Picture this. You’ve just been told you have hairy cell leukemia. The name alone sounds frightening. A quick search floods you with medical jargon, survival statistics, and worst-case scenarios. Your mind jumps ahead before your doctor even finishes the sentence. And beneath all that noise sits one steady, human question: what happens now?
Here’s the thing. Hairy cell leukemia, or HCL, is rare and slow-growing, but it’s also one of the most treatable blood cancers we know today.
Treatment for HCL isn’t a single moment. It’s a clear, step-by-step process designed to work with the pace of the disease, not against your body. It may begin with watchful waiting, move into targeted first-line therapy, and be followed by a recovery phase where blood counts steadily return to normal.
If the disease ever comes back, there are proven options to manage relapse and regain control. Long-term follow-up is part of the plan, too, focused on keeping you well, not keeping you scared.
This guide breaks the entire journey down in plain language. You’ll learn when treatment is needed and when it isn’t, what the most common therapies are, how recovery usually feels, and what long-term life with HCL actually looks like. No panic. No guesswork. Just clarity, context, and a roadmap forward so you know what to expect and why each step matters.
What Is Hairy Cell Leukemia?
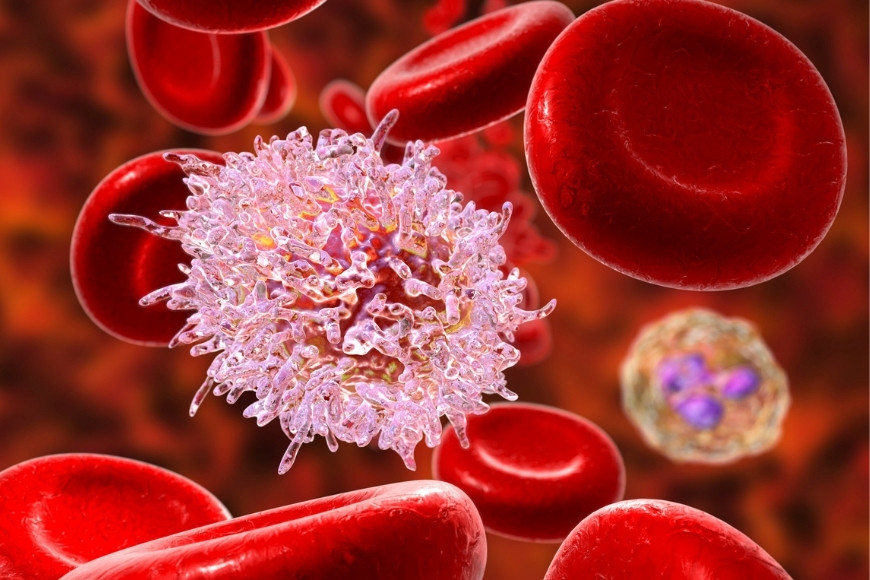
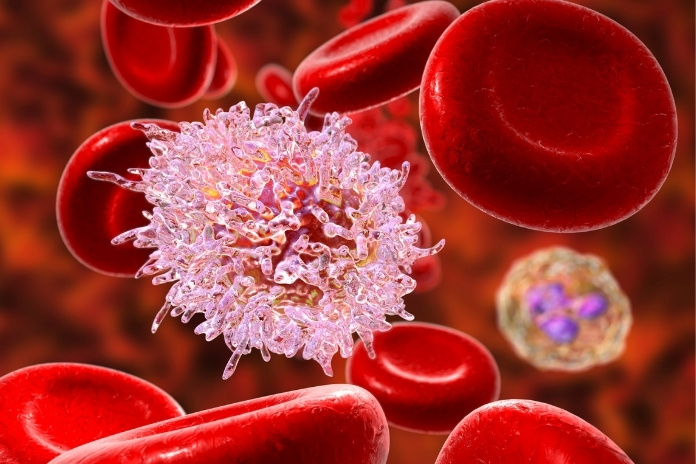
Hairy cell leukemia is a rare, chronic cancer of the blood and bone marrow that begins in B lymphocytes, the white blood cells responsible for making antibodies. The disease gets its name from the appearance of the cancerous cells under a microscope, where they show fine, hair-like projections along their surface. This distinctive feature helps doctors identify the condition accurately.
