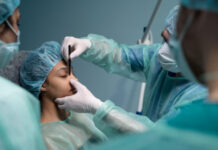
Nasal polyps rarely show up in childhood, and that’s exactly why doctors take them seriously when they do. These soft, teardrop-shaped growths form when the lining of the nose or sinuses stays inflamed long enough for the tissue to swell, collect fluid, and bulge outward.
In adults, this is common. A retrospective pediatric study noted: compared to adults … the frequency [of nasal polyps] in children younger than 10 years old is estimated at 0.1 %. That low number is a signal. When polyps appear in young patients, there’s often a deeper issue driving them, like cystic fibrosis, primary ciliary dyskinesia, or an immune system disorder.
Here’s what this really means for parents: when your child can’t breathe well, everything downstream suffers, sleep, appetite, energy, mood, school performance, and even long-term facial growth. Kids don’t always know how to describe what they’re feeling, so the symptoms can simmer quietly for months before anyone realizes something’s off.
That’s why understanding the causes, symptoms, diagnostic process, and treatment options makes a real difference. This guide walks you through everything with clarity, not alarm, not vague explanations, just evidence-based information that helps you make the right decisions for your child.
Quick Summary: What You’ll Learn
You’ll get a clear understanding of:
- What nasal polyps actually are, and why they behave differently in children.
- Pediatric-specific causes and risk factors.
- Symptoms that parents often miss.
- How ENTs diagnose polyps in kids.
- Treatment options and medication and surgery.
- Long-term management and when to call a specialist.
If your child has chronic nasal symptoms, this guide gives you the groundwork to talk confidently with your pediatrician or ENT.
Understanding Nasal Polyps in Children: What’s Different?

Nasal polyps in children are rare but important to notice. These soft growths develop when chronic inflammation causes the nasal lining to swell and retain fluid. Unlike adults, pediatric polyps often indicate an underlying systemic issue or persistent sinus problem.
Early detection is crucial because blocked airflow can affect breathing, sleep, and even facial growth. Understanding the types, causes, and implications helps guide timely treatment and prevent long-term complications.
Anatomy and Pathophysiology in Kids
Nasal polyps form when chronic inflammation causes the mucosal lining to swell, retain fluid, and gradually protrude into the nasal passage. This inflammatory cycle is well described in ENT literature, including the pediatric overview in Medscape.
In children, though, this process is much less common. Adults have structural, allergic, and inflammatory triggers that frequently repeat throughout life. But a young child has fewer years of exposure, which is why pediatric ENTs immediately look for systemic factors, or at least persistent ones, when polyps show up.
The few children who do develop them often have long-standing sinus inflammation, chronic infections, or a genetic condition affecting mucus, immunity, or ciliary function. Because pediatric sinuses are still developing, ongoing obstruction can also affect facial growth and airway development.
The Common Pediatric Polyp Types
Kids generally present with two main categories:
1. Multiple Bilateral Polyps
When polyps grow on both sides of the nose, doctors suspect systemic disease. These polyps look similar to the adult pattern, but because the incidence in childhood is so low, bilateral disease almost always leads to a deeper medical evaluation.
2. Antrochoanal Polyps
These are more common in children than in adults. Antrochoanal polyps start in the maxillary sinus and extend backward into the nasopharynx. They tend to be larger, unilateral, and don’t usually indicate systemic illness, but they do cause significant blockage.
A review in MDPI Diagnostics (as part of an article on nasal polyp endotypes) lists midline congenital defects, such as dermoid cysts, gliomas, meningoencephaloceles, and benign tumors, among pediatric differential diagnoses.
Why Early Onset Matters
Early appearance almost always raises suspicion of systemic disease. A cross‑sectional study in JAMA Otolaryngology found that about 50% of children with cystic fibrosis had sinonasal polyposis. Primary ciliary dyskinesia also increases risk because mucus stagnation leads to repeated infections.
Why this matters: a child’s airway, sleep cycle, and craniofacial growth depend on steady airflow. Chronic obstruction affects everything from appetite to school performance. Long-term inflammation also increases the likelihood of recurrent infections and repeated treatment cycles.
Read More: Nasal Breathing vs. Mouth Breathing: Which Is Better for Your Health?
