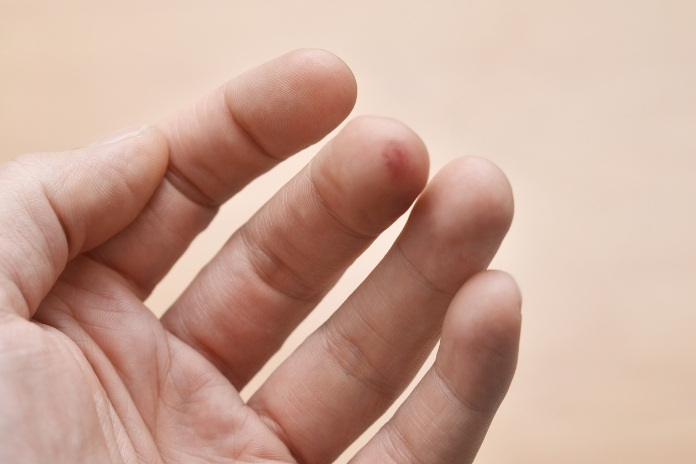
Seeing your fingertips turn dark, purplish, blue, or outright black is unnerving, and for good reason. The color of your fingertips can reveal a lot about what’s happening beneath the skin.
Sometimes it’s harmless, like a brief reaction to cold, mild bruising, or even dye stains that fade away. But other times, it’s a red flag for something more serious: poor circulation, nerve damage, tissue death, or an underlying condition that’s silently progressing.
Here’s the thing: Fingertip discoloration isn’t a diagnosis on its own. It’s a symptom that can range from minor and temporary to urgent and life-threatening. Understanding what your body is trying to say can make all the difference.
This article breaks down what “blackening” of the fingertips can actually mean, from the common culprits to the rare but dangerous ones. You’ll learn the early warning signs that shouldn’t be ignored, the safe first steps to take at home, how doctors pinpoint the root cause, and what treatment and prevention options exist to protect your hands and your overall health.
The Concern Behind Darkening Fingertips

Your fingertips are the body’s most distal, exposed tissues. Because they are tiny and at the end of the circulation line, they’re unusually sensitive to changes in blood flow, oxygen delivery, and local injury. When fingertips go from their normal pink to blue, purple, or black, that colour change is either:
- A benign, temporary response(for example, Raynaud’s attacks when cold or emotional stress briefly reduce blood flow), or
- A signal of real tissue compromise(poor arterial flow, blood clots, severe frostbite, chemical injury, or gangrene) that can lead to permanent damage if ignored.
The aim here is practical: Help you identify likely causes, spot the red flags that need a doctor right away, and explain what evaluation and treatment usually involve. Early action matters; many causes are treatable, and prompt care prevents tissue loss.
What Does “Blackening” or Darkening of Fingertips Mean?
“Blackening” is a lay term that can describe a range of appearances:
- Bluish or purplish tint (cyanosis/peripheral cyanosis):“When a fingertip turns bluish or dark, it often means the local tissue is not getting enough oxygen or blood flow. That’s a warning sign. If the area becomes hard, numb, charred or smells bad, you must consider that the tissue might be dying (necrosis or gangrene) and seek urgent care.” – Dr Ananya Mandal, MD for News-Medical.
- Dark brown/black patches: may be dried blood, deep bruising, a stain, necrotic tissue, or gangrene (dead tissue due to lack of blood flow or severe infection). Gangrenous tissue can be leathery and may have a foul smell.
- Black spots or lines: sometimes simple bruises, splinters, subungual hematomas (blood under the nail), or pigment changes. These are not always vascular in origin.
Surface staining or pigment change (from ink, dye, nicotine, or contact with chemicals) can look dramatic but isn’t dangerous; true tissue necrosis (gangrene) is a medical emergency. If the area is hard, numb, worsening, blistering, or producing a bad smell, assume tissue injury until a clinician confirms otherwise.
