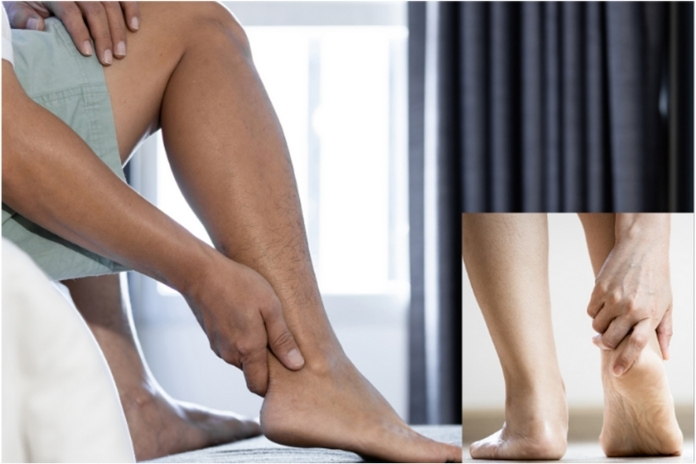
Ever felt that nagging tightness at the back of your heel after walking or climbing stairs? That could be your Achilles tendon – yes, that rope-like thing connecting your calf muscles to your heel – getting quietly tired. When it gets inflamed or irritated, you’re looking at Achilles tendonitis. And here’s the thing: once it flares up, recovery can drag for weeks or months. So it’s way smarter to prevent it in the first place.
Whether you’re running, lifting weights, or even just sitting at a desk all day, and then suddenly walking uphill – the Achilles takes a beating. Let’s look at a fresh way of preventing it: not just stretch more and train less, like everyone says – but stacking the footwear + training + lifestyle deck so your tendon stays strong, happy, and un-irritated.
Here’s what we’ll cover: how the tendon works → risk factors you probably don’t think about → footwear advice you may’ve overlooked → training tweaks you won’t find in generic blogs → everyday habits that quietly protect your Achilles.
Understanding the Achilles Tendon’s Role in Body
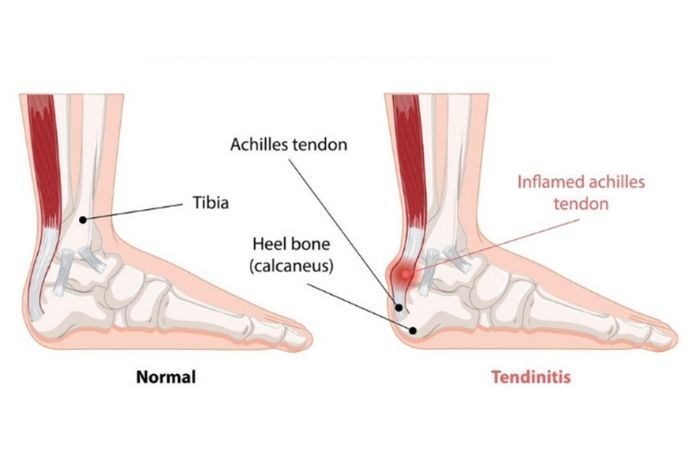
The Achilles tendon is your built-in shock absorber, just like a spring and gearbox all rolled into one. It takes the force from your calf muscles (Gastrocnemius and Soleus), and transmits it to your heel bone so you can push off, jump, run, and walk.
Here’s the catch: every time you push off, jump, accelerate, or decelerate, the tendon stretches, stores energy, then rebounds. Over time, if the load is too high or your system is not ready, that tendon can take more damage than repair. Even sitting all day tightens things up. Tendons are less forgiving with age – they lose elasticity, blood supply gets poorer, and recovery slows.
So it’s not just about “run more” or “stretch more”. It’s about how your entire movement-chain – foot, calf, tendon, heel, shoe – is working.
Common Risk Factors for Achilles Tendonitis
Here are some usual suspects… and some lesser talked-about ones:
- Sudden spike in activity or intensity (e.g., you ran 10 km last week, 20 km this week).
- Worn-out or unsupportive shoes.
- Tight calf or hamstring muscles (makes the tendon take extra pull).
- Foot shape: flat feet or very high arches can both shift the load uncomfortably.
- Over-pronation or poor running mechanics.
- Ageing: tendon elasticity declines, recovery slows.
