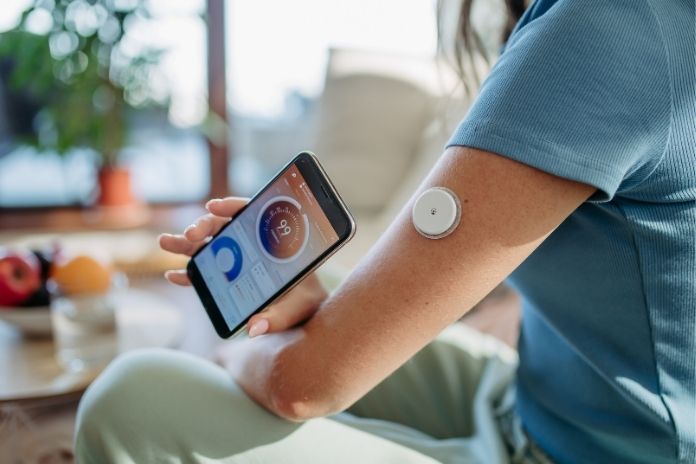
Continuous glucose monitors (CGMs) were first designed for people with diabetes, for whom finding and preventing hypoglycemia can be lifesaving. Today, CGMs are increasingly worn by people without diabetes. Several athletes, sports enthusiasts, weight-loss seekers, and individuals interested in metabolic health swear by CGMs.
As CGMs move into this non-clinical space, a new problem has emerged. The issue is interpreting numbers without the medical context in which they were designed.
The most common shock for non-diabetic CGM wearers is to receive a low glucose alert, usually below 70 mg/dL, and feel no symptoms whatsoever. No shaking, sweating, dizziness, or confusion, just a notification that suggests something is wrong. In most cases, it isn’t.
What is usually happening is false hypoglycemia, a situation where the CGM reports a low value that does not reflect true blood glucose levels or physiological danger. Understanding why this happens requires understanding how CGMs actually work, how human glucose regulation functions in healthy people, and the device limitations.
Read More: Needle-Free Blood Sugar Monitoring: How Continuous Glucose Monitors Work & Which One Fits You
What It Means When Your CGM Says “Low” But You Feel Fine
A CGM low alert is based on thresholds that were created for diabetes care, not healthy metabolism. For clinical use, an early warning threshold below 70 mg/dL is used since individuals with diabetes may not be able to self-correct efficiently. In a nondiabetic individual, this same regulation is much more dynamic and resilient.
True hypoglycemia is not defined by numbers alone. Clinically, it is characterized by a combination of low blood glucose levels and associated symptoms. An asymptomatic low reading on a CGM by itself does not define a medical problem.
This discrepancy appears significant due to the difference between interstitial glucose and blood glucose. CGMs measure glucose in the interstitial fluid. This is the fluid surrounding your cells, not inside your bloodstream. Interstitial glucose generally reflects blood glucose, but inaccurately and with a time delay. That gap is where many CGM false low readings originate.
The Science Behind False Hypoglycemia
Compression Lows
Another common reason for false readings about hypoglycemia for those who aren’t diabetic and use CGMs is the pressure. When you sleep and turn on one side or your stomach, the area where the CGM is placed gets pressed. The pressure impacts blood flow to that area and reduces glucose diffusion rates into or out of the interstitium.
As long as the CGM requires an adequate flow of glucose into this space, this temporary compression will trick the sensor into registering a lower glucose level than it actually is. These lows tend to appear quickly, usually during the nighttime hours. However, they immediately resolve when the pressure is removed. This does not cause any symptoms because it isn’t dropping to extremely low levels.
Physiological Lag Time
Even without any additional compression, there is an inherent delay in continuous glucose monitors (CGM). It is based on the time difference between the blood sugar values in real time and what is being reflected by interstitial fluid values. This varies from a few minutes to over ten minutes based on how quickly the sugar levels change.
After exercise, during recovery from stress, or when a spike in glucose levels rapidly follows a meal, the actual glucose level in the bloodstream could already be trending toward a flat level when the interstitial level appears briefly reduced. At these points, a CGM can potentially provide a low value when it doesn’t correspond with a blood level.
For a healthy, controlled individual, a delay can result in abnormal findings when something is normal physiologically.
Sensor Warm-Up and Calibration Effects
The new sensors in CGM systems are not fully reliable in the first one or two days. Since these sensors are introduced in the body after insertion by the individual, it causes slight injury to the tissue along with inflammation around the sensor filament, leading to glucose fluctuations in that area.
You will commonly see spurious lows at night in the first 24 to 48 hours of starting the system. Such an occurrence doesn’t indicate that there’s a problem with glucose control. It is a process of tissue adaptation. Therefore, one must check the trends rather than the specifics during this initial phase.
Device Accuracy and MARD
Continuous glucose monitors are highly advanced technologies, but they are still only estimates. Their accuracy is determined by MARD, which is the mean absolute relative difference. MARD shows the levels at which the readings from continuous glucose monitors correlate with actual blood glucose laboratory results.
