If you’re preparing for an induction with misoprostol, commonly known by its brand name Cytotec, you’re probably wondering one thing: How will the pain compare to natural labor contractions?
It’s a common and important question. Many people approach induction with apprehension, fearing that medication-induced contractions will be more painful or intense than spontaneous labor. Understanding what misoprostol is, how it works, and what you can expect from the sensations it causes can ease anxiety and help you prepare for birth with confidence.
In this guide, we’ll explore what misoprostol pain feels like compared to natural labor contractions, key differences in intensity and rhythm, the average timeline to active labor, and your options for pain relief. We’ll also outline the risks and warning signs to watch for and when to reach out to your healthcare team.
What Is Misoprostol and Why Is It Used in Labor?
Misoprostol is a synthetic prostaglandin E1 analog originally developed to prevent gastric ulcers. However, it has found wide use in obstetrics, off-label, as an induction agent due to its ability to ripen the cervix and stimulate uterine contractions.
How Misoprostol Works
Misoprostol mimics the effects of natural prostaglandins by:
- Ripening the cervix: It softens and thins the cervical tissue (effacement), which is necessary before dilation can occur.
- Stimulating contractions: It activates smooth muscle fibers in the uterus, encouraging contractions that can initiate labor.
Routes of Administration
There are three common ways misoprostol is given for labor induction:
- Vaginal: Often preferred because it produces more targeted uterine effects and tends to act more efficiently. A small tablet is inserted near the cervix.
- Oral: Swallowed or placed in the cheek to dissolve. This route may produce slower results, but can be better tolerated.
- Sublingual: Placed under the tongue, where it dissolves quickly and enters the bloodstream faster than other routes.
Each method varies slightly in how quickly it works, how intense the contractions feel, and how the body responds. Misoprostol’s role is to help initiate labor by preparing the cervix and stimulating uterine activity, especially when the body hasn’t started labor on its own.
Read More: How to Thicken Uterine Lining in 48 Hours: Fertility-Safe Tips Backed by Science
What Does Misoprostol Pain Feel Like?

The pain from misoprostol-induced contractions varies from person to person, but most describe it as more intense than natural early labor. The difference often lies in the suddenness and pattern of the pain rather than the pain itself.
Descriptions of Misoprostol-Induced Pain:
- Strong, period-like cramps: The pain often begins in the lower abdomen, resembling menstrual cramps but stronger and more persistent.
- Diffuse, non-cyclical pain: Instead of having distinct peaks and rests, the pain can sometimes feel continuous, especially early on.
- Abrupt onset: Many people report that the contractions come on quickly, leaving little time to mentally or physically adjust.
This abrupt start can create an emotional response, too, making the pain feel sharper because the brain hasn’t yet released as many natural endorphins to buffer it.
Factors That Influence Pain Experience
- Dosage and timing: Higher or more frequent doses can intensify contractions, increasing both pain and effectiveness.
- Route of administration: Vaginal misoprostol generally leads to stronger uterine activity than oral dosing.
- Baseline cervical status: A firm, closed cervix may lead to more painful contractions as the uterus works harder to initiate dilation.
- Body’s sensitivity: Everyone’s pain tolerance and uterine responsiveness differ. Some will find misoprostol manageable; others may find it overwhelming.
While both natural and induced contractions serve the same purpose, misoprostol can produce a sensation of unrelenting pressure, which differs from the gradual rise and fall seen in spontaneous labor.
How Do Natural Labor Contractions Feel?

Spontaneous labor begins when your body releases a carefully orchestrated sequence of hormones, setting in motion a gradual, rhythmical process designed to help you adjust physically and mentally. Unlike the abrupt onset of misoprostol-induced contractions, natural labor usually allows for a more gradual escalation of intensity, giving you time to adapt and respond.
Understanding how natural contractions feel can help you recognize early labor signs, reduce fear of the unknown, and better distinguish between spontaneous and induced labor sensations.
Hallmarks of Natural Contractions:
Starts Slow and Soft
In early labor, contractions typically start as mild sensations that may go unnoticed at first. They often feel like:
- Dull, achy cramps low in the abdomen or back.
- A sensation of tightening or pressure that comes and goes.
- Discomfort that resembles menstrual cramps or mild indigestion.
At this stage, contractions are usually short (30–45 seconds) and spaced 10 to 20 minutes apart. Many people can continue daily activities or even sleep through them in early labor. The gradual start gives your brain time to begin releasing endorphins, your body’s natural painkillers, which help you stay calm and focused.
Wave-Like Rhythm
One of the defining features of natural contractions is their patterned, wave-like rhythm. Each contraction typically has three distinct phases:
- Build-up (ascending phase): The sensation slowly intensifies over several seconds.
