A hiatal hernia occurs when part of the stomach pushes upward through an opening in the diaphragm into the chest area. It’s a common condition, especially with increasing age, and many people have a hiatal hernia without realizing it because it often causes no symptoms.
When symptoms do appear, they frequently overlap with acid reflux and heartburn, as the shifted stomach allows acid to move back into the esophagus. This can lead to burning chest pain, regurgitation, difficulty swallowing, bloating, or discomfort in the upper abdomen.
Because these signs are similar to common digestive issues, a hiatal hernia may go unnoticed for years. Treatment depends on symptom severity and ranges from simple lifestyle changes to medical or surgical care.
Stay tuned as we break down symptoms, causes, treatment options, and when to see a doctor.
Read More: The Link Between Acid Reflux and Breathing Patterns
What Is a Hiatal Hernia?
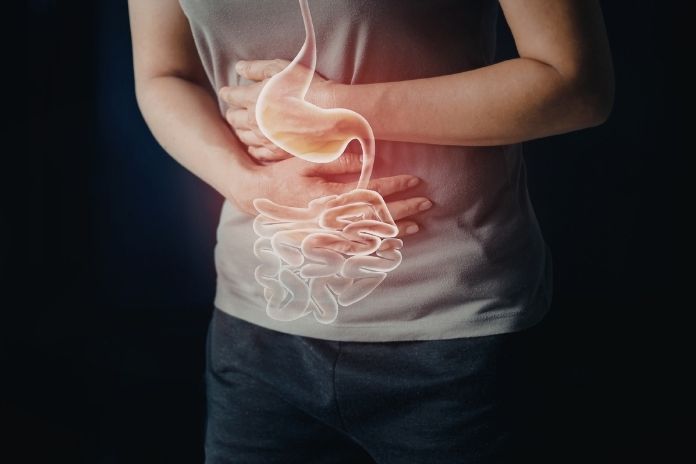
A hiatal hernia occurs when your stomach bulges through the diaphragm, a large muscle that separates your chest from your stomach. This muscle aids in the process of breathing by contracting and relaxing.
The diaphragm is located between your chest and stomach and protects you by allowing the food you eat to stay in your stomach. Over time, as you age, the muscles in this area relax and weaken. This is when hiatal hernias become a problem for older people.
In fact, some people may not experience any symptoms and discover the presence of GERD (Gastroesophageal Reflux Disease) during tests meant to check for something else. In cases where there are symptoms, they may include heartburn and the retrosternal return of food and acid into the esophagus.
In the case of smaller hiatal hernias, no treatment may be required at all. In other cases, particularly larger ones that may be causing discomfort, the first line of treatment would involve changes to one’s diet and the use of medications to combat excess acid. Often, surgery is the course of action.
Talking about Hiatus Hernia and its severity, Dr. Monisha Sudarshan, MD (Thoracic Surgeon, Cleveland Clinic) said, “If there’s a hiatal hernia and this patient is experiencing a lot of symptoms, such as nausea, vomiting, pain that is not going away, there is a possibility that stomach can move into the ches and twist, and cause problems.
That is on one spectrum. Then, at the other end of the spectrum, you have very small hiatal hernias that may not cause any problems, or the patient may not even know about them. So yes, it can be dangerous if it’s at the severe side of the spectrum.”
Read More: 7 Warning Signs and Side Effects of Poor Digestion You Shouldn’t Ignore
Types of Hiatal Hernia
A hiatal hernia isn’t the same for everyone. There are different types, each affecting the stomach and diaphragm in distinct ways. Understanding these types helps explain symptoms, risks, and why some cases need closer medical attention than others.
Sliding Hiatal Hernia
This is the most common type of hiatal hernia, accounting for around 95% of cases. In a sliding hiatal hernia, the spot where the esophagus (food tube) meets the stomach, called the gastroesophageal junction, and part of the stomach moves up through the opening in the diaphragm and into the chest.
What makes this hernia different is that it slides up and down through the diaphragm. As a result of this movement, symptoms such as heartburn or acid reflux may occur intermittently, depending on how often the stomach presses against the chest.
Many people with this type may not even notice symptoms, and often it is found during exams for other issues. Sliding hernias are closely linked to acid reflux or GERD because the shifting of the stomach makes it easier for stomach acid to travel back up into the esophagus.
Paraesophageal (Rolling) Hiatal Hernia
Paraesophageal hernias are less common but usually more serious than sliding ones. In these hernias, part of the stomach pushes up beside the esophagus and stays above the diaphragm even though the gastroesophageal junction remains in its usual place.
