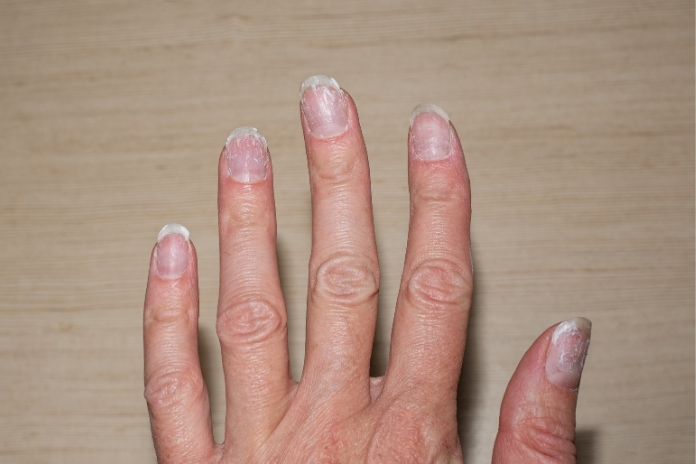
Not all nail changes are caused by fungus. If your nails are discolored, thickened, crumbling at the edges, or have tiny pits like someone took a pin to the surface, and antifungal treatments haven’t helped, there’s a good chance you’re not dealing with a fungal infection at all. You might be dealing with nail psoriasis.
Nail psoriasis is a chronic, inflammatory condition that affects the nails, and it’s more common than most people realize. It impacts up to 50% of people with plaque psoriasis, and a staggering 80% of those with psoriatic arthritis. Sometimes it’s the first sign of psoriasis. Other times, it shows up later, long after skin symptoms have appeared. And in some cases, nail changes might be the only sign.
This condition can affect both fingernails and toenails, and it’s not just a cosmetic issue. Nail psoriasis can cause pain, make basic tasks like buttoning a shirt or walking uncomfortable,
lead to emotional distress or self-consciousness.
The tricky part? It’s often misdiagnosed as a fungal infection or dismissed as “just brittle nails.” But the treatment path is completely different. That’s why understanding what nail psoriasis really looks like, and what’s happening beneath the surface, matters.
In this article, we’ll break down everything you need to know:
- What is nail psoriasis?
- How to spot the signs?
- What causes it?
- And which treatments actually work, from at-home care to prescription therapies that target the root of the problem.
Because once you know what you’re dealing with, you can finally stop guessing and start healing.
What Is Nail Psoriasis?
Nail psoriasis is a form of psoriatic disease where the immune system goes off track and attacks healthy nail tissue, leading to inflammation, distortion, and irregular nail growth. Just like skin psoriasis, it’s fueled by an immune malfunction, particularly an overproduction of skin cells in the nail matrix (the part responsible for nail formation) and the nail bed (the skin beneath the nail).
Psoriasis is a common skin condition that leads to the development of very dry and flaky skin. It can spread to the nails when the body’s white blood cells target your tips.
“The inflammation triggers an acceleration in the production of cells, known as keratinocytes,” explains Dr. Purvisha Patel, MD. “In the fingernails and toenails, the overproduction of keratinocytes can cause thickening, malformation, and discoloration as the cells are produced faster than they can be shed.”
The result? Nails that may pit, thicken, crumble, lift from the nail bed, or become discolored, sometimes resembling a fungal infection, but with different roots.
Nail psoriasis can show up in a few ways:
- On its own, without skin plaques.
- Alongside typical skin psoriasis.
- Or as part of psoriatic arthritis, where joints are also affected.
In fact, nail changes are often one of the earliest warning signs of psoriatic arthritis. Studies show that up to 80% of people with psoriatic arthritis have nail involvement, which makes early recognition especially important for diagnosis and treatment planning.
Though not life-threatening, nail psoriasis can seriously disrupt daily life. It can make simple tasks, like typing, gripping a pen, tying shoelaces, or walking in closed shoes, painful and frustrating. And because nails are always visible, it can also take a toll on confidence and self-image.
Understanding what’s behind the changes in your nails is the first step toward managing them and protecting your joints in the process.
Nail Psoriasis Symptoms
The symptoms of nail psoriasis vary depending on which part of the nail is affected, the nail matrix (the root under the skin) or the nail bed (the skin beneath the nail plate).
- Nail pitting: These are tiny depressions or dents on the surface of the nail, caused by defective keratinization. It’s one of the hallmark signs of psoriasis of the fingernails.
- Discoloration: Yellow-brown spots (known as oil-drop or salmon patches) often appear beneath the nail plate. Nails may also turn white, yellow, or reddish.
- Thickening or crumbling: As inflammation disrupts normal nail growth, the nail can become brittle, rough, and thickened, sometimes resembling fungal nail disease.
