When we think about climate change, melting glaciers and rising seas usually come first to mind. But here’s the thing, its impact isn’t just distant or environmental. Your own heart may already be under threat, quietly, every single day. The climate crisis doesn’t wait for the future; it’s unfolding now, and the human body, especially the cardiovascular system, is on the frontlines.
Extreme heat forces your heart to work harder just to keep you cool, raising the risk of dehydration, blood thickening, and even heart attacks. Wildfire smoke and air pollution clog the very air you breathe, inflaming blood vessels and straining circulation. Floods, storms, and other climate-driven disasters don’t just damage homes and infrastructure; they trigger stress responses that can destabilize blood pressure and worsen existing heart disease.
This isn’t abstract science; it’s a daily reality. Whether you live in a city smothered by smog or a region hit by record heatwaves, climate change is reshaping the conditions in which your heart beats. In this article, we’ll explore exactly how climate change affects cardiovascular health, and more importantly, what practical steps you can take to protect yourself in an increasingly unstable world.
Quick Take: Climate Change & Heart Health
Climate change isn’t only about rising seas or melting ice. It’s also reshaping the conditions your heart works in every day. Here are the key ways it affects cardiovascular health, and what you can do about it.
- Heatwaves: Increase risk of heart attacks, strokes, and heart failure.
- Air Pollution: Linked to cardiovascular disease, arrhythmias, and premature death.
- Wildfire Smoke: Worsens inflammation, raises blood pressure, and carries both immediate and lingering cardiovascular risks.
- Climate-Related Stress: Climate anxiety and disaster-related stress raise cortisol and other stress hormones; chronic stress damages the cardiovascular system.
- Prevention: Stay cool during heatwaves, track local air quality, limit smoke exposure, manage stress, and prioritize access to care, especially for vulnerable groups.
How Heat Affects the Heart
Heat isn’t just uncomfortable; it changes how your body works, and your cardiovascular system takes the brunt of it. When temperatures climb, your heart must work harder, your blood thickens, and existing conditions can tip into crisis.
What Happens in Your Body
- Increased heart rate and blood pressure. To cool itself, the body widens blood vessels (vasodilation) and pushes more blood toward the skin surface. That forces the heart to beat faster, often under stressful conditions, which can raise blood pressure and strain circulation.
- Dehydration and thicker blood. Sweating and fluid loss shrink plasma volume, leaving blood more concentrated and viscous. This makes it harder for the heart to pump and increases the risk of clot formation, which can trigger strokes or heart attacks.
- Extra strain on the existing disease. For people with coronary artery disease, heart failure, or arrhythmias, heat can quickly tip the balance. Oxygen demand rises while supply falls, which can trigger angina, arrhythmias, or even cardiac arrest. Breathing often becomes more difficult, worsening stress on the system.
“While climate change is a macro issue, cardiovascular specialists have long tackled public health challenges, just as we did with smoking. Ultimately, this is about changing behaviors to protect heart health, which is central to our mission,” says cardiologist Harlan Krumholz, MD.
Who Is Most Vulnerable
- Older adults (65+) face sharply increased risks. Studies show cardiovascular mortality rises with even small temperature jumps.
- People in tropical climates or those without reliable cooling options (like fans, air conditioning, or shaded housing) are more exposed.
- Outdoor workers and manual laborers experience sustained strain, especially during prolonged heat events.
- Anyone with pre-existing heart conditions is at a higher risk, as heat exacerbates their vulnerabilities.
New Findings in Heat Research
- Compound heatwaves, days that are scorching with nights that never cool, are far more dangerous than daytime-only or nighttime-only heat events. Without recovery time at night, the heart remains under pressure continuously.
- Cumulative effects, the later days of a heatwave tend to be deadlier than the first, because stress builds day after day. By the fourth or fifth day, the risk of heart-related events rises sharply.
- Urban heat islands add another layer. Cities with little green space trap heat, making recovery harder for residents and amplifying cardiovascular strain.