Common Causes of Fingertip Darkening
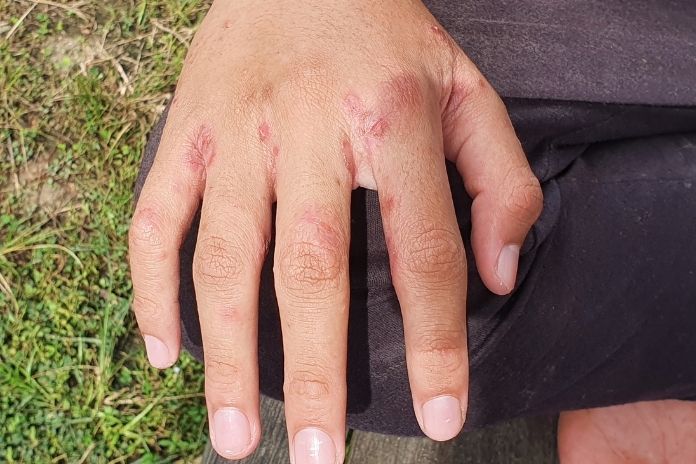
Below are the most common categories, explained clearly so you can think through which might fit your situation.
1. Cold-induced conditions: Raynaud’s phenomenon and acrocyanosis
- Raynaud’s phenomenon is extremely common. During an attack, the small arteries in fingers spasm in response to cold or stress; the typical colour sequence is white (pale), blue (deoxygenated), red (reperfusion).
Attacks are often brief and reproducible with cold exposure. Primary Raynaud’s (no other disease) is usually milder; secondary Raynaud’s (associated with autoimmune disease such as scleroderma) can be more severe and damaging.
- Acrocyanosis causes persistent bluish discoloration of hands and feet from prolonged small-artery constriction; it is usually painless and often benign, but should be evaluated if it’s new or asymmetric.
Why it matters: Cold-triggered colour change that returns to normal with warmth and has no ulceration is often manageable with lifestyle changes and medicines; persistent blackening, ulcers, pain, or progressive change is not a benign Raynaud’s presentation and needs urgent assessment.
According to a review of Acrocyanosis, the condition refers to a persistent, abnormally deep blue or cyanotic discoloration of the skin over the extremities, most commonly the hands and feet, resulting from decreased oxygenated hemoglobin in the blood.
The review emphasizes that, unlike Raynaud’s phenomenon which presents as episodic attacks, acrocyanosis is continuous, typically painless, and often benign, though new or asymmetric cases warrant medical evaluation.
2. Severe circulation problems and peripheral vascular disease
- Buerger’s disease (thromboangiitis obliterans) is an inflammatory disease of small and medium arteries and veins that almost always affects smokers. It can cause pain, ulcers, and gangrene in fingers and toes; the affected digits can become black from tissue death. Smoking cessation is the single most important intervention.
- Atherosclerotic peripheral arterial disease, emboli, or arterial thrombosis may block flow to a fingertip, producing a single-digit cold, painful, discolored finger that can progress to gangrene if not revascularized.
Why it matters: These causes are vascular emergencies when acute, loss of sensation, severe pain, rapidly darkening skin, or a single finger becoming cold and pale, then dark, should prompt immediate medical attention. Early revascularization or clot removal can save tissue.
According to Dr William Schuyler Jones, MD, author of the MSD Manual section on Thromboangiitis Obliterans (Buerger’s disease), the condition invariably worsens in people who continue to smoke, and amputation is commonly required; in contrast, if people stop smoking, the disease usually stops progressing.
3. Chemical/external causes, frostbite, and burns
- Chemical stains and contact reactionsfrom dyes, inks, work chemicals, or concentrated household agents can cause localized darkening or blistering. Frequently, the discolouration is superficial and will fade, but some chemicals (strong acids/alkalis) can chemically burn tissue and cause permanent damage. Protect hands and wash immediately after exposure.
- Frostbitein severe cases causes the skin and underlying tissues to freeze, then, after rewarming, may become dark, blistered, and eventually black if tissue necrosis occurs. Deep frostbite can lead to black, hard tissue weeks after the injury as the damaged tissue demarcates.
Why it matters: Frostbite with hard black tissue or spreading blisters needs urgent evaluation. Chemical exposures should be rinsed and assessed for burns; remove rings and constricting jewellery if swelling occurs.
Read More: Understanding Frostbite: Symptoms, Prevention, and Effective Treatment
4. Underlying systemic or autoimmune conditions
- Vasculitis(blood-vessel inflammation) can affect small digital arteries and cause ulceration and blackening. Conditions such as cryoglobulinemia cause proteins to precipitate in cold, reducing flow and sometimes leading to gangrene. Mount Sinai and other sources show how cryoglobulinemia can produce dark, gangrenous fingers.