- Onycholysis: This refers to the nail lifting or separating from the nail bed, starting at the tip and moving inward.
- Subungual hyperkeratosis: Chalky debris builds up under the nail due to overproduction of skin cells.
- Pain and tenderness: Inflamed nail beds or matrices can cause aching, especially when pressure is applied.
- Functional issues: Tasks requiring grip, fine motor skills, or walking (in toenail cases) can become painful.
- Confusion with fungal infections: Nail psoriasis is frequently mistaken for onychomycosis. Misdiagnosis can delay appropriate treatment.
What Causes Nail Psoriasis?
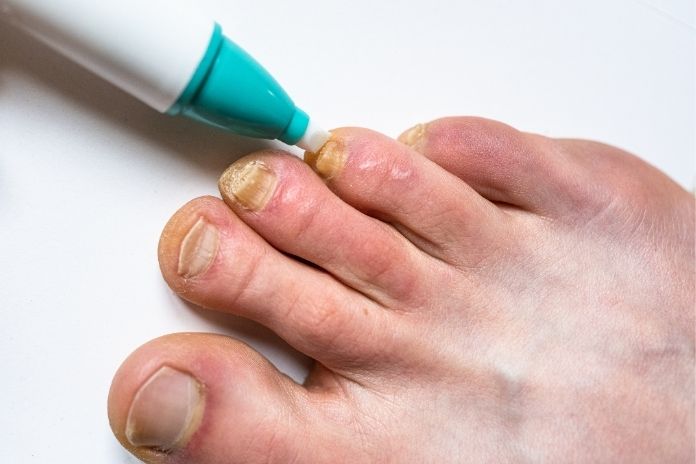
The root cause of nail psoriasis lies in immune system dysfunction. In people with psoriasis, immune cells called T-cells mistakenly attack healthy skin or nail cells, triggering inflammation and rapid cell turnover.
Contributing Factors:
- Genetics: Psoriasis runs in families. If a parent or sibling has psoriasis, your risk increases significantly.
- Immune system dysregulation: Autoimmune activity causes skin and nail cells to multiply faster than normal, leading to buildup and nail distortion.
- Triggers:
- Injury to the nail or cuticle: A phenomenon known as the Koebner response, where trauma leads to psoriasis flare-up at the site.
- Stress: Emotional or physical stress can exacerbate psoriasis, including its nail form.
- Infections or illness: Viral or bacterial infections may trigger or worsen symptoms by disturbing the immune balance.
Unlike fungal infections, nail psoriasis is not contagious. However, both conditions can coexist, making diagnosis and treatment more complex.
A study published in Acta Dermato-Venereologica found that the HLA-Cw6 allele is the most strongly associated genetic risk factor for psoriasis, present in approximately 40–60% of patients.
How Is Nail Psoriasis Diagnosed?
Diagnosis is usually clinical, meaning a dermatologist will evaluate your nail’s appearance and your personal and family history of psoriasis.
Diagnostic Tools:
- Clinical exam: Most dermatologists can identify nail psoriasis based on characteristic signs like pitting, oil spots, or onycholysis.
- KOH prep or fungal culture: To rule out fungal infections, a potassium hydroxide (KOH) scraping or lab culture may be performed.
- Nail biopsy: In rare or unclear cases, a small tissue sample from under the nail may be taken and analyzed microscopically.
Proper diagnosis is key; nail psoriasis doesn’t respond to antifungal treatment, and misidentifying it can delay care.
Read More: Top 5 Foods to Cure Psoriasis
Treatment Options for Nail Psoriasis

Nail psoriasis is notoriously difficult to treat due to the slow growth of nails and limited access to the nail bed and matrix. However, there are several treatment strategies available, depending on the severity of the condition and whether other areas (like skin or joints) are involved.
a. Topical Treatments
First-line treatments for mild to moderate cases.
- Topical corticosteroids: Potent options like clobetasol propionate reduce inflammation but need careful application to avoid thinning the skin around the nail.
- Calcipotriol: A vitamin D analog that slows down skin cell turnover and helps with nail thickening and pitting.
- Tazarotene: A topical retinoid that may help normalize keratinocyte differentiation.
Application Tips:
- Apply under the nail tip or around the nail fold for best absorption.
- Use occlusion (covering with tape or a bandage) to increase penetration.
- Expect results slowly; improvements can take 3–6 months or more.
Read More: Top 8 Psoriasis Creams: Soothing Skincare Solutions for Flare-Ups
b. Systemic Medications
Recommended when topical options fail or if psoriasis also affects skin or joints.
- Methotrexate: An immunosuppressant drug that reduces inflammation.
- Cyclosporine: Suppresses overactive immune cells.