- Sedentary lifestyle (yes – even desk jobs) because tight calves/popping out of shape = tendon vulnerability.
- Footwear changes (going too quick to minimalist shoes) or lots of uphill/downhill running.
- Nutrition, body weight, and systemic factors (yes – things like poor nourishment or metabolic issues can play a role).
By understanding which of these apply to you, you can tune your prevention strategy instead of generic “just stretch” advice.
Read More: Relief at Your Fingertips: 6 Topical Pain Relief Creams for Joint and Muscle Discomfort
Footwear Tips to Protect Your Achilles Tendon
Yes! You read it right… Footwear can help you protect your Achilles tendon:
1. Choose Supportive Shoes

Your shoes should cushion the heel, support the arch, and slightly reduce strain on the tendon. They are like a friendly buffer. Some things to check:
- Good heel-cushioning (so heel strike isn’t jarring).
- A gentle heel-lift (not so high that you’re tip-toeing all day, but enough to ease the tendon).
- Full-length sole (so the shoe flexes properly, not at the wrong spot).
- Replace shoes every ~300-500 miles (or earlier if heel worn or upper is collapsing) – heel wear increases tendon load.
2. Avoid Minimalist or Unsupportive Footwear Too Soon

Minimalist shoes (zero drop, very thin sole) appear cool and “natural”, but they dramatically increase load on the Achilles if your system is not ready. If you switch to them, do it gradually – yes, exactly like going from couch to 5K. Skip the impulse switch. Think of your tendon adapting over weeks.
3. Use Orthotics If Needed
If your foot mechanics are skewed (flat feet, over-pronation, leg length difference), then off-the-shelf insoles or custom orthotics might help distribute the stress more evenly through your foot-calf-tendon axis. It’s especially helpful when you already have Achilles discomfort. Getting a podiatrist or physiotherapist to assess your gait is smart.
Read More: Can You Prevent Osteoarthritis Progression? 6 Proven Methods for Managing Joint Health
Workout and Training Habits That Prevent Tendon Strain
You can take care of your tendons by following these workout and training habits:
1. Warm Up Before Exercise
Start with 5-10 minutes of light cardio (brisk walk, cycle) just to flush some blood through the calves and the tendons. Then, some dynamic calf/ankle movements (heel raises, ankle circles) so the system is ready.
2. Stretch And Strengthen Key Muscles
Here’s where you move beyond “just stretch”. You want both flexibility and strength.
- Calf stretches: Standing calf stretch (straight leg) & seated calf stretch (bent leg) to hit both gastrocnemius and soleus.
- Eccentric heel-drop exercise: Stand on a step with both heels off the edge; lift up on both legs, then slowly lower on one leg. This kind of loading strengthens the tendon’s ability to take loads. Nonoperative treatment literature supports eccentric loading for tendon health.
- Strengthening: Don’t just rely on body weight. As your calf/tendon adapts, add resistance (weights, bands) so the tendon’s used to being loaded.
- Flexibility for tendon-friendly mechanics: Sometimes it’s your hamstrings or glutes causing compensations that increase Achilles load – so holistic is better.
3. Avoid Overtraining
A big reason Achilles problems show up: the tendon is asked to ramp from 0 to 100 too fast. Follow a rule like “increase intensity or mileage by no more than 10% per week” (yes, the classic 10% rule). Include rest days – your tendon needs recovery. Studies show ignoring minor symptoms and pushing through tends to lead to more serious tendinopathy.
4. Cross-Train for Balance
It’s great to run, but if you run every day on the same surface, same stride, same shoe, your Achilles doesn’t get “variety”. Mix in cycling, swimming, elliptical, or strength training. These support the same muscles/tendons but without the high eccentric load of running every time.
5. Check Your Form
Poor gait, over-pronation, weak glutes, or running downhill a lot can all load your Achilles abnormally. If you’re often walking/running on hills, stairs, or uneven terrain, take note. A gait analysis at a sports clinic can unveil hidden issues.
Read More: Supplement Your Joint Health: Top 5 Glucosamine and Chondroitin Products
Daily Lifestyle Habits for Long-Term Protection
For long-term care and protection of your tendons, follow these lifestyle habits in your daily life:
- Maintain a healthy body weight: Extra kilos = extra load on that tendon every step.
