You stand up fast, smack your head on a cabinet, swear under your breath, and move on. Later, in the shower, you run your fingers over your scalp and wince. There’s a sore spot. Maybe even a little bump. Now your brain kicks in: Is this just a bruise… or something serious? Concussion? Bleeding? Should I be worried?
Mild head bumps are incredibly common, and most of them heal without drama. But sometimes, that pain when you touch the spot, or the symptoms that show up afterward, can be a warning sign of something deeper: a concussion, a scalp hematoma, or, in more serious cases, a skull fracture or bleeding inside the skull.
Knowing the difference between “annoying but harmless” and “you need a doctor now” is the entire game here. This guide walks you through what that sore spot can mean, which red flags you absolutely can’t ignore, how to treat mild bumps at home, and when you should stop guessing and get evaluated, including when you should go straight to the ER.
Quick safety note: This article is for information, not diagnosis. If you’ve had a head injury and are worried, especially if you notice confusion, worsening headache, vomiting, or trouble staying awake, get medical help immediately.
Key Takeaways: What You’ll Learn
- The most common reasons your head hurts when you touch it after you bump it are.
- How to recognize warning signs that suggest more than a simple bruise.
- Safe first-aid and home care steps for mild injuries.
- Clear guidance on when to call a doctor, urgent care, or head straight to the ER.
Common Causes of Pain After Hitting Your Head
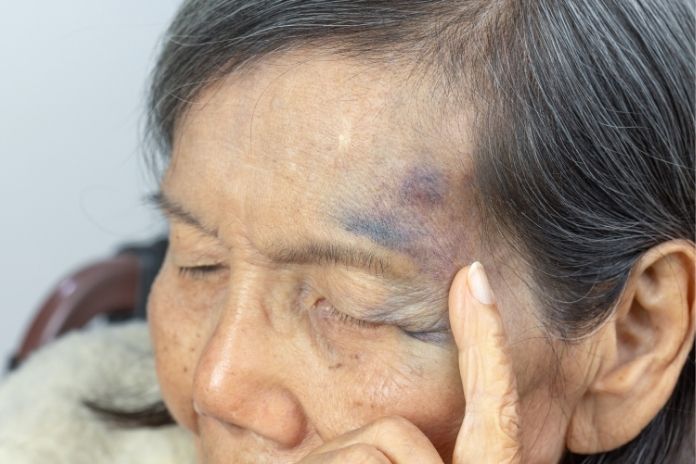
When you hit your head, several layers can be involved: skin, connective tissue, the scalp’s blood vessels, the skull, and the brain itself. Pain when you touch the area usually comes from irritated tissue in one of those layers, but the implications are very different depending on what’s been damaged.
1. Minor Soft Tissue Injury (Bump or Bruise)
The most common outcome of a low-force hit, like banging your head on a cabinet or car door, is a soft tissue injury.
What’s happening here is simple:
- Tiny blood vessels under the skin break.
- Local tissue becomes inflamed.
- You get pain, mild swelling, and tenderness when you press on the area.
In these cases:
- Pain is localized right where you hit your head.
- You feel it mainly when you touch or bump the spot again.
- You don’t have confusion, vision changes, vomiting, or trouble walking.
With rest and cold packs, this kind of bruising usually improves over a few days. That’s the “annoyed but stable” category of head injury.
2. Scalp Contusion or Hematoma
A scalp contusion is essentially a deeper bruise. A hematoma is a small pool of blood under the skin or soft tissues of the scalp, which causes a raised lump that’s painful to touch.
Because the scalp has a rich blood supply, even minor trauma can produce a dramatic-looking “goose egg.” You may notice:
- A visible lump where you were hit.
- Skin that’s swollen, possibly discolored.
- Pain when you press on or move the overlying area.
In many healthy adults, a small scalp hematoma is uncomfortable but not dangerous, as long as:
- Neurologic symptoms (like confusion or weakness) are absent, and
- Symptoms gradually improve over 24–48 hours instead of getting worse.
However, deeper hematomas, such as epidural, subdural, or intracerebral hematomas, can form inside the skull and compress the brain. These are medical emergencies and usually come with significant symptoms beyond just a tender lump.
3. Concussion (Mild Traumatic Brain Injury)
A concussion is a type of mild traumatic brain injury (mTBI) caused by a blow or jolt to the head or body that makes the brain move inside the skull. You can have a completely normal-looking scalp and still have a concussion, or you might have a tender area plus internal symptoms.
Key points from CDC and Mayo Clinic on concussion:
- Loss of consciousness is not required. Many concussions happen without blacking out.
- Symptoms can appear immediately or develop over hours to days.
Common concussion symptoms include:
- Headache or feeling of pressure in the head.
- Dizziness or balance problems.
- Nausea or vomiting (especially soon after the injury).
- Sensitivity to light or noise.
- Feeling “foggy,” slowed down, groggy, or confused.
- Trouble concentrating or remembering events before/after the hit.
- Irritability, unusual emotional swings, or sleep changes.
Tenderness at the impact site often coexists with these symptoms, but the bigger concern is what’s happening inside the skull, not just on the surface.