- Scleroderma and connective-tissue diseasescan permanently damage small blood vessels and cause severe Raynaud’s or digital ulcers. Diabetes and chronic kidney disease also impair circulation and wound healing.
Why it matters: If your fingertip symptoms are accompanied by other systemic signs (joint pain, skin tightening, unexplained fevers, rashes, weight loss), a systemic cause must be investigated by a specialist; early diagnosis changes management and outcomes.
Read More: Autoimmune-Friendly Supplements to Support Immune Regulation
When it’s a Red Flag, Warning Signs to See a Doctor Now
Not all discoloration is an emergency. But seek urgent evaluation if you notice any of the following:
- Rapid progression from pale to blue to dark/black in a finger or fingers.
- New, severe pain in the digit, loss of sensation, or the finger is cold to the touch are signs of critical ischemia.
- Open ulcers, blisters, pus, or foul smell, possible infection, or wet gangrene.
- Single-digit changes after trauma (for example, splinter, crush injury) that won’t pink up or have decreasing blood flow.
- Associated systemic symptoms like chest pain, shortness of breath, fever, sudden weakness, or signs suggesting an embolic or systemic vascular event.
- Exposure risk, including chemical burns, severe frostbite, or if a child ingests or has contact with caustic material.
If you have these signs, go to the emergency department or call your clinician. Interventions (oxygen, vascular imaging, anticoagulation, rewarming, surgical debridement, or removal of clots) may be time-sensitive.
What to Do at Home: Initial Steps

For mild, non-progressive cases (for example, temporary Raynaud’s or superficial stains), these steps can help:
- Warm the hand gently if cold is the trigger; warm (not hot) water or gloves, but do not massage a severely icy limb or apply direct heat if frostbite is suspected; get medical care. Return to warmth gradually.
- Avoid nicotine and smoking; tobacco constricts small blood vessels and worsens vascular disease (especially crucial in Buerger’s disease). Quitting smoking is often the single most effective long-term measure to protect digital circulation.
- Protect from further injury. Remove rings if swelling begins, keep the hand elevated if swollen, and avoid tight gloves or straps.
- Rinse and neutralize after chemical exposure, flush with water for at least 15 minutes, and remove contaminated clothing; seek medical attention for corrosive agents.
- Monitor and document – note when the discoloration started, triggers (cold, chemicals, injury), any change over time, and whether other symptoms appeared (numbness, fever). Photos with timestamps help clinicians.
If the situation is painful, worsening, or shows any red flags above, skip home remedies and get immediate medical evaluation.
Diagnosis and Treatment Overview
Clinicians will take a targeted history (onset, triggers, associated symptoms, smoking history, medications, systemic disease) and a focused physical exam. Common diagnostic steps include:
- Vascular assessment: Palpation of pulses, capillary refill, Doppler ultrasound, ankle–brachial index, or arterial duplex if large-vessel disease is suspected.
- Cold-challenge testing and nailfold capillaroscopy in suspected Raynaud’s or connective-tissue disease.
- Blood tests: Inflammatory markers, autoimmune panels (ANA, ANCA), cryoglobulins, complete blood count, infection markers as indicated.
- Imaging: Angiography (CT or conventional) when embolus or severe peripheral disease is suspected and revascularization is being considered.
Treatment depends on the cause
- Raynaud’s or acrocyanosis: Lifestyle measures (warmth, stress reduction), stopping smoking, and medications such as calcium-channel blockers (e.g., nifedipine) or topical vasodilators for severe attacks. Treat secondary causes (autoimmune disease) when present.
- Acute vascular occlusion, embolus, or thrombosis: Urgent vascular surgery or interventional radiology may be required to restore blood flow. Anticoagulation and clot-removal procedures are time-sensitive.
- Buerger’s disease: Strict smoking cessation is essential; wound care, pain control, and sometimes surgical management for advanced tissue loss.
- Frostbite: Rewarming protocols, tetanus status, wound care, and in severe cases, surgery or amputation for nonviable tissue weeks after injury.
- Chemical burns or contact dermatitis: Decontamination, topical therapies, and burn/wound specialist care when indicated.
- Infection and gangrene: Antibiotics, surgical debridement, and sometimes amputation when tissue is nonviable or infection is uncontrolled.
Early specialist input (vascular surgery, dermatology, rheumatology, or burns unit) is often necessary for complex or rapidly progressing cases.
