Are you feeling full or pressured “down there”? It could be more than just getting older or recovering from giving birth; it could be a prolapsed bladder. A cystocele, which is another name for a prolapsed bladder, happens when the muscles and tissues that hold your bladder in place weaken and let it sag against the wall of your vaginal canal.
This happens with many women, especially after giving birth or during menopause, but most women fail to realise this condition. A cystocele feels like the vagina has a bulge or is hanging. This feeling is usually worse when you stand up or lift something. You might have trouble peeing, like starting, stopping, or the bladder not fully emptying. You might also have urine leaks and often get infections.
There is also a lot of pain during sex. This condition can cause a lot of bladder issues if not addressed on time. Conservative treatments, like Kegel exercises for the pelvic floor, maintaining a healthy weight, avoiding heavy lifting or straining during motions, giving up smoking, or using a pessary, can help a lot.
If the problem is really bad, surgery might be suggested. If your symptoms are bothering you, get help. This article tells you what it is, what symptoms to look out for, and simple ways to feel better.
Read More: Strengthen Your Pelvic Floor with these Kegel Exercises
What Is a Prolapsed Bladder (Cystocele)?

A cystocele, which is another name for a prolapsed bladder, occurs when the bladder moves out of place and presses against the pelvic wall. This shift takes place when the muscles and connecting tissues in the pelvic floor, which hold the bladder in place, do not function properly. This is one of the most common post-childbirth bladder issues, and it can also happen if your pelvic support changes over time.
In medical terms, a cystocele is a type of pelvic organ collapse, which means that an organ in the pelvis has moved out of place. The bladder moving toward or into the vagina, often causes a visible or felt vaginal bulge, is what makes this condition unique, though the severity can vary.
Bladder prolapse is not a sickness but a change in the structure of the body. There are three levels based on how far the bladder has moved: mild, moderate, and serious. In some women, the bladder may only slightly drop, while in others, it may move toward the opening of the uterus. The main thing that describes bladder prolapse, no matter what stage it is in, is that the bladder’s position in relation to the vaginal wall changes.
Shannon Wallace, MD, Urogynecology Specialist, Cleveland Clinic, says, “We think of the pelvis as a bowl. There can be tissue weakness caused by age, vaginal delivery, obesity, connective-tissue disorders … When you have weakening of these tissues, you can have any of the pelvic organs fall.”
Figuring out what a prolapsed bladder is can help you tell it apart from other pelvic problems. It’s not an infection or a growth; the bladder has moved inside the pelvic region. Because it is closely related to the structural health of the pelvic floor, it is often discussed in terms of a woman’s sexual history, especially after childbirth, menopause, or pelvic surgery.
Read More: Breathing Techniques for Pelvic Floor Relaxation and Strength
What Causes a Bladder Prolapse?
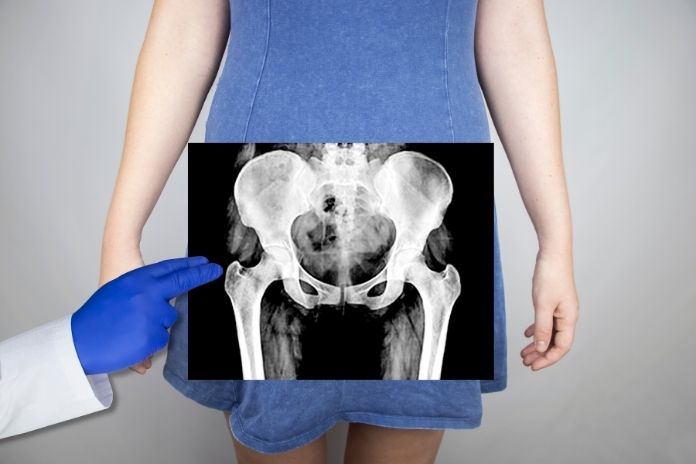
Another name for a bladder collapse is a cystocele. This is a type of pelvic organ prolapse. It takes place when the bladder moves out of place and presses against the wall of the vaginal canal. Women who have pelvic floor weakness in muscles and connecting tissues that support the bladder may experience this issue. Here are some of the most popular reasons.
