Acid reflux may act up after consuming certain foods that can cause the lower esophageal sphincter (LES) to relax, slow down digestion, or put additional pressure on the stomach. Trigger foods vary from one individual to another.
Hence, it is important to look for common patterns between what you eat and how your body responds.
Why Food Triggers Acid Reflux
Reflux of stomach acid into the esophagus happens when the LES relaxes or weakens, allowing acid to move upward and cause a burning sensation in the chest or heartburn.
A large meal can raise pressure inside the stomach and push acid into the esophagus and chest. Tight clothing around the waist can add extra pressure on the stomach and worsen symptoms.
Certain foods can slow stomach emptying or stimulate more acid production. For this reason, an acid reflux diet focuses on both what you eat and how you eat it.
Read more: The Link Between Acid Reflux and Breathing Patterns
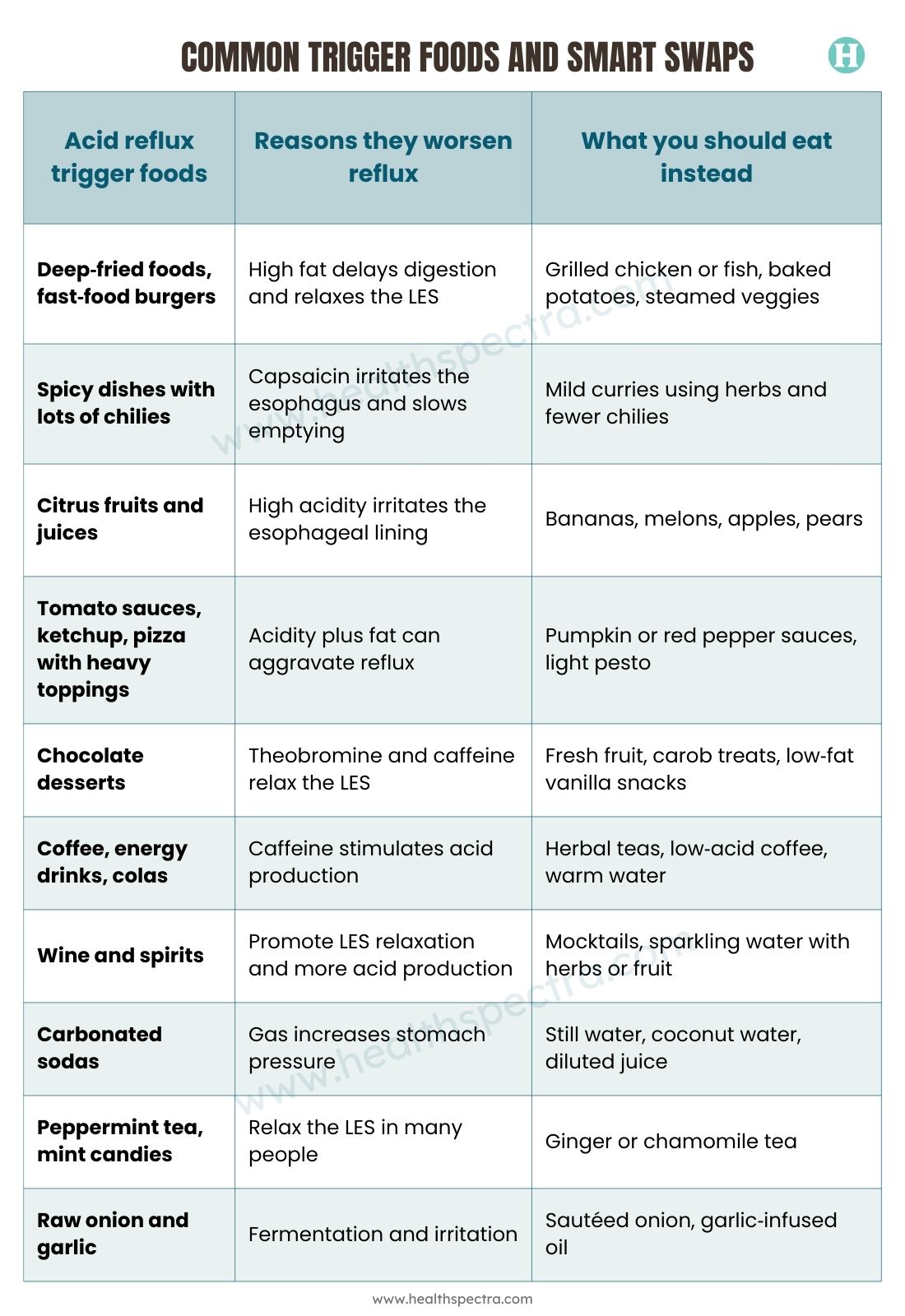
Foods Which Can Trigger or Worsen an Acid Reflux Problem

Fatty & Fried Foods
These foods cause delayed stomach emptying and promote LES relaxation, making them classic foods that cause acid reflux. Examples include fast‑food burgers, deep‑fried snacks, creamy sauces, and rich gravies.
