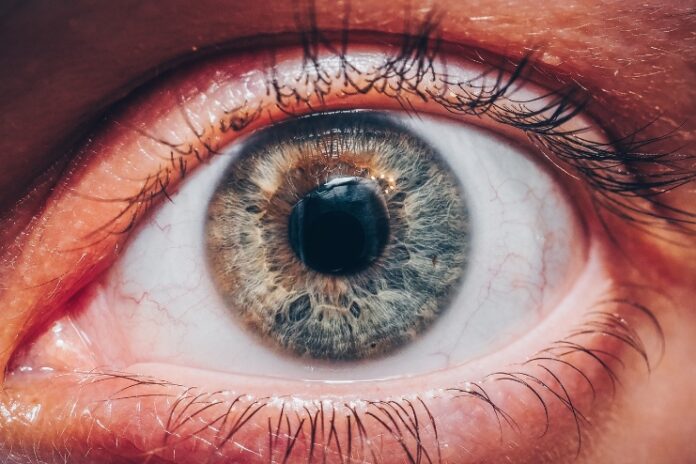
- Diabetic macular edema (DME) causes fluid buildup in the retina that can blur or distort vision. It’s a serious but treatable complication of diabetes.
- The condition often requires regular anti-VEGF injections, monitoring, and consistent diabetes management.
- While the treatment schedule can feel overwhelming, modern therapies help many people preserve useful vision for years.
- Visiting a retina specialist early and discussing injection anxiety openly can improve treatment outcomes and long-term eye health.
Some days, vision is manageable. Other days, floaters may drift across everything, faces blur, and text on a phone becomes a guessing game. That’s what diabetic macular edema daily life can look like, and it’s not consistent, which is part of what makes it so hard to plan around.
DME is the leading cause of vision loss among people with diabetic retinopathy, affecting more than 750,000 Americans over the age of 40. Most content about it explains what it is. This article explains what it is actually like to live with it, from how DME symptoms disrupt daily routines to what diabetic macular edema treatment involves week to week.
Read More: Understanding the Impact of High Blood Sugar on Vision
The Biology Behind the Blurriness, Explained Simply
Diabetic macular edema develops when high blood sugar damages the small blood vessels in the retina, causing them to leak fluid into the macula, the part of the retina responsible for central vision. The macula is what you use to read, recognize faces, and see fine detail. Think of it as the lens of a camera. DME is fluid getting trapped behind it.
The process involves breakdown of the blood-retinal barrier, drainage dysfunction, and inflammation, all of which cause the retinal layers to swell in ways that distort and blur the sharpest part of what you see. It can affect one or both eyes. It develops as a complication of diabetic retinopathy, and the longer blood sugar has been poorly controlled, the higher the risk.
Dr. Lloyd Paul Aiello, MD, PhD, Professor of Ophthalmology at Harvard Medical School and Director of the Beetham Eye Institute at Joslin Diabetes Center, Boston, explains, “Anti-VEGF drugs act like spot welders, plugging the leakage. This prevents the formation of these problematic new vessels and can cause ones already present to resolve.”
Central vision is the sharp, focused vision you use for reading and faces. DME specifically damages this, not peripheral vision. That is why people can walk around fine while being unable to read a screen at arm’s length.
How DME Changes Daily Life

The Vision Changes Nobody Warns You About
Diabetic retinopathy and DME are associated with poor self-reported visual functioning, reduced well-being, and lower health-related quality of life. The ability to perform basic everyday tasks drops as the disease progresses.
Reading text on a phone, driving, recognizing faces across a room, and working at a computer all become unreliable or impossible during flare-ups. The word “unreliable” is the part that does not come through in clinical descriptions. It is not simply that vision is bad. It is that it changes.
The Invisible Burden
For the most part, DME vision loss is invisible to others. People with the condition can look completely fine from the outside while their vision is anything but. That disconnect makes it genuinely difficult to explain to employers, family members, and healthcare providers what diabetic macular edema daily life actually involves on a bad day.
One patient described restructuring her entire career after DME made the unpredictability of her vision incompatible with her previous role in retail management. She eventually found work she could schedule around her injection appointments, taking the day off after each procedure to recover. That kind of life reorganization is common. It just rarely makes it into clinical intake forms.
The Appointment Burden Is Real
In a global survey across 78 clinics and 24 countries, the most commonly reported patient challenges around DME treatment were traveling to the clinic, cited by 48.4% of patients, long waiting times at 48%, and managing other chronic health conditions simultaneously at 45%. More than a quarter of patients doubted at some point whether their treatment was even necessary.
Dr. Rishi P. Singh, MD, Chair of Ophthalmology at Mass Eye and Ear/Harvard and former Clinical Professor at Cleveland Clinic, puts the burden plainly, “We always want to strive to treat our patients less… Some of these people are working age, or they have caregivers who need to bring them, so they’re often always worried about how they can get into the office.”