Vaginal childbirth
A lot of women get bladder prolapse after giving birth, especially when they have given birth multiple times or delivered babies through the use of forceps. The pelvic muscles and ligaments can be hurt by the stretching and pressure of giving birth. This can cause bladder problems after giving birth, where it moves down, which some people describe as feeling like the bladder falling out.
Aging and menopause
Estrogen is very important for keeping the muscles in the pelvis strong and flexible. However, the body produces less estrogen as women age, particularly after menopause. When levels drop, the tissues of the muscles get weaker, which raises the risk of pelvic floor weakness and bladder displacement.
Chronic straining
The pelvic floor is put under a lot of pressure over and over again due to constipation, heavy lifting, or coughing. This lowers the support structures over time, which makes it more likely that the bladder will prolapse.
Pelvic surgery
Surgery, such as a hysterectomy, can change the structure of the pelvis and make it harder for the pelvic organs to stay in place. The bladder may fall into the vaginal space if the supporting tissues are taken away or changed.
Obesity or high-impact exercise
The pelvic floor is constantly under stress from carrying extra weight, and high-impact sports like running, jumping, or lifting heavy weights can weaken the tissue even faster. Both of these things raise the risk of pelvic organ prolapse.
Understanding the causes of bladder prolapse is the first step in protecting pelvic health. Recognizing risks like pelvic floor weakness early can help women make informed choices about childbirth, lifestyle habits, and activities that safeguard pelvic support.
Read More: Why Some Women Leak When They Sneeze?
Symptoms of a Prolapsed Bladder Women Shouldn’t Ignore

A cystocele, which is another name for a prolapsed bladder, happens when the bladder moves out of place and into the vaginal wall. This kind of pelvic organ prolapse can happen slowly and get worse over time. In the early stages, some women don’t have any signs that they can see, while others go through changes that make it hard to go about their daily lives.
If you know the most common bladder prolapse symptoms in women, you can take action before the problem gets worse.
Mild to Moderate Symptoms
- Feeling of pressure or heaviness in the pelvic area
A common early cystocele sign is a feeling of heaviness or dragging in the pelvis that doesn’t go away, especially after long periods of standing, walking, or moving. A lot of women say it feels like something is “falling down” inside them.
- A bulge or tissue protruding from the vagina
Some women feel or see a soft bulge in their vaginal area. In mild cases, it might only be found during a pelvic check. In more severe cases, you might feel it when you wash or wipe your body.
- Needing to push or reposition to fully empty the bladder
You might have to press on your vagina, perineum, or lower abdomen to get pee to flow or to know that your bladder is empty.
- Difficulty starting urination or experiencing incomplete emptying
The urethra can move when the bladder prolapses, which makes it harder to start peeing. You might still feel like some pee is there after going to the bathroom.
- Leaking urine when coughing, laughing, or exercising
This happens when the pressure inside the belly rises, like when you sneeze, laugh, or work out. It’s also called stress incontinence.
Advanced Symptoms
- Discomfort or pain during sex
A prolapsed bladder can change the shape of the vaginal canal, which can make sexual activity uncomfortable or painful.
- Increased urinary tract infections (UTIs)
If you don’t empty your bladder all the way, germs can grow and cause you to get UTIs more often.
- Lower back pain or abdominal pressure
In more severe cases, the extra stress on the pelvic organs can cause pain in the lower back or abdomen that won’t go away.
- Bulge becomes visible or worsens by end of the day
The bulge may become more obvious as the day goes on because of gravity and movement. If the problem is really bad, the bulge might stick out past the vaginal hole.
Why You Shouldn’t Ignore These Symptoms
Many women think that the signs of bladder prolapse are just “part of getting older” or a normal side effect of giving birth. But these problems aren’t normal and can be fixed. Ignoring cystocele signs can make pelvic floor weakness worse, cause bladder problems, or even hurt the pelvic organs nearby.
Talk to a urogynecologist if you have a vaginal bulge, pelvic pain, or changes in the way you urinate. Early detection and treatment can make people feel better, stop further damage, and improve their quality of life.
