We often overlook dental problems or ulcers, thinking they are just another small issue. However, these are not just simple oral problems but can mean something more. I have heard my family saying that the mouth is the mirror to your health. Is that true? Let’s read on to know more.
Most people see oral health as separate from the rest of the body. But, in reality, the mouth tends to indicate other conditions in an early stage. Small changes in the gums, tongue, teeth, or breath can be the initial signs of conditions like diabetes, heart disease, autoimmune disease, bone loss, and even cancer.
Dentists are likely to be the first medical practitioners to identify these warning signs, which can translate to precious referrals for treatment.
The relationship between oral and overall health is increasingly supported by science. Infection, inflammation, and blood flow in the mouth can influence and be impacted by the rest of the body. Most of these oral signs, if caught early, can result in early detection and improved control of serious health diseases.
These are eight oral symptoms that should never be overlooked, what they can indicate, and when to see a specialist.
Read More: Effortless Oral Care: The Top 7 Water Dental Flossers for Superior Dental Hygiene
1. Chronic Bad Breath (Halitosis)

Sometimes, having bad breath after eating foods that smell strong is normal. But if bad breath happens all the time, even when you take care of your teeth, it might mean there is a health problem. This is despite brushing and flossing regularly.
One of the common causes is uncontrolled diabetes. Diabetic ketoacidosis in severe conditions leads to the release of lots of ketones by the body, which leads to a fruity or acetone smell to the breath.
The other cause is gastroesophageal reflux disease (GERD), as the food particles and stomach acids can lead to a bad smell. Chronic liver or kidney disease is also one of the causes of bad breath as a result of the build-up of certain chemicals in the blood.
When to visit a dentist versus a doctor:
If halitosis continues, even after getting treatment for plaque, gum infection, or cavities, it’s time to seek a medical cause. Dentists can assist in identifying causes of bad mouth odor, and physicians can do tests to screen for medical conditions such as diabetes, disorders of digestion, or organ disorders.
2. Bleeding or Swollen Gums
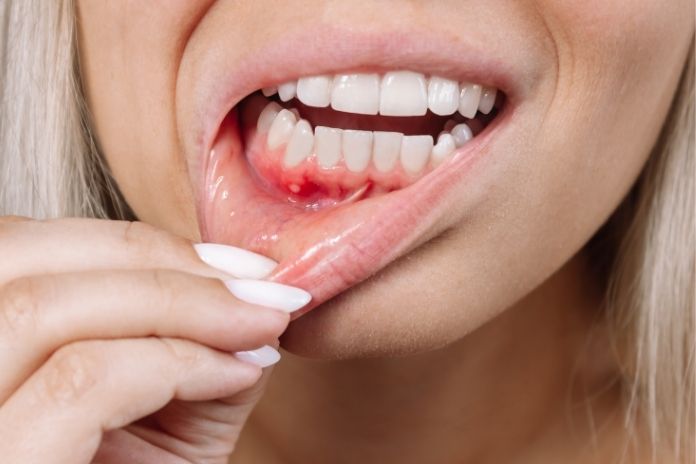
Healthy gums are firm, pale pink, and do not bleed when you floss or brush. Bleeding or swelling are typically indications that you have gingivitis or the more serious periodontitis. The bacteria in plaque are the cause of these diseases, and they are also indications that there is inflammation that may be occurring elsewhere in the body.
Various studies have shown a direct link between heart disease and gum disease. Gum inflammation would also act as a vasoconstrictor, decreasing blood flow in the arteries. This makes a person susceptible to a heart attack and stroke. Individuals with diabetes are also prone to gum disease, as high blood sugar would make it more difficult for the body to combat infection.
The two-way relationship:
Periodontal disease can impact gum health, but gum inflammation can be resolved to improve total health. For example, type 2 diabetic patients have better blood sugar levels after gum treatment. This shows that gum health plays an important role in the control of chronic health conditions.
3. Dry Mouth (Xerostomia)

Saliva is a very crucial aspect of maintaining a healthy mouth. It aids in balancing acids, dislodges food particles, and protects against infection. When the body produces less saliva, the mouth is more likely to have tooth decay, gum disease, and fungal infection, such as oral thrush.
Uncontrolled diabetes that results in high blood sugar levels can lead to dry mouth by draining fluid from tissues. Autoimmune disorders like Sjögren’s syndrome damage salivary glands directly, and it becomes increasingly hard for them to produce saliva. Radiotherapy for head and neck cancers, some antihistamines, antidepressants, and high blood pressure medication are some of the causes of dry mouth.
Why it matters:
Dry mouth is more than just an issue of discomfort; it can speed up tooth decay and make eating, speaking, and swallowing difficult. All individuals with ongoing dryness require both dental assessment and a medical diagnostic workup to determine the cause.
