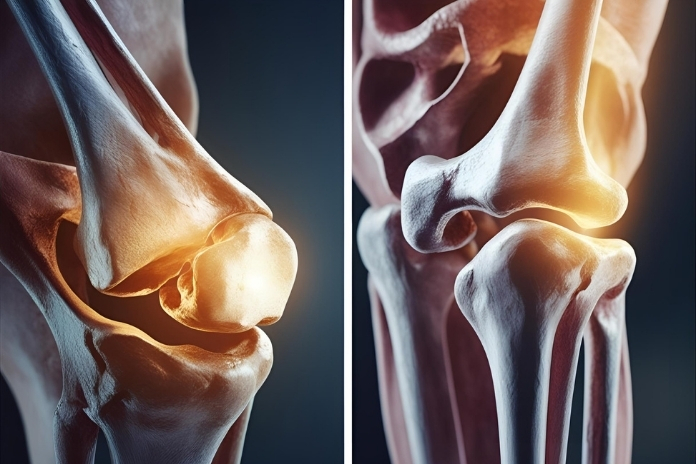
Joint pain affects people of all ages and lifestyles. From the active athlete to the aging individual, it’s not hard to confuse one type of joint pain with another. The two most frequently confused conditions are arthritis and bursitis. Although they have similar symptoms like pain, swelling, and reduced mobility, they have distinct differences in cause, treatment, and long-term effects.
This in-depth article differentiates bursitis vs arthritis to help you understand the symptoms, underlying causes, diagnostic methods, and treatments so you can live with confidence.
Read More: 5-Minute Daily Mobility Routine for Arthritis You Can Do at Home
What Is Bursitis?

Bursitis is inflammation of the bursae, small fluid-filled sacs that serve as cushions between tendons, muscles, skin, and bones. If a bursa becomes inflamed, it can swell and cause pain, particularly with movement or pressure.
Affected Areas:
- Shoulders (subacromial bursitis)
- Hips (trochanteric bursitis)
- Elbows (olecranon bursitis)
- Knees (prepatellar or infrapatellar bursitis)
- Heels or the bottom of the big toe
Causes of Bursitis:
- Repetitive stress or overuse
- Direct trauma
- Infection (septic bursitis)
- Gout or rheumatoid arthritis
- Poor posture or biomechanical imbalance
Symptoms of Bursitis:
- Stabbing, localized pain close to a joint
- Swelling, tenderness, redness
- Heat at the location
- Pain increased by pressure or motion
- Typically improves with rest
What Is Arthritis?

