Graves’ disease happens when the immune system misfires and pushes the thyroid into overdrive. Instead of defending you from infections, immune cells begin producing antibodies that behave like a stuck accelerator pedal. The thyroid, the organ that normally sets the rhythm for metabolism, temperature, and energy use, starts releasing far more hormones than your body actually needs.
When that surge hits, everything speeds up: heart rate, digestion, heat production, mental activity, and even how quickly your muscles burn energy. These shifts form many of the classic Graves’ disease symptoms, from anxiety and weight loss to tremors, heat intolerance, and sleep disruption. Endocrinologists often point out that Graves’ disease is the most common cause of hyperthyroidism in adults, especially women between 30 and 60.
The American Thyroid Association estimates that hyperthyroidism affects about one percent of the population, and Graves’ disease accounts for most of those cases. Early detection matters because it doesn’t just touch the thyroid; it can affect the heart, eyes, muscles, skin, and emotional health.
Understanding what causes Graves’ disease is part of the puzzle. Genetics, immune dysregulation, stress, infections, smoking, and high iodine exposure all play a role, creating the conditions in which the immune system tips into overactivity.
This guide breaks down how the condition develops, how it presents in daily life, and the evidence-based Graves’ disease treatment options doctors use to restore balance. It also looks at long-term management, lifestyle support, and what recovery usually feels like once the thyroid begins to stabilize.
Key Takeaways: What You’ll Learn
- What Graves’ disease actually is and how it disrupts normal thyroid function.
- The autoimmune and genetic mechanisms behind the condition.
- Common early symptoms and physical signs to look out for.
- How doctors diagnose it using lab tests and imaging.
- The major treatment options include medications, radioactive iodine, and surgery.
- Practical lifestyle strategies that support recovery.
- Why long-term monitoring remains essential, even after remission.
What Is Graves’ Disease?
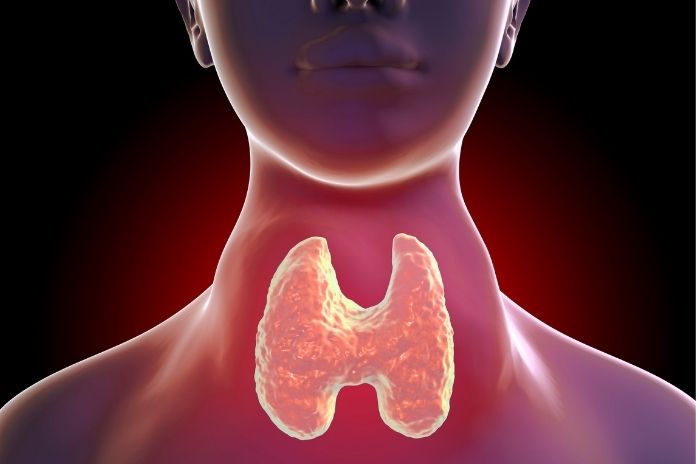
At its core, Graves’ disease is an autoimmune disorder characterized by uncontrolled thyroid hormone production. Instead of regulating hormones through the pituitary gland, the body produces thyroid-stimulating immunoglobulins (TSI), antibodies that latch onto thyroid cells and instruct them to continue producing more hormone.
With rising levels of triiodothyronine (T3) and thyroxine (T4), the metabolism accelerates. The cardiovascular system works harder, heat production increases, the gut moves faster, and the brain becomes overstimulated.
The thyroid hormone affects virtually every organ system in the body, including the heart, CNS, autonomic nervous system, bone, GI, and metabolism. Due to this hormonal overload, people often chalk up early signs, like anxiety, sweating, or unexplained weight loss, to stress or lifestyle changes before realizing something deeper is going on.
How Common Is It?
According to MedlinePlus Genetics, Graves’ disease is fairly common; roughly one in every two hundred people is affected, and women develop it far more frequently than men, possibly due to hormonal factors. Estimates suggest women are five to ten times more likely to develop Graves’ disease than men, a pattern researchers link to the higher overall susceptibility of women to autoimmune disorders.
A family history also increases risk. A recent population-based study found that having a first-degree relative with Graves’ disease gave a 3.39× higher risk (hazard ratio 3.39). This reinforces the idea that genes help set the stage, while environment and immune triggers flip the switch.
Causes and Risk Factors of Graves’ Disease

Graves’ disease doesn’t appear out of nowhere. It is the result of an immune system that starts behaving unpredictably, a genetic background that makes that misfire more likely, and environmental triggers that push the thyroid into overdrive.
When you break it down, the condition follows a clear pattern: the immune system initiates it, genes set the stage, and lifestyle or environmental factors flip the switch. Here’s how each piece fits together.
Autoimmune Cause
The core driver of Graves’ disease is the production of thyroid-stimulating immunoglobulins (TSI). These antibodies imitate thyroid-stimulating hormone (TSH) and continually push the thyroid to produce T3 and T4.
What actually triggers that initial misfire is still being uncovered. Although most evidence points to a blend of genetic predisposition and environmental pressures.
Read More: Managing Autoimmune Diseases: The Role of Diet and Exercise
Genetic Predisposition
Graves’ disease is not necessarily hereditary, but genes can make the immune system more prone to overreact.
Some of the most discussed genes include:
- HLA-DR variants, which influence immune recognition.
- CTLA-4 is a key regulator that prevents immune overactivation.
- TSHR gene polymorphisms, which affect the receptor targeted by TSI.
These genetic patterns don’t guarantee disease; they simply create a more reactive immune landscape. The NIH notes that people with relatives who have autoimmune conditions like type 1 diabetes, celiac disease, Hashimoto’s thyroiditis, or rheumatoid arthritis carry a higher overall risk, suggesting shared genetic pathways across these disorders.
Environmental Triggers
Genetics might load the gun, but environmental factors often pull the trigger. Common triggers include:
- Significant emotional or physical stress.
- Smoking not only doubles the risk but also worsens Graves’ eye disease.
- Viral infections
- Pregnancy and postpartum immune shifts.
- Excess iodine from supplements or diet.
Stress is one factor that consistently stands out. A meta-analysis (2023) in BMC Endocrine Disorders found that stressful life events are significantly more common in people before they develop Graves’ disease, suggesting stress is an environmental trigger.
Stress can push an already-vulnerable immune system into overdrive, and while it isn’t the root cause of Graves’, it can accelerate the process in someone who’s at risk.
Who’s Most at Risk?
Drawing from National Institutes of Health data and endocrine research, risk is highest among:
- Women aged 30–60
- Smokers
- Individuals with a family history of autoimmune disorders.
- Those with high iodine intake.
- People are exposed to chronic stress or recurring infections.
Recognizing these patterns helps clinicians catch Graves’ earlier, especially when symptoms first appear as anxiety, weight loss, or heat intolerance rather than thyroid-related issues.
Common Symptoms of Graves’ Disease
A molecular review also says that in autoimmune thyroid disease, there’s a loss of immune tolerance with infiltration of T and B lymphocytes into the thyroid and production of antibodies against self-antigens like the TSH receptor.