- Peak: The most intense portion of the contraction, lasting a few seconds.
- Release (descending phase): The pain fades, offering a clear sense of relief before the next one begins.
This rhythm creates a predictable pain pattern, which many people find helpful for coping. Knowing that a contraction will peak and then subside gives you moments to breathe, regroup, and recover, something often missing in the early stages of induction.
Progressively Intensifies
As labor advances, contractions gradually become:
- Longer (lasting 60–90 seconds)
- Stronger (with deeper pressure or cramping)
- Closer together (every 3–5 minutes)
This transition from early to active labor doesn’t usually happen all at once. Instead, the body slowly increases oxytocin production, which enhances both the strength and frequency of contractions while also supporting emotional resilience through rising endorphin levels.
By the time active labor is underway, many people describe the pain as deep and powerful, but not chaotic. It often feels more purposeful than frightening because the gradual build-up allows your body to catch up and cope.
More Physiological Support
In spontaneous labor, your body orchestrates a delicate hormonal symphony that helps regulate the pace of labor and your emotional state. The key players include:
- Oxytocin: Stimulates contractions and promotes bonding and calmness.
- Endorphins: Your body’s natural opioids, which blunt pain perception and produce a euphoric or “zoned in” feeling.
- Adrenaline: Released in small amounts during transition to help with energy and alertness.
Together, these hormones balance stress with strength. Unlike the more mechanical stimulation of induced labor, natural labor is a hormonal cascade that adapts moment by moment to your body’s cues.
People often report feeling “in the zone” during active labor, a state where the body takes over and mental focus narrows. This altered awareness helps manage intense contractions and allows you to work with your body instead of fighting against it.
Other Sensory Characteristics of Natural Labor
- Pressure, not just pain: As the baby descends, many describe a growing pressure in the pelvis or rectum, sometimes more intense than the contractions themselves.
- Radiating sensations: Discomfort may extend into the thighs, hips, or back, especially if the baby is in a posterior position.
- Intermittent clarity: Between contractions, many people feel mentally alert and physically relaxed. These breaks are crucial for emotional stamina and pain coping.
In summary, Natural labor contractions are intense but often more predictable, rhythmic, and supported by your body’s own chemistry. The slow escalation, hormonal balance, and physical feedback help many people cope better, even when the pain becomes significant.
Key Differences Between Misoprostol and Natural Labor Contractions

When it comes to inducing labor or managing miscarriage, Misoprostol is a commonly used medication that triggers uterine contractions. But these contractions often feel quite different from those experienced during natural labor. Understanding the key differences between the two can help women prepare physically and emotionally for what to expect.
From the onset and intensity to how the body responds, each type of contraction carries its own pattern and experience. Here’s a breakdown of how Misoprostol-induced contractions compare to those of natural labor.
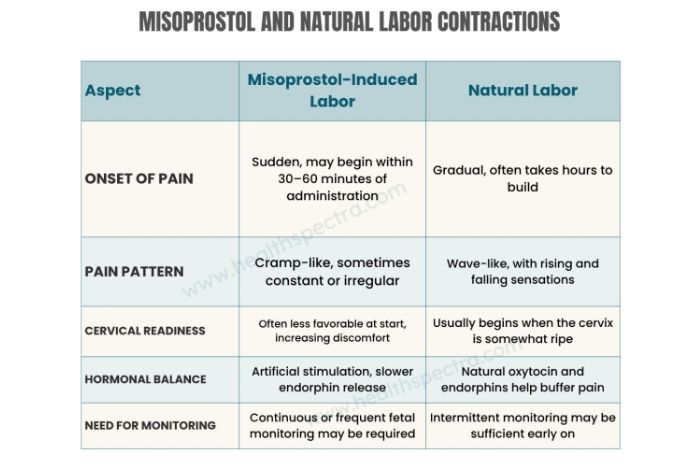 In essence, Misoprostol contractions can feel more sudden, irregular, and relentless in early labor, especially when the cervix isn’t yet ready.
In essence, Misoprostol contractions can feel more sudden, irregular, and relentless in early labor, especially when the cervix isn’t yet ready.
How Long Does It Take for Misoprostol to Start Active Labor?
Labor is officially considered “active” when contractions are regular and strong, and cervical dilation has progressed beyond 4–6 cm.
Typical Timeline with Misoprostol:
- Most people begin experiencing contractions within 30 to 90 minutes of the first dose.
- However, active labor may take 6 to 24 hours, or even longer, depending on how ready the cervix is.
- Those with prior vaginal deliveries or a partially dilated cervix may progress much faster.
