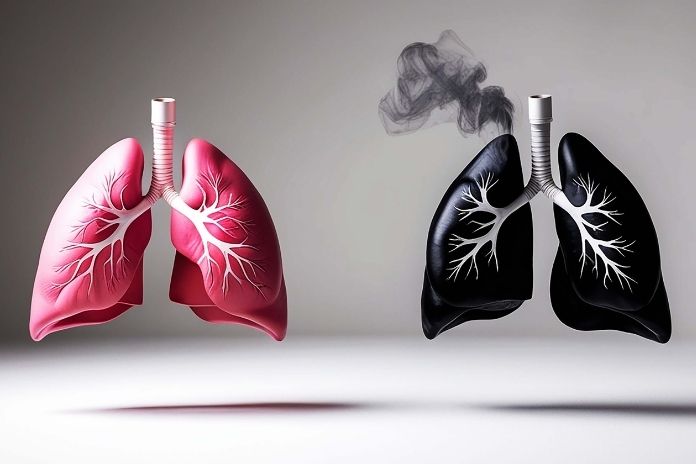
Breathlessness is tougher to manage when COPD and lung cancer coexist because airflow limitation and tumor-related effects add up, but practical breathing techniques, airway-clearance routines, pulmonary rehab, and targeted medical support (oxygen, NIV, inhaler optimization) can substantially reduce symptoms and improve daily life.
If you have COPD and are being evaluated or treated for lung cancer, you know how frightening shortness of breath can feel. COPD narrows the airways and traps air, and additional factors- like a tumor, cancer-related inflammation, treatment effects (surgery, radiation, or chemotherapy), or anemia- can put extra strain on your lungs and make breathing even harder.
This guide gives you practical, evidence-based breathing strategies to use immediately (pursed-lip and diaphragmatic breathing), airway-clearance routines to loosen mucus, pacing and energy-conservation tactics, and safe ways to build capacity (pulmonary rehabilitation and inspiratory-muscle training).
In this article, we’ll also explain when supplemental oxygen or non-invasive ventilation (NIV) may be appropriate, which red-flag symptoms require urgent medical attention, and how to collaborate effectively with your clinical care team.
These strategies are meant to complement, never replace, professional medical care, so always consult your clinician before adjusting oxygen settings, starting new devices, or changing prescribed medications.
Why Breathlessness Hits Harder with COPD + Lung Cancer
Two problems stack up. COPD causes long-standing airflow limitation, air trapping, and hyperinflation, so your diaphragm sits flattened, and breathing becomes inefficient. Add a lung tumor, and you may have extra airway narrowing, local inflammation, pleural irritation, or pain that limits full breaths.
Treatments can also worsen breathlessness: lung resection reduces lung volume, radiation can cause pneumonitis, and chemotherapy or anemia can lower oxygen delivery. Together, these factors increase the work of breathing and reduce reserves, so even small activities feel exhausting.
Psychological factors matter too. Anxiety and panic raise respiratory drive and create a vicious cycle of breathlessness, fear, and more breathlessness. Recognizing this “double hit” helps explain why practical breathing strategies and rehabilitation matter. They both ease symptoms and rebuild functional reserve.
Quick-Relief Breathing Techniques You Can Use Anywhere

These are the first tools to try when breathless. Practice them when calm so they’re automatic during flare-ups.
Pursed-lip breathing (PLB). Inhale slowly through the nose for 2 counts, then pucker your lips and exhale gently for 4 counts (exhale 2–3× longer than the inhale). PLB slows respiratory rate, reduces air-trapping, and helps you feel in control during panic. It’s simple and effective in COPD and during acute shortness of breath. Practice 5–10 minutes several times daily and whenever you feel breathless.
Diaphragmatic (belly) breathing. Place one hand on your chest and one on your belly. Breathe in slowly through the nose, letting the belly rise more than the chest; exhale with relaxed pursed lips. This reconditions the diaphragm and reduces the reliance on accessory neck muscles. Begin this practice lying down, then transition to a seated position and finally to a standing position. Short, regular practice sessions (5–10 minutes, 2–3×/day) build endurance.
Recovery positions. Sit forward with forearms on your thighs (“tripod”); if standing, lean forward against a counter or wall; when lying, prop with pillows. These positions mechanically help the diaphragm work more effectively and can rapidly reduce breathlessness when combined with PLB.
