The world is full of triggers for those who suffer from atopic dermatitis, the most prevalent type of eczema. To just a few, the list of things that cause flare-ups includes wool clothes, laundry detergents, cigarette smoke, and bath and body products.
Redness, itching, and irritation are some of the symptoms of atopic dermatitis, also known as eczema, a persistent skin disorder. Although the precise origin is unknown, specific triggers are frequently associated with flare-ups. The first step to controlling your symptoms and maintaining the health of your skin over time is identifying these triggers.
However, some eczema triggers are less evident. While everyone will have their own inflammation, itching, and pain from varying causes, look out for these possible triggers.
Let’s review ten common eczema triggers and management strategies recommended by dermatologists.
Read More: 7 Effective Ways to Use Coconut Oil for Faster Relief from Eczema
Why Do Flare-Ups Happen?
Atopic dermatitis, often referred to as eczema, is a skin disorder characterized by dry, irritated, and itchy skin. Skin disorders are characterized differently in each person.
Doctors refer to the symptoms of eczema—such as red, itchy patches or cracked, leaking skin—as flare-ups. Flare-ups are often the result of both internal and external factors, which could vary from individual to individual.
Various factors, including weather changes, exposure to different chemicals, and certain types of clothing, can trigger eczema. As an eczema sufferer, it is essential to avoid anything that has caused flare-ups in the past, to learn what stops the itch and patch, and to find the comfort your skin needs.
Examples of eczema treatments include over-the-counter skin care products that relieve itching, as well as lifestyle changes that reduce exposure to eczema triggers.
You cannot cure eczema, but you can drastically minimize flare-ups by avoiding irritants and following a basic anti-eczema skincare plan.
10 Everyday Triggers of Atopic Dermatitis
If you have atopic dermatitis, you should be aware of these ten typical triggers.
1. Dry Skin
Dry skin is a typical cause of flare-ups of atopic dermatitis. An eczema flare can result from overly dry, fragile, harsh, or scaly skin. Developing a skin care regimen can help avoid flare-ups of eczema brought on by dry skin. Try the following to lessen the dry skin that comes from taking a bath:
- Use warm, but not hot, water for your regular bath. Your skin gets dried out by hot water.
- Baths and showers should not last longer than ten minutes.
- Dry your skin gently with a cloth.
- Use a mild, non-soap cleanser to wash.
- While your skin is still damp after taking a bath, moisturize within three minutes.
To combat dryness, moisturizing is exceptionally crucial. Make an effort to moisturize at least twice every day. Ointments, creams, lotions, and shea butter are products that aid in the retention of moisture in your skin. Petroleum jelly may help shield infants from atopic dermatitis.
2. Air fresheners and Candles

Skin responses are a well-known side effect of fragrances and scents included in cosmetics and personal care products.
However, you can also find scents in unlikely locations, including air fresheners and candles. “If a product has a scent, there could be some kind of triggering chemical in there,” says Danilo Del Campo, MD, a dermatologist with the Chicago Skin Clinic. “Candles may especially be an eczema trigger during the winter holidays. People want that holiday feel in the house, but it can cause eczema problems.”
Read More: 5 Skincare Products You Should Never Use on Sensitive Skin
3. Hot water

A long, steaming bath or shower may sound enticing. However, hot water may dry out the skin, and physicians caution that it can exacerbate eczema symptoms. Instead of taking long, hot baths, take shorter, cooler ones. In addition, you could get a severe burn at very hot temperatures.
To assist your skin in absorbing water without drying it out, take a quick daily soak in either warm or cold water. After finishing, use a towel to pat the skin dry gently. Then, to seal in moisture, apply a moisturizing cream, gel, or fatty ointment.
4. Bites of Insects
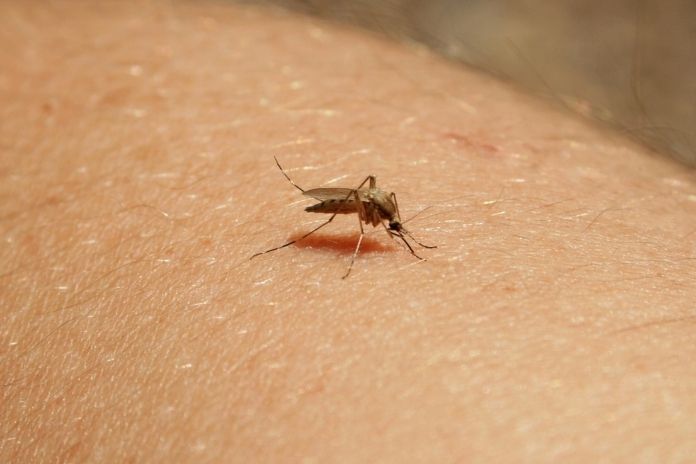
Allergic reactions to insect bites and bee stings can trigger a flare-up of atopic dermatitis.
Cockroaches don’t bite people, but proximity to them can lead to a flare, according to Edidiong Kaminska, MD, a founder and the medical director of Kaminska Dermatology in Chicago. “It’s not the cockroach itself that produces a reaction, but insects carry a lot of things on them,” says Dr. Kaminska. “
The particles it sheds can trigger an eczema reaction in the skin.” You can avoid cockroaches by cleaning your house after meals, repairing plumbing issues, sealing cracks, and clearing out debris.
5. Dry, Cold Temperatures