The Emotional and Mental Health Impact

Anxiety, Depression, and the Weight of the Diagnosis
Research has found that quality of life can be affected by DME before significant vision loss has even occurred. Anxiety about the future and the emotional weight of diagnosis and treatment itself can diminish well-being early in the disease course.
Severity of disease, higher anxiety levels, and unemployment were all found to be significantly and negatively associated with quality of life in people with diabetic retinopathy and DME.
The Mental Load of Injections
Patients living with DME describe pain, intravitreal injection anxiety, and the challenge of attending frequent appointments as ongoing burdens that do not stay inside the clinic. The rhythm of injections creates an anticipatory anxiety that touches the weeks leading up to each appointment, not just the procedure itself.
Nearly half of DME caregivers in a multinational study reported persistent concern and worry, and some described managing their own distress alongside the patient’s.
Dr. Monika Fleckenstein, MD, professor of ophthalmology and retina specialist at the Moran Eye Center, University of Utah, addresses intravitreal injection anxiety, “I can absolutely understand that you are scared. I would be scared as well… But again, it’s fast, usually, it’s safe, we don’t have a lot of complications, and it’s proven that it helps.”
Anxiety about DME is not a weakness. It is a documented, well-studied response. Informing a doctor about it is a clinical step, not an overreaction. Clinical teams can adjust protocols, anesthesia, and appointment pacing when they know.
How DME Is Treated, and What Patients Actually Experience
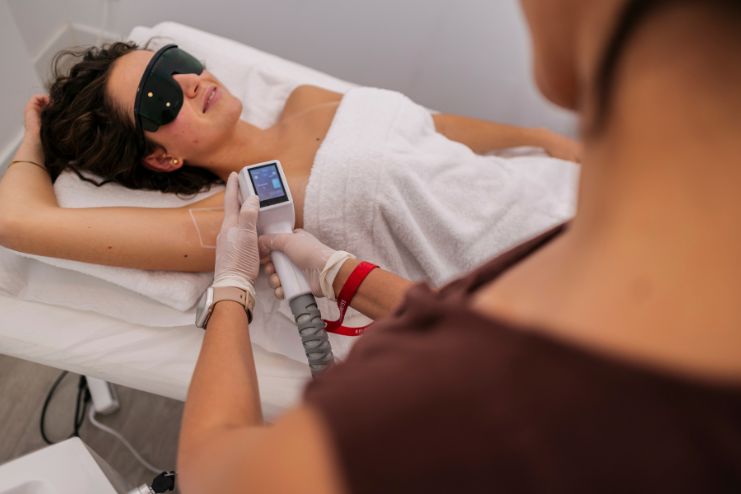
Anti-VEGF Injections: The First-Line Reality
The standard of care for center-involving DME is intravitreal injection of anti-VEGF agents. Three main drugs, aflibercept, ranibizumab, and bevacizumab, have shown efficacy in clinical trials for reducing central retinal thickness and improving visual acuity.
In practice, injections are administered directly into the eye at regular intervals, often monthly during the loading phase, then extended as vision stabilizes. Despite overall improvement in many patients, more than 30% still experience persistent DME even after four or more injections.
VEGF alone does not fully explain the condition in all patients, and additional pathways remain under active investigation. This is why some people respond well quickly, and others require extended or alternative regimens.
Data from a PHOTON clinical trial showed that most patients treated with the higher-dose formulation achieved dosing intervals of 12 weeks or more at 3 years, representing a meaningful reduction in the appointment burden that weighs most heavily on DME quality of life.
Other Treatment Options
Corticosteroid implants are used when the anti-VEGF response is insufficient. They are longer-lasting but carry risks of elevated eye pressure and cataract formation. Laser photocoagulation is an older approach now used more selectively, often in combination with injections.
Faricimab, approved in 2022 by the FDA, targets both VEGF-A and Ang-2 and has extended dosing intervals to every 16 weeks in some patients, directly reducing the frequency burden that affects daily life.
The Role of Blood Sugar Control
Managing HbA1c is not just diabetes care. It is directly protective for the eyes. Poor glycemic control accelerates DME progression and reduces how well treatment works. Every percentage point improvement in HbA1c is meaningful.
This is the one lever that patients can pull independently of injections, and it matters throughout the entire course of the condition, not just at diagnosis.
Practical Ways to Manage Life With DME
Build a care team around the whole condition. A retina specialist handles the eye. An endocrinologist handles blood sugar. A mental health professional is worth considering if intravitreal injection anxiety is affecting treatment adherence, which it measurably does.
Tell your doctor about injection anxiety directly. Patients who discuss their fears with their retina specialist report better experiences and higher adherence. Clinical teams can adjust anesthesia protocols, appointment pacing, and pre-procedure communication when they know anxiety is present.