There are several paraesophageal types (types II, III, and IV): one in which only the stomach bulges beside the esophagus; another in which both the stomach and the junction move up; and a rare type in which another organ, such as part of the intestine or spleen, also enters the chest.
Because the stomach stays in the chest, there’s a greater risk of complications, such as the stomach twisting or losing its blood supply, so doctors often monitor these hernias more closely and may recommend surgical repair even when symptoms are mild.
Read More: 5 Essential Exercises to Avoid When Dealing with Back Pain
Common Symptoms of a Hiatal Hernia
A hiatal hernia happens when part of the stomach pushes up through the diaphragm into the chest. Many people never notice they have one because small hernias often cause no symptoms and are found only by accident during exams for other problems.
Heartburn
This is the most frequent complaint, a burning sensation in the chest or throat, usually after eating or when lying down. It happens because stomach acid flows back into the esophagus (acid reflux).
Acid Reflux
Also called gastroesophageal reflux, acid reflux involves stomach acid or food backing up into the throat or mouth. This can leave a sour taste, bad breath, or irritation in the throat.
Chest Discomfort
Many people feel a burning, squeezing, or pressure-like pain in the chest or upper belly. Sometimes this pain can be mistaken for a heart-related issue.
Regurgitation
This is when food, liquid, or stomach acid rises back up into the mouth or throat, especially after eating or bending over.
Difficulty Swallowing
Also known as dysphagia, this happens when a hernia presses on the esophagus, making swallowing solid foods feel slow or uncomfortable.
Shortness of Breath (in Some Cases)
A larger hernia can press on the diaphragm or lungs, causing breathlessness. This is less common but can occur, especially if the stomach pushes high into the chest.
In many cases, people with hiatal hernias have no symptoms at all, especially with smaller, sliding hernias. When symptoms do occur, they often resemble heartburn or reflux and can usually be managed with lifestyle changes or medications. If symptoms are severe or persistent, it’s important to talk to a healthcare provider.
Read More: Is Cold Weather Making Your Back Pain Worse?
What Causes a Hiatal Hernia?

A hiatal hernia doesn’t develop overnight. It usually results from a combination of muscle weakness and abdominal pressure. Understanding the common causes helps explain who is at risk and why certain everyday activities can trigger or worsen it.
Weakening of the Diaphragm Opening
A hiatal hernia happens when part of the stomach pushes up into the chest through the hiatus, the natural opening in the diaphragm where the esophagus passes.
In many people, the exact reason isn’t fully known, but weakness in the muscles and tissues around this opening allows the stomach to slip upward.
This weakness often develops as people age, as muscles lose strength and elasticity, making hernias more common in adults over 50.
Increased Abdominal Pressure
Extra pressure inside the belly can push the stomach upward and contribute to a hiatal hernia.
Everyday situations that increase abdominal pressure include:
- Heavy lifting or straining during exercise.
- Chronic coughing from smoking, lung conditions, or persistent sneezing.
- Obesity, where excess belly fat pushes against the diaphragm.
- Pregnancy, as the growing uterus increases pressure in the abdomen.
- Straining during bowel movements or frequent vomiting.
Genetic and Age-Related Factors
Some people are born with a naturally larger hiatus or weaker connective tissues, making a hernia more likely even without heavy strain. Family traits and genetics can influence the strength of the diaphragm and the surrounding ligaments.
Overall, hiatal hernias are usually the result of a combination of muscle weakness and increased abdominal pressure, and the risk increases with age, certain activities, and body weight. When these factors come together, the stomach can gradually move upward through the diaphragm opening and form a hernia.
Read More: Exercises to Combat Screen Time Strain
Hiatal Hernia vs GERD: What’s the Difference?

Hiatal hernia and GERD are often confused because they share similar symptoms. While they’re closely linked, they’re not the same condition. Understanding the difference helps in choosing the right treatment and managing symptoms better.
How a Hiatal Hernia Can Worsen Reflux
A hiatal hernia is a physical condition in which part of the stomach pushes up into the chest through an opening in the diaphragm, the muscle that separates the chest from the belly.
This shift can weaken the lower esophageal sphincter (LES), the muscle that normally keeps stomach acid from flowing back up into the esophagus. When the LES doesn’t work well, stomach acid can rise more easily, leading to acid reflux and symptoms like heartburn.
In some people, especially with larger hernias, this increases the likelihood of developing GERD (chronic acid reflux disease). A hernia doesn’t always cause reflux, but it can make reflux more frequent or severe.
