Why Psoriasis Treatment Sometimes Needs to Change
Living with psoriasis is often a long journey of trial and discovery. It is a chronic inflammatory condition, and what works well at the beginning can sometimes lose effectiveness over time. If you have been following your routine faithfully but notice your symptoms creeping back, it may be time to ask yourself: when should you change your psoriasis treatment?
It is normal for both your body and your condition to change. Many people experience a reduced response to therapy over time, in which their immune system stops responding as well to the same treatment.
Others find that they have a flare of psoriasis despite treatment, in which the redness, itching, or scaling returns, even though medication or creams have not been changed. These are common signs and symptoms that may indicate your current psoriasis medication is not working quite as well as it has been.
Read More: What Is Nail Psoriasis? Symptoms, Causes, and Treatment Explained
How Psoriasis Treatment Works (Quick Refresher)
There are several reasons psoriasis treatments can stop working. Your skin may simply get used to the medication, or a shift in stress, diet, weather, weight, or infections may be setting off new flares.
Even newer treatments such as biologics, which zero in on specific parts of the immune system, can, over time, become less effective. If you think your biologic therapy isn’t helping as much anymore, or if your plaques are getting worse, you may want to talk with your dermatologist about switching treatments.
Knowing when to change your current psoriasis treatment can make a big difference in your condition. Persistent scaling, slowed healing, or relief after several weeks is considered a warning signal. If it feels like your skin is stuck in a flare-up and is again affecting daily life, this is a clear indication that you need to revisit your psoriasis management plan with a specialist.
The best next step is to talk with your dermatologist, rather than making changes or stopping medicines on your own. Getting professional guidance ensures you are not guessing what is going on. Your doctor may review your symptoms, adjust your dosage, suggest combination therapy, or guide you toward newer options that match your current needs.
Psoriasis can be a lifelong condition, but finding the right treatment rhythm helps you stay in control and closer to clearer, healthier skin.
Read More: Top 8 Psoriasis Creams: Soothing Skincare Solutions for Flare-Ups
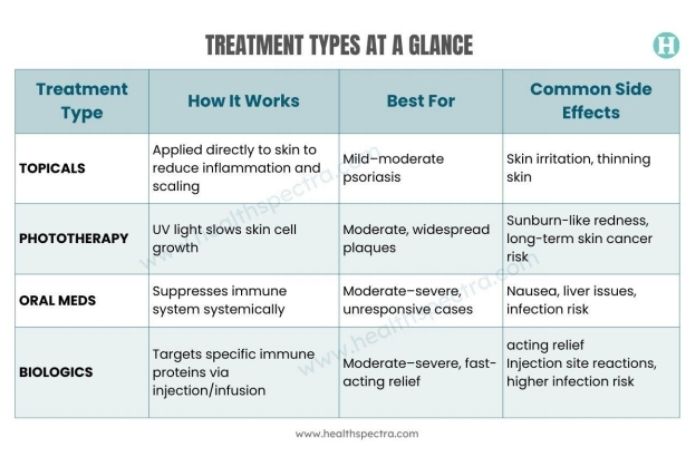
Treatment Types at a Glance
Here’s a quick visual breakdown of psoriasis treatment options to see how they stack up:
 Signs Your Psoriasis Treatment Is Not Working Anymore
Signs Your Psoriasis Treatment Is Not Working Anymore
Recognizing those red flags early will be your signal to rethink and speak with your dermatologist.

Your Symptoms Aren’t Improving
If, after many weeks or several months, your plaques still seem thick and rough, a given treatment may not be providing adequate benefit. When the redness, scaling, or itching hasn’t changed much despite consistent use of creams, light therapies, or systemic medications, something may be off.
Monitoring your skin with weekly photos or notes will help you and your doctor recognize whether progress has stalled.
Your Psoriasis Is Getting Worse
If plaques thicken, grow larger, or crop up in new places, that’s a sign your psoriasis is becoming more active. Even when you’re sticking to your regular routine, small patches can become large ones that may be constant, painful, and even cracked.