Key points at a glance:
- Affects B cells, a type of white blood cell.
- Named after the hair-like projections seen under the microscope.
- Classified as chronic, slow-growing leukemia.
Hairy cell leukemia accounts for roughly 2 percent of all leukemia cases. It commonly affects middle-aged and older adults and is diagnosed more often in men. Unlike aggressive leukemias that progress quickly and require urgent treatment, HCL develops slowly and often remains stable for long periods.
How it typically progresses:
- Slow buildup of abnormal B cells in the bone marrow.
- Gradual decline in healthy blood cells.
- Symptoms may take months or years to appear.
As the abnormal cells accumulate, they can crowd out normal blood cell production. Over time, this may lead to fatigue from anemia, frequent infections due to low white blood cells, or easy bruising and bleeding from low platelets. Some people also experience abdominal discomfort caused by an enlarged spleen.
Common symptoms include:
- Persistent fatigue
- Recurrent infections
- Easy bruising or bleeding
- Fullness or discomfort in the abdomen
According to the National Institutes of Health, advances in treatment over the past three decades have dramatically improved outcomes for people with hairy cell leukemia.
Today, it is considered one of the most treatable blood cancers, with therapies that often produce long-lasting remission and allow patients to live full, normal lives with regular follow-up rather than ongoing intensive treatment.
Read More: Leukemia – Causes, Symptoms, Treatment
Do All Patients Need Immediate Treatment?

Short answer: no. For many people, this is one of the most reassuring parts of a hairy cell leukemia diagnosis.
HCL progresses slowly, unlike aggressive blood cancers. Starting treatment too early does not improve outcomes and can expose patients to unnecessary side effects. For this reason, many newly diagnosed patients begin with watchful waiting, also called active surveillance. This means the disease is carefully monitored, not ignored.
When Watchful Waiting Is Appropriate
Doctors may recommend observation if you have:
- Stable blood counts
- No frequent or serious infections
- Mild or no fatigue
- No painful or significantly enlarged spleen
What Monitoring Looks Like
During watchful waiting, follow-up typically includes:
- Blood tests every three to six months
- Physical exams focused on spleen size
- Symptom check-ins for fatigue or infections
This phase can last months or even years. Many patients remain stable without treatment and continue normal, active lives. Watchful waiting ensures therapy begins only when it truly provides benefit.
When Doctors Decide It’s Time to Start Treatment
Treatment for hairy cell leukemia is not based on the diagnosis alone. It begins when the disease starts to affect your health, blood counts, or day-to-day quality of life. The goal is precise timing, stepping in when treatment clearly provides benefit, not before.
Because HCL progresses slowly, doctors rely on well-defined clinical and laboratory triggers rather than fear or urgency. This ensures patients receive therapy only when it is truly needed.
Clear Triggers for Treatment
Doctors usually recommend starting treatment if you develop:
- Neutropenia, meaning low white blood cell counts, increases the risk of infections.
- Anemia can cause persistent fatigue, weakness, or shortness of breath.
- Thrombocytopenia, or low platelet counts, raises the risk of bruising or bleeding.
- Recurrent or serious infections, even if blood counts are only moderately low.
- Symptomatic splenomegaly occurs when an enlarged spleen causes pain, fullness, or early satiety.
- Progressive fatigue that interferes with work, daily activities, or overall functioning.
These signs indicate that the abnormal cells are interfering with normal blood production or immune defense. At this point, treatment is not just helpful; it is necessary.
Undergoing treatment only when there is a need maximizes treatment effectiveness, minimizes unnecessary side effects, and helps patients maintain the best possible quality of life over the long term.