Heat is more than a discomfort; it’s a direct cardiovascular stressor. For vulnerable groups, even modest temperature increases can mean the difference between stability and crisis. Recognizing the signs of heat stress, staying hydrated, and ensuring cooling access aren’t just comfort measures; they’re heart protection strategies.
Air Pollution & Cardiovascular Disease

Air pollution is one of the most damaging byproducts of climate change. Wildfires, dust storms, and rising ground-level ozone all intensify pollution levels, creating invisible but potent threats to cardiovascular health. For millions worldwide, simply breathing in polluted air can set off a cascade of harmful effects inside the body.
Mechanisms: How Pollution Harms the Heart
- Fine particles: These microscopic particles slip deep into the lungs and can even pass into the bloodstream. Once inside, they trigger systemic inflammation, oxidative stress, and direct injury to the vascular endothelium (the delicate inner lining of blood vessels). This accelerates atherosclerosis and makes blood vessels more prone to narrowing and clotting.
- Ozone and gaseous pollutants: Elevated ozone levels and other reactive pollutants increase the workload on the cardiovascular system. They raise blood pressure, worsen endothelial dysfunction, and can destabilize the electrical activity of the heart, increasing the likelihood of arrhythmias.
Evidence and Scale
- Global burden: The World Health Organization estimates that air pollution contributes to millions of deaths annually, with cardiovascular disease accounting for a significant portion. Heart attacks, strokes, and heart failure events all rise when pollution levels climb.
- Heat plus pollution: a dangerous mix: A 2023 study of more than 202,000 fatal heart attacks in China revealed a striking pattern: on days with both extreme heat and high PM₂.₅, the risk of dying from a heart attack surged, sometimes doubling compared to normal days. This underscores how climate change magnifies pollution’s impact by stacking multiple stressors on the body.
- Urban exposure: Cities concentrate pollution due to traffic, industrial emissions, and fewer green buffers. Urban populations are thus at higher risk, especially those with pre-existing heart conditions or limited healthcare access.
Prof. Haidong Kan, from Fudan University in Shanghai, led a large study showing that brief exposure to pollutants (fine particulate matter, nitrogen dioxide, etc.) could sharply increase the risk of acute coronary syndrome, especially in older adults. “The adverse cardiovascular effects of air pollution have been well documented. But we were still surprised at the very prompt effects.”
Air pollution doesn’t just irritate the lungs; it silently sabotages the cardiovascular system. By damaging blood vessels, thickening the blood, and stressing the heart, polluted air increases both the likelihood and severity of cardiovascular events. As climate change drives more wildfires, smog episodes, and ozone spikes, protecting your heart increasingly means protecting the air you breathe.
Extreme Weather Events & Heart Health
Climate change not only raises temperatures, it amplifies the frequency and severity of extreme weather events, each with its own ways of straining the cardiovascular system. From wildfire smoke to hurricanes and sudden cold snaps, these events compound existing health risks and make life more dangerous for people with heart conditions.
Wildfire Smoke: A Hidden Cardiovascular Hazard
Wildfires now burn longer and hotter than before, and their smoke is far from harmless haze. The air becomes packed with fine particles, carbon-based compounds, heavy metals, and volatile organic chemicals. These pollutants don’t just irritate the lungs; they cross into the bloodstream, fueling inflammation and oxidative stress that directly harm the heart and blood vessels.
The consequences are measurable. On days following major wildfire smoke exposure, hospitals see spikes in heart attacks, irregular heart rhythms, strokes, and cases of ischemic heart disease. Recent long-term data suggest that repeated smoke exposure compounds the damage: older adults and women, in particular, face a heightened risk of developing heart failure after seasons of recurring wildfire smoke.
Other Climate-Driven Events: Heat’s Not the Only Threat
Wildfires aren’t the only extreme events taking a toll. Hurricanes and floods can cut people off from medical care, destroy pharmacies, and disrupt access to critical medications, such as blood pressure medications or blood thinners. For patients with existing heart conditions, even a short lapse in treatment can quickly become life-threatening.