Paced-activity breathing. Match breathing to movement: inhale for 1–2 steps, exhale for 3–4 steps. Use this for stairs, dressing, or carrying light items. It prevents breath-holding and reduces spikes in breathlessness.
Panic-reset add-ons. Brief box-breathing (4-4-4-4 counts), grounding phrases, or a handheld fan to the face can lower perceived breathlessness quickly. These tools act on the brain’s perception of dyspnea and are useful during anxiety-driven episodes.
Clear the Mucus: Airway-Clearance Routines
When COPD and cancer produce excess secretions, active airway-clearance helps prevent infections and reduces cough-related breathlessness.
Active Cycle of Breathing Techniques (ACBT) & Huff cough. ACBT cycles breathing control (gentle, relaxed breaths), thoracic expansion (deep breaths with 3–4 second holds), and huffing (sharp, open-mouth exhalation: “ha”) to move mucus from small to larger airways for easier expectoration.
Only cough when necessary; huffing is less tiring and more effective than repeated forceful coughing. Physiotherapy teams commonly teach ACBT; typical sessions last 10–15 minutes once or twice daily or as needed.
Hydration and humidification are important. Adequate oral fluids help thin secretions. If indoor air is dry, a clean humidifier can ease mucus mobilization, but it’s important to follow cleaning recommendations to avoid mold. Nebulized saline, when prescribed, may help loosen secretions in some patients. Always check with your healthcare team before using home nebulizers.
Devices (when prescribed). Positive expiratory pressure (PEP) devices and oscillatory PEP devices (Acapella, Flutter) can mobilize secretions effectively and are supported by trials showing similar benefits to other chest-physio methods.
These devices are used under the guidance of a physiotherapist. Evidence shows PEP techniques can improve expectoration and patient comfort, though no single method is clearly superior for everyone.
Post-op & radiation tips. After surgery, use incentive spirometry, take regular deep-breath sessions, and “splint” your incision with a pillow when you cough to reduce pain and encourage effective coughing. Your physiotherapist will tailor the routine to your recovery stage to avoid undue strain.
Read More: Persistent Cough vs. Lung Cancer: When to Worry
Build Capacity Safely: Pulmonary Rehab & Training

Improving fitness and respiratory muscle function reduces breathlessness and improves quality of life, even during or after cancer therapy when cleared by your team.
Pulmonary rehabilitation (PR). PR is a supervised, multidisciplinary program that combines aerobic training, strength training, breathing retraining, education, and psychosocial support.
High-quality evidence and ATS guidance show PR reduces dyspnea, increases exercise capacity, and improves health-related quality of life in people with COPD; PR is increasingly offered around lung-cancer surgery as prehabilitation and post-op recovery to shorten complications and speed return to function.
Dr. Carolyn L. Rochester, lead author on the ATS PR guideline, emphasizes that PR is an evidence-based cornerstone for breathlessness management.
Inspiratory Muscle Training (IMT). IMT uses threshold devices to strengthen the diaphragm and other inspiratory muscles. Cochrane and recent trials show IMT can increase inspiratory muscle strength and may help people with documented respiratory muscle weakness; combined PR+IMT sometimes adds benefit, particularly in those with muscle weakness or prolonged disability. Your rehab team will test and prescribe the appropriate resistance and schedule.
Gentle conditioning plan. Begin with interval walking (1–2 minutes walk/1–2 minutes rest) and progress slowly as tolerated. Add light resistance training for legs and core to support posture and reduce breathlessness during daily tasks. Consistency matters more than intensity; small, regular gains translate into major daily-life improvements.
Read More: Exercises to Increase Lung Capacity and Strength
Oxygen & Ventilatory Support, When and How
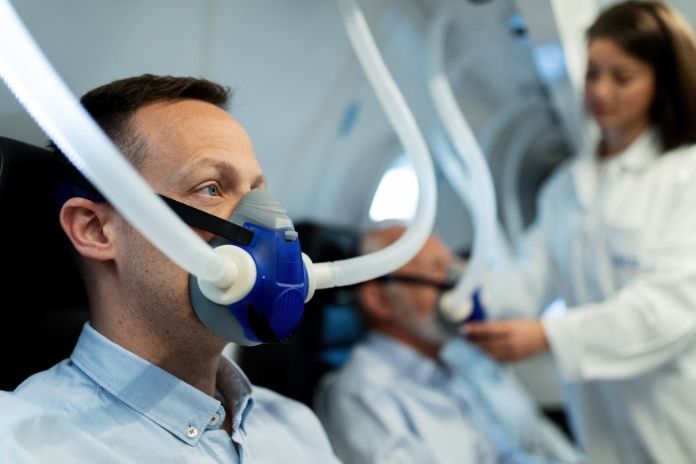
Some patients with COPD + lung cancer will need supplemental oxygen or ventilatory support; these decisions are clinical and individualized.