Healthier alternatives include grilled or baked chicken or fish, steamed vegetables, and soups made with vegetable broth instead of cream.
Spicy Foods
Chili peppers contain a compound called capsaicin that can irritate the esophageal lining and slow stomach emptying, adding to reflux discomfort.
However, spice tolerance varies from individual to individual. Therefore, not everyone needs to avoid all spicy dishes that may trigger acid reflux.
Switch to milder flavors like basil, oregano, coriander, and a pinch of black pepper instead of extremely hot chilies.
Citrus Fruits and Juices
Oranges, grapefruits, and lemons are highly acidic and often appear on GERD trigger‑food lists.
They can cause burning, sour, and unpleasant sensations, especially when eaten on an empty stomach.
Choose non‑citrus fruits such as bananas, melons, apples, and pears, which are gentler on the esophagus in an acid reflux diet.
Tomatoes & Tomato-Based Products
Tomatoes and products such as ketchup, pasta sauce, and salsa are acidic and commonly listed as foods that may trigger acid reflux symptoms.
Combining tomato sauces with high‑fat ingredients like cheese or processed meats can further increase reflux risk.
Roasted red peppers, pumpkin or carrot‑based sauces, or light pesto can serve as flavourful alternatives.
Chocolate
Chocolate contains theobromine and caffeine, which can relax the LES and encourage reflux episodes.
Even small amounts can act as acid reflux trigger foods for people who experience frequent GERD.
Try carob‑based desserts, fruit with a spoonful of low‑fat yogurt, or low‑fat vanilla pudding instead.
Coffee and Caffeinated Beverages
Caffeine stimulates gastric acid secretion and can contribute to heartburn.
Coffee may still cause symptoms even in decaffeinated form, likely because other compounds also affect the LES.
More reflux‑friendly drinks include herbal teas such as ginger or chamomile, low‑acid coffee, and warm water.
Alcohol
Alcohol relaxes the LES muscles and can stimulate excess stomach acid, making it another common GERD trigger.
Research suggests a stronger association between reflux and wine or spirits as compared to small amounts of beer.
Opt for alcohol‑free mocktails, sparkling water with herbs or fruit slices, or buttermilk when possible.
Carbonated Drinks
Sodas and other carbonated beverages create bubbles that increase pressure in the stomach, pushing acid upward.
Even sugar‑free varieties can worsen reflux, because not sugar but the carbonation is the main issue.
Still water, coconut water, or diluted non‑citrus juices are better choices when deciding what to drink with acid reflux.
Mint and Peppermint
While mint can soothe digestion for some people, it may relax the LES and act as a hidden reflux trigger.
Strong peppermint teas, candies, and after‑dinner mints can worsen nighttime heartburn.
Choose ginger, chamomile, or fennel tea, which are soothing and more reflux‑friendly.
Onions and Garlic (Raw)
Raw onions and garlic can ferment in the gut, increasing gas and pressure that push acid upward.
They may also irritate the esophageal lining, making them foods to avoid during acid reflux flare‑ups.
Well‑cooked onions, garlic‑infused oil, or flavoring with celery, leeks, and chives can add taste with fewer symptoms, if tolerated.
Read More: Can Acid Reflux Lead to More Serious Health Issues? What You Should Know
Foods for a Reflux‑Free Life

Proteins
Lean poultry and fish, as well as trimmed meats, provide protein without the heavy fat that worsens reflux.
Egg whites and plant proteins such as tofu, beans, and lentils, if tolerated, are also good options in an acid reflux diet.
Carbohydrates
Oatmeal and other whole‑grain breakfast foods have high water and fiber content, which can help absorb stomach acid and keep you full without excess fat.
