular risk or lead to unnecessary medication if misdiagnosed.
Understanding which category you fall into is crucial. The good news? There are clear, practical ways to check your blood pressure at home, interpret the readings accurately, and work with your healthcare provider to make informed decisions. No panic, no guesswork, just reliable insight into what your numbers really mean.
Understanding White Coat Syndrome: When Anxiety Mimics Hypertension

White coat syndrome refers to a temporary rise in blood pressure caused by stress or anxiety during medical visits. The name comes from the white coats traditionally worn by doctors, but the trigger isn’t the clothing. It’s the situation.
At Mayo Clinic, this is called white coat hypertension. The emotional stress or anxiety many people feel during a checkup can temporarily raise blood pressure. A single high reading in the clinic doesn’t always mean you have chronic hypertension, but it can signal future risk if it happens consistently.
Doctors often recommend home or ambulatory monitoring so you get a fuller picture of your typical blood pressure outside the clinic.
This isn’t imagined. It’s physiology.
When you feel anxious, your body activates the sympathetic nervous system. Adrenaline increases heart rate. Blood vessels constrict. Cortisol rises. All of that pushes systolic and diastolic readings upward, sometimes by 20 to 30 mmHg.
The problem is that repeated high readings in clinics can look exactly like chronic hypertension on paper. And that can lead to unnecessary medication or, just as concerning, ignoring the role anxiety plays in your health.
Why It Matters to Tell the Difference
Understanding the difference between true hypertension and white coat hypertension matters because it shapes both your health outlook and your treatment. Not all high readings are the same; some reflect chronic risk, while others are temporary spikes caused by stress or anxiety in a medical setting. Knowing which is which helps you make informed decisions and avoid unnecessary treatment or missed warning signs.
1. Long-Term Health Risks Are Not the Same
True hypertension is a chronic condition. Over time, persistently elevated blood pressure damages arteries, strains the heart, and increases the risk of stroke, heart attack, kidney disease, and vision loss.
White coat hypertension is different. Research published in Hypertension and indexed in PubMed shows that people with isolated white coat syndrome generally have a lower cardiovascular risk than those with sustained hypertension.
That said, it’s not completely benign. A large meta-analysis found that people with white coat hypertension have a higher likelihood of developing true hypertension later compared to people whose readings are always normal.
What this really means is that white coat syndrome is a warning signal, not a diagnosis to ignore or panic over.
2. Treatment Decisions Depend on Accuracy
Blood pressure medication lowers numbers, whether the cause is anxiety or artery stiffness. But if your blood pressure is only high during stress, medication may not be necessary and could cause side effects like dizziness or fatigue.
The American Heart Association estimates that up to 20 percent of people diagnosed with hypertension based on clinic readings alone may actually have white coat hypertension. That’s a big margin for error.
Accurate diagnosis helps clinicians focus on the right solution. Sometimes that’s lifestyle support. Sometimes it’s anxiety management. Sometimes it truly is medication. But you can’t choose wisely without good data.
How to Check for White Coat Hypertension at Home

Checking your blood pressure at home is the most reliable way to understand whether high readings at the doctor’s office reflect true hypertension or a temporary stress response. With the right technique, consistent tracking, and careful discussion with your healthcare provider, you can separate real risk from white coat anxiety and make informed decisions about your health.
Step 1: Prepare and Measure Correctly
Most inaccurate blood pressure readings aren’t caused by faulty machines; they come from rushing or improper technique. To get reliable measurements at home:
- Sit quietly for five minutes before measuring. No phone, no talking, just rest.
- Feet flat on the floor, not crossed, and back supported by a chair.
- Arm at heart level on a table, with the cuff snugly fitted on bare skin.
- Avoid caffeine, nicotine, or exercise for at least 30 minutes beforehand.
Even small posture errors can inflate readings. The National Institutes of Health notes that improper posture alone can raise systolic readings by 10 points or more.
Take two measurements one minute apart and average them. This is more meaningful than a single reading spike.
Use a digital upper-arm monitor validated by the American Medical Association, which is considered accurate when used correctly. Wrist monitors are generally less reliable.
Step 2: Track Your Readings Over Several Days
A single reading can be misleading. Patterns reveal the real story.
- Measure your blood pressure at the same time each day, ideally once in the morning before food or medication and once in the evening.