Oxygen therapy. Long-term oxygen therapy (LTOT) is indicated for chronic, severe hypoxemia (documented low resting PaO₂ or SpO₂) and reduces mortality in patients who meet strict criteria; ambulatory or nocturnal oxygen may be prescribed for exertional or nocturnal desaturation.
Don’t change flow rates on your own; your clinician will set target saturations (often 88–92% for people at risk of hypercapnia, higher in others). Follow oxygen-safety rules: no smoking near oxygen, keep tanks secure, and watch tubing to prevent falls.
Non-invasive ventilation (NIV). NIV (BiPAP/CPAP) is used for acute hypercapnic respiratory failure and, in selected patients, as home therapy for chronic hypercapnic COPD to improve gas exchange and reduce hospitalizations. Use only under specialist supervision with monitoring and titration by respiratory teams.
Pulse oximetry. A home pulse oximeter is a useful trend tool to track your personal baseline and discuss safe target ranges with your team. Don’t panic over single low readings; note trends, activity context, and symptoms. If you have sudden large drops or readings well below your target range, seek urgent care.
Read More: Top 10 Breathing Support Products to Enhance Lung Health Naturally
Medications & Inhaler Technique Matter

Optimizing inhaler therapy and medication review prevents avoidable breathlessness.
COPD regimen optimization. Long-acting bronchodilators (LAMA, LABA), with or without inhaled corticosteroid, depending on phenotype and exacerbation history, are the backbone of symptom control. Keep a fast-acting rescue inhaler accessible. Your team will tailor combos based on symptoms and prior exacerbations.
Inhaler technique checks. Critical errors in inhaler use are common and reduce treatment effectiveness. Regular technique reviews (including spacer use for pMDIs and correct inhalation for DPI devices) should be part of every visit. Studies show training reduces exacerbations and improves symptom control. Ask a nurse, pharmacist, or respiratory therapist for a hands-on demo at each appointment.
Treatment interactions & red flags. New or worsening breathlessness during cancer therapy can signal infection, radiation pneumonitis, immune-related pneumonitis from immunotherapy, or anemia; report changes promptly. Also, review medications for cough-causing drugs (ACE inhibitors) and discuss alternatives if needed.
“A dedicated inhaler technique service produced a significant reduction in the rate of moderate-to-severe exacerbations of asthma and COPD, as well as a reduction in hospital admissions and length of stay.” – Dr. Toby GD. Capstick, Respiratory Medicine Researcher
Pacing & Energy Conservation for Daily Life

Small changes let you do more with less breath.
- Plan, prioritize, position. Break tasks into steps, do the hardest parts at your best time of day, and keep commonly used items at waist level to avoid reaching. Sit for grooming, use a shower chair, and employ long-handled tools for dressing and housework. When lifting or pushing, exhale on effort; this reduces breath-holding and breathlessness.
- Pacing techniques. Use the “one-to-one” or “two-to-three” pacing rules: perform an activity in short bouts interspersed with rest (e.g., fold laundry for 5 minutes, rest 2 minutes). Measure progress by steps or time rather than symptom severity; slowly increase activity as tolerated.
- Food & fluids. Small, frequent meals can help reduce abdominal bloating, which limits diaphragm descent. Prioritize protein to preserve muscle mass; dehydration thickens mucus, so keep fluids up unless your clinician advises fluid restriction. Limit alcohol and foods that trigger reflux, which worsen cough and nighttime breathlessness.
- Sleep & restorative routines. Elevate the head of the bed to reduce reflux-related cough. Establish a regular sleep routine and manage nighttime symptoms with the help of your healthcare team. A good night’s sleep supports daytime breathing and energy.
Mind–Breath Connection: Taming the Dyspnea–Anxiety Loop

Breathlessness and anxiety fuel each other. Brief cognitive-behavioral techniques, mindfulness, and guided imagery have been shown to reduce panic and perceived breathlessness.
Practicing PLB or diaphragmatic breathing during calm moments strengthens your confidence so techniques become automatic under stress. Digital apps for paced breathing and short mindfulness sessions can be useful adjuncts.
