Atopic dermatitis of the feet can feel particularly frustrating. This is because flare-ups tend to happen in the very place you rely on every single day. Moisturizers, prescription ointments, and barrier creams are essential for maintaining healthy skin. However, most people overlook one of the biggest everyday triggers: their footwear.
Shoes and socks create a small, closed environment around the feet. Every day, the heat builds up, sweat collects, and shoes rub against the skin repeatedly. To add to it, materials such as leather, rubber, glues, dyes, and synthetic fibers touch the same areas of skin for hours.
As a result, the feet are exposed to several potential irritants simultaneously: moisture, friction, pressure, and chemical contact. Podiatrists and dermatologists consistently consider footwear as one of the most common but least recognized culprits of foot eczema.
We often take good care of our skin, but go wrong in one place. They continue wearing the same shoes that keep provoking their flare-ups.
In this article, we will learn how socks and shoes can either trigger or prevent atopic dermatitis of the feet, what materials and habits matter most, and how to choose protective footwear that promotes the healing process.
Key Takeaways — What You’ll Learn
- How shoes and socks made of particular materials or certain chemicals can cause flare-ups in people’s feet with eczema.
- Things to look for in socks that can help reduce friction, moisture, and irritation.
- Practical hygiene habits that reduce risk: sock rotation, airing of shoes, and detergent choices.
- How to select materials, styles of construction, and fits for shoes that minimize heat and contact dermatitis.
- Early warning signs that your shoes are causing inflammation.
- What to do during high-risk times: traveling, long walks, workouts, or active flare-ups.
Read More: Rotating Your Shoes: Why Switching Pairs Can Improve Foot Health and Performance
Why Footwear & Socks Trigger Atopic Dermatitis on the Feet
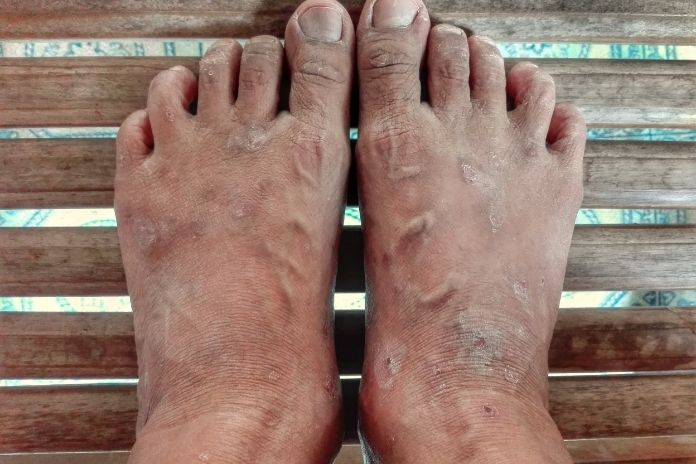
Knowing how footwear impacts eczema will help you make wiser choices for its prevention. The foot is the only part of the body that comes in contact with shoes and socks. Hence, choosing the right fit, make and material of footwear makes a significant difference in eczema.
Warm, Humid Conditions in Shoes:
Your feet have more sweat glands per square inch than most other areas of the body. Once you put on your shoes, that sweat gets trapped. Heat quickly builds up, and humidity gets sealed in.
Podiatry experts explain that this “mini climate” can break down the skin barrier over time. When the skin becomes moist and softened, it is more prone to irritation, cracks, itching, and flare-ups.
Materials and Chemicals Can Irritate Sensitive Skin:
The following mix of chemicals is usually used in the treatment of footwear materials during manufacturing:
- Rubber components such as soles, backs, and insoles also contain rubber accelerators including thiurams and carbamates.
- Leather shoes might contain chromium-based tanning agents.
- Fabric can include azo dyes, preservatives, and adhesives.
- Adhesives, resins, or stabilizing agents may be part of foam insoles.
- Synthetic fabrics can retain more heat and moisture.
Dermatologists and experts suggest that allergic contact dermatitis related to shoes is very common. It may be due to the same chemical touching the spot repeatedly for hours.
Friction and Pressure Cause Micro-Trauma:
Tight shoes may cause excessive friction. Even stiff materials or tight stitching are responsible for the same. This constant friction leads to the following issues over time:
- Redness
- Chafing
- Micro-cracks
- Thickening or hardening of the skin
- Increased irritation during sweat buildup
Even the best-fitted shoes will eventually cause friction on long walks, exercise, or simply because feet swell naturally during the day. Medical dermatology sources list friction among the top triggers of foot eczema.
Moisture and Sweat Build-Up Fuels Flare-Ups:
Sweat does not just make the feet damp; it also contains salt and natural irritants. Combined with bacteria and heat, sweat makes a perfect environment for irritation and further infection. According to the National Eczema Association, sweaty feet flare up often because moisture compromises the skin barrier and may trap allergens or irritants inside socks and shoes.
How to Choose Protective Socks for Foot Eczema