When you see psoriasis plaques worsening, it’s time to take action; ignoring it could be a sure sign that the prescription you’re using isn’t strong enough.
Frequent or Unpredictable Flares
Flares that are more frequent, appear rapidly, or last longer, even if you are using your medications properly, indicate that the current medical strategy is failing to control inflammation. If flare-ups persist without an evident cyclical pattern, this could indicate that your topicals, oral medications, or biologics are no longer effective in controlling it.
A symptom diary, including potential triggers related to stress, illness, or even weather changes, can be very informative for your dermatologist.
Side Effects Are Too Hard to Manage
Side effects should never feel worse than the condition you are treating. Other examples include skin thinning or visible blood vessels from long-term steroid creams, nausea or fatigue from oral medicines, or repeated infections and injection-site reactions with biologics.
If the downsides of treatment are impacting sleep, mood, or daily activities, this is a strong reason to revisit options. Often, safer alternatives, dose adjustments, or different treatment types are available.
You Need Larger or More Frequent Doses
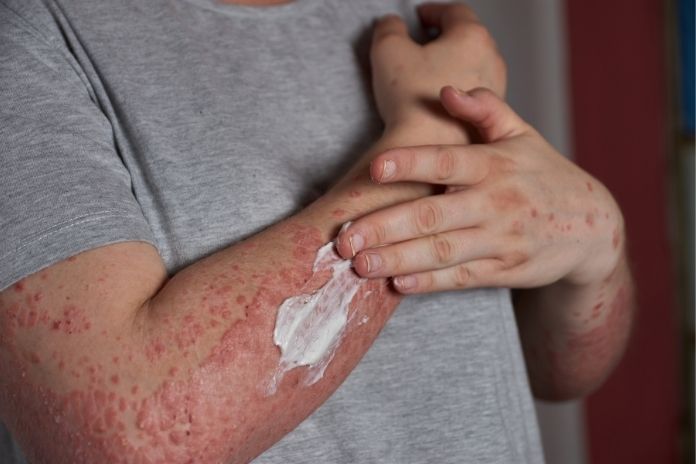
If the amount of medication that once controlled your symptoms needs to be increased time and again, your body may be responding less well to that treatment. Taking larger or more frequent doses on your own increases the risk of side effects, particularly with very potent topical steroids or systemic drugs.
Instead of taking matters into your own hands, discuss these changes with your dermatologist; they might switch you to a different medication or add another treatment.
Psoriasis Starts Interfering With Daily Life Again
When psoriasis awakens you in the middle of the night, restricts the clothes you can wear, makes you self-conscious about going out, or slows you down at work or in the gym, it means your plan is no longer working.
Itching, pain, and visible plaques can be just as damaging to confidence and emotional well-being as they are to the skin. If the disease feels like it is “out of the box” and calling the shots in your life once more, it is time to revisit your psoriasis management plan with your doctor.
New Symptoms Develop
New symptoms, such as joint pain, morning stiffness, swollen fingers or toes, or changes in your nails, may indicate that you are developing psoriatic arthritis or that your pattern of disease is changing. Nail pitting, thickening, or separation from the nail bed, and even resistant scalp psoriasis, are also potential warning signs that your condition is changing.
These symptoms need to be evaluated quickly, so your dermatologist or rheumatologist can adjust your treatment and help you avoid long-term complications.
Read More: 15 Stress Management Tips For Psoriasis – Know The Details
Why Psoriasis Treatments Stop Working
Treatments rarely fail overnight. Knowing why they lose their punch helps you and your doctor stay one step ahead.

Your Body Develops Treatment Resistance
Over time, the immune system can become accustomed to some biologics and systemic drugs. When this occurs, the same dose that was once effective may no longer adequately control plaques and inflammation.
If your psoriasis is slowly returning despite proper use of your medications, your dermatologist may suspect a diminished response and recommend an alternative drug, another biologic target, or combination therapy.
