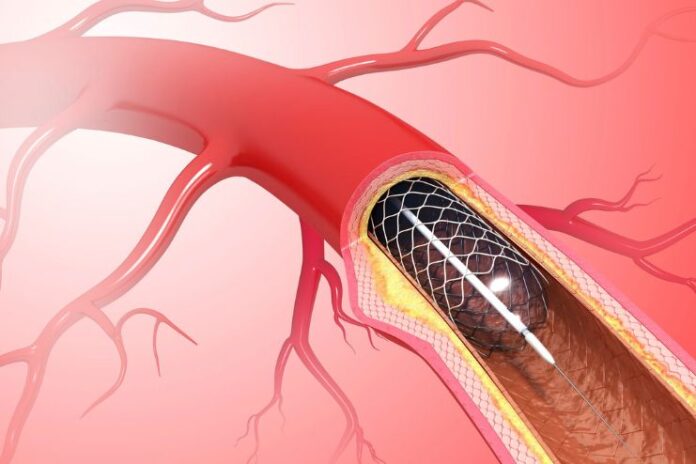
Heart stents represent an excellent medical innovation that restores normal blood flow to the heart after a blockage occurs. These slender mesh tubes, typically made of metal, are inserted into blocked or narrowed coronary arteries to keep them open, preventing heart attacks and ensuring overall cardiac health.
While short-term results are revolutionary, most patients and their families want to understand what happens ten, fifteen, or twenty years after the procedure. Are stents permanent? Can complications arise down the road? How should heart health be monitored long-term?
This comprehensive article addresses what the future holds for heart stents, examining their lifespan and potential risks such as stent thrombosis and restenosis.
More than 20.5 million Americans suffer from coronary artery disease, the most common cardiac illness. It claimed over 680,000 lives in 2023, with one in five cardiovascular disease deaths occurring in people under 65.
Read More: Daily Supplements for Heart Health: Vitamins and Minerals to Manage Cholesterol
What Is a Heart Stent and Why Is It Used?
A coronary artery may narrow due to plaque accumulation, resulting in symptoms like chest discomfort and decreased blood flow to the heart. If a clot forms in this narrow opening and blocks blood flow completely, a heart attack occurs.
A cardiac stent is a tiny mesh tube made of metal or polymer that acts as a scaffold inside a coronary artery, preventing it from narrowing or becoming blocked. The stent may or may not have a medication coating.
During coronary stent implantation, doctors insert a balloon and stent into the narrowed coronary artery to widen it and restore blood flow to the heart muscle. This process reduces heart damage and prevents heart attacks, allowing patients to return to their regular activities without chest pain.
Atherosclerosis is a disorder that obstructs blood flow and leads to serious outcomes, including coronary heart disease. While medications can help restore normal blood supply to the heart, coronary angioplasty may be necessary when medication alone proves insufficient.
Important Note: Stenting is not considered major surgery because it’s a minimally invasive procedure that doesn’t require large, open incisions. However, you may need specific tests or medications before receiving a stent to prepare for the procedure.
After stent placement, you’ll likely need to take certain medications, such as aspirin and other antiplatelet drugs that prevent blood clot formation. Your doctor may recommend continuing this medication for a year or more following arterial stent placement to avoid complications.
Types of Coronary Stents
- Bare Metal Stents (BMS): Simple metal mesh tubes without medication coating.
- Drug-Eluting Stents (DES): Coated with medication that gradually releases into the artery, preventing re-narrowing.
- Biodegradable Stents: Temporary stents that dissolve within a few months to two years.
What Happens to a Stent in Your Body Over Time?

Coronary stents, first introduced in the mid-1980s, have undergone significant advancements since their initial use. These improvements have reduced two major stent-related complications: restenosis (gradual narrowing of the space inside the stent) and stent thrombosis (clot formation inside the stent).
Permanence and Durability
Coronary stents are typically made of metal and remain permanently in the artery, except for biodegradable versions that dissolve within two years. A stent’s effective lifespan—the time it remains functional—usually ranges from ten to fifteen years for keeping coronary arteries stable.
However, if patients and physicians fail to properly control the factors that cause coronary artery hardening, this timeframe can be shortened to as little as a few months.
Risk Factors for Stent Problems
Several factors can lead to stent restenosis:
- Smoking (the primary cause)
- High-fat diet
- Medication non-compliance
- Uncontrolled diabetes
- High blood pressure or cholesterol
- Insufficient stent coverage of lesions
- Sedentary lifestyle
Critical Point: Patients must take dual antiplatelet therapy for the prescribed period following stent insertion. Without proper antiplatelet medication, platelets and red blood cells will adhere to the stent and form blood clots—a dangerous complication with high mortality rates since the stent is a foreign object in the body.