1. Sock Material & Make
The best way to avoid flare-ups, and one of the simplest, is to choose the right material for your socks.
Best materials for eczema-prone feet include:
- Cotton material is breathable, soft, and gentle on sensitive skin.
- Merino wool blends of high-quality; they regulate heat and wick moisture away effectively. These blends have been preferred as they are non-itchy and comfortable.
- Silk or bamboo material is extremely soft and perfect for friction reduction.
- Athletic moisture-wicking blends are great if you tend to sweat heavily. You must avoid those socks with heavy dyes or fragrances.
High-quality materials help prevent overheating, reduce moisture retention, and decrease direct skin irritation.
What to Avoid:
- Footwear or socks with rough seams, particularly across the toes.
- Socks with tight, thick elastics at the cuff that dig into the skin.
- Socks made of cheap synthetics that trap heat and sweat.
- Fuzzy socks or the ones with textured inside surfaces that create friction.
If you are prone to sweating or friction, consider wearing double-layer socks. Wearing a thin liner sock of silk or cotton under a regular breathable sock reduces chafing and helps wick moisture into the outer layer.

2. Sock Hygiene & Rotation
Sock hygiene is just as important as sock material. Here are a few tips that’ll help maintain it and prevent atopic dermatitis flare-ups on your feet:
- Change socks at least once each day. Change twice if your feet are very sweaty.
- Always change socks after workouts or long walks.
- Let shoes and insoles dry completely overnight since leftover moisture can be a cause of morning flare-ups.
- Use fragrance-free and dye-free detergents. Residues from scented or harsh detergents can irritate eczema.
- Avoid fabric softeners entirely. They coat fabric in a way that can retain heat and cause chafing of sensitive skin.
- Wash socks at a warm temperature to rid them of the bacteria and sweat salts left within their fibers.
2. Sock Fit & Style Tips
Small details in fit make a big difference. Here are a few sock fit and style tips:
- It should fit snugly without being tight. Socks that are too tight will restrict airflow and increase sweating, whereas loose socks can bunch and chafe.
- Seamless socks or socks with flat seams reduce the rubbing on toes, which is where irritation often occurs.
- Wear your normal socks over a liner sock to help reduce moisture and friction if you know you’ll be on your feet or moving around a lot.
Read More: Supportive Footwear for Arthritis: 6 Orthopedic Shoes for Pain-Free Walking
How to Choose Footwear That Reduces Eczema Risk

Now that we know about the perfect tips to choose the right socks, let’s discuss footwear. Here’s how you can select the right footwear that reduces eczema risk.
1. Material & Construction Matters
Footwear materials matter more than many people realize. Let’s discuss more about this and ways to prevent atopic dermatitis flare-ups on your feet:
Best shoe materials for eczema include:
- Breathable mesh or fabric uppers
- Soft textile linings that don’t chafe
- Minimal adhesives
- Vegetable-tanned leather (reduced allergen risk compared with chrome-tanned leather)
- Insoles of cork or felt if an allergy to rubber is suspected
Most mainstream and popular shoe brands are made from rubber, adhesives, and chemically treated leather. These are safe for the average person but can cause flare-ups in people with sensitive skin or contact allergies.
Materials to Handle with Care:
- Chrome-tanned leather
- Thick soles of rubber, or straps backed with rubber
- Strong synthetic dyes
- Inexpensive foam insoles with a powerful chemical smell
- Shoes using heavy glue or adhesives
If you have ever noticed a flare in the same spot where a part of the shoe touches your skin, it may be due to the material.
2. Fit & Ventilation
Dr Divya Shokeen, MD, FAAD, a Los Angeles-based dermatologist, shares with SELF, “Breathable shoes enhance the circulation of air and reduce the chances of heat and perspiration.”
- The right fit reduces pressure, chafing, and overheating.
- Shoes should have a roomy toe box so the toes can move freely.
- Avoid narrow or pointed shoes that can cause the toes to rub together.
- Look for ventilation features that include mesh uppers, perforated panels, and removable breathable insoles.
- Rotate pressure points by wearing different shoe styles from one day to another.
- Allow shoes to breathe in a dry, open area rather than in a closed drawer, cabinet, or gym bag.