Read More: 10 Everyday Triggers of Atopic Dermatitis (Eczema) Flare-Ups—and How to Avoid Them
Prevention and Long-term Management
If you’re at risk or have a chronic condition that affects circulation, keep the following practices as part of your routine:
- Quit smoking and avoid nicotine; this is the most powerful single change for people with smoking-related vascular disease. Public health and clinical data emphasize improved healing and reduced progression after quitting.
- Protect from cold, gloves, warm clothing, and heated hand warmers in cold weather; avoid sudden temperature drops.
- Treat underlying disease; control diabetes, high blood pressure, and high cholesterol; manage autoimmune disease with specialist care.
- Avoid repetitive vibration or occupational exposures that affect small vessel function (jackhammers, vibrating tools).
- Regular follow-up for those with recurrent Raynaud’s, vasculitis, or connective-tissue disease, nailfold capillaroscopy, and serial exams may detect deterioration before tissue loss occurs.
Prevention is about reducing triggers, addressing modifiable risks (especially smoking), and close monitoring for early signs of tissue compromise.
Key Takeaway
Fingertip darkening ranges from harmless stains and reversible cold-induced colour changes to signs of severe vascular compromise and gangrene. The difference between “benign” and “dangerous” is often in the details: pain, rapid progression, single-digit ischemia, ulceration, numbness, and foul odor are red flags. Early medical review can preserve tissue and prevent major complications. If you’re unsure, err on the side of evaluation.
Short checklist:
- If the change is brief, linked to cold, symmetrical, and resolves with warmth, likely Raynaud’s/acrocyanosis; see your clinician for long-term management.
- If the change is rapid, painful, localized to one digit, ulcerated, or associated with systemic symptoms, seek urgent medical attention.
- Quit smoking, protect your hands from cold, avoid chemical exposure, and get specialist follow-up for recurrent or unexplained changes.
FAQs
Q: Why do my fingertips turn blue or black when I’m cold?
Cold triggers vasospasm in conditions such as Raynaud’s, small vessels constrict, reducing blood and oxygen to the skin and turning the fingers white/blue. In most people, this is reversible when warmed; if it progresses to blackening or ulcers, see a clinician.
Q: Can Raynaud’s cause permanent fingertip damage?
Primary Raynaud’s rarely causes permanent tissue loss. Secondary Raynaud’s (associated with autoimmune disease) can cause ulcers and, in severe cases, gangrene. That’s why new, severe, or asymmetric symptoms merit specialist evaluation.
Q: Is darkening of the fingertip always an emergency?
Not always. If it’s a temporary, symmetrical response to cold that resolves with warmth, it’s usually not emergent. But if it’s painful, progressive, affects a single finger, or includes ulcers, blisters, numbness, or foul smell, treat it as urgent.
Q: What is gangrene, and how is it related to black fingertips?
Gangrene is tissue death due to a lack of blood flow or a severe infection. When fingertips go black and the tissue becomes hard, numb, and foul-smelling, that’s consistent with gangrene. Prompt surgical and medical management is often needed.
Q: Can quitting smoking reverse fingertip darkening due to vascular causes?
Quitting smoking is the most important intervention for smoking-related vascular disease (including Buerger’s disease). It can improve healing, reduce progression, and, in many cases, prevent further tissue loss, but existing necrotic tissue will not spontaneously recover.
References
- https://www.quora.com/I-have-a-dark-band-running-across-my-finger-nails-Should-I-be-concerned
- https://www.doubtnut.com/qna/13842941
- https://www.malacards.org/card/pigmentation_anomaly_of_the_skin
- https://www.sciencedirect.com/medicine-and-dentistry/brown-spot
- https://pmc.ncbi.nlm.nih.gov/articles/PMC10095087/
- https://www.ojp.gov/pdffiles1/nij/225320.pdf
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8211329/
- https://patents.google.com/patent/EP3363426B1/zh
- https://www.sciencedirect.com/science/article/pii/S2214662824000215
- https://www.nature.com/articles/148285a0.pdf
- https://fssai.gov.in/upload/uploadfiles/files/Manual-Microbiology-Methods.pdf
- https://www.researchgate.net/publication/6373280_Enhancement_of_Ninhydrin-_or_DFO-Treated_Latent_Fingerprints_on_Thermal_Paper
- https://jhpolice.gov.in/sites/default/files/documents-reports/jhpolice_ebook_a_forensic_guide_for_crime_investigators.pdf?pNHAV=0Cw9AoUb0U
In this Article