For refractory, severe dyspnea, specialist teams sometimes consider low-dose opioids under palliative guidance; systematic reviews show opioids may relieve breathlessness in advanced disease, but they require careful balancing of benefits and respiratory risks and must be managed by specialists. Always discuss risks, goals, and monitoring with your clinical team.
Home Air Quality & Prevention

Clean air at home reduces symptom triggers.
Stop smoking and avoid secondhand smoke. Smoking cessation is the single best action to slow COPD progression and improve surgical and treatment outcomes if you have lung cancer. Seek clinician support (nicotine replacement, medications, counseling).
Indoor air improvements. Use cross-ventilation, limit use of strong cleaners/air fresheners, reduce dust, and consider a HEPA air purifier if you live near heavy traffic or use biomass fuels. Keep humidifiers clean to avoid microbial growth. Test for radon and remediate if levels are high, as radon exposure increases the risk of lung cancer.
Vaccinations. Stay current with seasonal influenza and pneumococcal vaccines to prevent infections that can set back lung function and recovery during cancer treatment. Discuss timing with your oncology and pulmonary teams.
Read More: 10 Simple Indoor Air Quality Solutions
Monitoring & When to call the Doctor
Track simple objective and subjective measures: breathlessness on exertion (e.g., mMRC scale), distance or time you can walk, cough frequency, sputum color/volume, daily resting SpO₂ trends, and weight/appetite. Record changes and bring them to appointments.
Seek urgent care for: sudden or rapidly worsening breathlessness, chest pain, coughing up blood, fever/chills, confusion, blue lips/fingertips, oxygen saturation well below your usual target, or new leg swelling (possible clot).
These signs can indicate infection, pulmonary embolism, major bleeding, or acute respiratory failure and need prompt evaluation. For non-urgent worsening (slowly increasing exertional breathlessness, more frequent nocturnal cough), arrange a clinician visit within days.
FAQs
Will breathing exercises replace the need for inhalers or oxygen?
No, breathing techniques help symptoms and reduce anxiety, but do not substitute for prescribed inhaled medications or oxygen. Always follow your medication and oxygen plan and check with your clinician before making changes.
Is pulmonary rehab safe during cancer treatment?
Often yes, with medical clearance. Prehabilitation and perioperative rehabilitation programs are increasingly used to improve surgical outcomes and speed recovery; the intensity and timing are tailored to minimize treatment side effects and individual energy levels.
Which technique helps most during activity?
Combine pursed-lip breathing, paced steps, and a recovery position practiced when calm; that combination is the fastest way to lower breathlessness during exertion. Practice regularly so it becomes automatic.
Key Takeaways
When COPD and lung cancer coexist, breathlessness can be intense, but it’s still manageable. Pair fast, practical techniques (pursed-lip and diaphragmatic breathing, recovery positions) with airway-clearance routines (ACBT/PEP), supervised pulmonary rehabilitation, and optimized inhaler and medical care.
Use oxygen or NIV only under clinician guidance, monitor trends (pulse oximetry, mMRC, sputum), and act fast for red-flag signs (sudden breathlessness, bleeding, fever). Small, consistent steps, pacing, nutrition, vaccinations, and clean air add up to meaningful improvements in daily life. Work closely with your respiratory and oncology teams to individualize a safe plan.
References
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4718929/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9448004/
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/lung-cancer/manage-shortness-of-breath-with-lung-cancer
- https://www.webmd.com/lung/copd/lung-cancer-copd
- https://www.cancercenter.com/community/blog/2020/09/shortness-of-breath
- https://www.who.int/news-room/fact-sheets/detail/chronic-obstructive-pulmonary-disease-(copd)
- https://supporting-breathlessness.org.uk/support_copd/understanding-breathlessness-copd/
- https://www.cancerresearchuk.org/about-cancer/coping/physically/breathing-problems/causes-breathlessness
- https://my.clevelandclinic.org/health/symptoms/16942-dyspnea
- https://www.mayoclinic.org/diseases-conditions/copd/symptoms-causes/syc-20353679
- https://www.healthdirect.gov.au/shortness-of-breath
- https://www.urmc.rochester.edu/encyclopedia/content
- https://my.clevelandclinic.org/health/diseases/8709-chronic-obstructive-pulmonary-disease-copd
- https://lungfoundation.com.au/support-and-resources/living-with-a-lung-disease/breathlessness/
In this Article