Read More: Tongue Scraping: An Ayurvedic Practice for Detox & Oral Health
4. White spots or Ulcers
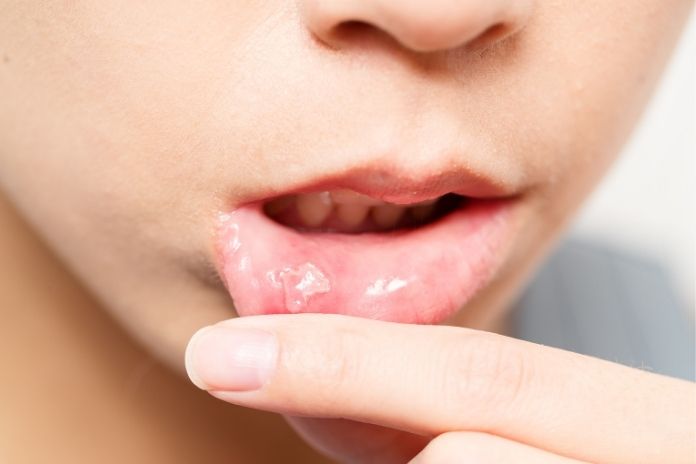
White spots in the mouth, particularly on the cheeks, tongue, or gums, could be leukoplakia. Leukoplakia occasionally is caused by chronic irritation from smoking or poorly fitting dentures. While leukoplakia is not generally dangerous, some spots can develop into oral cancer.
More persistent sores that fail to heal within two weeks are also a cause for concern. Oral cancers typically start as small, painless sores or red and white patches. A weak immune system, for instance, caused by HIV, can cause delayed healing and predispose to such sores.
Early detection is lifesaving. Early oral cancer has a survival rate of approximately 80 to 90 percent. Regular visits to a dentist and early check-ups for any lingering sores are very important for early treatment.
5. Recurring Mouth Sores
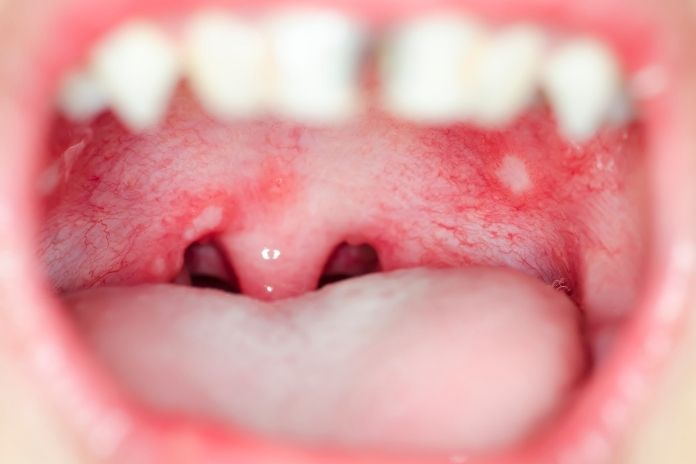
Mouth ulcers, also known as canker sores, are common and usually caused by stress, minor trauma, or acidic foods. But if you have many or large ulcers, it may mean there is something else going on. Recurrent ulcers can be caused by low levels of vitamin B12, folate, and iron.
Autoimmune disorders such as celiac disease or inflammatory bowel disease may present in the mouth. In such cases, ulcers may be observed along with gastrointestinal symptoms such as bloating, diarrhea, or stomach pain.
When to probe further:
If the ulcers occur more than three or four times per year, for longer than two weeks, or with other symptoms, you should have a full check-up with a doctor. Blood work will be able to detect any deficiency, and a gastrointestinal examination might be needed to check for long-term problems.
6. Loose Teeth Without Obvious Cause
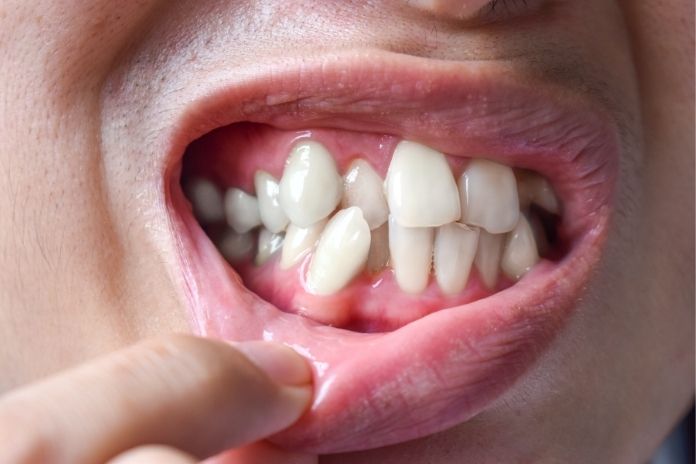
Tooth loss in an adult is always pathological. Although trauma can be a cause of acute tooth loss, gradual loosening of teeth tends to indicate serious periodontal disease. In periodontitis, infection and inflammation cause loss of tissue and bone that hold teeth in place.