Read More: Monitoring Heart Health at Home: 7 Essential Devices You Need
Can a Stent Move or Break After Years?
While rare, stents can malfunction, necessitating surgery to replace or repair an existing stent that can no longer maintain an open blood vessel. Blocked, kinked, or broken stents may worsen symptoms or cause the return of problems they were meant to treat, such as discomfort, swelling, or skin changes.
Stent repair or replacement is usually required if the current stent has moved out of position or become kinked, obstructed, or broken. Surgeons perform these complex, minimally invasive procedures from inside the vessel through small incisions in the neck or groin, using X-rays and ultrasound to locate and fix problem areas.
shows that invasive treatments like stents or bypass surgery are more successful in reducing symptoms and improving quality of life for individuals with coronary artery disease who experience angina (chest pain caused by reduced blood supply to the heart).
As Dr. David Maron, co-chair of the ISCHEMIA trial and clinical professor at Stanford School of Medicine, notes: “These results are very reassuring for patients with severe but stable heart disease who do not want to undergo invasive procedures.”
What Side Effects Might a Stent Cause?

While stents are considered very safe, complications can sometimes occur during or after the procedure. People with chronic conditions such as diabetes, kidney disease, or heart failure, or those who have had previous procedures to clear blocked arteries, face higher complication risks.
Possible Complications Include:
Reactions to Contrast Dye: The dye used to visualize blood vessels on X-rays can trigger allergic reactions. Rarely, contrast dye may cause kidney damage.
Catheter-Related Issues: Bleeding or discomfort may occur during catheter insertion, and the catheter may damage surrounding blood vessels.
Blood Clotting: One of the most serious risks is blood clot formation, which can increase the likelihood of a heart attack or stroke. According to the National Heart, Lung, and Blood Institute, blood clots at the stent site occur in approximately 1 to 2 percent of patients.
Restenosis: Chest pain may indicate restenosis—when the artery where the stent was placed narrows again due to abnormal tissue growth. Treatment involves repeat angioplasty and typically uses a different stent, usually a drug-eluting stent.
Read More: Dietary Guidelines for a Healthy Heart: Foods That Support Cardiovascular Health
Signs That May Indicate a Problem With Your Stent
Stent failure can present with various symptoms, depending on the underlying cause and stent location.
Common Signs of Stent Failure:
Primary Symptoms:
- Chest discomfort and/or pain, typically similar to heart attack sensations
- Chest tightness, described as a squeezing or pressure-like sensation
- Pain during physical exertion or at rest
Additional Symptoms:
- Shortness of breath
- Fatigue (unexplained weakness or exhaustion)
- Palpitations or irregular heartbeat
- Swelling in ankles, feet, or legs
- Lightheadedness or dizziness
- Sweating and nausea
These symptoms are significant and should not be ignored or dismissed. Regular medical examinations are highly recommended to monitor for potential stent complications.
How to Monitor and Maintain Heart Health After a Stent
Most people require a few weeks to resume regular activities following angioplasty or stenting. Before hospital discharge, you’ll receive comprehensive instructions regarding exercise, medication, follow-up appointments, wound care, and returning to normal activities.
You’ll be strongly encouraged to enroll in a specialized cardiac rehabilitation program designed to support your healing process and help you return to regular activities safely.
Dietary Recommendations
Following angioplasty or stenting, focus on maintaining a healthy diet to facilitate healing, reduce complication risks, and ensure full recovery. A nutritious diet also lowers the risk of recurring plaque buildup in arteries.
Heart-Healthy Diet Components:
- Fish: Two servings weekly of oily fish like salmon, mackerel, or sardines provide heart-healthy omega-3 fatty acids.
- Whole Grains: Choose wholemeal bread, brown rice, quinoa, barley, oats, and other whole grain options.
- Low-Fat Dairy: Opt for reduced-fat dairy products.
- Healthy Fats: Include nuts, seeds, avocados, and oily fish.
- Hydration: Drink plenty of water while avoiding sugary soft drinks and limiting alcohol intake.
- Portions: Aim for two servings of fruit, five servings of vegetables, and four or more servings of whole grains daily, adjusted for your energy needs.