3. Maintenance & Care
Even the best shoe materials will cause flares if they are not regularly cleaned.
- Wipe the inside and outside of shoes every few days with a soft, unscented cloth.
- Replace insoles when they become worn, compressed, or persistently damp.
- If shoes get wet, let them dry completely before wearing them again.
- Use moisture absorbers if you live in a humid climate or tend to sweat heavily.
Read More: 12 Best Moisturizing Socks 2021; Pedicure At Home, Feet Treatment
Specific Tips During Flare-Up or High-Risk Times

Certain situations require special protection:
During Active Flare-Ups:
- Wear open-toed or breathable sandals when possible to reduce heat and pressure.
- Stick to soft cotton or seamless socks, which won’t cause much friction.
- Avoid shoes made from materials you have not worn before.
During Travel:
- Airports, long walks, and closed shoes for hours increase the risk of flare-ups.
- Carry extra socks.
- Wear breathable walking shoes instead of fashion footwear.
In Gyms or Locker Rooms:
The floors are communal, damp, and warm, which can be ideal for irritation.
- Wear protective sandals.
- Change out of sweaty socks immediately.
During Long Days on Foot:
- Use double socks or liner socks.
- Consider applying a barrier cream before wearing your shoes.
- Rotate between two pairs of breathable shoes.
Quick Recap
Flares of foot eczema are frequently related to the environment inside the shoe, which promotes moisture, heat, friction, and chemical exposure. Irritation can be radically reduced by choosing breathable, seamless socks and well-ventilated shoes.
Care habits make a big difference, such as rotating shoes, avoiding strong detergents, and wearing moisture-wicking socks. For flare-ups or periods of heavy activity, reduce pressure and heat by wearing open footwear or liner socks.
If there is repeated eczema at the same locations, then you must find an alternative to the shoe material and visit your medical provider.
Frequently Asked Questions
Can my shoes cause atopic dermatitis on my feet?
Yes, shoes can cause eczema through the buildup of friction, perspiration, and exposure to leather, dyes, glues, rubber, and adhesives.
Which material of socks is best for foot eczema?
Generally, the best are cotton, bamboo, silk, and merino wool blends. Look for seamless socks that are breathable to wick away moisture.
How often should shoes or insoles be replaced in cases of foot eczema?
Replace shoes every 6-12 months if you wear them regularly. Replace insoles every few months or when they lose structure and absorb moisture.
Are there certain shoe brands or materials that are safe for eczema-prone feet?
Brands with mesh athletic shoes or vegetable-tanned leather options are generally safer. The key is avoiding strong adhesives, heavy rubber, and harsh dyes.
Should I completely avoid socks with seams if I have foot eczema?
You don’t have to avoid them completely, but flat-seam or seamless styles significantly reduce friction, especially during flare-ups.
How can I test if my shoes are causing my foot eczema?
Try removing one pair from rotation for 1–2 weeks. If symptoms ease, you likely identified a trigger. Dermatologists can also perform patch testing.
References
- https://certifiedfoot.com/understanding-and-managing-eczema-on-feet/
- https://www.cdc.gov/hygiene/about/foot-hygiene.html
- https://www.ijord.com/index.php/ijord/article/download/1254/691/5367
- https://www.researchgate.net/publication/318179141_Effects_of_Socks_and_Shoes_on_Normal_Foot_Skin_Temperature
- https://nationaleczema.org/blog/hand-and-foot-eczema/
- https://nationaleczema.org/eczema/
In this Article





