- Stretch calves after long sitting: If you have a desk job, your calf and Achilles tendon shorten over time. Before you stand up, do a 30-second calf stretch just to loosen the chain.
- Warm up before morning walks/runs: After sleep, your muscles and tendons are stiffer – don’t just spring into activity.
- Hydrate and eat nutrient-rich foods: You want good collagen support, healthy tendon tissue. Vitamins (C), minerals (magnesium), protein, and some healthy fats.
- Wear proper shoes even at home: If you’re walking barefoot all day with flat feet or prior Achilles discomfort, you’re still loading that tendon. Flip-flops, very flat shoes, heels with no support – take note.
- Monitor “non-pain” warning signs: If you feel stiffness, mild tightness, it’s your body telling you “slow down a little”. Fixing early is easier than a major flare-up.
Read More: Do Collagen Supplements Really Help With Joint Pain? What Research Says
Early Warning Signs You Shouldn’t Ignore
Don’t wait until full-blown pain. Catching small signs early helps you avoid downtime. Watch for:
- Mild heel/back-of-ankle stiffness in the morning or after sitting for a while.
- Tenderness or ache along the back of the heel or under the calf.
- Creaky or “clicky” feeling when flexing the foot.
- Pain that shows up after a tough workout but not during.
- Swelling or warmth along the Achilles (means inflammation).
If you notice these, reduce load, do extra yield/stretch work, and check your shoes and training.
Read More: Bursitis vs Arthritis: What’s Causing Your Joint Pain? A Clear Comparison Guide
When to Seek Professional Help
Okay, we’re talking prevention – but sometimes things sneak past you. Get help if:
- Pain persists beyond a week despite reducing load and stretching.
- There’s swelling, warmth, or redness around the tendon (could mean degeneration).
- You feel a sharp pop or sudden intense pain (possible partial tear or worse).
- Pain significantly limits push-off, jumping, and walking up stairs.
In those cases, a sports-medicine doc or physiotherapist can check you out, maybe analyse gait, foot mechanics, and give a more targeted plan.
Read More: Ease Arthritis Symptoms: 5 Best Heating Pads for Joint Pain Relief
Key Takeaway
Preventing Achilles tendonitis is not rocket science – but it’s smart science. You’ll win if you:
- Pick the right shoes, avoid sudden minimalist switches.
- Warm up, stretch, and strengthen the game-changer exercises (like eccentric heel drops).
- Train smart (no abrupt increases), cross-train for balance.
- Life-hack your day (stretch after sitting, maintain a healthy weight, keep the tendons mobile).
- Listen to the small signals – not just full pain.
Consistency makes the tendon stronger. Intensity makes the tendon stressed. If you pick one, pick consistency.
Read More: Low-Impact WODs for People with Joint Pain
FAQs
Q1. How can I tell if my shoes are causing Achilles pain?
Check the heel-counter (back of the shoe) – if it’s collapsed or worn, the heel strike becomes unstable and the tendon absorbs more shock. If you feel more back-of-heel ache after changing shoes, that’s a clue. Also, if you switch to very low-drop shoes and your Achilles starts grumbling, that could be it.
Q2. Are heel lifts good or bad for preventing Achilles tendonitis?
They can help if you’re prone to Achilles strain (they slightly reduce tendon stretch). But they’re not a “fix all” – you still need good mechanics and calf strength. Over-using them long-term without strength work can mask underlying weakness.
Q3. Can walking too much cause Achilles inflammation?
Yes – especially if you suddenly increase walking distance or do a lot of uphill/downhill. The tendon doesn’t know the difference between running and walking if the load is high or repetitive. So yes, even walking too much (especially if you’re untrained) can trigger it.
Q4. What’s the best stretch to keep the Achilles healthy?
A straight-leg calf stretch + bent-leg calf stretch (which hits soleus) are good daily staples. But even more important is adding the heel-drop eccentric exercise, which builds tendon resilience rather than just loosening.
Q5. Should I rest completely if I feel mild Achilles discomfort?
Not necessarily “complete rest” – but you should reduce high load (running, jumping), switch to lower-impact (cycling, swimming), do your strength/stretch routine, and monitor. If symptoms don’t ease in a few days, reduce further and get assessed.
In this Article