- Track readings for at least five to seven days. Record them manually or use a home blood pressure app; consistency matters more than convenience.
Here’s what patterns may indicate:
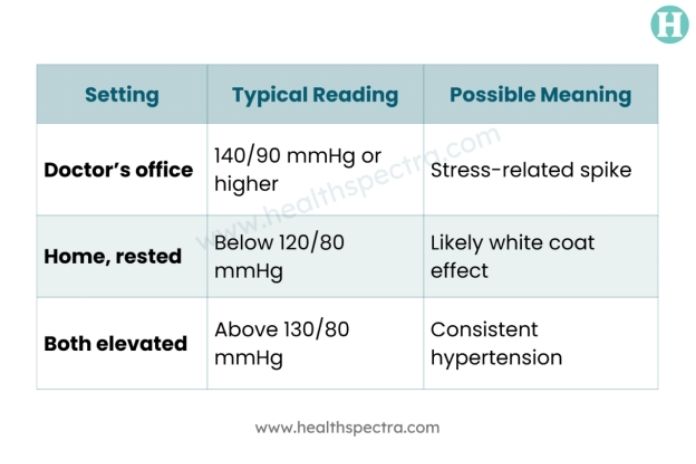 If your home readings remain normal while clinic readings are repeatedly high, white coat hypertension is likely.
If your home readings remain normal while clinic readings are repeatedly high, white coat hypertension is likely.
Step 3: Compare and Discuss With Your Healthcare Provider
Home monitoring doesn’t replace medical care, but it informs it. Bring your blood pressure log to appointments and share patterns, not just single numbers. Clinicians increasingly rely on home data to guide treatment decisions.
If uncertainty persists, ambulatory blood pressure monitoring (ABPM) may be recommended. This involves wearing a device for 24 hours that measures your blood pressure during daily activities and sleep.
According to the World Health Organization, ABPM is considered the gold standard for distinguishing white coat hypertension from sustained high blood pressure. It gives a complete picture of your blood pressure throughout the day, eliminating anxiety-driven spikes from office visits.
How Anxiety and Stress Temporarily Raise Blood Pressure
Understanding the mechanism helps reduce fear. When anxiety hits, the hypothalamus signals the adrenal glands to release adrenaline and cortisol. Blood vessels tighten. Heart rate increases. Blood pressure rises. This is your body switching into fight-or-flight mode.
This response is designed to keep you safe from a perceived threat. It is temporary. It is not the same process that causes chronic hypertension, which involves long-term changes in blood vessel structure, kidney regulation, and hormone signaling.
Dr. Paul Whelton, former chair of the hypertension writing committee for the American College of Cardiology, explains why single readings are often misleading: “Blood pressure is one of those factors that has a lot of variability. It’s all over the place.”
What this means is simple. Stress, fear, or even mild anxiety during a medical visit can push blood pressure up for a short time without reflecting what your body does the rest of the day.
Common triggers include fear of test results, past medical trauma, performance anxiety, or even just hearing the cuff inflate. Once the stress fades, the blood pressure elevation fades with it. The body settles. The numbers come back down. That temporary spike is a stress response, not damaged arteries.
Read More: How Stress Affects Blood Pressure and 7 Ways to Lower It
Practical Tips to Stay Calm During Blood Pressure Checks
You don’t need gimmicks or complicated tricks; simple, evidence-based relaxation strategies are enough to help your body settle before a reading. The goal isn’t to “cheat” the number; it’s to let your body reach its true baseline so you and your healthcare provider get accurate information.
Before measuring your blood pressure:
- Breathe slowly and deliberately: Inhale through your nose for four seconds, then exhale through your mouth for six. Focusing on extending the exhale helps calm the nervous system.
- Sit quietly without talking: Conversation, even casual, can raise blood pressure temporarily.
- Relax your posture: Feet flat on the floor, back supported, and arm at heart level.
- Use calming aids if helpful: Soft instrumental music or a quiet environment can reduce anxiety.
- Keep perspective: One elevated reading does not define your overall health.
A meta-analysis of breathing exercises also found that paced breathing techniques meaningfully lowered systolic and diastolic blood pressure across multiple studies, supporting the idea that even brief slow-breathing sessions can calm the body and yield more reliable readings.