Cold extremes also carry hidden dangers. When temperatures plunge, blood vessels constrict, blood pressure rises, and the blood itself becomes thicker, all of which sharply raise the risk of heart attack and stroke. Studies across diverse regions, from Iran to Brazil, consistently show an increase in cardiovascular hospitalizations during cold spells.
The Overlapping Burden
What makes these events especially concerning is that they rarely occur in isolation. A wildfire may be followed by a heatwave, or a hurricane by a cold snap. Each adds strain to an already taxed cardiovascular system, creating a cycle where recovery never fully catches up with the next hit. For those living with heart disease or even early risk factors, this cycle can push the body past its limits.
The Stress Factor: Climate Anxiety & the Heart

When we talk about climate change, the conversation often centers on physical dangers like heat or pollution. But there’s another, quieter threat at play: the psychological strain of living in a world increasingly shaped by climate disasters. That stress doesn’t just stay in the mind; it seeps into the body, and the heart is one of the first organs to feel the impact.
Chronic Stress and Cortisol Overload
Long-term stress keeps the body locked in a “fight or flight” mode. Cortisol, the body’s main stress hormone, stays elevated for far longer than it should. Over time, this hormonal imbalance increases blood sugar, pushes blood pressure higher, and raises cholesterol and triglyceride levels. Each of these changes chips away at cardiovascular health, creating fertile ground for heart disease.
Anxiety, Depression, and PTSD
The emotional weight of climate change, whether it’s witnessing wildfires, fearing floods, or losing homes and jobs, can spark anxiety, depression, and even post-traumatic stress disorder. These conditions are increasingly being tied to higher rates of arrhythmias, strokes, and coronary artery disease. In other words, mental health struggles linked to climate change are not just about mood; they actively translate into measurable heart risks.
The Behavioral Ripple Effect