Brown rice, quinoa, and whole-grain breads or rotis without oily toppings are generally gentle alternatives to common GERD trigger foods.
Fruits and Vegetables
Non‑citrus fruits and well‑cooked vegetables offer plenty of fiber, which supports healthy digestion and weight management, both important for reflux control.
Leafy greens, carrots, beans, and pumpkin are usually safer than fried or heavily spiced vegetable dishes.
Healthy Fats
Small amounts of olive oil, flaxseed oil, or canola oil provide beneficial fats without overfilling the stomach.
Avocado, eaten in moderation, can be part of what to eat for acid reflux. Although, large portions may cause trouble to some people.
Read More: Acid Reflux vs. Heart Attack: How to Tell the Difference
How You Eat Matters Too

- Eating large, heavy meals makes the stomach work harder and raises pressure,
- Eat smaller, more frequent meals, as it can ease acid reflux symptoms.
- Finishing dinner at least 2-3 hours before bedtime and skipping late‑night snacks helps prevent nighttime reflux.
- Eating slowly, chewing food thoroughly, and staying upright after meals gives the stomach time to empty and reduces backflow.
Common Myths About an Acid Reflux Diet
- Not all acidic foods automatically cause reflux. Some people tolerate small portions of tomatoes or citrus when other factors are well controlled.
- Spicy foods aren’t universally harmful, and extremely bland diets can be hard to follow. Find what works best for you through trial and error.
- Milk may briefly soothe burning, but full‑fat milk can later stimulate acid secretion and may worsen symptoms for some.
When Diet Changes Aren’t Enough
- More than two heartburn episodes per week, nighttime choking, or difficulty swallowing may signal chronic GERD rather than food intolerance.
- Chronic reflux can lead to complications such as esophagitis or Barrett’s esophagus. Hence, persistent symptoms should always be checked by a doctor.
- A healthcare provider can review medications, test for conditions including H. pylori, and recommend treatments such as acid-suppressing medicines if needed.
Read More: How Yogurt Can Help Soothe Your Acid Reflux Naturally
Final Takeaway
Often, foods that trigger acid reflux share features such as high fat content, acidity, carbonation, caffeine, or the ability to relax the LES. Tracking your personal trigger foods and focusing on lean proteins, whole grains, non‑citrus fruits, and cooked vegetables makes it easier to maintain a reflux‑friendly diet.
Substituting better options for trigger foods and consulting a doctor if symptoms persist is the best way to support long‑term esophageal health.
References
- Newby, F. D., & Newby, D. E. (2017). Foods inducing typical gastroesophageal reflux disease symptoms. PMC
- Bansal, N., & Bansal, A. (2023). Functional food in relation to gastroesophageal reflux disease. PMC.
- Nilsson, M., & Tarp, J. (2021). Dietary intake in relation to the risk of reflux disease. PMC.
- Yazbek, E., & Yazbek, T. (2021). Elimination of dietary triggers is successful in treating symptoms. PubMed.
- Khan, M., & Khan, A. (2025). Natural products in the management of gastroesophageal reflux. PMC.
- Yazbek, E., et al. (2023). Dietary factors involved in GERD management. ScienceDirect.
- Yazbek, E., et al. (2023). The relationship of gastroesophageal reflux with nutritional habits. ScienceDirect.
- Bansal, N., et al. (2023). Current complementary and alternative therapy. PMC.
- ClinicalTrials.gov. (2025). Prevalence of GERD, its effect on. ClinicalTrials.gov.
- National Center for Complementary and Integrative Health. (2023). Gastroesophageal reflux disease (GERD) and complementary health approaches.
- Yazbek, E., et al. (2023). Dietary factors involved in GERD management. PubMed.
- Nilsson, M., et al. (2019). The role of diet in the development and management of gastroesophageal reflux disease. PMC.
- Nilsson, M., et al. (2018). Are diet and micronutrients effective in treating gastroesophageal reflux disease? PMC.
- Yazbek, E., et al. (2017). Food and gastroesophageal reflux disease. PubMed.
- Katz, P. O., et al. (2025). Gastroesophageal reflux disease (GERD). NCBI Bookshelf.
- National Institute of Diabetes and Digestive and Kidney Diseases. (2025). Eating, diet, & nutrition for GER & GERD.
In this Article