Incomplete Adherence
Missing doses, using topicals irregularly, or stopping treatment when skin looks better can all make psoriasis seem resistant, even when in fact the medicine itself is effective. Life can get busy, and it’s easy to forget applications or appointments, especially with routines like phototherapy that require regular visits.
Simple tools-reminders on your phone, a checklist, or setting treatments at the same time each day-can improve consistency and may restore your results without needing a new prescription.
Worsening Triggers
Common triggers like stress, smoking, alcohol, cold and dry weather, infections, or some medicines may overpower your treatment. A trigger that previously caused only mild flares may, at times, provoke more intense or more frequent outbreaks.
Also, discussing with your healthcare professional lifestyle issues, such as sleep, stress management, quality diet, smoking, and alcohol consumption, could help alleviate this burden and further support your current treatment.
Disease Progression
Psoriasis is not always a stationary condition. In some patients, it can progress from mild to moderate or severe over time, with plaques spreading, thickening, or affecting more sensitive areas like the face, hands, or genitalia. Psoriatic arthritis can also develop, leading to joint pain and stiffness associated with skin symptoms.
As the disease progresses, treatments that were initially effective may become inadequate, necessitating an upgrade to more robust options or targeted therapies.
Medication Interactions
It is not uncommon for new medications, over‑the‑counter drugs, or herbal supplements to interfere with psoriasis medicines. Some medicines can make systemic and biologic therapies less effective or even increase the risk of side effects.
Always inform your dermatologist and pharmacist of any new tablets, injections, or supplements you start. They can check for interactions and adjust your plan before problems arise.
Read More: Top 5 Best Foods to Cure Psoriasis
When to Talk to Your Dermatologist About Switching Treatment

Do not wait until it is a dominant factor in your everyday life, and be brave enough to ask for assistance. Knowing when to switch your psoriasis medication starts with understanding when to involve your dermatologist.
Call if there is no improvement or only a slight improvement after about 8–12 weeks of regular use, unless your doctor has mentioned otherwise. Most topical, light-based, and systemic treatments demonstrate at least some improvement within that time.
If flares continue to occur even with proper use, consult your dermatologist. Recurring flare-ups may indicate underlying problems such as decreased responsiveness, more potent triggers, and disease progression.
Seek urgent help if symptoms suddenly worsen, plaques spread quickly, become very painful, or new areas, such as the face, nails, or joints, are affected.
If any of the following side effects are problematic to manage, speak up: persistent irritation, stomach upset, fatigue, frequent infections. Often, safer or better‑tolerated alternatives are available.
For long-term control with fewer flares, talk to your doctor about biologics or combination therapy. These are usually considered for moderate to severe disease or when other options have not worked well.
Never stop, reduce, or switch your psoriasis medication on your own; your dermatologist must guide any dose or drug change to keep you safe and maintain control of the disease.
Read More: How to Manage Psoriasis With Essential Oils
Final Summary
Final Psoriasis treatment can also become less effective over time due to reduced response, lifestyle triggers, medication interactions, or natural disease progression. When plaques worsen, flares become more frequent, side effects become harder to tolerate, or daily life is disrupted, it is a sign that your current plan may need changing.
A thorough re-evaluation by a dermatologist helps identify the cause, review how you are using your medicines, and decide whether to adjust doses, add combination therapy, or switch to more advanced options such as biologics.
Early, proactive changes support better long-term skin health, comfort, and confidence. Track symptoms, snap photos, and book that visit today.
Read More: Top 7 Psoriasis Shampoos: Gentle Hair Care Products for Scalp Relief
References
- American Academy of Dermatology. (n.d.). Psoriasis clinical guideline. American Academy of Dermatology.
- American Academy of Dermatology. (n.d.). How long will I have to treat my psoriasis? American Academy of Dermatology.
- Mayo Clinic Staff. (2025, February 21). Psoriasis: Diagnosis and treatment. Mayo Clinic.