On symptoms, typical signs of concussion as listed by CDC include headache, dizziness or balance problems, nausea, sensitivity to light or noise, changes in sleep, and cognitive difficulties such as confusion or memory problems.
4. Skull Fracture or Deeper Bleeding (Serious)
A skull fracture can occur from a higher-force blow (falls from height, motor vehicle crashes, heavy objects) or sometimes from what didn’t seem like a huge hit, especially in older adults or people with thinner bones. These injuries may be associated with:
- Sharp, severe, or persistent pain at one spot on the skull.
- A “step-off,” depression, or soft area you can feel in the bone.
- Swelling plus bruising around the eyes (“raccoon eyes”) or behind the ears (“Battle’s sign”).
- Bleeding or clear fluid from the nose or ears.
- Worsening headache, vomiting, confusion, seizures, or loss of consciousness.
Deeper bleeding, such as epidural or subdural hematomas, may present with initially mild symptoms and then sudden deterioration as blood builds up and compresses the brain. In some chronic subdural hematomas, symptoms may not appear for days or weeks, especially in older adults or people taking blood thinners.
These are “don’t wait and see” situations. They require immediate ER care and usually CT scanning.
Warning Signs: When Head Pain May Be Serious
Most minor bumps don’t lead to serious complications, but when they do, the signs are there if you know what to look for. Major health organizations align on a core set of red flags after a head injury.
Seek emergency medical care right away (ER or emergency number) if you notice:
- Headache that keeps getting worse, not better.
- Persistent or repeated vomiting.
- Confusion, disorientation, or difficulty recognizing people or places.
- Memory loss about what happened before or after the injury.
- Drowsiness or trouble staying awake, especially if it seems to be increasing.
- Unequal pupils (one larger than the other).
- Slurred speech, weakness in an arm or leg, trouble walking, or loss of balance.
- Seizures (shaking or convulsions).
- Clear fluid or blood leaking from the nose or ears.
- Any loss of consciousness, even briefly.
In children, you also watch for:
- Unusual irritability or inconsolable crying.
- Won’t eat or nurse.
- Difficulty waking or staying awake.
- Not acting like themselves (less responsive, less playful).
If any of this shows up, or your gut says “something is off”, don’t overthink it. Get checked.
Read More: Headache Hacks: 6 Simple Breathing Exercises to Soothe Your Mind and Relieve Pain
What to Do Right Away (First Aid Steps)
If you or someone nearby hits their head and seems alert and stable, basic first aid can reduce discomfort and help you catch early warning signs. Most major guidelines are consistent on the basics.
1. Stop and assess
- Stop what you’re doing. Sit or lie down somewhere safe.
- Quickly check: Are you fully awake? Can you speak clearly? Any obvious confusion, weakness, or heavy bleeding? If yes to any serious symptom, call emergency services.
2. Apply a cold compress
- Use an ice pack or a bag of frozen peas wrapped in a thin cloth.
- Apply over the tender area for 15–20 minutes at a time, several times during the first 24 hours.
- This helps reduce swelling and numbs some of the pain.
3. Be careful with pain medication
For a simple bump with no red flags, many guidelines advise:
- Acetaminophen (Tylenol) is usually the preferred first-line pain reliever after a head injury.
- Avoid aspirin and NSAIDs (like ibuprofen, naproxen) in the first 24–48 hours after a significant head injury or suspected concussion unless your doctor specifically says otherwise, because they may increase the risk of bleeding.
If you’re already on blood thinners or daily aspirin for heart disease, do not change or stop them on your own; talk to a doctor urgently if you’ve had a head injury.
4. Rest: both physically and mentally
For the first 24–48 hours after a head injury, most concussion and TBI guidelines recommend:
- Avoid heavy exercise, sports, or anything that risks another head impact.
- Limit intense screen time, loud environments, and tasks that require heavy concentration if you feel symptomatic.
- Light, quiet activity around the house is usually fine if you feel up to it.
5. Monitor for the next 24+ hours
Even if you feel okay at first, symptoms can evolve. Someone should ideally check on you for the next day (especially overnight) to make sure you:
- Wake normally.
- Are you thinking clearly?
- Don’t develop new or worsening symptoms (headache, vomiting, confusion, weakness).
If anything seems off, that’s your cue to seek urgent care.
Home Care for Mild Head Tenderness
If you’ve had a minor bump, no red flags, and a doctor (or urgent care) isn’t worried about serious injury, home care focuses on comfort and gradual return to normal.
First 24–48 hours
- Continue cold packs for 10–20 minutes several times a day to limit swelling and numb the soreness.
- Use acetaminophen as directed for pain.
- Stay hydrated, eat normally if you don’t feel nauseated.
- Avoid alcohol, sedatives, or recreational drugs, which can mask symptoms and delay recognition of deterioration.
After 48 hours
- If swelling is down but the area still feels tight or sore, you can switch to warm compresses to help relax muscles and increase blood flow.
- Gradually return to routine activities as long as they don’t worsen headaches or other symptoms. If work, driving, or screen time makes symptoms flare, dial it back and talk to your doctor.