Why Not All Reflux Is Caused by a Hernia
While hiatal hernias and reflux often occur together, they are not the same thing. GERD is a digestive disorder where acid repeatedly flows back into the esophagus, causing irritation and inflammation. GERD can occur without anyone having a hiatal hernia.
Factors like a weak LES, pressure on the stomach from obesity, pregnancy, certain foods, smoking, or lifestyle habits can trigger GERD even when there’s no structural hernia. Likewise, many people with a hiatal hernia may never develop troublesome reflux.
When the Two Conditions Overlap
Often, a hiatal hernia and GERD are found together, especially when reflux symptoms are frequent or long-lasting.
In these cases, the hernia can make acid reflux harder to control. It may require more focused treatment, such as lifestyle changes, medications that reduce stomach acid, or even surgery if symptoms are severe.
It’s essential to get a proper evaluation so a doctor can determine whether symptoms are due to GERD, a hiatal hernia, or both.
Read More: Can Standing Desks Reduce Your Risk of Chronic Back Pain?
How Hiatal Hernias Are Diagnosed
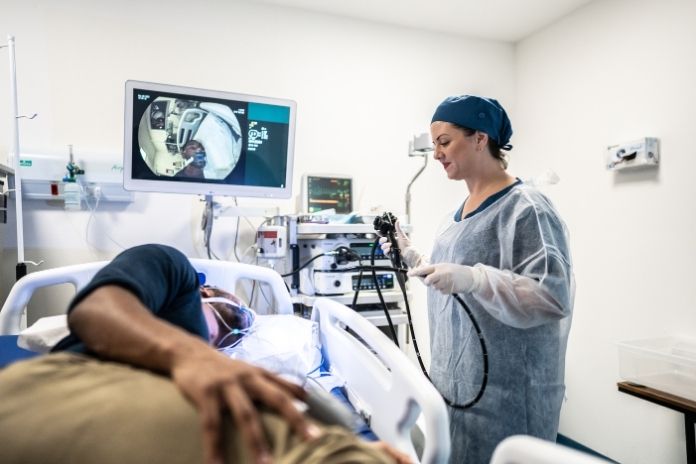
Diagnosing a hiatal hernia usually starts with understanding symptoms and medical history. In some cases, simple imaging tests help confirm the condition, especially when symptoms are persistent or severe.
Medical History and Symptom Review
Diagnosis often begins with a doctor asking about your symptoms and medical history. This helps determine whether heartburn, chest pain, regurgitation, or swallowing troubles might be linked to a hiatal hernia.
Your doctor will also perform a physical exam and may ask about acid reflux or symptoms of gastroesophageal reflux disease (GERD). This step guides which tests are needed next.
Imaging Tests
Barium Swallow (Upper GI Series)
In this test, you drink a chalky liquid called barium, which coats your upper digestive tract. As it moves down your esophagus and stomach, X-rays are taken to help doctors see whether part of your stomach is pushing up through the diaphragm. This is one of the most common ways to confirm a hiatal hernia and to view its size and position.
Endoscopy
An upper endoscopy uses a thin, flexible tube with a tiny camera that is passed through your mouth into your esophagus and stomach. This lets doctors directly see the hernia and check for irritation or inflammation from acid reflux. Endoscopy can also detect complications like esophagitis or Barrett’s esophagus.
When Testing Is Necessary vs Optional
Not everyone needs all the tests. If a person has mild or no symptoms, or a hernia is found accidentally during tests for another condition, further imaging may not be necessary immediately.
However, if symptoms are frequent or severe, your doctor will typically order imaging tests, such as a barium swallow or endoscopy, to confirm the diagnosis and guide treatment.
In some cases, tests that measure esophageal muscle movement (manometry) or acid exposure (pH testing) may also be used.
Read More: Why Your Neck Hurts: Uncovering Hidden Causes
Treatment Options for Hiatal Hernia

Treating a hiatal hernia focuses on easing symptoms and preventing complications. Options range from simple lifestyle changes and medications to surgery in more severe cases, depending on symptom severity and overall health.
Lifestyle Changes
For many people, simple changes in daily habits can greatly reduce symptoms of a hiatal hernia:
- Eating smaller meals: Eating less at one time decreases pressure on the stomach and reduces acid moving up into the esophagus.
- Avoiding trigger foods: Foods that worsen heartburn (like spicy or fatty foods, chocolate, caffeine, and citrus) are best limited.
- Not lying down after eating: Waiting at least 2-3 hours before lying down or going to bed helps prevent reflux.
- Weight management: Losing extra weight can reduce pressure on the abdomen and improve symptoms, especially in people who are overweight or obese. Staying upright after meals and wearing loose clothing around the waist also helps ease discomfort.