Causes and Risk Factors of Nasal Polyps in Children

Nasal polyps in children are uncommon, and when they occur, they usually signal something beyond routine sinus irritation. Understanding what triggers these growths is crucial for early detection, targeted treatment, and preventing long-term complications.
Causes can be broadly divided into underlying systemic conditions, chronic inflammation, and environmental or genetic factors.
- Underlying Systemic Conditions: Pediatric polyps often point to systemic issues that affect mucus clearance, immunity, or sinus function.
- Cystic Fibrosis (CF): CF alters the consistency of mucus throughout the respiratory system, making it thick and sticky. This clogs the sinuses, leading to chronic inflammation and, eventually, polyps. ENTs typically screen for CF in children with bilateral polyps, especially if symptoms appear early.
- Primary Ciliary Dyskinesia (PCD): In PCD, the tiny cilia that normally clear mucus don’t work properly, resulting in backup, repeated infections, and chronic sinus inflammation. Polyps can form as a secondary consequence.
- Immunodeficiency Disorders: Children with weakened or malfunctioning immune systems are more susceptible to recurrent sinus infections. Repeated inflammation from these infections increases the likelihood of polyp formation.
- Chronic Upper Airway Inflammation:Polyps often coexist with chronic inflammatory conditions, reflecting the interconnected nature of the nose, sinuses, and lungs.
Common contributors include:
- Allergic Rhinitis– Triggers inflammatory responses in the nasal tissue.
- Asthma– Linked to similar inflammatory pathways as sinus disease.
- Chronic Rhinosinusitis (CRS)– Persistent sinus inflammation is both a cause and effect of polyps.
ENT pathology data also show that in children with CRS, eosinophils and mast cells, key cells in allergic inflammation, are increased in both sinus and bronchial tissues of asthmatics, suggesting common inflammatory mechanisms.
Read More: 6 Breathing Exercises To Fight Asthma- A Natural Relief and Normal Breath
- Environmental and Genetic Factors:Even in the absence of systemic disease, certain environmental and genetic factors increase risk:
- Persistent exposure to pollutants and passive smoke.
- Anatomical factors, such as narrow sinus passages.
- Genetic variations affecting mucosal immunity.
According to a 2023 MDPI study, “Endotypes of Nasal Polyps in Children,” the authors found that genetic and systemic factors, including cystic fibrosis, primary ciliary dyskinesia, and immunodeficiencies, often underlie pediatric nasal polyp development.
Children are at higher risk for nasal polyps if they have:
- History of asthma or allergies.
- Chronic rhinosinusitis.
- Cystic fibrosis or PCD.
- Ongoing exposure to irritants (smoke, pollution).
- Family history of sinus disease.
- Older age or adolescence (incidence rises slightly, but still much lower than in adults).
Recognizing these risk factors early helps pediatricians and ENT specialists evaluate children promptly, ensuring the underlying cause is addressed, and airflow, sinus health, and overall development are preserved.
Recognizing Symptoms of Nasal Polyps in Children

Nasal polyps in children can be tricky to spot because many early signs mimic common allergies or routine sinus infections. Parents often notice subtle changes only after symptoms persist or worsen. Understanding both typical and warning signs is key to seeking timely evaluation and preventing complications.
Typical Signs
Most children with nasal polyps experience symptoms that resemble ongoing sinus issues or allergies:
- Persistent nasal congestion or blockage.
- Chronic nasal discharge.
- Post-nasal drip.
- Mouth breathing.
- Snoring during sleep.
- Reduced sense of smell.
- Daytime fatigue or irritability.
Children are highly adaptable and may not complain, making it easy for parents to overlook gradual changes in airflow or nasal function.
Less Common or Red-Flag Signs
Certain symptoms indicate a potentially more serious underlying issue and require prompt medical attention:
- A unilateral (one-sided) nasal growth.
- Frequent nosebleeds.
- Swelling around the face or eyes.
- Vision changes.
- Unexplained fatigue or slowed growth.
- Recurrent ear infections.
Unilateral polyps, in particular, often warrant imaging studies to rule out tumors or congenital masses.
When to See an ENT? Parents should schedule an evaluation if:
- Symptoms persist longer than 12 weeks despite allergy or sinus treatments.