Read More: 10 Gentle Workouts Safe for the Postpartum Body
How a Prolapsed Bladder Is Diagnosed
There are several steps needed to prove that someone has bladder prolapse (cystocele), figure out how bad it is, and decide what to do next. There are stages of bladder prolapse; it can be mild (the bladder only sags a little) or serious (the bladder sticks out of the vaginal opening). Figuring out the stage helps with treatment and care.
Pelvic Exam (Lying Down & Standing)
The first thing your doctor does is a pelvic check to see and feel the bladder’s position. You could be checked out while you’re lying down, standing, or facing down. You can use this to find out how far your bladder has dropped and what stage of bladder prolapse you are in.
Bladder Scan to Check Urine Retention
An ultrasound is used after you’ve gone to the bathroom to see if any urine is still in the bladder. This helps find problems with urine incontinence, like leakage or not emptying all the way, which can happen when pelvic organs prolapse.
May Also Include:
- Urinalysis
If there is an infection or another problem with the urine that could be connected to the prolapse, a simple urine test can find it.
- Urodynamic Testing
Your doctor may suggest urodynamic testing if you have urinary incontinence or difficulty controlling your urine flow. To find out how the prolapse affects bladder function, these tests check bladder pressure, urine flow, and the bladder’s ability to store urine.
- Referral to a Urogynecologist
You may be sent to a urogynecologist, who specializes in pelvic organ prolapse and other pelvic floor diseases, if the prolapse is complicated or far along. Based on the stage of your prolapse, they can do more thorough tests and talk about your choices.
- Why Multiple Tests Matter
Each test gives out different information. Urodynamic tests show how the prolapse affects bladder control, pelvic checks show the stage of the prolapse, and bladder scans show if urine is being retained. When put together, they show how your bladder is working and how the prolapse is affecting your urinary health.
Quick Summary Table
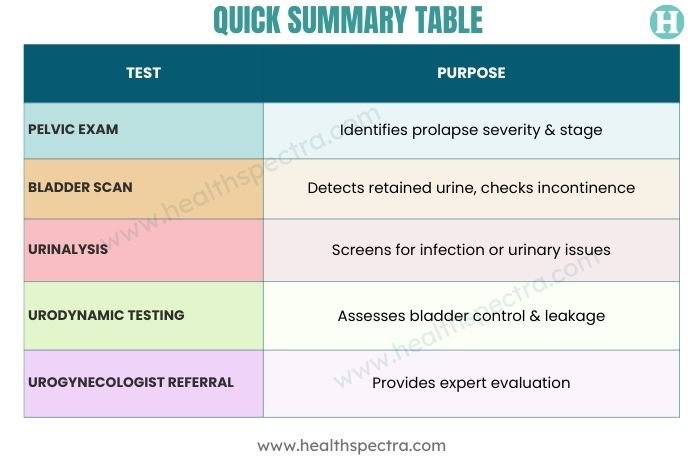 This diagnostic method makes sure that your prolapse is correctly found, staged, and checked for bladder problems like urinary incontinence so that you can make the best care plan.
This diagnostic method makes sure that your prolapse is correctly found, staged, and checked for bladder problems like urinary incontinence so that you can make the best care plan.
Read More: Understanding Pelvic Health: Common Issues and Tips
Treatment Options for Bladder Prolapse

The best way to have a prolapsed bladder treatment relies on how bad it is, your symptoms, and your own preferences. Most of the time, the goal is to ease the pain, make the bladder work better, and keep the disease from getting worse.
1. Mild Cases
Pelvic Floor Physical Therapy
Physical treatment for the pelvic floor can be very helpful for people with mild bladder prolapse. It’s not enough to just do Kegel exercises by yourself. A trained pelvic floor therapist will show you specific movements, breathing techniques, and ways to improve your posture that will help strengthen the muscles that support your bladder and other organs in your pelvis.
Lifestyle Changes
Some things you do every day can help the pelvic floor feel better and keep the prolapse from getting worse. Some of these are:
- How to treat constipation so you don’t have to work when you go to the bathroom.
- Keeping a healthy weight can help your pelvic organs feel less pressure.