Stress rarely exists in isolation; it shapes how people live their day-to-day lives. Under pressure, many turn to coping mechanisms that inadvertently make things worse for the heart: poor sleep, unhealthy eating, smoking, alcohol, or skipping exercise. Over months and years, these habits amplify the physiological damage caused by stress itself, creating a cycle that accelerates cardiovascular decline.
Why This Matters
Taken together, the psychological and behavioral effects of climate change form an invisible but powerful driver of heart disease. Even for people who never face a wildfire or flood directly, the chronic anxiety about climate threats can slowly wear down both mental resilience and physical health. Protecting the heart, then, isn’t just about cleaner air and cooler temperatures; it’s also about addressing the stress that comes with a changing planet.
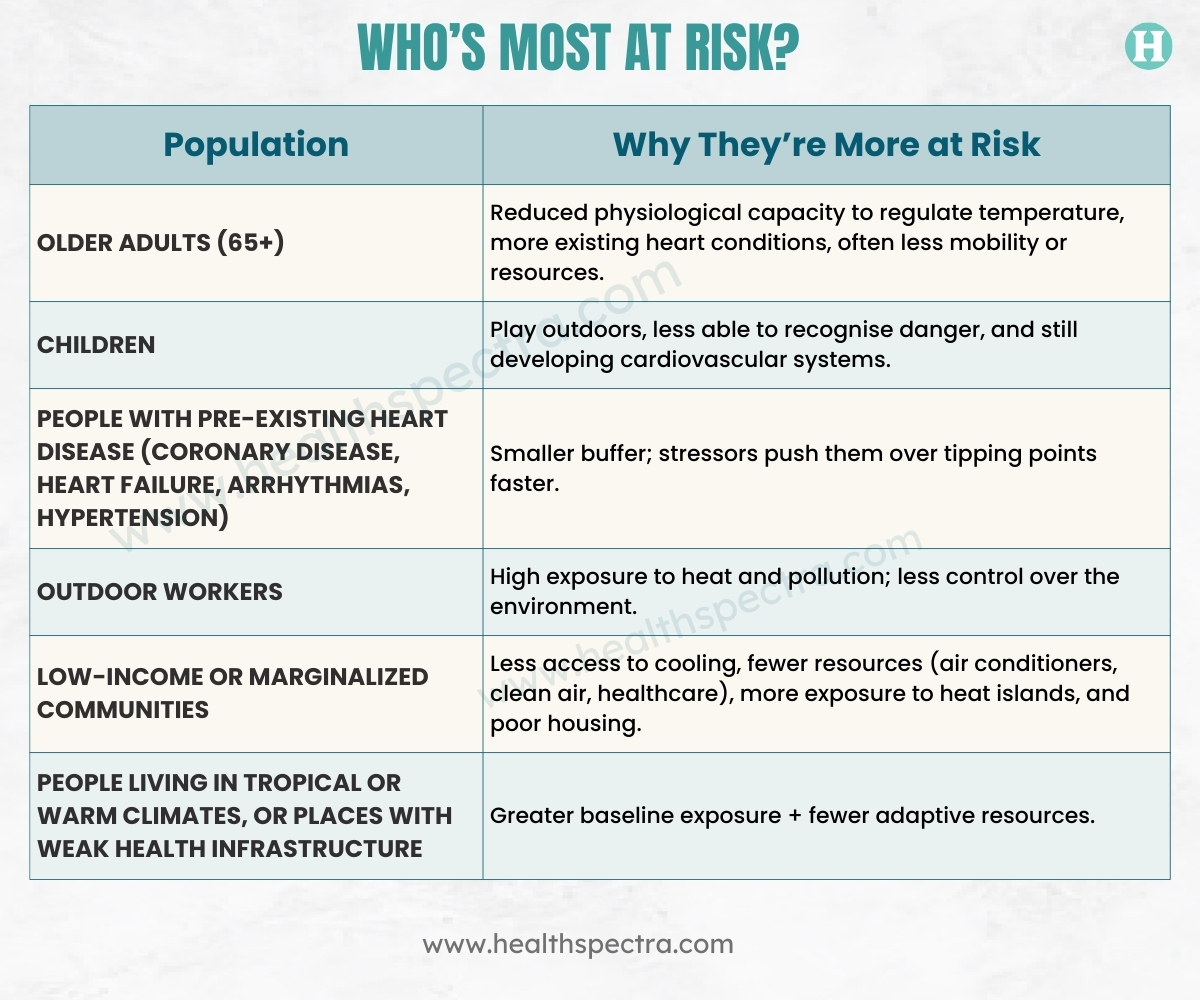
Who’s Most at Risk?
Some groups are much more vulnerable than others. Knowing who you are at higher risk can help you take preventative action early.
 How to Protect Your Heart in a Changing Climate
How to Protect Your Heart in a Changing Climate

You can’t control global temperatures or pollution on your own, but you can reduce personal risks. These strategies fall into five buckets: heat, air, emergencies, stress, and long-term care.
1. Beat the Heat
- Avoid outdoor exertion during peak hours (midday to early afternoon).
- Stay hydrated; replace electrolytes if sweating heavily.
- Cool down with fans, AC, or cool showers.
- Use public cooling centers if available.
2. Monitor Air Quality
- Track local Air Quality Index (AQI) via apps or alerts.
- Minimize outdoor exposure on high-pollution or smoke-heavy days; wear N95/FFP2 masks if outside.
- Indoors: close windows during bad air days, run HEPA filters, and avoid indoor smoke or biomass burning.
3. Prepare for Extreme Weather
- Have an emergency plan for access to medicines, healthcare, and power during outages.
- Stock and store heart medications properly.
- In cold events: layer clothing, insulate homes, and avoid abrupt temperature shifts.
4. Manage Stress and Mental Health
- Practice mindfulness, meditation, or breathing exercises daily.
- Limit doomscrolling if constant news fuels anxiety.
- Stay socially connected; strong networks buffer stress.
- Seek professional support if anxiety, depression, or PTSD symptoms persist.
5. Lifestyle & Medical Care
- Maintain heart-healthy habits: balanced diet, regular exercise, adequate sleep.
