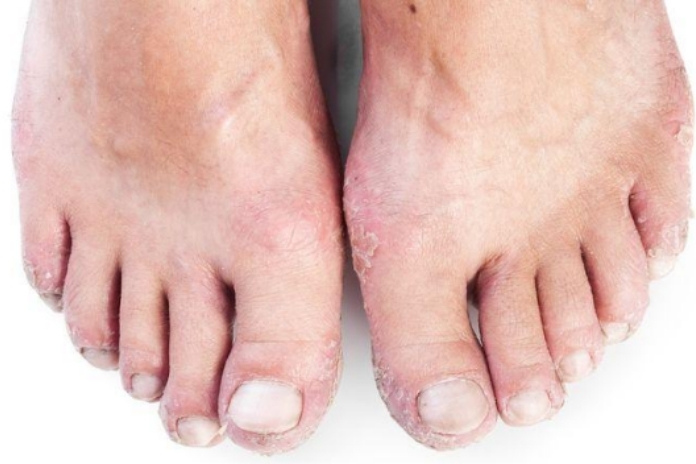
You notice the skin on your soles, heels, ankles, or between your toes never quite feels “normal” anymore – it stays dry, rough, itchy, and sometimes cracks so much that every step stings. What looks like stubborn dryness is often atopic dermatitis on the feet, a form of foot eczema where an already sensitive skin barrier is pushed to its limits by pressure, sweat, and constant rubbing from footwear.
While atopic dermatitis is usually associated with creases like behind the knees or inside the elbows, the feet are just as vulnerable and bring their own set of challenges: closed shoes that trap heat and moisture, socks that irritate, and hard floors that keep stressing inflamed skin.
This article explores why atopic dermatitis strikes the soles and toes, how to tell it apart from other common foot rashes, and the most practical ways to soothe, protect, and support your feet day to day.
Key Takeaways
- Why atopic dermatitis can appear specifically on the feet and soles, and how the warm, enclosed environment inside shoes increases flare risk.
- How to recognise foot eczema and what atopic dermatitis typically looks and feels like on the feet.
- Key differences between foot eczema and other conditions, such as fungal infections, contact allergies, or simple dry skin.
- Common foot-related atopic dermatitis triggers include shoes, socks, sweat, irritants, and friction.
- Practical changes in footwear and fabrics can help reduce flare-ups.
- Evidence-based treatment ideas for eczema on the soles of the feet and long-term management strategies for adults.
- Tips on moisturizers, gentle cleansing, and barrier-support habits.
- Clear guidance on when persistent or severe foot eczema should prompt a visit to a healthcare professional for diagnosis, prescription treatments, or allergy testing.
When Eczema Hits Your Feet — More Than Just a Rash
Imagine having persistent dryness, itching, or cracking on the bottom of your feet, your ankles, or between your toes. If this sounds familiar, you’re not alone. While atopic dermatitis is generally associated with areas like behind the knees or the insides of the elbows, it can also affect your feet, leading to unique challenges such as pressure, sweat, friction, and issues with shoes and socks.
This guide explains why your feet are vulnerable, how to recognize atopic dermatitis on the feet (and tell it apart from other rashes), and offers science-backed ways to manage flare-ups and prevent recurrences.
Read More: Flat-Feet-Vs-High-Arches-How-To-Care-For-Your-Foot-Type
Why Feet Are a “Hot-Spot” for Atopic Dermatitis
Skin Barrier and Foot Environment
Atopic dermatitis on the feet stems from a genetically weakened skin barrier and immune dysregulation. Feet are constantly exposed to friction, sweat, and the occlusive conditions created by shoes and socks. These factors further erode the barrier, making the soles especially vulnerable.
- The foot’s thicker skin and constant use require more intensive care.
- Humid microclimates in footwear increase irritation and the risk of infection.
Read More: Best-Moisturizing-Socks-Pedicure-At-Home-Feet-Treatment
Unique Foot-Specific Triggers
- Moisture accumulation (from sweat, humidity) is a primary irritant for atopic skin.
- Shoe materials & sock fabrics may contain allergens like dyes, rubber, and synthetic glues.
- Pressure points and micro-trauma (walking, standing) cause cracked skin and further barrier breakdown.