Arthritis is an inflammatory joint disease that produces chronic symptoms such as wearing away cartilage and other joint tissues over time. In contrast to bursitis, which involves cushioning sacs on the outside of the joint, arthritis is caused in the inside space of the joint.
Common Types:
- Osteoarthritis (OA): Degenerative joint disease resulting from wear and tear
- Rheumatoid Arthritis (RA): An Autoimmune disorder in which the immune system attacks the joint linings
- Psoriatic Arthritis, Gout, Lupus-related Arthritis
Causes of Arthritis:
- Aging and deterioration of cartilage
- Autoimmune dysfunction (RA)
- Joint injuries
- Genetic predisposition
- Infections or metabolic disorders (e.g., gout)
Symptoms of Arthritis:
- Dull, aching, deep pain
- Stiffness in the morning that lasts longer than 30 minutes
- Swelling, redness, and heat
- Reduced flexibility of joints
- Joint deformities in advanced stages
- Fatigue and systemic symptoms (especially in RA)
Read More: Isometric Exercises for Arthritis: Safe Ways to Build Strength Without Movement
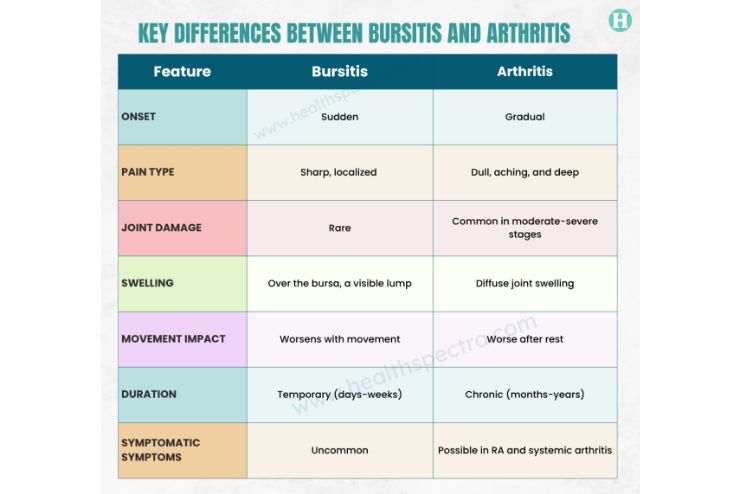 Shared Symptoms That Can Confuse You
Shared Symptoms That Can Confuse You
Bursitis and arthritis can be caused by dissimilar mechanisms, but they have several overlapping signs; hence, they are often misdiagnosed or mistaken:
- Pain Near Joints Due to Movement: Both develop pain, especially on movement or while bearing weight.
- Redness or Swelling: Visible signs of inflammation may appear on either side
- Decreased Range of Motion: Stiffness and difficulty in mobility are characteristic signs
What Makes Them Difficult to Distinguish?
The reason for the confusion is the site and nature of the pain. In bursitis, the pain is stabbing and localized, mostly to a specific area. Arthritis produces a more dispersed, deep-seated pain, which is often accompanied by grinding or joint instability over time.
Also, the two can happen together or even cause each other. An example is how arthritis inflammation might inflame an adjacent bursa, which in turn induces bursitis as a secondary condition. Also, long-term bursitis can change the mechanics of a joint and cause more cartilage wear, ultimately causing arthritis.
Diagnosing the Cause of Your Joint Pain
Accurate diagnosis is essential in determining the proper treatment approach. Here is how physicians rule between arthritis vs bursitis:
Medical History:
- Onset: Sudden implies bursitis; gradual implies arthritis
- Activity-Related Symptoms: Overuse indicates bursitis; chronic decline implies arthritis
- Family History: Especially relevant in autoimmune arthritis
- Fever or Fatigue: Perhaps suggestive of RA or septic bursitis
Physical Exam:
- Palpation: Tenderness over a bursa favors bursitis; increased joint tenderness favors arthritis
- Range of Motion Tests: Active pain with targeted motion typically indicates bursitis; passive and active restriction indicates arthritis.
- Swelling Evaluation: Localized mass vs diffuse joint swelling
Imaging:
- X-rays: Show joint space reduction, bone spurs, or erosions in arthritis
- Ultrasound or MRI: Identify fluid collection or bursal inflammation
Lab Tests:
- Blood tests: Rheumatoid factor (RF), Anti-CCP, CRP, and ESR for autoimmune markers
- Joint or bursal fluid aspiration: Determines infection (septic bursitis), crystals (gout), or inflammatory markers
Diagnostic Tip:
If the swelling develops rapidly, bursitis is more likely the reason. If the whole joint is stiff, swollen, and becomes worse over months, arthritis is the suspect.
Treatment Options for Bursitis vs Arthritis
Although symptoms may overlap, treatment approaches to bursitis and arthritis vary based on etiology and chronicity.
Bursitis Treatment:
- Reduce inflammation and avoid further irritation with ample rest. Applying ice to the swollen joint can also relieve pain.
- Opt for NSAIDs to relieve pain and inflammation.
- Compression and mild pressure reduce localized swelling.
- Prevent movements that worsen the condition and strain the bursa.
Medical Treatments:
Here are a few ways your doctor might help you get rid of pain. He might prescribe:
- Corticosteroid injection provides prompt relief for chronic pain.
- Physical therapy and gentle stretching, and strengthening exercises that prevent recurrence.
- Antibiotic treatment, if the area is infected (septic bursitis).
- Aspiration, a process that involves the withdrawal of excess fluid for relief and diagnosis.
- Surgery though not often required unless bursitis is chronic or frequently recurrent.
Treatment of Arthritis:
Here’s what your doctor might prescribe if you suffer from arthritis:
- Low-impact exercises such as swimming or cycling maintain joint mobility.
- Weight management to reduce joint burden and disease progression of osteoarthritis.
- NSAIDs and Analgesics to treat flare-ups and chronic pain.
- Disease-Modifying Agents (particularly for Rheumatoid Arthritis):
- DMARDs: Methotrexate, sulfasalazine slow down disease progression.
- Biologic Agents: Target specific immune mechanisms.
- Steroid Injections: Short-term, decrease inflammation during flare.
Lifestyle and Supportive Care:
Medical interventions are necessary, but so are lifestyle changes. These small habits help you deal with both conditions better and also help in pain relief. These include:
- Physical Therapy: Maintains mobility and muscle strengthening.
- Supplements: Glucosamine, chondroitin, and omega-3 may have beneficial effects on joints (but results are mixed)
- Assistive Devices: Bracing or orthotics may be helpful for stability
- Joint Replacement: Considered in late stages when damage is extreme
The key difference? Bursitis may be treated by brief intervention. Arthritis, on the other hand, needs lifelong control and often vigorous immunosuppression.
Read More: 9 Essential Supplements for Joint Health and Arthritis Relief
When to See a Doctor

You should visit a doctor if:
- Pain or swelling lasts more than a few days.
- Redness, heat, or infection signs are experienced.
- Your joint will not move or become extremely stiff.
- Pain disrupts sleep or daily function.
- You observe systemic signs such as fever or tiredness.
Timely attention avoids minor inflammations from becoming chronic conditions or joint destruction.
Prevention Tips for Both Conditions
- Warm up before exercise. This prepares joints for use.
- Avoid repetitive stress. Plan tasks and take enough rest.
- Maintain good posture. Avoid unnecessary strain on joints and bursae.
- Strengthen supportive muscles, which help joint alignment and cushioning.
- Use joint protection devices, which include pads, braces, and ergonomic devices reduce risk.
- Keep a healthy weight as this reduces joint stress, particularly on the hips and knees.
- Stay hydrated and consume anti-inflammatory foods that include Omega-3s, green leafy vegetables, and berries to help maintain healthy joints.
Conclusion
Being aware of whether your joint pain is the result of bursitis vs arthritis is essential to getting the appropriate treatment and preventing long-term issues. While bursitis is usually acute due to overuse or trauma and will likely heal rapidly with resting and anti-inflammatory treatment, arthritis is a long-term condition that demands constant care.
Both conditions may affect your mobility and comfort, but focused diagnosis and treatment can regain function and enhance quality of life. If your joint pain is new, persistent, or increasing, don’t disregard it—get a professional assessment and work hard towards having a healthy joint.
References
- https://timesofindia.indiatimes.com/life-style/health-fitness/health-news/arthritis-vs-bursitis-what-you-need-to-know-to-understand-the-differences/articleshow/118092964.cms
- https://www.ncbi.nlm.nih.gov/books/NBK518992/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6221932/
- https://www.topdoctors.co.uk/medical-dictionary/bursitis/
In this Article