Lifestyle Strategies to Prevent and Manage White Coat Hypertension

While white coat syndrome is largely anxiety-driven, how you live day-to-day can influence both your baseline blood pressure and your stress response. Focusing on lifestyle strategies doesn’t just help lower readings at home; it can reduce anxiety spikes in the clinic, too.
1. Stress Management Practices
Stress is the central driver behind white coat spikes. Regular techniques to calm the nervous system, like mindfulness meditation, yoga, tai chi, or progressive muscle relaxation, train your body to stay regulated.
Even five to ten minutes per day of deep, paced breathing can lower resting heart rate and blood pressure. Over time, these practices make your body less reactive to situational stress, meaning fewer exaggerated spikes in the doctor’s office.
Read More: 6 Stress-Relief Techniques to Help Manage Hypertension
2. Exercise and Cardiovascular Fitness
Regular physical activity improves vascular health, strengthens the heart, and lowers baseline blood pressure. Aerobic activities like walking, swimming, or cycling are particularly effective. Resistance training also helps, especially when paired with aerobic exercise.
Importantly, exercise can reduce anxiety and enhance mood, giving you a twofold benefit: lower resting blood pressure and reduced white coat responses.
3. Nutrition and Blood Pressure
Diet influences both blood pressure and inflammation, which indirectly affects cardiovascular risk. Focus on the DASH (Dietary Approaches to Stop Hypertension) diet or a Mediterranean-style diet: plenty of fruits, vegetables, whole grains, lean protein, and healthy fats.
Reducing sodium intake, added sugars, and ultra-processed foods supports healthy blood pressure levels and overall heart health. Omega-3 fatty acids, found in fatty fish and walnuts, can also improve vascular function and support a calmer nervous system.
4. Sleep and Recovery
Poor sleep raises stress hormones and can elevate blood pressure, both at home and in clinical settings. “When your body doesn’t have enough time to do the things it needs to do during sleep, it won’t do them in an optimal way,” says Dr. Michael Grandner, director of the Sleep and Health Research Program at the University of Arizona.
Maintaining a consistent sleep schedule, minimizing screens before bed, and creating a relaxing pre-sleep routine can reduce sympathetic nervous system activation and help your blood pressure stabilize.
Read More: How Sleep Affects Hypertension: Tips for Better Rest
5. Behavioral Preparation for Clinic Visits
Simple behavioral steps before your appointment can help mitigate white coat spikes. Arrive a few minutes early to settle in. Practice a brief relaxation routine in the waiting room.
Avoid coffee, nicotine, or intense activity right before measurement. Even small behavioral adjustments can reduce the magnitude of blood pressure elevation and give clinicians a more accurate reading.
6. Mental Health Support
For people with persistent anxiety about medical visits, professional support from a therapist or counselor may be valuable. Cognitive-behavioral therapy (CBT) and exposure-based techniques can help you reframe fears, reduce anticipatory anxiety, and gain confidence in healthcare settings. Addressing anxiety directly often lowers white coat responses over time.
The key takeaway is that while white coat syndrome is often benign, combining accurate home monitoring with lifestyle strategies creates a strong, proactive approach.
You’re not just controlling numbers; you’re improving cardiovascular resilience, managing stress, and supporting overall health. These strategies make future clinic visits less stressful and give both you and your healthcare provider a clearer, more reliable picture of your blood pressure.
Read More: The Role of Meditation and Mindfulness in Hypertension Control
When Elevated Readings Are Not Just Stress

White coat syndrome should never be used to dismiss consistently high readings at home. If your blood pressure repeatedly measures 130/80 mmHg or higher while resting, this meets the CDC’s criteria for hypertension.
Seek medical attention promptly if high readings are accompanied by symptoms such as persistent headaches, dizziness, chest pain, shortness of breath, or vision changes.
Importantly, never stop or adjust prescribed medication on your own. Anxiety and hypertension can coexist, and both require proper management. Accurate measurement, monitoring, and professional guidance ensure you’re treating the real problem, whether it’s stress-driven spikes, true hypertension, or both.
Read More: 6 Lifestyle Changes to Reduce Your Risk of Hypertension
Key Takeaway: Don’t Let Fear Skew the Facts
White coat hypertension is common, real, and, in most cases, not dangerous. A single high reading at the doctor’s office does not automatically mean you have chronic high blood pressure. Anxiety and stress can temporarily raise numbers, creating a misleading snapshot of your health.