Why This Matters
Lesions from atopic dermatitis on the feet can cause significant pain, affecting mobility and daily activities, which lowers overall quality of life. The feet’s unique anatomy with thicker, tougher skin in weight-bearing areas makes managing eczema challenging. Continuous use of shoes and standing for long periods repeatedly put pressure on these vulnerable spots, often causing cracked skin and further damage to the skin barrier. Moisture buildup from sweat or humidity worsens irritation, while shoe materials and sock fabrics may introduce allergens, such as dyes, rubber, or synthetic adhesives, that trigger flares. These factors combine to make effective treatment and healing of foot eczema more difficult compared to other body parts, requiring specialized approaches focusing on both skin care and environmental trigger management.
Recognising Atopic Dermatitis on the Feet — Signs and Differential Diagnosis
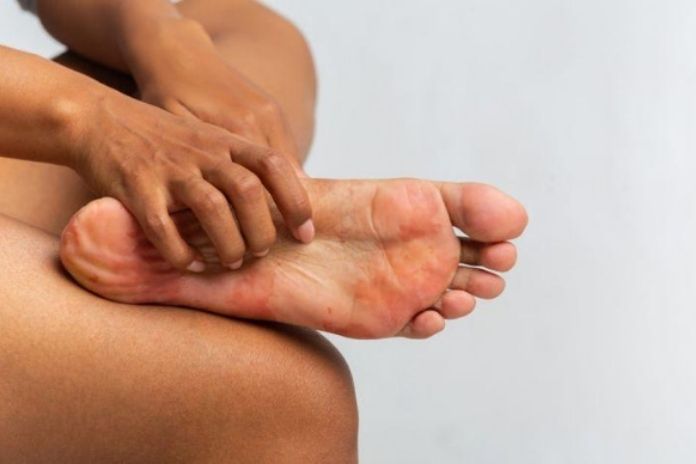
Typical Features of Foot Atopic Dermatitis
- Itchy, red-brown, or purplish patches on the soles, sides, or ankles, most common in those with a history of atopic dermatitis.
- Dry, cracked, scaling skin; possible weeping or crusting if scratched or infected.
- Bilateral involvement (both feet) occurs frequently, though not always.
Read More: Foot-Shape-Says-About-Your-Personality
Conditions Often Mistaken for Foot Eczema
- Allergic Contact Dermatitis: Caused by exposure to shoe materials/buckles; may show up in one spot.
- Dyshidrotic Eczema (Pompholyx): Features small, itchy blisters on toes/soles.
- Tinea Pedis (Athlete’s Foot): Fungal infection, often shows as ring-shaped, scaly patches, but can coexist with eczema.
When to Go for a Specialist Evaluation
Seek a dermatologist if:
- The rash is only on one foot, or is persistent, painful, bleeding, or turns warm/swollen (possible infection).
- You have a history of severe eczema, but new symptoms on the feet.
Eczema Soles of Feet Treatment: Soothing and Management Strategies

1. Core Skin Barrier Repair and Moisturisation
- Use thick, fragrance-free emollients (such as petroleum jelly or ceramide creams) immediately after washing, ideally within 3 minutes to lock in moisture.
- At night, consider occlusive moisturisers with clean cotton socks to reduce friction and prevent water loss.
- Apply moisturiser between toes, but sparingly to avoid
2. Topical Anti-inflammatory Treatments
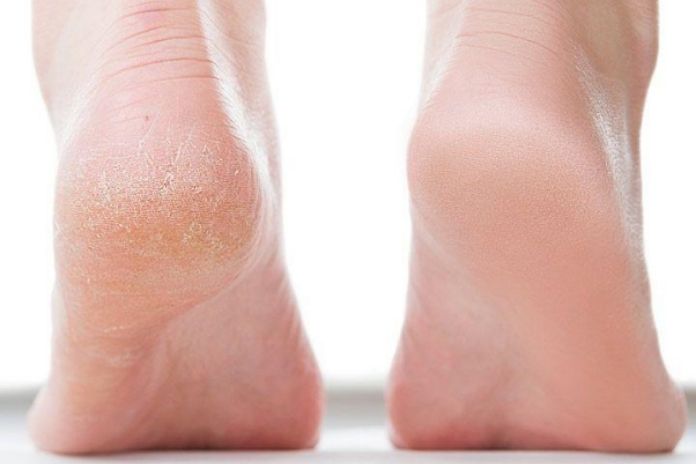
- For flare-ups: topical corticosteroids or calcineurin inhibitors (as prescribed).