- Children with known cystic fibrosis (CF) or primary ciliary dyskinesia (PCD) develop new nasal obstruction.
- Sleep problems emerge alongside nasal blockage, including snoring, apnea, or restless sleep.
Early evaluation is important because the longer chronic inflammation continues, the more difficult it becomes to treat without medical intervention. Timely intervention protects airflow, sinus health, and overall growth and development.
Diagnosis and Evaluation of Nasal Polyps in Children
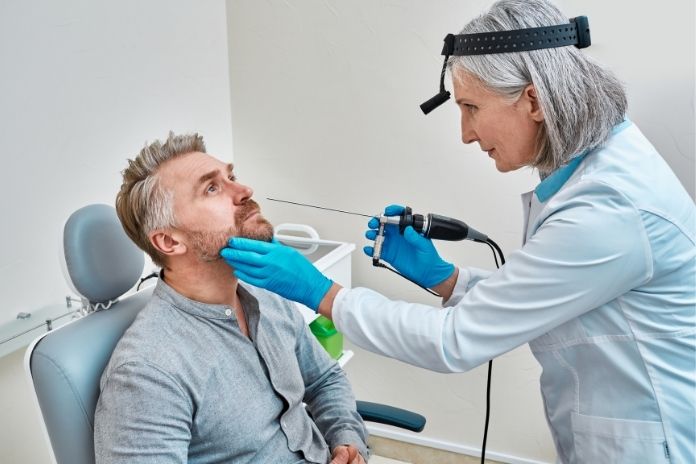
Identifying nasal polyps in children requires careful evaluation, as early detection can guide treatment and prevent complications. Pediatric ENTs rely on a combination of clinical history, physical examination, imaging, and specialized tests to distinguish polyps from other conditions and determine the underlying cause.
Medical History and Physical Exam
A thorough initial assessment typically includes:
- Nasal endoscopy: A thin camera inserted into the nostril allows the ENT to visualize polyps directly. This is considered the gold standard for diagnosing polyps in children.
- Allergy and asthma review: Evaluating past or current allergic conditions and asthma helps identify associated inflammatory triggers.
- Screening for systemic diseases: Tests for conditions like cystic fibrosis (CF) or immunodeficiency are often considered, especially in children with bilateral or recurrent polyps.
Nasal endoscopy not only confirms the presence of polyps but also helps assess their size, location, and potential impact on airflow and sinus drainage.
Imaging and Tests
Depending on the initial findings, further tests may include:
- CT scan of the sinuses: Evaluates the extent of polyps, sinus anatomy, and rules out structural issues or mass-like lesions.
- Sweat or genetic tests: Ordered if CF is suspected.
- Ciliary function tests: Help diagnose primary ciliary dyskinesia (PCD).
- Immunological work-up: Conducted if immune dysfunction is a concern.
Imaging and specialized tests are essential to distinguish nasal polyps from other structural, infectious, or neoplastic causes.
Differential Diagnosis
Pediatric ENTs must differentiate polyps from other nasal masses, including:
- Antrochoanal polyps– typically unilateral and originating from the maxillary sinus.
- Benign tumors– growths that are not cancerous but may mimic polyps.
- Malignant tumors– rare but critical to rule out.
- Congenital nasal masses– structural or developmental anomalies present from birth.
Careful differentiation ensures children receive the appropriate intervention without unnecessary procedures.
Classification and Endotypes
Recent research highlights that pediatric nasal polyps can reflect distinct inflammatory “endotypes.” For example, Th2-dominant pathways are commonly associated with allergies and asthma. Understanding a child’s polyp endotype helps predict:
- How they might respond to medications, such as corticosteroids or biologics.
- The likelihood of recurrence after treatment.
This endotype-based approach enables personalized care, improving outcomes and reducing the need for repeated interventions.
Treatment Options for Nasal Polyps in Children

Treating nasal polyps in children focuses on relieving symptoms, addressing underlying causes, and preventing recurrence. Management typically starts with medical therapy and progresses to surgery only if necessary. Long-term follow-up and multidisciplinary care are essential for sustained results.
Medical Management (First-Line)
Most pediatric ENTs begin with non-surgical approaches:
- Saline irrigation: Helps flush mucus and reduce nasal congestion.