Misoprostol is usually administered every 4 to 6 hours up to a certain maximum number of doses. If there’s minimal response after several rounds, other interventions may be added.
When Misoprostol Alone Isn’t Enough:
- Oxytocin (Pitocin): A synthetic form of oxytocin may be used via IV to strengthen and regulate contractions.
- Amniotomy: If the cervix is dilated but labor stalls, breaking the water may speed things up.
- Foley Balloon: Sometimes used alongside misoprostol to mechanically dilate the cervix.
Every labor follows its own path. Some people respond quickly to the first dose, while others require multiple interventions over 24–48 hours.
Managing Pain During Misoprostol Induction

Pain is an expected part of labor, but that doesn’t mean you have to suffer through it. There are multiple options, both non-medical and medical, to help you manage pain during misoprostol induction.
Non-Medical Strategies
- Positioning: Upright or forward-leaning positions may reduce pressure and help with cervical dilation.
- Movement: Gentle walking, swaying, or sitting on a birth ball can reduce tension and pain perception. Encouraging women to assume upright positions or to walk during the first stage of labour reduces the duration of labour and is associated with a reduced risk of caesarean delivery and need for epidural analgesia.
- Heat therapy: A warm shower or heating pad on the back can soothe muscles and cramping.
- Focused breathing: Deep, slow breaths help release tension and activate the parasympathetic nervous system.
- Visualization or hypnosis: Mental imagery can promote relaxation and distract from contraction pain.
Medical Pain Relief
- Epidural anesthesia: Provides profound pain relief and is especially useful during intense or prolonged induced labor.
- IV opioids (e.g., fentanyl): Offer moderate relief and can be used in earlier stages before epidural placement.
- Nitrous oxide: Fast-acting and allows self-administration, although it’s not as effective for stronger contractions.
- Acetaminophen or NSAIDs: Sometimes used in very early labor for mild discomfort, but with limited effect on true contractions.
Pain relief is not a sign of weakness; it’s a tool. You can adapt your plan as labor progresses and choose what’s right for your body and mind.
Read More: When Is the Best Time to Get an Epidural During Labor? What Experts Recommend
When to Contact Your Care Team
While misoprostol is generally safe, you should immediately alert your provider if you experience any of the following:
Signs of Concern:
- Unmanageable pain: If your pain is continuous, unbearable, or unrelieved by usual measures.
- Hyperstimulation (tachysystole): More than 5 contractions in 10 minutes, lasting over 2 minutes, or occurring with little to no rest between.
- Fetal distress: Changes in fetal heart rate or significantly reduced fetal movement.
- Heavy bleeding: Flow heavier than a period, presence of large clots, or signs of placental abruption.
- Signs of infection: Fever, chills, foul-smelling discharge, or rapid heart rate.
Don’t second-guess your instincts. If something feels wrong or unusual, speak up immediately. Your care team is there to support and protect both you and your baby.
Conclusion
Pain during misoprostol induction can feel different from the ebb and flow of natural labor, but “different” does not mean wrong, weaker, or less valid. For some, induced contractions are sharper and less rhythmic; for others, they’re manageable and efficient. What remains constant is this: every labor is personal, and every birth is powerful.
What truly matters is that you walk into the process informed, supported, and prepared, knowing that your voice, your choices, and your comfort are all essential parts of the journey.
You are not passive in this process. You have:
- Tools to manage the pain.
- Options to shape your care.
- The right to ask questions and be heard.
Whether your labor starts naturally or with a small white tablet, it’s the strength with which you meet it that defines your experience, not the method by which it begins.
Your labor isn’t less meaningful because it was induced. It’s meaningful because it’s yours.
And when the final contraction fades and your baby is in your arms, it won’t matter how labor started, only that you faced it with courage, clarity, and power.
From medication to meeting your baby, this is still your story. And it ends in triumph.
References
- https://pmc.ncbi.nlm.nih.gov/articles/PMC2760893/
- https://www.ncbi.nlm.nih.gov/books/NBK538944/
- https://medlineplus.gov/druginfo/meds/a689009.html
- https://go.drugbank.com/drugs/DB00929
- https://www.heyjane.com/articles/do-abortions-hurt
- https://www.medicalnewstoday.com/articles/325598
- https://my.clevelandclinic.org/health/treatments/21899-medical-abortion
- https://my.clevelandclinic.org/health/symptoms/contractions
- https://www.pregnancybirthbaby.org.au/giving-birth-contractions
- https://www.whattoexpect.com/pregnancy/symptoms-and-solutions/labor-contractions.aspx
- https://www.ncbi.nlm.nih.gov/books/NBK538944/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6513439/
In this Article





