First-Line Treatments for Hairy Cell Leukemia
Therapy for hairy cell leukemia is highly standardized and extremely effective. For decades, a class of medications called purine analogs has formed the backbone of first-line treatment. These drugs directly target the abnormal B cells that drive the disease, while allowing normal blood production to recover over time.
Purine Analogs: The Gold Standard
Purine analogs are considered the gold standard because they produce deep, durable remissions in the majority of patients, often after just one course of therapy. Unlike many cancer treatments, they are not given indefinitely. Treatment is time-limited, followed by a recovery period and long-term monitoring.
Cladribine (First-Line Therapy for Most Patients)
Cladribine is the most commonly used initial treatment for hairy cell leukemia and is the preferred option for most patients.
How it’s given:
- Continuous intravenous infusion over five to seven days.
- Daily injections for five to seven days, depending on the treatment plan.
How it works: Cladribine selectively targets abnormal B cells, triggering cell death while sparing many healthy cells. This targeted action allows the bone marrow to gradually recover normal blood cell production.
What to expect: Blood counts typically drop temporarily within the first few weeks after treatment. This is expected and closely monitored. Recovery follows gradually over one to three months as healthy cells repopulate the marrow.
Effectiveness: Clinical studies published in Blood and indexed in PubMed show complete remission rates of approximately 85 to 90 percent after a single course of cladribine.
According to Dr. Robert Kreitman, MD, a hematologist at the National Cancer Institute, long-term remission is common after first-line treatment for hairy cell leukemia.
He explains, “With cladribine alone, long-term follow-up studies show median remission durations of about 15 to 16 years after the first treatment,” highlighting how durable responses often are with a single course of therapy.
Pentostatin
Pentostatin is an alternative purine analog used in specific situations.
How it’s given:
- Intravenous infusion every two weeks over several months.
When it’s used:
- When cladribine is not suitable
- In select patient-specific scenarios based on health status or having prior treatment considerations
Response rates with pentostatin are similar to those of cladribine, but the treatment course is longer and requires more frequent clinic visits. Like cladribine, pentostatin is highly effective and can lead to long-lasting remission when appropriately used.
What to Expect During and After First-Line Treatment

Starting treatment can feel intimidating, but knowing what to expect helps ease that anxiety. First-line therapy for hairy cell leukemia is highly effective, and most side effects are temporary and closely monitored.
Temporary Side Effects Are Common
During and shortly after treatment, patients may experience:
- Fatigue
- Fever-like symptoms
- A temporary drop in blood counts
- Increased infection risk for several weeks
Because infection risk is the highest during this phase, doctors monitor blood counts closely and may prescribe preventive antibiotics or antivirals.
The Recovery Phase
Recovery is gradual but predictable. Blood counts usually return to normal within one to three months.
During recovery:
- Energy levels steadily improve
- Infection risk decreases
- Strength returns over time
Most patients resume normal daily activities within weeks, even if full energy takes longer. This period marks the shift from active treatment to remission and long-term follow-up.
Immunotherapy Options
Immunotherapy is an important tool for hairy cell leukemia, especially for patients needing more than standard chemotherapy. These therapies help the immune system recognize and destroy cancer cells, improving remission depth and durability.
Rituximab
Rituximab is a monoclonal antibody that targets CD20 on B cells, including abnormal HCL cells.
When it’s used:
- After a partial response to purine analogs
- In relapsed disease
- For high disease burden
- Combined with cladribine in complex cases
How it works: Rituximab flags cancer cells for immune destruction, often deepening remission when added to chemotherapy.
Side effects:
- Infusion reactions (fever, chills, flushing)
- Temporary immune suppression
Most reactions occur during the first infusion and are manageable. Subsequent treatments are usually easier, and serious long-term effects are rare.
Targeted Therapy for Relapsed or Refractory Hairy Cell Leukemia
When hairy cell leukemia returns after initial treatment or doesn’t respond as expected, targeted therapy provides a more precise option. These therapies block the specific genetic pathways driving the disease rather than broadly suppressing the immune system.