Loose teeth are among the symptoms of osteoporosis, a condition that weakens bones in the whole body, even the jaw. This connection is especially crucial in women after menopause, as they are likely to develop osteoporosis and lose teeth.
Why bone health is crucial in oral/dental care:
The dentist may be able to identify loss of bone density on dental X-rays before other signs and symptoms arise. If teeth shift without cause, referral for bone density testing can identify osteoporosis.
Read More: Is Jaw Pain a Sign of a Heart Attack? Left Side vs. Right Side Explained
7. Sore or Swollen Tongue (Glossitis)
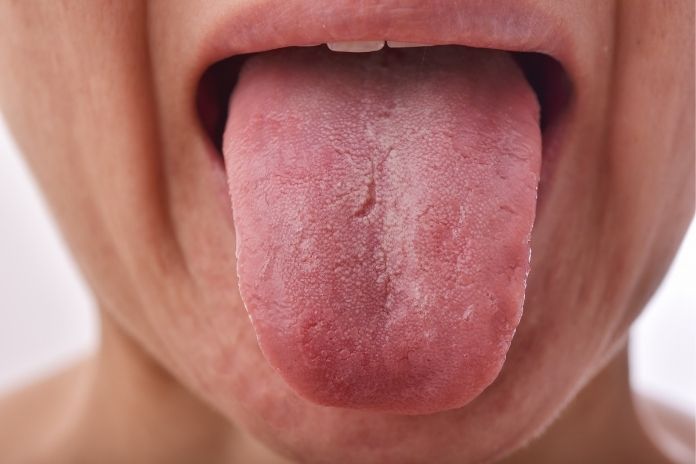
Your tongue has much to tell about your health. In glossitis, the tongue becomes swollen and smooth, and painful. Iron deficiency anemia is a frequent problem, as are vitamin B12 and folic acid deficiencies. Allergic responses, infections, and celiac disease may also lead to inflammation of the tongue.
In autoimmune disorders such as lupus, the tongue may develop painful ulcers. In some cases, swelling of the tongue is a result of severe issues such as bad allergic reactions, which require immediate medical attention.
Pay attention to small changes. Tongue color, texture, or sensitivity changes must be assessed, particularly if they are persistent. Blood tests will reveal nutritional etiologies, and additional work-up may reveal immune or gastrointestinal disease.
8. Jaw Pain or Tightness

Jaw pain usually arises from problems with the temporomandibular joint (TMJ), gum disease, or tooth infection. Jaw pain may, however, be a sign that the heart is not healthy. When there is a heart attack, pain may be referred to the jaw, neck, or shoulders, and may even occur without chest pain. This is also the case, particularly with women. They will experience less typical heart attack symptoms such as jaw pain, shortness of breath, fatigue, and nausea.
When to go to urgent care:
Jaw pain with other unusual symptoms, particularly in individuals with risk factors for heart disease, must be considered a medical emergency until it is proven otherwise. Even if the issue is a dental one, it is the safest course to first look for heart problems.
Conclusion
The mouth is an important part of the body. It is a reflection of your health and impacts the general health of the body. Dry mouth, white patches, painful gums, chronic halitosis, frequent sores, changes in the tongue, loose teeth, and jaw pain are not just oral issues; they may be symptoms of more significant health problems.
Dental check-ups are not for looks, but for overall health. According to Dr. Kemia Zeinali, founder of Dreamhouse Dental in Bell Gardens, Calif, visiting a dentist regularly is essential. “Regular dental visits are critical for early detection of oral health issues before they escalate or spread to other parts of the body,” She adds, “For example, untreated cavities, tooth decay, and gum disease can lead to serious health problems like heart disease and diabetes.”
Dentists and doctors can work together to catch diseases before they become harmful, which improves health and even saves lives. If you notice any of these symptoms, do not let them get worse. Visit a dentist for examination of your mouth and a doctor for a complete medical examination. By paying attention to what your mouth is saying, you may be able to discover serious diseases before they turn fatal.
References
- https://www.whitecosmeticdentist.com/blog/jaw-pain-on-one-side-heart-attack/
- https://www.carehospitals.com/symptoms/swollen-tongue
- https://mcilwaindentistry.com/2024/02/21/osteoporosis-and-oral-health-what-you-need-to-know/
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/inflammatory-bowel-disease
- https://www.health.harvard.edu/diseases-and-conditions/gum-disease-and-the-connection-to-heart-disease
In this Article