- Acitretin: An oral retinoid that can improve nail appearance but may take months and has more side effects.
These drugs affect the entire immune system, so they’re used when nail psoriasis is part of a broader psoriatic disease picture.
c. Biologic Therapies
Biologics are newer, highly targeted medications that block specific immune pathways. They are often the most effective treatment for nail psoriasis, especially when psoriatic arthritis is also present.
Examples:
- Adalimumab (Humira)
- Ustekinumab (Stelara)
- Secukinumab (Cosentyx)
- Ixekizumab (Taltz)
These agents work by blocking tumor necrosis factor (TNF) or interleukins like IL-12/23 or IL-17, key drivers of psoriatic inflammation.
Clinical trials show that biologics significantly improve nail symptoms in as little as 12–16 weeks, with continued improvement over time. However, they are expensive and typically reserved for moderate to severe cases.
d. Intralesional Corticosteroid Injections
This involves injecting steroids directly into the nail matrix using a fine needle.
- Pros: Can improve pitting and thickening.
- Cons: Painful, risk of infection, and must be repeated every few weeks.
Used selectively for severe or resistant nail involvement when other treatments are ineffective or contraindicated.
e. Laser and Light Therapies
- Excimer laser: Targets inflammation with UVB light.
- PUVA therapy: Combines UVA light with a photosensitizing medication (psoralen).
These are not first-line options but may be used in specific cases, often in combination with topical or systemic therapies.
Home Care and Nail Management Tips

While medical treatments address the underlying disease, daily care and protection strategies can minimize damage and discomfort.
Dos:
- Keep nails short and filed: Reduces trauma and risk of lifting or breaking.
- Moisturize regularly: Hydrated cuticles and nail beds are less prone to cracking.
- Use gloves: Protect your hands from harsh cleaners, soaps, or gardening tools.
- Opt for gentle nail products: Avoid acetone, nail hardeners, and acrylic nails, which can worsen symptoms.
Read More: Manage Psoriasis With Essential Oils
Don’ts:
- Don’t bite your nails or pick at the cuticles; this can trigger flares via the Koebner phenomenon.
- Don’t assume it’s fungal without testing; many people waste months on ineffective antifungal treatments.
Consistent home care supports the medical treatment process and may prevent future flares.
When to See a Dermatologist
Nail psoriasis often progresses slowly, but early intervention can prevent permanent nail damage or deformity. You should see a dermatologist if:
- Nail changes last longer than 6 weeks without improvement.
- You experience pain, swelling, or difficulty using your hands or feet.
- You already have psoriasis or psoriatic arthritis and notice new nail symptoms.
- Over-the-counter treatments aren’t working.
The longer nail psoriasis goes untreated, the harder it can be to reverse structural changes in the nail unit.
Final Thoughts
Nail psoriasis is more than a cosmetic issue; it’s a sign of immune system dysfunction that can affect daily life and overall health. It can be mistaken for a fungal infection, especially in its early stages, and that confusion often delays proper treatment.
But with a thoughtful approach, combining prescription treatment, daily nail care, and trigger management, nail health can significantly improve. Whether you’re managing mild pitting or dealing with more severe nail damage, progress is possible. It just takes patience and consistency.
If you’re seeing signs of nail psoriasis, don’t wait for it to worsen. Talk to a dermatologist and get started on a care plan that works for you.
References
- https://my.clevelandclinic.org/health/diseases/22841-nail-psoriasis
- https://www.aad.org/public/diseases/scaly-skin/psoriasis/diagnosis-and-treatment-of-psoriasis/what-is-nail-psoriasis-and-how-can-i-treat-it
- https://www.webmd.com/skin-problems-and-treatments/psoriasis/nail-psoriasis
- https://www.ncbi.nlm.nih.gov/books/NBK559260/
- https://www.psoriasis.org/hands-feet-nails/
- https://en.wikipedia.org/wiki/Psoriatic_onychodystrophy
- https://emedicine.medscape.com/article/1107949-overview
- https://my.clevelandclinic.org/health/diseases/22841-nail-psoriasis
- https://www.aad.org/public/diseases/scaly-skin/psoriasis/diagnosis-and-treatment-of-psoriasis/what-is-nail-psoriasis-and-how-can-i-treat-it
- https://www.psoriasis.org/hands-feet-nails/
- https://www.webmd.com/skin-problems-and-treatments/psoriasis/nail-psoriasis
- https://www.mayoclinic.org/diseases-conditions/psoriasis/symptoms-causes/syc-20355840
- https://dermnetnz.org/topics/nail-psoriasis
- https://my.clevelandclinic.org/health/diseases/6866-psoriasis
- https://emedicine.medscape.com/article/1107949-overview
In this Article