Protect the vision you have. Use high-contrast settings on devices, good lighting, and magnification tools without shame. Adaptive technologies are practical tools, not signs of giving up.
Build schedule flexibility where possible. Many patients find that planning recovery time after injection days reduces the cascading disruption to work and family that builds up over the months of treatment.
Connect with others living with DME. Systematic review evidence supports patient-reported benefit from peer connection, particularly around injection anxiety and adherence to treatment schedules.
Read More: Home Remedies for Healthy Eyes: 6 Tips to Support Vision Naturally
Conclusion
Living with diabetic macular edema is hard in ways that are not always visible, not always in the medical notes, and not always understood by people who have not experienced it. It is invisible. It is unpredictable. It is treatment-intensive. And it sits on top of an already demanding diabetes management routine.
It is also not a sentence. With consistent DME treatment, regular monitoring, and blood sugar control, many people preserve meaningful central vision for years. If you are newly diagnosed, ask your retina specialist about treatment scheduling flexibility.
Share about any anxiety you might be experiencing around anti-VEGF injections for DME. It changes what they can do for you, and that conversation is part of the clinical care.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare provider for diagnosis and treatment decisions.
Frequently Asked Questions
1. What does it actually feel like to live with diabetic macular edema?
Most people describe it less as total vision loss and more as unreliability. Some days, vision is close to normal. Other days, there is a blurry smear or a dark spot right in the center of what they are trying to look at, making reading, recognizing faces, and screen work genuinely difficult. Floaters can move across the field of vision without warning. The unpredictability is what patients find hardest to explain, because from the outside, nothing looks wrong.
2. Can diabetic macular edema cause complete blindness?
DME vision loss targets the macula specifically, so peripheral vision often stays largely intact. It does not typically cause complete blindness the way some other conditions do. That said, severe or long-standing diabetic macular edema without adequate treatment can reach a level of central vision impairment that makes driving, reading, and independent daily function very difficult.
3. Is the injection painful? What do patients actually say about it?
Most patients say the anticipatory anxiety is considerably worse than the procedure itself. The eye is numbed beforehand, so the injection typically feels like pressure rather than sharp pain. A minority experience more discomfort, and clinical teams can adjust the anesthesia protocol when they know. Telling your retina specialist about intravitreal injection anxiety before your first appointment changes how the procedure is managed.
4. How does blood sugar affect diabetic macular edema?
Blood sugar control DME is not separate from treatment; it is part of it. High HbA1c accelerates damage to the small retinal blood vessels that drive diabetic retinopathy and macular edema, and also reduces how well anti-VEGF injections work. Every meaningful reduction in HbA1c reduces both the risk of progression and the rate at which fluid re-accumulates between visits.
5. Can DME be reversed, or is the damage permanent?
When caught early and treated consistently, anti-VEGF injections DME can meaningfully reduce macular swelling and improve visual acuity. Some patients recover substantial central vision. If diabetic macular edema has been present for a long time before treatment begins, or if retinal layers have undergone structural changes, some damage may not fully reverse. Early diagnosis and consistent adherence matter more than most people realize.
6. Why do some people with DME not respond to anti-VEGF injections?
More than 30% of people with DME experience persistent swelling even after multiple injections because VEGF is not the only driver of the condition. Inflammation and blood-retinal barrier breakdown continue independently. When that happens, retina specialists may switch agents, add a corticosteroid implant, or consider faricimab, which targets both VEGF-A and Ang-2 simultaneously.
7. What should I tell my doctor if I am struggling emotionally with DME treatment?
Tell them directly. DME quality of life research consistently shows that the emotional burden of this condition is real and measurable, and intravitreal injection anxiety is documented in the clinical literature. Your retina specialist can adjust pacing, modify the numbing protocol, and prepare you better for each visit when they know. If the weight of the diagnosis extends beyond the clinic, asking for a referral to a mental health professional is a clinically appropriate step.
References
- Aiello, L. P. (2021). From high blood sugar to vision loss with DME. HealthCentral.
- Do, D. V. et al. (2024). Intravitreal aflibercept 8 mg for diabetic macular edema: 96-week results from the randomized Phase 2/3 PHOTON trial. Ophthalmology.
- Fleckenstein, M. (2023). What to expect with intravitreal injections. University of Utah Health.
- Mitchell, P. et al. (2021). Patient burden in DME: Global survey of 78 clinics.
- Sivaprasad, S. et al. (2016). Impact of injection therapy on retinal patients with DME or RVO. PubMed.
- Singh, R. P. (2023). Extending treatment intervals in nAMD and DME. HCPLive.
- Wieder, M. S. (2020). Improving patient comfort with intravitreal injections. Modern Retina.
- Loerzel, A. (2025, June 22). How has diabetic macular edema affected your daily life? HealthCentral.
- Everyday Health. (n.d.). The world is not set up for people with diabetic macular edema.
In this Article