- The feet may require a stronger formulation due to thicker skin, and always follow a dermatologist’s advice to minimize risks.
Read More:
10-Everyday-Triggers-Of-Atopic-Dermatitis-Eczema-Flare-Ups-And-How-To-Avoid-Them
3. Foot-Specific Habits and Footwear Adjustments
- Choose breathable, natural-material socks (cotton/wool blends) and ventilated shoes.
- Rotate shoes to allow them to dry; avoid tight or non-breathable footwear.
- Wash socks in fragrance-free detergents and avoid shoe-care chemicals.
- Use cushioned insoles if friction is an issue.
4. Preventing and Managing Triggers
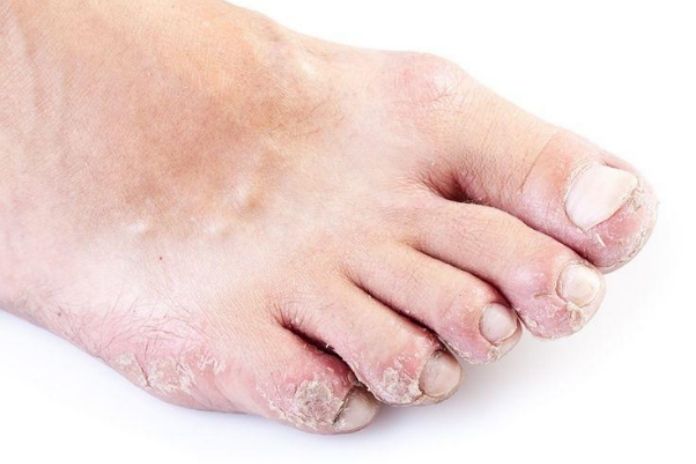
- Dry feet thoroughly after bathing, especially between toes.
- Never walk barefoot in damp communal spaces like pools, showers, or locker rooms if you have foot eczema this significantly lowers the risk of picking up fungal infections that can complicate your condition.
- Always wear flip-flops or shower shoes in these areas to protect your vulnerable skin barrier from the athlete’s foot fungus that thrives in moist public environments.
- Identify and eliminate allergens (patch-test shoes, dyes, glues if recurrent reactions occur).
- Change into dry socks often; moisture-wicking options can help those prone to sweaty feet.
5. Severe or Recurrent Cases
- UVB light therapy may be prescribed for stubborn eczema under specialist care.
- Treat secondary infections (bacterial/fungal) with appropriate medication.
- Systemic treatments may be needed for severe or widespread cases where topical methods fail.
Read More: Top-barefoot-running-shoes-for-injury-free-training-natural-movement
Quick Recap
The feet are a particularly common site for atopic dermatitis due to barrier stress, friction, sweating, and footwear. Early recognition, targeted soothing strategies, and trigger avoidance are vital for controlling flare-ups, protecting mobility, and improving quality of life.
References
- https://my.clevelandclinic.org/health/diseases/24299-atopic-dermatitis
- https://www.mayoclinic.org/diseases-conditions/atopic-dermatitis-eczema/diagnosis-treatment/drc-20353279
- https://www.medicalnewstoday.com/articles/eczema-on-feet-pictures
- https://www.webmd.com/skin-problems-and-treatments/eczema/eczema-basics
- https://piedreseau.com/en/tips-advice/5-tips-to-relieve-foot-eczema/
- https://chicagoskinclinic.com/meet-our-doctors/
- https://www.everydayhealth.com/skin-conditions/things-to-know-about-atopic-dermatitis-on-the-feet
- https://www.myeczemateam.com/resources/atopic-dermatitis-on-the-legs-pictures-and-treatments
- https://www.aafp.org/pubs/afp/issues/2020/0515/p590.html?utm_
- https://www.health.com/condition/eczema/light-therapy-atopic-dermatitis?utm_
- https://www.medicalnewstoday.com/articles/eczema-on-feet-pictures?utm_
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11627575/?utm_
- https://www.mayoclinic.org/diseases-conditions/atopic-dermatitis-eczema/diagnosis-treatment/drc-20353279?utm_
- https://www.sciencedirect.com/science/article/pii/S1578219019302264?utm_
- https://www.medicalnewstoday.com/articles/eczema-on-feet-pictures?utm_
In this Article