Your skin is already dry if you have atopic dermatitis. Climates with low humidity and cold temperatures cause your body to become even drier, which might irritate your skin. Seasonal changes might occasionally trigger symptoms as well.
Come the first cold snap in October, patients in the upper Midwest start itching, said Jon Hanifin, MD, professor emeritus of dermatology at Oregon Health & Science University in Portland, Ore. Even on rainy days in Portland, when people turn on their furnaces, symptoms ensue. “A humid climate is the best place for eczema patients to be,” said Dr. Hanifin. To prevent sweating at night, turn down the thermostat and wear light clothing.
6. Jewelry

Rings, earrings, necklaces, and other kinds of body ornaments made of nickel might cause issues, particularly if you have an allergy, but not all jewelry aggravates skin prone to atopic dermatitis. Contact eczema, a condition associated with atopic dermatitis, is often triggered by nickel allergies.
Jewelers frequently blend nickel in trace amounts with silver or white gold, making its presence in jewelry not immediately apparent. People can become allergic to nickel by being exposed to it repeatedly and for an extended period of time.
Once a person develops a nickel allergy, they remain sensitive to it and must avoid contact. Remember, buttons, zippers, snaps, and spectacles can also contain nickel.
Read More: Hives or Rash? How to Tell the Difference and When to See a Doctor
7. Sweating

Are you itching from your workout? Whether they’re performing cardio or just lounging around in damp sheets at night because they’re too hot, people with atopic dermatitis frequently have symptoms when they sweat. The body uses sweating as a natural cooling mechanism.
Sweat, however, can dry up the skin and leave a salty residue behind when it evaporates, which can make eczema worse. Reduce the intensity of the sweaty workout or choose a low-impact activity if you’re experiencing an atopic dermatitis flare-up.
8. Food Allergy and Acidic Foods

Although not common, certain foods can cause atopic dermatitis to flare, according to Del Campo. He adds that acidic foods can be a particular issue, including strawberries, tomatoes, and citrus fruits such as oranges, lemons, limes, and grapefruit. Seafood, peanuts, dairy, eggs, sugar, alcohol, and gluten can also cause common allergens and flare-ups of atopic dermatitis.
According to specialists, some people with atopic dermatitis may benefit from an anti-inflammatory diet in addition to avoiding known food allergies. This diet calls for consuming more omega-3 fatty acids and avoiding trans fats, saturated fats, refined carbohydrates, and added sugars.
9. Face Masks and Fabrics

When it comes to atopic dermatitis, fabrics that cause skin irritation or trap heat are known to cause problems. While materials composed of pure cotton, silk, or bamboo are generally more eczema-friendly, polyester, latex, wool, denim, rough linen, and leather can all exacerbate atopic dermatitis and other types of skin inflammation.
Del Campo suggests that the pandemic introduced a new skin agitator: the face mask.
Make sure the mask isn’t too tight or loose, wash your face gently, pat dry, and use moisturizer before putting it on to lessen the chance that it could trigger an eczema flare-up. After removing the mask, reapply the moisturizer.
10. Cleaners, Shampoo, and Soap

