Are you trying to conceive but not getting the results you want? You may wonder when it’s time to seek professional help.
The process of trying to conceive (TTC) can be filled with hope, but also frustration, especially when each cycle passes without a positive result. Most couples don’t know how long they should try before consulting a fertility specialist, or if their struggles mean something is serious.
This article will help you understand the signs if you require fertility assistance, provide a timeline of fertility testing, and give an idea of what to expect during an infertility appointment.
Read More: Semen Quality Is Declining Worldwide – What Can Men Do to Protect Their Fertility?
When to See a Fertility Specialist

When it comes to fertility, time matters. Age plays a major role in determining when to take the next step.
Women under 35: If you’ve been having regular, unprotected sex for 12 months without conceiving, it’s time to schedule a fertility evaluation. This is the standard timeline recognized by most fertility experts.
Women aged 35–39: If you’ve been trying for 6 months or more without success, don’t delay. Age-related fertility decline begins in the mid-30s, so it’s crucial to act sooner rather than later.
“Women above 35 must consult a fertility specialist if they are trying to get pregnant for six months, without success,” Dr. Shreya Gupta, Fertility Specialist at Birla Fertility and IVF, Lucknow, India.
Women 40 and older: For this group, it is advisable to see a reproductive endocrinologist right away—even if you have not been trying for long. ReproArt Fertility states that early assessment can preserve such choices as egg freezing or IVF before ovarian reserve is reduced further.
And don’t forget—these rules apply no matter how well you feel or how regular your periods are. Fertility is complicated, and delicate problems often won’t show up without medical analysis.
Read More: How BPA Exposure in Everyday Products Could Be Hurting Your Fertility
Medical Conditions That Warrant Early Evaluation

Even if you have not reached the TTC timeline indicated above, some medical conditions are red flags for earlier intervention.
If you or your partner experiences any of the following, it’s best to consult a specialist sooner rather than later:
- Irregular or missing periods may be a symptom of anovulation, thyroid issues, or hormonal imbalance.
- Endometriosis or PCOS are the two conditions that can affect ovulation and implantation success directly.
- Pelvic inflammatory disease (PID) or any previous infections can lead to tubal obstruction or the formation of scar tissue.
- Uterine fibroids or ovarian cysts can hinder conception or cause miscarriage.
- Multiple miscarriages, such as two or more pregnancy losses, require a complete reproductive health assessment.
- Male factor infertility includes conditions such as low sperm count, poor motility, or testosterone imbalance, all of which can contribute to TTC delays.
- Previous cancer therapy or pelvic surgeries can impact reproductive organs or hormonal systems.
Don’t wait in these situations. Early fertility testing can reveal correctable problems and enhance your conception success.
When It’s More Than “Just Stress”
It’s natural and common to downplay fertility challenges as a temporary issue. Friends may tell you, “Relax, it’ll work out.” But this attitude can stall essential care.
Here’s reality: Stress isn’t the root of infertility, but infertility can induce stress.
If your cycles are always irregular, painful, or accompanied by abnormal symptoms, don’t dismiss them. According to Cloudnine Fertility, emotional suffering is typically the result of physical problems underneath. And if those problems remain untreated, your mental well-being as well as fertility results may suffer.
Getting an infertility consultation doesn’t mean jumping into treatment. It means understanding why things aren’t working and what you can do about it.
What a Fertility Specialist Can Do
Once your history is reviewed, your doctor will likely recommend several tests to assess reproductive health in both partners:
Hormone Panels:
Blood tests are done at specific times in the cycle to check levels of:
- Follicle-stimulating hormone (FSH) and luteinizing hormone (LH) regulate ovulation
- Anti-Müllerian hormone (AMH) – gives an estimate of ovarian reserve
- Estradiol and progesterone – help assess ovulatory function
- Prolactin – high levels can interfere with ovulation
- Thyroid hormones (TSH, T3, T4) – imbalances can impact fertility
- Testosterone and other androgens, especially if PCOS is suspected
Ovulation Tracking:

Your cycle may be monitored with blood tests and transvaginal ultrasounds to check for:
- Follicular growth
- Ovulation timing
- Luteal phase support
Semen Analysis:
For male partners, this test measures:
- Sperm count – total number of sperm in a sample
- Motility – how well sperm move
- Morphology – shape and structure
- Volume and pH – overall health of semen
Hysterosalpingography (HSG): A radiographic test with special X-rays using contrast dye to evaluate if fallopian tubes are open and if the uterus is shaped normally.
Pelvic Ultrasound:
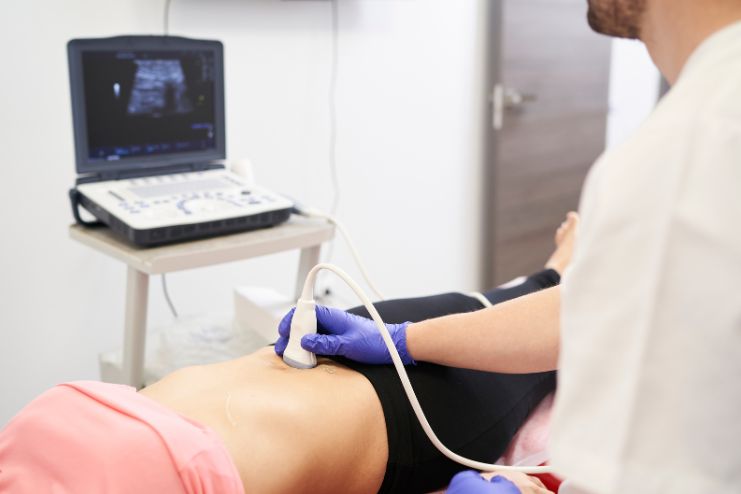
Used to detect:
- Ovarian cysts or low antral follicle count (an indicator of ovarian reserve)
- Uterine fibroids, polyps, or abnormalities
- Endometriosis signs (such as endometriomas)
- Additional testing may include:
- Sonohysterography or hysteroscopy for closer uterine evaluation
- Genetic screening for both partners
- Laparoscopy to detect and treat endometriosis or pelvic adhesions
Personalized Treatment Options
After testing is complete, your fertility expert will develop an individualized treatment plan based on your test results, age, and TTC objectives. Treatment plans may include:
- Lifestyle & Nutrition Guidance: Weight management, stress reduction, better sleep, and diet improvement to enhance hormone balance and ovulation.
- Supplements: You may be advised to take:
- CoQ10 for egg health
- Myo-inositol for PCOS-related insulin resistance
- Prenatal vitamins with folic acid and other fertility-boosting nutrients
- Vitamin D or omega-3s if deficiencies are noted
- Medications:
- Clomiphene citrate(Clomid) or letrozole to induce ovulation
- Gonadotropin injections for stronger stimulation in IUI/IVF
- Metformin if insulin resistance is impacting ovulation
Intrauterine Insemination (IUI):
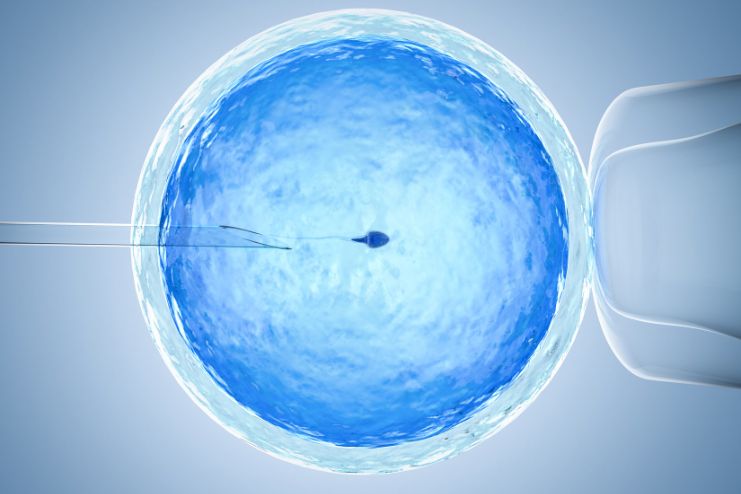
A procedure where sperm is washed, concentrated, and directly inserted into the uterus during ovulation to increase the chances of fertilization.
In Vitro Fertilization (IVF):
In In Vitro Fertilization (IVF), the eggs are retrieved, fertilized in a laboratory, and then implanted into the uterus. IVF may be recommended if:
- Tubes are blocked
- There’s severe male factor infertility
- Previous treatments have failed
Fertility Preservation: If you’re not ready to conceive now but want to preserve your options, egg freezing or embryo freezing may be offered, especially for women in their early to mid-30s or those facing medical treatments that affect fertility.
Emotional Support & Counseling: Fertility struggles can be emotionally taxing. Many clinics offer fertility coaches or referrals to therapists who specialize in reproductive health.
Read More: Know The Infertility Causes And Treatments
Don’t Wait If You Feel Something’s Off

If your gut is telling you something’s not right, listen to it.
You don’t have to “earn” a fertility consultation by suffering in silence. Early intervention results in less complicated, minimally invasive treatments. And more importantly, it gives peace of mind.
According to Healthcare Utah, seeing a specialist doesn’t indicate you are out of options—it means you are considering them. If you’re experiencing early signs of infertility or simply need reassurance, a fertility specialist can interpret what your body is communicating.
Takeaway

Consulting a fertility specialist isn’t a last resort—it’s an active step toward clarity, options, and hope. It’s about taking uncertainty, turning it into understanding, and changing the “what-ifs” in a clear direction.
No matter what your path may be—whether it involves minor hormonal adjustments, lifestyle changes, or high-tech fertility treatments—a specialist will help you make informed choices based on your body, timeline, and goals.
You don’t have to keep guessing, waiting, or carrying the weight alone. Expert guidance provides more than medical insight—it provides reassurance, strategy, and a renewed sense of control.
You don’t have to do this alone. You deserve answers, expert care, and a plan that gives you control over your fertility journey.
References
- https://naitre.com/blogs/journal/the-psychological-impact-of-trying-to-conceive-ttc-understanding-navigating-and-supporting-mental-health
- https://healthcare.utah.edu/fertility/when-should-you-see-a-fertility-specialist
- https://extendfertility.com/female-fertility-supplements/
- https://www.ncbi.nlm.nih.gov/books/NBK559292/
- https://www.newhopefertility.com/blog/when-to-see-a-fertility-specialist-5-signs-its-time/
- https://healthcare.utah.edu/fertility/when-should-you-see-a-fertility-specialist
- https://www.newhopefertility.com/blog/when-to-see-a-fertility-specialist-5-signs-its-time/
- https://www.cedars-sinai.org/provider/jessica-chan-2988261.html
In this Article





















