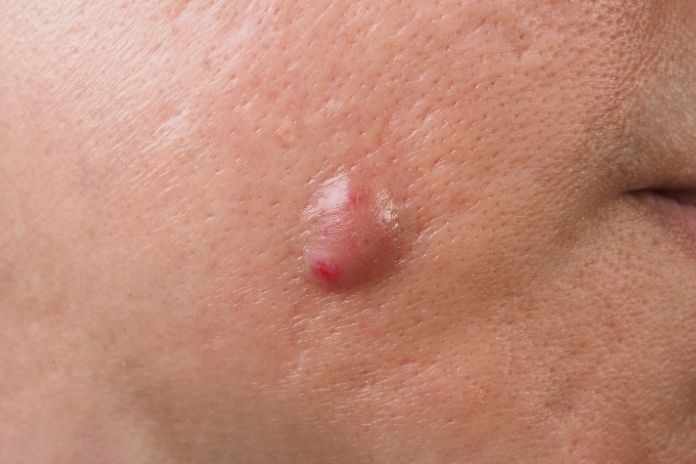
A painful boil heals, then weeks later, another forms on the neck, back, or thighs. Carbuncles are more than frustrating skin bumps; repeated outbreaks can signal underlying health issues or continual exposure to bacteria such as Staphylococcus aureus.
This guide examines the causes of recurring carbuncles, the major risk factors, and effective methods for prevention and chronic carbuncle treatment.
What Is a Carbuncle?

A carbuncle is a cluster of deep, red, swollen, pus-filled lesions originating from infected hair follicles. In contrast to a simple boil or furuncle, a carbuncle may be much larger and more painful, and it can cause fever or even fatigue if the infection has spread throughout the body.
The most common cause is a recurrence of staph infection, since Staphylococcus aureus (“staph”) naturally resides on the skin, nose, and throat of many people. If cuts, shaving, or friction compromise the skin barrier, staph bacteria invade, causing clusters rather than single boils.
Read More: Allergic to Touch? Understanding Dermatographia (Skin Writing Hives)
Why Do Carbuncles Keep Coming Back?
Recurrent carbuncles, also called chronic carbuncles, seldom occur by chance. To understand why carbuncles recur, one must consider bacterial persistence, immune defenses, and daily habits.
1. Persistent Staphylococcus aureus (Including MRSA) Colonization
Staph bacteria are stealthy residents of the skin and nasal passages. About one-third of people carry them persistently, while many more are intermittent carriers. These bacteria can bind tightly with nasal cells, sometimes lurking in deeper layers and evading both immune defenses and surface treatments.
As long as staph or MRSA remains in these reservoirs, it can regularly re-infect the skin, especially after small injuries or abrasions. MRSA skin infection recurrence is especially concerning, since this strain resists common antibiotics and topical treatments.
Identifying persistent carriers through nasal or wound swabs enables more effective decolonization of staph infections, including medical protocols that target these deeper reservoirs.
2. Compromised Immunity
The body’s natural defenses against infection—including carbuncles—depend on the immune system. Conditions such as diabetes mellitus, kidney disease, HIV, and even chronic stress, poor rest, or nutrition, put a dent in immunity.
A weakened immune response invites bacterial overgrowth after minor skin cuts, leading to more frequent or severe outbreaks. Underlying immune disorders need to be addressed in chronic carbuncle treatment, treating not just the infection but also strengthening a person’s immunity.
3. Poor hygiene or re-exposure to contaminated items
Personal care and household hygiene also play a more critical role in carbuncle risk factors than most people realize. The use of unwashed towels, bed linens, or razors just prolongs the life of bacteria that can reinfect the skin.
Shared items in homes, gyms, and hostels greatly heighten this risk. At the same time, the frequently touched surfaces of door handles and exercise equipment may also house the same bacteria responsible for recurrent infections. Prevention requires frequent washing and disinfection of all such items, and not sharing personal care tools.
4. Skin Friction, Sweat, and Micro-Injuries
Carbuncles are usually clustered boils that appear in areas of the body where the skin is exposed to day-to-day friction, such as tight clothing, backpacks, belts, or repetitive shaving. This area normally sweats and gets irritated; hence, it becomes very easy for the germs to enter, especially in the warm and moist regions like armpits, neck, buttocks, and thighs.
These minor injuries compromise protective skin barriers and allow staph bacteria to enter, where they multiply rapidly. Carbuncle prevention tips emphasize reducing such friction and keeping the affected areas clean and dry.
5. Presence of Skin/Hormonal Conditions
Acne, eczema, and dermatitis can obstruct hair follicles and trap bacteria, creating the perfect environment for recurrent carbuncles. Hormonal fluctuations during puberty, PCOS, menopause, or pregnancy increase oil and perspiration, thereby providing more food for bacterial growth and inflammation.
The management of these skin and hormonal changes is an essential feature of both prevention and chronic carbuncle treatment.
Read More: Hard Lump Under the Skin: Causes, Diagnosis, and When to Worry
Risk Factors That Predispose Some Individuals to Developing Recurring Carbuncles
Understanding the risk factors for carbuncles helps in effective prevention and focused treatment strategies. Some critical risks include the following:
- Diabetes mellitus: High blood sugar supports bacterial growth, delays the healing process, and impairs immune responses, making carbuncles more prone to recurrence.
- Obesity: Increased skin folds, friction, and sweating all favor the proliferation of staph.
- Weakened immune system: Various diseases (HIV, kidney disease) or medications such as steroids reduce resistance to infection.