- Mayo Clinic Staff. (2025, February 21). Psoriasis: Symptoms and causes. Mayo Clinic.
- DermNet NZ. (2024, September 28). Guidelines for the management of psoriasis. DermNet New Zealand.
- National Health Service. (2025, July 29). Psoriasis – Treatment. NHS.
- International Psoriasis Council. (n.d.). Disease severity. International Psoriasis Council.
- James, W. D., Elston, D. M., Treat, J. R., Rosenbach, M. A., & Neuhaus, I. M. (2023). Psoriasis. In MSD manual professional edition. Merck Sharp & Dohme LLC.
- BMJ Best Practice. (n.d.). Psoriasis. BMJ Publishing Group.
- Slevin, S. M., Murphy, M., & O’Donnell, D. F. (2017). Diagnosis and management of psoriasis. Prescriber, 28(5), 29–37.
- Klopotowska, D., Reich, A., & Szepietowski, J. C. (2021). Current treatment of psoriasis: An interdisciplinary approach. Advances in Dermatology and Allergology, 38(4), 563–573.
- Khosravi, H., et al. (2023). Systemic treatment of psoriasis: A review of new and emerging therapies. Dermatology and Therapy, 13(2), 345–366.
- Vilar-Alejo, J., et al. (2024). Long-term effectiveness and safety of biologics in psoriasis: Real-world evidence. Journal of Clinical Medicine, 13(5), 1234.
- Menter, A., Strober, B. E., Kaplan, D. H., Kivelevitch, D., Prater, E. F., Stoff, B., Armstrong, A. W., Connor, C., Cordoro, K. M., Davis, D. M. R., Elewski, B. E., Gelfand, J. M., Gordon, K. B., Gottlieb, A., Kavanaugh, A., Kiselica, M., Korman, N. J., Kroshinsky, D., Lebwohl, M., … Hariharan, V. (2019). Joint American Academy of Dermatology–National Psoriasis Foundation guidelines of care for the management and treatment of psoriasis with topical therapy and alternative medicine modalities for psoriasis severity measures. Journal of the American Academy of Dermatology, 80(4), 1029–1072.
- Elmets, C. A., Leonardi, C. L., Davis, D. M. R., Gelfand, J. M., Lichten, J., Mehta, N. N., Armstrong, A. W., Connor, C., Cordoro, K. M., Elewski, B. E., Gordon, K. B., Gottlieb, A., Kavanaugh, A., Kiselica, M., Korman, N. J., Kroshinsky, D., Lebwohl, M., Young, M., Van Voorhees, A. S., … Hariharan, V. (2021). Joint American Academy of Dermatology–National Psoriasis Foundation guidelines of care for the management and treatment of psoriasis with awareness and attention to comorbidities. Journal of the American Academy of Dermatology, 84(2), 433–462.
- Mahajan, R., et al. (2023). Systemic treatment of psoriasis in special populations. International Journal of Dermatology, 62(10), 1234–1248.
- Smith, C. H., et al. (2025). Emerging systemic therapies for moderate-to-severe psoriasis: An updated review. Expert Opinion on Pharmacotherapy, 26(2), 145–160.
- Dupire, G., et al. (2024). Comparative effectiveness of systemic treatments for chronic plaque psoriasis: A real-life cohort study. Annales de Dermatologie et de Vénéréologie – FMC, 151(2), 85–94.
- Svedbom, A., Dalén, J., Mamolo, C., Cappelleri, J. C., Petersson, I. F., & Ståhle, M. (2016). Treatment patterns with topical therapies in psoriasis: A Swedish database analysis. Journal of Managed Care & Specialty Pharmacy, 22(4), 396–404.
- Dogra, S., & Mahajan, R. (2016). Systemic treatment of psoriasis in special population: A review. Indian Journal of Dermatology, Venereology and Leprology, 82(4), 381–392.
In this Article





