- Not lifting heavy things or learning better ways to lift things.
- Taking care of a cough or allergies that cause a lot of cough.
Support Garments for Heavy Activity
Wear clothes that are specially designed for you to be worn during sports, exercise, and other activities that are hard on your body. These make it easier to hold your bladder in place and ease pain.
2. Moderate to Severe Cases
Pessary Device
A pessary is a small, removable object that is put inside the vagina to support the walls and bladder. A healthcare professional fits you for it, and you can wear it for a long time as long as you clean it regularly. If you want to avoid or put off surgery, pessaries are a good choice. They can be especially helpful if you still want to have children.
Estrogen Therapy
Low-dose vaginal estrogen, which can come in cream, ring, or tablet form, may help make vaginal tissues stronger and more flexible in women who have gone through menopause. This may make the prolapse less bothersome and help with the signs of urinary incontinence that can happen due to pelvic organ prolapse.
Surgery
Surgery might be suggested if the symptoms are very bad or if other treatments aren’t helping. Some common choices are:
- Anterior repair (anterior colporrhaphy) – It makes the front wall of the vagina tighter to hold the bladder better.
- Procedures based on mesh – Surgical mesh is sometimes used to strengthen tissue that is weak, but this choice is carefully thought through because it could have risks.
Before choosing surgery, your doctor will talk to you about issues such as the stage of your bladder prolapse, your overall health, your plans for having children in the future, and your own recovery goals.
Read More: Understanding Pelvic Floor Disorders and Pain
Can You Prevent a Bladder Prolapse?

Bladder prolapse can happen for reasons you can’t control, like giving birth, getting older, or your genes. But there are things you can do to lower your risk and protect your pelvic floor health.
Stay Regular with Bowel Movements
The pelvic floor muscles can get weaker over time if you have chronic constipation or strain when you go to the bathroom. Eating a lot of fiber, drinking a lot of water, and keeping active can help your digestion work better and keep you from having to strain.
Avoid Chronic Straining or Heavy Lifting
When you lift large things a lot, at work, at the gym, or at home, the muscles that support your bladder can get strained. If you have to lift something, make sure you do it right by bending your knees instead of your waist and not holding your breath.
Maintain Core and Pelvic Floor Strength
The bladder and other organs in the pelvis need strong core and pelvic floor muscles to stay in place. It helps to perform targeted pelvic floor movements (like Kegels) and gentle core strengthening as part of your routine. You should work with a pelvic health physiotherapist to get the technique right and a routine that fits your needs.
Treat Chronic Cough or Respiratory Issues
When you cough for a long time because of asthma, smoking, allergies, or some other respiratory disease, the pelvic floor is pressed down over and over again. Taking care of the underlying problem and staying away from triggers can help protect the structures that support your bladder.
Avoid Long-Term High-Impact Exercise Without Proper Support
If you do high-impact exercises, running, or other activities like these for a long time without getting enough muscle support, they can put stress on your pelvic floor. Mix up your workouts with low-impact sports like walking, swimming, or cycling, and when you need to, use supportive gear.
Read More: Essential Products to Manage Incontinence for Everyone
When to See a Doctor

Bladder prolapse can be mild to serious. In the early stages, the symptoms may not be very obvious, but it’s important to know what they are. If you see a doctor right away, you can better control the condition and often avoid having surgery.
If You Notice:
- Vaginal Bulging
A feeling or sight of a bulge in the vagina is a common sign of bladder prolapse. Some women say they feel like something is “falling out.” This might be more obvious after standing for a long time, lifting big things, or working hard.
- Persistent Pelvic Pressure
If you feel heavy or pressure in your pelvic area for a long time, it could mean that your bladder is not supported properly. This feeling might get worse at the end of the day or after working out.
- Urinary Leakage or Incomplete Emptying
Bladder prolapse can make you leak urine, especially when you cough, sneeze, or work out. It may also make it harder to empty your bladder completely, which could mean you have to go to the bathroom more often.
- Pain with Intercourse or Chronic UTIs
Because of the change in bladder position, some women feel pain or discomfort during sex. Not emptying your bladder all the way can also make you more likely to get urinary tract infections (UTIs), which can happen more than once.