- Close contact environments: Shared housing, gyms, military, or dormitory situations are conducive to staph transmission.
- Occupations that involve skin trauma may expose skin to continuous nicks, cuts, and abrasions, as with factory work, cleaning, and construction.
- Poor wound care or incomplete antibiotic courses: Not allowing the wound to heal completely or stopping antibiotics too early leaves bacteria to reinfect the skin.
Addressing these risk factors forms the basis for breaking this cycle and safeguarding against the recurrence of staph infection.
Read More: 5 Skincare Products You Should Never Use on Sensitive Skin
How to Avoid Recurrence of Carbuncles

Prevention is multifaceted. The following carbuncle prevention tips are evidence-based and supported by dermatologists and infectious disease specialists.
1. Enhancing Skin Hygiene
- Bathe daily with antibacterial or antiseptic washes (chlorhexidine, benzoyl peroxide).
- Keep the skin clean and dry; gently exfoliate areas prone to friction.
- Wash your hands before and after touching infected areas.
- This helps eliminate bacteria before they invade the follicles, which is important for preventing recurrent carbuncles.
2. Eliminate Re-Exposure to Bacterial Sources
- Wash all fabrics (sheets, towels, clothes) in hot water regularly.
- Never share razors, towels, or grooming tools.
- Disinfecting high-contact surfaces, such as door handles and gym equipment, can reduce microbial reservoirs.
- Environmental cleanliness disrupts the cycle of reinfection.
3. Address Nasal Staph Colonization
- Physicians may recommend topical mupirocin (Bactroban) for application to the nares to eliminate staph carriage.
- For MRSA skin infection recurrence, a short course of decolonization combines nasal ointment and antiseptic skin washes.
- Medical tests confirm the presence of persistent staph or MRSA colonization in a person and create a basis for proper treatment.
4. Fortify Your Immune System
- Immunity is supported by balanced nutrition, hydration, stress management, and adequate sleep.
- Chronic illnesses such as diabetes require effective management.
- Avoid smoking since it impairs wound healing and immune function.
- Improved immunity protects against recurrent carbuncles.
5. Handle Skin Gently
- Wear loose, breathable clothing to minimize friction and keep skin dry.
- Never squeeze boils, as this can force the infection deeper or spread bacteria.
- Use clean razors or electric grooming tools to reduce the number of micro-injuries.
- Gentle care of skin barriers prevents chronic needs for carbuncle treatment.
6. Seek Professional Help for Recurrent Cases
- If outbreaks recur, consult a dermatologist or an infectious diseases specialist to obtain cultures and perform resistance testing.
- A whole family and household evaluation may be necessary if MRSA is identified.
- Chronic or widespread carbuncles may need oral antibiotics, specific topical therapies, or medical decolonization to break the cycle.
These strategies cover immediate and long-term approaches to preventing recurrent carbuncles and staph infections.
Read More: Toilet Infections: Types, Symptoms, Prevention, and Treatment
When to Seek Medical Care
Early assessment by a healthcare professional will avoid severe complications and restore skin health. Consult a doctor if:
- You have recurring carbuncles: three or more episodes in a year
- Bumps are accompanied by fever, spreading redness, or swollen lymph nodes.
- The lesions are large and painful, and will not drain or heal.
- Infections remain despite good hygiene and medication.
- You have a chronic medical condition, such as diabetes or an immune disorder.
A specialist can provide cultures, guide chronic carbuncle treatment, and recommend decolonization for staph infections or MRSA skin infection recurrence.
Read More: Skin Cycling: The Skincare Trend Revolutionizing Your Routine
Quick Recap: How to Break the Cycle of Recurring Carbuncles
Carbuncles tend to recur due to bacterial persistence, poor hygiene, friction, or impaired immunity. Hygiene, decolonization, immune support, and medical follow-up are all part of a multi-step regimen in chronic carbuncle treatment.
Most individuals should be able to minimize flare-ups considerably with regular, proactive care and recognition of their own risk factors. Taking care of one’s skin is not just about treating the boils as they appear, but also breaking that deeper cycle that allows them to keep coming back.
Read More: 5 Types of Infections That You Must Know in Detail
References
- https://www.ncbi.nlm.nih.gov/books/NBK554459
- https://my.clevelandclinic.org/health/diseases/15153-boils-and-carbuncles
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3934592
- https://www.webmd.com/skin-problems-and-treatments/carbuncles-causes-treatments
- https://patient.info/doctor/dermatology/boils-and-carbuncles
- https://www.healthline.com/health/carbuncle
- https://www.kauveryhospital.com/nightingale/a-case-report-on-carbuncle
- https://www.mayoclinic.org/diseases-conditions/boils-and-carbuncles/symptoms-causes/syc-20353770
- https://www.clinikally.com/blogs/news/risk-factors-and-prevention-tips-for-carbuncles
- https://www.sciencedirect.com/science/article/pii/S1572100019305630
- https://www.healthline.com/health/recurring-boils
- https://medlineplus.gov/ency/article/000825.htm
- https://www.mayoclinic.org/diseases-conditions/boils-and-carbuncles/diagnosis-treatment/drc-20353776
- https://www.msdmanuals.com/professional/dermatologic-disorders/bacterial-skin-infections/furuncles-and-carbuncles
- https://www.sciencedirect.com/topics/pharmacology-toxicology-and-pharmaceutical-science/carbuncle
- https://www.ncbi.nlm.nih.gov/books/NBK513141
In this Article