- Get regular check-ups for blood pressure, cholesterol, and blood sugar.
- Learn the early warning signs of a heart attack and stroke.
6. Advocate for Change
- Support policies that cut emissions and improve air quality.
- Push for urban designs that add trees, shade, and cooling spaces.
- Ensure vulnerable groups, including older adults, outdoor workers, and low-income communities, have access to resources such as cooling centers, clean air, and healthcare.
FAQs: Climate Change and Heart Health
Q: Can heatwaves really trigger heart attacks?
Yes. Heatwaves, especially when combined with high humidity or high nighttime temperatures, significantly increase the risk of acute cardiovascular events, including heart attacks. Research shows that even a 1 °C rise in temperature is associated with higher cardiovascular mortality. The danger is even greater when extreme heat overlaps with poor air quality, such as high levels of fine particulate matter.
Q: Is air pollution worse for the heart or lungs?
Both are severely affected. While air pollution is widely known to damage the lungs, its harmful particles and gases also enter the bloodstream. This triggers systemic inflammation, damages blood vessels, stresses the heart muscle, and disrupts normal heart rhythms. Cardiovascular deaths linked to PM₂.₅ are substantial worldwide, making air pollution one of the leading modifiable risk factors for heart disease.
Q: How does wildfire smoke affect cardiovascular health?
Wildfire smoke is rich in fine particles and toxic compounds. Short-term exposure is linked to spikes in emergency visits for heart attacks, irregular heart rhythms, and ischemic heart disease. Long-term or repeated exposure raises the risk of heart failure, particularly in older adults and vulnerable populations. What’s more, the cardiovascular effects of smoke, including inflammation and vascular damage, can linger for months after the initial exposure.
Conclusion
Climate change is not just reshaping landscapes and coastlines; it’s reshaping the way our hearts beat, struggle, and sometimes fail under pressure. Heatwaves, polluted skies, choking wildfire smoke, and relentless stress all converge on the same vulnerable system: the cardiovascular system. Science is no longer a warning; it’s evidence that climate change is already a public health crisis beating inside our chests.
But this story doesn’t end with despair. Protecting your heart in a changing climate is possible through personal choices, community preparedness, and demanding stronger policies. Staying cool, monitoring air quality, caring for mental health, and maintaining healthy routines are frontline defenses. At the same time, collective action to cut emissions, clean the air, and build climate-resilient health systems can reduce risks for millions.
Your heart is resilient, but it isn’t invincible. The choices you make today, both personally and as a society, decide whether climate change remains a distant worry or becomes a daily threat to your most vital organ. Protect your heart, and in doing so, protect the future.
References
- https://www.health.harvard.edu/blog/heat-is-hard-on-the-heart-simple-precautions-can-ease-the-strain-201107223180
- https://www.who.int/news-room/fact-sheets/detail/climate-change-heat-and-health
- https://ctvstexas.com/how-heat-affects-your-heart/
- https://www.felixhospital.com/blogs/summer-heart-care-tips-how-heat-impacts-your-heart-and-what-to-do
- https://continentalhospitals.com/blog/how-summer-heat-affects-your-heart-and-how-to-stay-safe/
- https://pubmed.ncbi.nlm.nih.gov/37396980/
- https://www.epa.gov/air-research/air-pollution-and-cardiovascular-disease-basics
- https://www.sciencedirect.com/science/article/pii/S0735109718383554
- https://www.escardio.org/Journals/E-Journal-of-Cardiology-Practice/Volume-22/air-pollution-a-new-risk-factor-for-cardiovascular-disease
- https://world-heart-federation.org/news/new-report-highlights-worsening-levels-of-cardiovascular-illness-and-deaths-from-air-pollution/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8941724/
- https://hms.harvard.edu/news/climate-change-fueled-weather-events-linked-worsened-heart-health
- https://pmc.ncbi.nlm.nih.gov/articles/PMC10548486/
- http://www.ifm.org/articles/extreme-weather-heart-health
In this Article
