Lifestyle changes don’t fix the hernia itself, but they can significantly decrease reflux and pain.
Medications
Doctors often recommend medicines to reduce acid and relieve symptoms:
- Antacids: Provide quick, short-term relief by neutralizing stomach acid.
- H2 blockers: Reduce acid production for longer relief than antacids.
- Proton pump inhibitors (PPIs): Stronger acid-blocking drugs that help heal irritation in the esophagus.
These medications help control symptoms and protect the esophagus from damage, but they don’t cure the hernia itself; they simply reduce the acid that causes discomfort. Long-term use should be monitored by a doctor.
Surgery
When surgery is considered:
Surgery may be recommended when symptoms are severe, don’t improve with lifestyle and medications, or complications like difficulty swallowing or bleeding occur.
Goals of surgical repair:
The most common operation, fundoplication, strengthens the barrier between the stomach and esophagus and repairs the hernia. Newer options like the LINX device use a ring of magnetic beads to support the lower esophageal sphincter and reduce reflux.
Risks and recovery overview:
As with any surgery, there are risks such as infection, difficulty swallowing, or gas bloating. Recovery typically involves a gradual return to normal activities and a temporary special diet. Most people feel significant relief from reflux after successful surgery.
Read More: 10 Top Coccyx Cushions to Buy for Relief
Foods and Habits That Can Make Symptoms Worse

If you have a hiatal hernia, certain foods and daily habits can trigger or worsen symptoms like heartburn, acid reflux, and discomfort. Being aware of these can help you feel better and manage symptoms more effectively.
Large or Fatty Meals
Eating big meals puts extra pressure on your stomach and diaphragm, making it easier for acid to move up into the esophagus. High-fat foods (like fried foods, creamy sauces, fast food, and rich desserts) also slow digestion and increase reflux. Smaller, more frequent meals are easier on the digestive system and help reduce pressure.
Spicy or Acidic Foods
Spicy foods (such as hot peppers or curries) and acidic foods (like citrus fruits, tomatoes, and vinegar-based sauces) can irritate the esophagus and increase heartburn. If these foods trigger burning or discomfort, it’s best to limit or avoid them.
Alcohol and Caffeine
Drinks containing alcohol or caffeine (like coffee, tea, energy drinks, and soda) can relax the lower esophageal sphincter (LES), the muscle that helps keep acid in the stomach. When the LES relaxes, acid can flow back up more easily, worsening reflux symptoms. Cutting back on these beverages often helps improve comfort.
Tight Clothing
Wearing tight belts, waistbands, or clothing that squeezes your belly increases pressure on your stomach and can push acid upward. Choosing looser, more comfortable clothing helps reduce strain around your abdomen.
Late-Night Eating
Eating close to bedtime doesn’t give your body enough time to digest before lying down. Gravity helps keep acid in the stomach when you’re upright, so it’s better to finish eating at least 2-3 hours before lying down or sleeping.
Expert’s Advice
Most of the time, simple lifestyle tweaks can bring relief for mild hiatal hernia pain and symptoms, explains Dr. Anish Sheth, MD, gastroenterologist and Chief of Gastroenterology at Penn Medicine Princeton Medical Center. The condition does not heal on its own.
“Controlling acid reflux with common acid-blockers, like Prilosec, and making dietary changes—such as avoiding spicy foods, caffeine, and alcohol—are usually sufficient.” Eating smaller meals, not lying down soon after eating, and weight loss (for individuals with obesity) may also help.
Read More: 8 Best Back Stretchers – Reviews and Buying Guidance
Living With a Hiatal Hernia

Living with a hiatal hernia often means making small but consistent lifestyle adjustments. With proper care, most people manage symptoms well, stay comfortable, and avoid complications while continuing their normal daily activities.
Long-Term Outlook
If your hiatal hernia doesn’t cause symptoms, many people live with it without trouble for years and may never need treatment. A hernia itself won’t go away on its own and might slowly get larger over time, but it doesn’t always lead to serious problems.
If symptoms like acid reflux or heartburn occur, most can be managed well with lifestyle changes and medicines, and only a small number of people need surgery.
Managing Symptoms Day to Day
Everyday habits can make a big difference in how you feel. Eat smaller, more frequent meals to reduce pressure on your stomach. Avoid trigger foods like fatty, spicy, or acidic foods, chocolate, caffeine, and alcohol. These can worsen acid reflux. Don’t lie down soon after eating; wait a few hours to let your food digest.