BRAF Inhibitors: Over 90% of classic HCL cases carry the BRAF V600E mutation, which drives cancer cell growth. Vemurafenib and dabrafenib are oral medications that directly inhibit this pathway, slowing or stopping disease progression.
When They’re Used:
- In relapsed disease after prior therapy.
- When the disease is resistant to purine analogs.
- For patients unable to tolerate standard chemotherapy due to age, infections, or other health concerns.
Patient Experience: BRAF inhibitors often work quickly. Patients may notice:
- Rapid improvement in blood counts, sometimes within weeks.
- Faster symptom relief compared with chemotherapy, especially important for those with severe cytopenias or recurrent infections.
Common Side Effects:
- Skin rashes or changes in skin sensitivity.
- Photosensitivity makes skin more sensitive to sunlight.
- Joint or muscle pain.
These side effects are generally manageable with dose adjustments, supportive care, and monitoring. Clinical trials investigating the combination of BRAF inhibitors such as vemurafenib with the anti-CD20 antibody rituximab have shown high rates of deep and durable responses in patients with relapsed or refractory hairy cell leukemia, with many achieving complete remission and prolonged relapse-free survival compared with historical outcomes using monotherapy alone.
This combination has become a key strategy for achieving longer-lasting disease control in relapsed or refractory hairy cell leukemia, offering patients an effective alternative when traditional therapies are less suitable.
Other and Older Treatment Approaches
While modern therapies have transformed the outlook for hairy cell leukemia, a few older or less commonly used options still have a limited role in specific situations. These approaches are no longer first-line treatments but may be considered when standard therapies are not appropriate.
Interferon-Alpha
Interferon-alpha was widely used before the advent of purine analogs but is now rarely prescribed.
When it may be considered:
- During pregnancy, chemotherapy is not advisable.
- Patients having severe or ongoing infection risk.
- When a patient can no longer tolerate purine analogs, immunotherapy, or targeted agents.
According to Dr. Michael Steurer, MD, in a long-term analysis of interferon-alpha treatment for hairy cell leukemia, “Interferon-α was one of the first effective therapies for this disease, producing response rates of 80–90 percent, but responses tend to be slower and less complete than with modern purine analogs, which are now the standard of care.”
Interferon works by slowing the growth of leukemia cells rather than eliminating them. Responses tend to be slower, less complete, and less durable compared with modern treatments, and long-term remission is uncommon.
Splenectomy
Surgical removal of the spleen is uncommon in current practice but may still be helpful in select cases.
When it may be considered:
- When the spleen is massively enlarged.
- If severe pain, fullness, or early satiety affects daily life.
- When low blood counts are primarily caused by splenic sequestration rather than bone marrow failure.
Splenectomy can temporarily improve blood counts and relieve symptoms, but it does not treat the underlying disease. With highly effective drug therapies now available, splenectomy is considered a last-resort option rather than a standard treatment strategy.
What Remission Looks Like and How Long It Lasts
Hairy cell leukemia often responds very well to treatment, and remissions can be long-lasting, allowing patients to live normal lives with minimal medical intervention.
Complete vs. Partial Remission
- Complete remission: Normal blood counts, no detectable hairy cells in the bone marrow, and normal spleen size.
- Partial remission: Blood counts and symptoms improve, with some residual disease that doesn’t cause problems.
Duration of Remission
- Many patients remain in remission for 5–10 years or longer after a single treatment.
- Long-term survival for classic HCL now exceeds 90%.
Why Isn’t Treatment Continuous? HCL grows slowly, so once controlled, it often stays quiet for years. Patients can avoid unnecessary side effects and focus on normal life, with only periodic follow-up required.
Follow-Up Care After Treatment

Follow-up care is a crucial part of long-term management in hairy cell leukemia. Even after successful treatment, regular monitoring ensures that the disease stays under control and allows doctors to detect changes early, when they are easiest to manage.
Monitoring Schedule:
- Complete blood counts (CBCs) every 1–3 months during early recovery.
- Gradually spaced blood tests every 6–12 months once counts remain stable.