An MARD of 9 to 10%, as is common with current continuous glucose monitors (CGM), indicates small numerical discrepancies are to be expected. With this, where a CGM displays a reading in the high 60s, this could very well represent a normal value of blood glucose. However, normal variation could be misinterpreted as an issue when those without diabetes interpret readings this way.
Read More: Best Continuous Glucose Monitor (CGM) in 2026: What to Look For and Top Picks
Other Factors That Can Trigger False Lows

Hydration is essential when it comes to CGM accuracy. The interstitial glucose you’re measuring depends on the level of adequate fluid in the body. Even mild dehydration can sometimes make those downward swings significant. This tends to show up in people who work out a lot, follow low-carb eating plans, or spend time in saunas.
Temperature also plays a role in how the sensor behaves. Very hot or very cold temperatures can impact the sensor’s chemistry, briefly altering enzyme activity and presenting incorrect CGM readings. Hot tubs, cold baths, and extreme outdoor weather are common culprits behind unexplained low alerts.
Certain medications and compounds can also deceive sensor readings. Salicylic acid, the active ingredient in aspirin and several topical preparations, can impact some models of CGM. It tends to be a small effect, but it can play into consistent low alerts that don’t seem to match how you are feeling.
Finally, keep in mind that normal individuals naturally experience some glucose-lowering overnight. Research indicates that asymptomatic values less than 70 mg/dL may occur during REM and deep sleep with no injury. These are transient and self-correcting and simply a manifestation of normal metabolic regulation, not dysfunction.
What to Do When Your CGM Reads “Low” and You Feel Fine

Step 1—Confirm with a Fingerstick
In cases where your CGM indicates a low when you do not feel any symptoms, first confirm it before correcting. The only correct way to determine whether a reading is false or a real low is to use a finger-prick blood glucose. BG checking by a finger prick is still considered the gold standard.
“Clinicians need to tell them if you don’t feel like your sugar is low and the device says it’s low, whether they do or don’t have diabetes, they should do a fingerstick glucose test to confirm the low before rushing to take in sugar,” says Dr. Shichun Bao, MD, PhD, Diabetes Technology Program Leader at the Vanderbilt Eskind Diabetes Clinic of Vanderbilt University in Nashville, Tennessee.
Step 2—Inspect the Sensor Site
If your fingerstick value is normal, then check your sensor site to ensure there are no problems that could cause error readings, such as pressure on the site, exercise, your level of hydration, alcohol consumption, sleep position, or just placing a new sensor on your body.
Step 3—Review Contextual Factors
Before taking action on a low alert, take a moment to consider what you were doing when the glucose level was measured, including recent eating, exercise, hydration levels, alcohol consumption, stress, and sleep. Often, false alarms about hypoglycemia will trigger when a CGM is triggered by exercise, overnight sensor pressure, or temporary fluid shifts.
Step 4 – Track Patterns:
Typically, one low result is not significant. When there are lows at about the same times or situations often enough, it indicates a mechanical or behavioral pattern. A journal of lows over time helps distinguish between false lows and lows that require further exploration.
When to Seek Medical Advice
However, recurring or symptomatic hypoglycemia, or false hypoglycemia, should not be overlooked. When it is recurrent or occurs along with symptoms such as sweating, trembling, palpitations, confusion, or vision changes, it becomes suggestive of true hypoglycemia.
Healthcare professionals can then check for potential underlying causes like reactive hypoglycemia, hormone imbalances, or rare genetic disorders. For patients who do not have diabetes, CGM results should aid in professional judgment but should not substitute it.
Read More: Signs You Passed Your 3-Hour Glucose Test (and What the Results Mean)
Key Takeaways
Generally, the low CGM readings in healthy people do not always indicate an emergency. Trends reflect the manner in which the interstitial glucose concentration is assessed, the device’s inherent inaccuracy, and physiology. Factors such as compression lows, lag time, hydration, and sensor warm-up drive the association with falsely low readings of hypoglycemia.
Taking up a fingerstick prick test for confirmation, interpreting numbers correctly, and checking symptoms, not numbers, is essential for safe and effective use of a CGM. When used wisely, a CGM can provide valuable information, provided you understand its limitations.
References
- National Center for Biotechnology Information. (2023). Hypoglycemia. In StatPearls. StatPearls Publishing.
- National Center for Biotechnology Information. (2023). Blood glucose monitoring. In StatPearls. StatPearls Publishing.
- Edelman, S. V. (2022, February). CGM values vs. finger sticks: How close should the values be? Taking Control of Your Diabetes.
- Diabetes Care Editors. (2024). Consensus considerations and good practice points for continuous glucose monitoring systems. Diabetes Care, 47(12), 2062–2074.
- Diatribe Editorial Team. (2023). Medications to avoid when wearing a continuous glucose monitor. diaTribe.
- Veri Editorial Team. (2023). Why does blood sugar drop at night?
- Glucosense Editorial Team. (2023). CGM accuracy troubleshooting: False lows and highs explained. Glucosense.
- Chuwi Health. (2023). The role of hydration: Water’s underrated effect on glucose readings.
In this Article