- Topical nasal corticosteroids: Sprays or drops reduce inflammation and shrink polyps.
- Short courses of oral steroids: Reserved for severe or resistant cases.
- Allergy and asthma management: Controlling these conditions often improves nasal symptoms.
Topical steroids have strong evidence supporting their effectiveness and remain the cornerstone of non-surgical management in children. According to the Mayo Clinic, consistent use of nasal steroids is often enough to control symptoms and reduce polyp size.
When Surgery is Considered
Surgery is reserved for cases where medications do not provide adequate relief or when polyps severely affect breathing, sleep, or daily life.
- Functional Endoscopic Sinus Surgery (FESS):This minimally invasive procedure removes polyps and opens sinus pathways to improve drainage. Pediatric ENT literature, including studies in Lippincott ENT journals, highlights its effectiveness in carefully selected children.
Special Considerations for Pediatric Surgery:
- Developing sinus anatomy increases technical complexity.
- Anesthesia risks must be carefully managed.
- Children with CF or PCD have a higher risk of polyp recurrence.
- Surgery is not a cure; ongoing medical therapy is usually required afterward.
Long-Term Prevention and Follow-Up
Successful long-term management depends on treating polyps and controlling the root cause of inflammation.
Recommendations include:
- Continued nasal steroid therapy to prevent regrowth.
- Regular ENT follow-ups for monitoring.
- Allergy evaluation and environmental control (reducing dust, smoke, and pollutants).
- Coordination with pulmonology, genetics, or immunology teams for children with systemic conditions.
Recurrence is common, particularly when underlying inflammation or systemic disease persists. A review in PMC emphasizes that pediatric patients benefit most from a long-term, multidisciplinary approach combining medical therapy, lifestyle interventions, and close monitoring.
Quick Recap
Nasal polyps in children, though rare, are more than just a nuisance; they often indicate an underlying systemic or chronic inflammatory condition that requires careful evaluation. Early recognition of symptoms, including persistent nasal blockage, snoring, or subtle changes in breathing, is essential to prevent long-term complications affecting sinus health, sleep, and even facial development.
Parents and caregivers play a critical role in noticing these signs and seeking timely medical attention. Diagnosis relies on a combination of thorough medical history, nasal endoscopy, imaging, and, when appropriate, genetic or immunological testing.
Differentiating polyps from other nasal masses, tumors, or congenital anomalies ensures that children receive accurate, targeted care. Advances in understanding pediatric inflammatory endotypes further help clinicians predict treatment response and recurrence risk, allowing for personalized management strategies.
Treatment and long-term management focus on controlling inflammation, addressing underlying causes, and preventing recurrence. Medical therapy with nasal corticosteroids, saline irrigation, and management of coexisting allergies or asthma is first-line, while surgery is reserved for resistant cases.
Ongoing follow-up and multidisciplinary care are essential to maintaining nasal health, ensuring proper growth, and improving quality of life. With timely intervention and consistent care, most children with nasal polyps can achieve symptom relief and healthy sinus function.
References
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8620101/
- https://my.clevelandclinic.org/health/diseases/15250-nasal-polyps
- https://www.mdpi.com/2075-4426/13/5/707
- https://emedicine.medscape.com/article/994274-overview
- https://www.abeergroup.com/ksa/HealthBlogDetails.aspx?id=50
- https://www.thenextbreath.com/nasal-polyps
- https://www.mayoclinic.org/diseases-conditions/nasal-polyps/symptoms-causes/syc-20351888
- https://onlinelibrary.wiley.com/doi/10.1111/j.1398-9995.2007.01323.x
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/nasal-polyps
- https://aafa.org/asthma/asthma-triggers-causes/health-conditions-that-trigger-asthma/nasal-polyps/
- https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0139945
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6963757/
- https://jccpractice.com/article/clinical-characteristics-and-management-outcomes-of-pediatric-nasal-polyps-a-tertiary-care-experience-1194/
- https://www.researchgate.net/publication/355845845
- https://www.kidsvillepeds.com/blog/1343104-breathe-easy-spotting-and-treating-nasal-polyps-in-kids/
- https://www.childrensnational.org/get-care/health-library/nasal-polyps
In this Article