Why Early Treatment Matters
The best chance for getting rid of symptoms and stopping further prolapse is to see a doctor as soon as possible. Before your situation gets worse, your doctor can suggest treatments like pelvic floor therapy, using a pessary, or making changes to how you live.
If you don’t treat bladder prolapse, it can get worse and a surgery might be needed. Getting help early can keep the pelvic floor strong, improve quality of life, and lower the risk of problems.
Dr. Stephen Jones, Gynecologist, McLeod Health, warns that a prolapsed bladder rarely resolves by itself and underscores the need for timely evaluation. Dr. Jones stresses that “It’s important for women to know that prolapse, left alone, seldom improves on its own.”
Final Thoughts
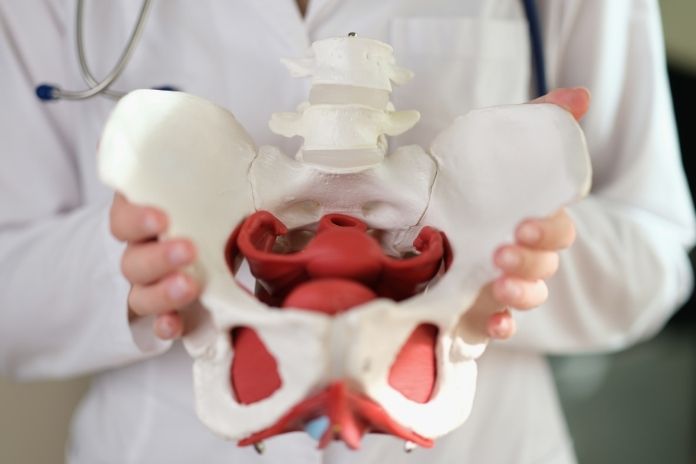
It’s common for women to have a prolapsed bladder, which is also called a cystocele. But you don’t have to accept it as a part of your life. If you know the signs of bladder prolapse in women, like vaginal bulging, urine incontinence, or pelvic pressure, you can catch the problem early.
The sooner you see a doctor, the more treatment choices you’ll have, from making changes to your lifestyle to medical procedures, leading to a more comfortable life.
Talk to your doctor if you think you have bladder prolapse or if you notice changes in the health of your pelvis. Taking the first step to improving your health and well-being makes all the difference.
References
- https://my.clevelandclinic.org/health/diseases/15468-cystocele-fallen-bladder
- https://www.healthdirect.gov.au/prolapsed-uterus
- https://www.niddk.nih.gov/health-information/urologic-diseases/cystocele
- https://www.pacehospital.com/cystocele-prolapsed-bladder-symptoms-causes-prevention-and-treatment
- https://www.acog.org/womens-health/experts-and-stories/the-latest/5-things-i-wish-all-women-knew-about-pelvic-organ-prolapse
- https://www.webmd.com/women/prolapsed-bladder
- https://www.orlandohealth.com/content-hub/is-it-time-to-see-a-urogynecologist-7-signs-you-shouldnt-ignore
- https://carle.org/conditions/gynecology-conditions/uterine-prolapse
- https://my.clevelandclinic.org/health/diseases/24046-pelvic-organ-prolapse
- https://nyulangone.org/conditions/pelvic-organ-prolapse/diagnosis
- https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/bladder-prolapse
- https://www.aurorahealthcare.org/services/womens-health/services-treatments/pelvic-floor-dysfunction/bladder-prolapse
- https://www.emedicinehealth.com/prolapsed_bladder/article_em.htm
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/pelvic-floor-repair
- https://www.acog.org/womens-health/faqs/surgery-for-pelvic-organ-prolapse
- https://www.lompocvmc.com/blogs/2023/may/7-ways-to-prevent-pelvic-floor-prolapse
- https://www.healthdirect.gov.au/bladder-prolapse
- https://www.medicalnewstoday.com/articles/bladder-prolapse-symptoms
- https://advancedgynecology.com/urogynecology-conditions/bladder-prolapse
In this Article
