Long-Term Monitoring
Regular follow-up appointments with your cardiologist are essential. These may include:
- Annual stress tests
- ECGs (electrocardiograms)
- Imaging studies based on your risk profile
- Blood work to monitor cholesterol and other markers
Lifestyle Modifications
- Exercise: Engage in regular, doctor-approved physical activity
- Weight Management: Maintain a healthy weight
- Blood Pressure Control: Monitor and manage hypertension
- Diabetes Management: Keep blood sugar levels controlled
- Smoking Cessation: Quit smoking completely
- Stress Management: Develop healthy coping strategies
Medication Compliance
Strict adherence to prescribed medications is crucial, especially antiplatelet therapy. Never stop or modify medications without consulting your physician.
Read More: 10 Essential Tips for Men’s Heart Health: Understanding Risk Factors
Can Heart Stents Last a Lifetime?
Longevity isn’t guaranteed. While stents protect your heart, they don’t necessarily improve long-term survival rates for heart patients. However, they do significantly reduce the need for follow-up procedures to reopen the treated artery, both early and long-term.
Research demonstrates that inserting stents into newly reopened coronary arteries reduces the likelihood of requiring repeat angioplasty treatments. However, studies also show that stents don’t necessarily affect long-term mortality rates.
For physicians choosing between less invasive coronary stent implantation and coronary artery bypass grafting, these findings have significant clinical and cost implications.
Key Point: Physicians hope that following your cardiologist’s recommendations and managing other risk factors will help stents enable you to live longer. However, diet and exercise remain the most crucial factors.
The type and quantity of food you consume directly influence heart attack risk factors, including obesity, diabetes, and high blood pressure.
Read More: Why Heart Disease Remains the Leading Cause of Death in the U.S.
Long-Term Risks of Heart Stents (10+ Years Later)
1. Restenosis (Re-narrowing of Artery)
Scar tissue or plaque buildup may occur inside the stent. Risk is higher with older bare-metal stents or when lifestyle changes aren’t implemented.
2. Stent Thrombosis
Rare but life-threatening—blood clots form inside the stent. This can occur years later, especially if antiplatelet therapy is discontinued prematurely.
3. New Blockages in Other Arteries
A stent only treats one specific area and isn’t a cure for overall heart disease. Disease progression can still occur elsewhere in the cardiovascular system.
4. Metal Fatigue or Structural Issues (Rare)
Rarely, stents can fracture, particularly in high-motion arteries or with certain types of mechanical stress.
Conclusion
Stents are effective, long-lasting medical devices that can significantly improve quality of life and prevent heart attacks. However, they’re not a permanent cure for heart disease unless combined with comprehensive, long-term heart care.
Key Takeaways:
- Stents can remain effective for 10-15 years or longer with proper care
- Success depends on stent type, underlying health conditions, and adherence to medical advice
- Lifestyle modifications are crucial for long-term success
- Regular monitoring allows for early detection and treatment of complications
- Many people live 15-20+ years without issues after stent placement
Taking control of your health through long-term lifestyle modifications including a heart-healthy diet, regular exercise, smoking cessation, and stress management is essential for maximizing stent effectiveness and overall cardiovascular health.
Remember: Understanding potential long-term complications like stent thrombosis or restenosis allows you to recognize warning signs early and seek prompt medical attention when necessary.
References
- https://www.news-medical.net/health/Risks-and-Side-Effects-of-Heart-Stents.aspx
- https://www.nhlbi.nih.gov/health/stents
- https://www.heart.org/en/health-topics/heart-attack/treatment-of-a-heart-attack/stent
- https://www.health.harvard.edu/heart-health/complications-after-receiving-a-stent
- https://ufhealth.org/conditions-and-treatments/stent-repair
- https://www.ahajournals.org/doi/10.1161/JAHA.120.017434
- https://www.news-medical.net/health/Risks-and-Side-Effects-of-Heart-Stents.aspx
- https://www.webmd.com/heart-disease/what-to-know-restenosis
- https://www.dxnimble.com/symptoms-of-a-stent-failure-key-insights
- https://www.dxnimble.com/how-long-to-monitor-a-stent-after-placement
- https://www.nhlbi.nih.gov/health/stents/living-with
- https://www.svhhearthealth.com.au/rehabilitation/overview-rehabilitation/overview-rehabilitation
- https://www.svhhearthealth.com.au/rehabilitation/after-coronary-angioplasty-stenting
- https://www.mountsinai.org/health-library/discharge-instructions/angioplasty-and-stent-heart-discharge
- https://www.addmoretolives.com/life-expectancy-after-stenting/
- https://med.stanford.edu/profiles/david-maron
- https://med.stanford.edu/news/all-news/2019/11/invasive-heart-treatments-not-always-needed.html
- https://abcnews.go.com/Health/HeartDiseaseLivingWith/story?id=4224509
In this Article