The most reliable way to understand your blood pressure is through accurate home monitoring, manual measurement, and tracking patterns over time. This approach shows the difference between stress-driven spikes and true hypertension, giving you a clearer picture of your cardiovascular risk.
Consistent, high-quality data protects you in two ways: it prevents unnecessary medication when your blood pressure is normal outside the clinic, and it ensures genuine hypertension is detected and managed early. Both matter for your long-term health.
Remember, a few elevated readings do not define you. What matters is accuracy, consistency, and calm; these are the tools that put you back in control of your health and help you make informed decisions with your doctor.
By understanding the difference between temporary stress responses and sustained hypertension, you can reduce anxiety, avoid unnecessary interventions, and focus on strategies that truly protect your heart, arteries, and overall well-being.
FAQs: People Also Ask
What are common white coat syndrome symptoms?
White coat syndrome usually doesn’t cause physical symptoms beyond temporary anxiety. You might notice a racing heart, sweaty palms, or a feeling of tension during medical visits. Outside the clinic, your blood pressure and body sensations generally return to normal. The main “symptom” is the spike in readings that occurs when stressed.
Can anxiety cause high blood pressure long-term?
Anxiety can trigger short-term blood pressure spikes during stressful moments, but it doesn’t directly cause chronic hypertension. Persistent stress may contribute indirectly by affecting sleep, diet, and daily habits. Over time, these lifestyle factors can influence heart health. Managing stress supports overall cardiovascular well-being.
How accurate are home blood pressure monitors?
Validated upper-arm monitors are generally reliable when used according to instructions. Proper posture, cuff placement, and timing matter for accuracy. Wrist and finger devices are less precise and can give misleading readings. Consistency and correct technique are key to trustworthy home measurements.
Should white coat hypertension be treated?
White coat hypertension usually does not require medication by itself. Monitoring patterns at home, supporting lifestyle changes, and managing anxiety are often enough. Treatment decisions depend on overall cardiovascular risk and other health factors. Regular follow-ups help ensure any real hypertension is caught early.
How often should I check my blood pressure at home?
During evaluation, it’s recommended to measure once or twice daily for five to seven days. Take readings at the same times each day for consistency. After diagnosis, follow your clinician’s guidance for ongoing monitoring. Keeping a log of patterns is more important than individual numbers.
References
- American Heart Association. (2018, September 18). The task force says 24-hour monitoring best at confirming high blood pressure diagnosis.
- American Heart Association. (2023, March 16). What happens when we sleep and why we need just the right amount each night.
- American Heart Association. (2024, June 25). The rules for measuring blood pressure and why they exist.
- Eureka Health. (n.d.). White coat syndrome: Blood pressure 160/95.
- International Society of Hypertension Writing Group. (2018–2024). Understanding high blood pressure.
- Mayo Clinic. (n.d.). High blood pressure: White coat hypertension.
- Medical Forum Monthly. (n.d.). White coat hypertension: Diagnosis and management.
- National Center for Biotechnology Information. (2017). White coat hypertension is a risk factor for cardiovascular events and total mortality. Journal of Hypertension, 35(4).
- National Center for Biotechnology Information. (2019). Ambulatory blood pressure monitoring: Current status and clinical relevance.
- National Center for Biotechnology Information. (2016). White coat hypertension: Cardiovascular outcomes.
- National Center for Biotechnology Information. (2020). Slow breathing for hypertension: A meta-analysis.
- Paige Pradko. (n.d.). Understanding and overcoming white coat syndrome: A deep dive into anticipatory anxiety.
- ResearchGate. (2023). White coat hypertension: Cardiovascular outcomes.
- Springer. (2021). White coat hypertension and anticipatory stress: Implications for blood pressure management.
- Woodruff Medical Center. (n.d.). How medical assistants can help ease patient anxiety.
- Wiley Online Library. (2020). Psychological and physiological factors in white coat hypertension.
- PMC. (2020). White coat hypertension: Pathophysiology and clinical implications.
- ESC Cardio Online. (n.d.). White-coat hypertension: Not so innocent.
In this Article
