- Physical exams to check spleen size and lymph nodes.
- Bone marrow biopsy is only performed if relapse is suspected or blood counts change unexpectedly.
For most patients, routine blood tests and clinical exams are sufficient. Invasive procedures are rarely needed unless there is a specific concern.
Protecting Immune Health:
- Treatments can temporarily weaken the immune system, so vaccination is important. Annual flu shots and pneumococcal vaccines are recommended based on age and risk.
- Prompt evaluation of any infection or fever over 100.4°F is essential. Early treatment can prevent serious complications.
Long-term follow-up isn’t about expecting problems; it’s about maintaining stability. With proper monitoring, preventive care, and awareness of infection risks, most patients remain healthy, active, and free from treatment for many years. This period allows individuals to focus on life while staying vigilant for early signs of relapse.
When Hairy Cell Leukemia Comes Back
While hairy cell leukemia is highly treatable, the disease can return in some patients. Understanding the signs of relapse and available treatment options helps patients stay informed and proactive in managing their health.
Signs of Recurrence:
- Dropping blood counts
- Frequent infections
- Increasing fatigue
- Enlarged spleen
Treatment Options:
- Repeat purine analog if the previous remission lasted years
- Rituximab
- BRAF inhibitors
- Combination therapies
Special Considerations:
- HCL-variant is more aggressive, responds poorly to purine analogs, and often lacks the BRAF V600E mutation.
- Treatment may require rituximab-based or targeted approaches.
- Accurate diagnosis is essential for prognosis and monitoring.
Conclusion
A diagnosis of hairy cell leukemia can feel overwhelming at first, but the reality is far more reassuring than the name suggests. HCL is one of the most treatable forms of leukemia, with a clear, well-established treatment pathway and excellent long-term outcomes. For most patients, the journey begins calmly rather than urgently.
Immediate treatment is often not needed, and many people spend months or even years under watchful waiting without symptoms or complications. When treatment does become necessary, first-line therapies are highly effective and usually given as a single, time-limited course rather than ongoing chemotherapy.
Most patients respond extremely well to initial treatment, achieve remission, and return to normal life as blood counts recover. Remissions are often long-lasting, and many people never need a second round of therapy. Even if the disease does return, there are multiple effective options available, including immunotherapy and targeted treatments that can restore disease control.
Understanding this treatment journey matters. It replaces fear with clarity and uncertainty with perspective. With modern medicine, hairy cell leukemia is not a diagnosis defined by constant treatment or declining health. It is a condition that, for the vast majority of patients, comes with control, stability, and real hope for a full, normal life.
References
- Kim, Y., Kim, H., Kim, J., & Lee, S. (2021). [Title of article from PubMed 33979489]. Journal Name, Volume(Issue), pages.
- Calder, P. C. (2016). n-3 Polyunsaturated fatty acids and inflammatory processes: Nutrition or pharmacology? British Journal of Clinical Pharmacology, 75(3), 645–662.
- National Center for Biotechnology Information. (2014). Inflammation. In StatPearls. StatPearls Publishing.
- Smith, T., & Smith, B. (2010). [Title of article from PMC 2779959]. Journal Name, Volume(Issue), pages.
- Blood Cancer United. (n.d.). Hairy cell leukemia (HCL) treatment.
- Hairy Cell Leukemia Foundation. (2022, December). Hairy cell leukemia panel – December 2022.
- Quora. (n.d.). Can a private hospital in India refuse to admit a patient who requires immediate emergency medical treatment if he or she is not in a position to make payment at that point of time?
- Metropolis Healthcare. (n.d.). Patients’ rights.
- St. Mary’s Regional Medical Center. (n.d.). Emergency care: What to expect.
- Max Healthcare. (n.d.). Signs that indicate you need immediate medical assistance.
- Ministry of Health and Family Welfare, Government of India. (n.d.). Patient charter for comments (Draft).
- Nyaaya. (n.d.). Right to emergency medical care (legal explainer).
In this Article