According to the Cleveland Clinic (on the RICE method), ice (cold therapy) is recommended immediately after a soft tissue injury; rest, ice, compression, elevation, to reduce inflammation, swelling, pain, and bleeding in the first phase of healing.
If a visible lump or significant tenderness persists beyond 7–10 days, or the pain actually gets worse instead of better, it’s time to follow up with a healthcare professional.
Read More: 8 Immediate Actions to Take in Case of a Head Injury
When to See a Doctor or Go to the ER

You don’t need to rush to the ER for every bump on a cabinet. But you also don’t want to shrug off something serious.
Call your doctor / urgent care within 24 hours if:
- The sore spot and headache aren’t improving after a day or two.
- Pain is mostly when you touch the area, but you feel more tired, “off,” or foggy than usual.
- You’ve had a concussion or head injury before, and this one feels different.
- You notice mild dizziness, difficulty concentrating, mood changes, or sleep issues in the days after the injury. These can be signs of concussion or persistent post-concussive symptoms.
Go to the ER or call emergency services immediately if:
- Headache or scalp pain keeps getting worse or is suddenly severe.
- You have vomiting, especially if repeated.
- You feel confused, very drowsy, or have trouble waking up.
- You notice weakness, numbness, slurred speech, balance problems, or trouble walking.
- You see or feel a dent, soft spot, or obvious deformity of the skull.
- There’s clear fluid or blood from the nose or ears, or bruising around the eyes or behind the ears.
- Have you had any loss of consciousness, even for a few seconds?
Also, treat a head injury more aggressively (lower threshold for ER) if:
- You’re over 60.
- You take blood thinners (warfarin, DOACs), daily aspirin, or have a bleeding disorder.
These groups are at higher risk for bleeding inside the skull even after what seemed like a mild blow.
Quick Recap
A tender lump after hitting your head is usually a simple soft-tissue injury. It can hurt, bruise, and feel swollen, but it generally settles on its own as long as the discomfort improves day by day. That kind of bump, by itself, isn’t usually a sign of something serious.
The genuine concern is a concussion, because you don’t need a visible lump to have one. Symptoms such as headache, dizziness, nausea, fogginess, or memory trouble indicate that the brain has been shaken, not just the scalp. Those issues deserve proper medical evaluation rather than waiting them out.
And then there are the true red flags: worsening pain, repeated vomiting, confusion, weakness, seizures, fluid leaking from the nose or ears, trouble waking up, or drastic behavior changes. Those signs call for immediate care. If you’re unsure, go in anyway. It’s always better to get checked and reassured than to risk overlooking an injury that needs urgent attention.
FAQs
Is it normal for a head bump to hurt for several days?
Yes, mild soreness or a small lump can stay tender for a few days to a week as the tissue settles. What’s not normal is pain that worsens, spreads, or is accompanied by dizziness, confusion, or vomiting. If the soreness isn’t clearly improving after a few days, get checked.
How can I tell if my headache after hitting my head is a concussion?
You can’t diagnose it yourself, but patterns help. Headache paired with dizziness, fogginess, memory issues, or sensitivity to light or noise points toward a concussion. The CDC says anyone with these symptoms after a hit to the head should be evaluated by a trained professional.
Can I sleep after hitting my head?
Yes, if you’re alert, talking normally, and have no red-flag symptoms. Ideally, someone should check on you and make sure you can wake normally. If you’re hard to wake, confused on waking, or symptoms worsen, go to the ER.
Should I see a doctor if the pain is only when I touch the spot?
If the bump was mild and you feel normal otherwise, local tenderness alone usually isn’t urgent. See a doctor if the pain worsens, the area feels soft or oddly shaped, the lump doesn’t settle within a week, or you develop any concussion-like signs.
What if there’s a lump but no headache?
A lump without headache is often a simple scalp hematoma. It can be tender but isn’t always serious. Still, watch for dizziness, vomiting, confusion, or behavior changes, and seek care if the lump is large, very painful, or if you’re on blood thinners or older.
References
- Centers for Disease Control and Prevention. (2025). Symptoms of mild TBI and concussion.
- Centers for Disease Control and Prevention. (2025). Signs and symptoms of concussion (HEADS UP).
- Cleveland Clinic. (n.d.). Traumatic brain injury (TBI).
- Mayo Clinic. (2024). Head trauma: First aid.
- Mayo Clinic. (2024). Traumatic brain injury – Symptoms & causes.
- Mayo Clinic. (2024). Concussion – Symptoms & causes.
- Mayo Clinic. (2024). Intracranial hematoma – Symptoms & causes.
- MedlinePlus. (2023). Head injury – First aid.
- MedlinePlus. (2024). Concussion in adults – Discharge instructions.
- National Health Service (NHS). (n.d.). Head injury and concussion: Symptoms and care.
- NHS Northern Ireland. (n.d.). Minor head injury.
- Royal Children’s Hospital Melbourne. (n.d.). Head injury – General advice.
- Johns Hopkins Medicine. (2025). Head injury.
- RadiologyInfo.org. (n.d.). Head injury – Treatment.
In this Article