Maintain a healthy weight and avoid smoking, as these reduce pressure on your stomach and diaphragm. Over-the-counter antacids or acid-reducing medicines can also help relieve reflux and heartburn when used as directed.
When Symptoms May Change Over Time
Symptoms can change or worsen over time, especially if acid reflux becomes more frequent. If lifestyle changes and medicines no longer help, or if you start having trouble swallowing, vomiting, unexplained weight loss, or severe chest pain, it’s important to see a doctor; these changes may signal complications or the need for further treatment.
Read More: 10 Pressure Points That Provide Relief from Cramps
When to See a Doctor?

Even though many people with a hiatal hernia have mild discomfort, there are certain times when you should seek medical help right away.
Persistent or Worsening Symptoms
If symptoms like heartburn, acid reflux, or upper belly pain don’t improve despite lifestyle changes (like small meals, avoiding trigger foods, and not lying down after eating) or medications, it’s essential to talk to a doctor. Ongoing or worsening symptoms can indicate that your condition requires stronger treatments or additional tests.
Chest Pain That Doesn’t Feel Like Heartburn
Sometimes, pain in the chest may not be simple heartburn. Sudden, severe pressure, squeezing pain, or pain that spreads to the arm, shoulder, or jaw could signal a more serious problem, such as heart issues or complications from the hernia. If chest pain feels unusual or severe, seek urgent medical care.
Difficulty Swallowing
If you begin to have trouble swallowing or feel like food is stuck in your throat or chest, this needs prompt evaluation. This can happen if the hernia affects the esophagus or if there’s swelling or a blockage.
Vomiting Blood or Black Stools
These are warning signs that there may be bleeding somewhere in your digestive tract. Vomiting blood or passing black, tar-like stools should never be ignored; you should see a doctor immediately or go to the emergency room.
When in doubt, getting checked out early can prevent complications and give you peace of mind, especially if symptoms suddenly change or become more intense.
Final Takeaway

These types of hiatal hernias are very common, and for most, there are no issues. People can live with this condition without any problems, while some may experience a few difficulties, which could be associated with acid reflux.
In most instances, symptoms can be managed through dietary changes, such as taking smaller portions, avoiding inducements, maintaining a healthy weight, and taking medications as directed by doctors.
Although it’s quite rare, the need for surgery is normally entertained in cases of severe symptoms or when complications arise. That said, it is always best to consult a medical professional for symptoms such as difficulty swallowing, chest discomfort, or bleeding.
In cases where you are experiencing symptoms regularly and are unsure if it’s normal, it’s advised to consult a doctor and take measures to protect your digestive system.
References
- Hiatal hernia – Diagnosis and treatment – Mayo Clinic. (n.d.).
- Hiatal Hernia. (2025, December 11). Cleveland Clinic.
- Hiatal hernia Symptoms & Treatment | Aurora Health Care. (n.d.).
- Smith, R. E., Sharma, S., & Shahjehan, R. D. (2024, July 17). Hiatal Hernia. StatPearls – NCBI Bookshelf.
- Hiatal hernia: MedlinePlus Medical Encyclopedia. (n.d.)
- Booth, S. (2025, August 4). What is a hiatal hernia? WebMD.
- Indigestion vs. a Hernia: How to Tell the Difference: Surgical Associates of North Texas: Advanced Laparoscopic Surgeons. (n.d.)
- Sami, S. (2024, April 19). Gastro-Oesophageal Reflux Disease (GORD) | Digestive health. Digestive Health UK.
- The connection between hiatal hernias and GERD | Banner Health. (n.d.).
- NHS inform. (2023, May 29). Hiatus hernia | NHS inform. NHS Inform.
- CARE Hospitals. (n.d.). CARE hospitals.
- Singhal, V. K., Suleman, A. M., Senofer, N., & Singhal, V. V. (2024). Current Trends in the Management of hiatal Hernia: A Literature review of 10 years of data. Cureus, 16(10), e71921
- RefluxUK. (2025, October 20). Treatment options for hiatus hernia: medication, surgery & more. RefluxUK.
- Hiatal hernia Symptoms & Treatment | Aurora Health Care. (n.d.-b).
- Ezhilarasan, M. L. (n.d.). Hernia Diet Best and Worst foods to eat.
- The best diet for managing a hiatal hernia | The Hospital of Central Connecticut | CT. (n.d.).
- Hiatus hernia. (n.d.). HSE.ie.
- LivGastro. (2023, April 6). Hiatal Hernia: Understanding its Symptoms, Diagnosis & Treatment.
In this Article


