Numerous personal hygiene items can remove the natural oils that keep skin hydrated and aggravate delicate eczema skin. Avoid using bubble bath products and only use cleansers when necessary to prevent drying out your skin and exacerbating your symptoms. To assist in restoring the skin’s barrier, choose a cleanser that doesn’t irritate if you do use one.
You should avoid fragrances. Although “unscented” items can seem preferable, you should also stay away from them because they still have a disguised aroma.
Read More: 15 Effective Natural Remedies to Get Rid of Skin Rashes Easily
When to See a Dermatologist
Recognizing when eczema is worse than self-care is the first sign of when to contact your dermatologist. Eczema can typically be managed with over-the-counter topical therapies and moisturizers when symptoms are mild, but more severe symptoms may require assistance from a specialist. It’s time to contact your doctor when your eczema flare-ups include severe itching, redness, or swelling that limits your daily activities and sleep.
It’s also essential to contact your doctor when the affected skin patches are cracked or oozing, or if you have symptoms of infection, like pus or yellow crust. A dermatologist can also assess and rule out any underlying conditions that may be contributing to worsening eczema.
An advanced treatment from a dermatologist can provide better options than what you can find at the pharmacy. Doctors may use oral medications for more severe situations, but prescription topical medications relieve inflamed skin and inflammatory conditions. Phototherapy, using controlled UV light, can also improve the health of your skin to reduce inflammation.
Expert Tips to Manage Flare-Ups Daily
While eczema is incurable, there are practical solutions to relieve symptoms and minimize flare-ups. Below are some helpful tips:
- Keep Skin Moisturized often: You must keep your skin moisturized. You should be using a fragrance-free, thick moisturizer several times daily, especially after you shower, to keep moisture in and keep a barrier of protection on the skin.
- Identify and avoid Triggers: You should avoid all triggers that aggravate your eczema. You may need to start using a humidifier if the environment is dry, switch to softer clothing that breathes better, or even change the skin care product you are using.
- Take quick Showers in lukewarm Water: Hot water can aggravate and dry the skin. You should take timely showers and/or mild hypoallergenic soap and lukewarm water.
- Use an Anti-Inflammatory lotion with Hydrocortisone: Over-the-counter lotion with hydrocortisone can help reduce inflammation and itch. If you are having more severe problems or problems that don’t go away, your dermatologist can give you more potent oral or topical medicine.
- Limit or Eliminate Stress: Stress has a way of triggering eczema flare-ups. You can work on controlling stress-induced eczema symptoms by incorporating yoga, meditation, or deep breathing techniques into your daily life.
Read More: How to Treat a Rash on the Neck
Conclusion
While flare-ups can happen at random times, there is usually a natural factor involved that may have caused the flare-up or reaction. For example: dryness, soaps used on the skin, humidity or weather changes, stress, or environmental allergies. Understanding all the factors will help you start to understand why your skin acts the way it does.
The main take-home message is quite simple. Suppose you can identify your triggers and wear them with a consistent skincare routine that includes protecting and moisturizing your skin daily and using non-irritating products. In that case, you will likely experience fewer and less severe flare-ups overall. A simple lifestyle change can keep your skin more comfortable and calm!
FAQs
- Can stress alone cause an eczema flare-up?
Yes, stress is a very common trigger that can exacerbate eczema flare-ups by weakening the skin barrier and increasing inflammation in the body. The body produces cortisol and other kinds of stress hormones when under stress, which can weaken the immune system and exacerbate skin inflammation, resulting in symptoms like rashes, itching, and flaky, dry skin.
- Is eczema always triggered by food?
No, it’s not always food that’s to blame. Allergens, irritants, dry skin, and stress are some of the many things that can cause eczema. Some people may be affected by food sensitivities, but not everyone is.
- Does atopic dermatitis ever go away?
Atopic dermatitis has no known cure; thus, even after therapy, the rash usually returns. For this reason, it’s critical to be aware of your triggers and steer clear of them.
References
- https://www.myeczemateam.com/resources/triggers-of-atopic-dermatitis
- https://www.cerave.com/skin-smarts/skin-concerns/eczema/living-with-eczema-common-triggers-and-everyday-tips-for-relief
- https://www.happyskindermatology.com/2025/05/16/top-common-eczema-flare-up-triggers-you-should-know/
- https://www.everydayhealth.com/eczema/surprising-triggers-for-atopic-dermatitis-eczema-flares/
- https://chicagoskinclinic.com/meet-our-doctors/
- https://www.health.com/condition/eczema/atopic-dermatitis-triggers
- https://www.kaminskadermatology.com/provider/edidiong-kaminska-md-mbs
- https://www.doximity.com/pub/jon-hanifin-md
- https://plymouthmeetingdermatology.com/see-doctor-about-eczema/
- https://www.mayoclinic.org/diseases-conditions/atopic-dermatitis-eczema/diagnosis-treatment/drc-20353279
- https://alamoheightsderm.com/expert-tips-for-managing-eczema-and-keeping-your-skin-healthy/
In this Article