Graves’ disease affects the body on multiple levels. Its symptoms rarely stay confined to one system. What starts as small changes can quickly grow into a pattern that feels impossible to ignore.
1. General Body Symptoms
Since thyroid hormones influence almost every metabolic process, symptoms can appear across different systems.
Some of the most common include:
- Unexplained weight loss despite eating normally or more than usual.
- Rapid or irregular heartbeat, often described as pounding or fluttering.
- Heat intolerance and constant sweating.
- Fine tremors, particularly in the hands.
- Anxiety, irritability, and trouble concentrating.
- Feeling constantly tired and overstimulated at the same time.
- Insomnia or difficulty staying asleep.
- Increased bowel movements or mild diarrhea.
Symptoms of hypothyroidism may emerge gradually and can be mistaken for signs of aging, depression, or stress. “That’s why diagnosis can be delayed,” says Chien-Hsiang Weng, MD, MPH, Clinical Associate Professor in the Department of Family Medicine. He adds, “We need to raise awareness that subtle neurologic symptoms may actually stem from the thyroid.”
2. Physical Changes
Beyond internal symptoms, Graves’ disease can lead to noticeable physical changes:
- Goiter (thyroid enlargement) creates a visible swelling in the neck.
- Thin, warm, or moist skin.
- Fine, brittle hair that breaks easily.
- Muscle weakness, especially in the thighs and upper arms.
These changes reflect how hard the body works to keep up with the heightened metabolic demand.
3. Eye Symptoms (Graves’ Ophthalmopathy)
About 25–30% of people with Graves’ develop eye involvement, known as Graves’ ophthalmopathy or thyroid eye disease.
Common symptoms include:
- Bulging or protruding eyes (exophthalmos).
- Gritty, dry sensation.
- Light sensitivity.
- Swelling or redness.
- Double vision.
This occurs when immune cells mistakenly target tissues behind the eyes, causing inflammation and tissue expansion. Eye symptoms do not always match thyroid hormone levels. In some people, the inflammation continues even after hormone levels stabilize.
Smoking is the strongest modifiable risk factor; studies show smokers have a four to eight times higher risk of severe eye involvement.
4. Skin Symptoms (Graves’ Dermopathy)
Less commonly, Graves’ disease can affect the skin. Pretibial myxedema is a condition that causes the skin on the shins or tops of the feet to become thick, reddish, and waxy. It’s usually painless and often mild, but it signals ongoing autoimmune activity.
Diagnosis: How Doctors Confirm Graves’ Disease

Graves’ disease can show up in many ways. Hence, doctors rely on a mix of physical signs, blood work, and imaging to confirm what’s going on. The goal is to understand whether the thyroid is overactive and identify the autoimmune trigger behind it.
1. Physical Exam
During evaluation, doctors look for:
- Enlarged thyroid gland.
- Rapid pulse or irregular heartbeat.
- Fine hand tremors.
- Eye bulging or swelling.
- Skin changes around the shins.
These clues, paired with the person’s symptoms, usually lead to immediate lab testing.
2. Blood Tests
Thyroid blood tests form the core of diagnosis. Common findings include:
- Low TSH, because the pituitary senses excessive thyroid hormones.
- High T3 and T4, confirming hyperthyroidism.
- Presence of TSI antibodies, the hallmark of Graves’.
Doctors may also check anti-thyroid peroxidase (anti-TPO) antibodies, which often appear in people with overlapping autoimmune thyroid conditions.
3. Imaging Tests
Imaging becomes important when blood test results are unclear or when doctors need to pinpoint the exact cause of hyperthyroidism.
- Radioactive iodine uptake (RAIU):Elevated uptake strongly supports Graves’, since the thyroid absorbs iodine aggressively when overstimulated.
- Thyroid ultrasound:Helps identify goiter, nodules, or other structural abnormalities.
According to the American Thyroid Association, RAIU testing (radioactive iodine uptake) is a key diagnostic tool. High uptake can point toward nodular overactivity (like toxic nodules), while very low uptake is a hallmark of thyroiditis.
Treatment Options for Graves’ Disease
Graves’ disease does not have a one-size-fits-all treatment plan. Doctors choose the approach based on age, severity, pregnancy status, eye involvement, and how the body responds over time. The goal is to control excess hormones, calm the autoimmune activity, and protect long-term health.
1. Anti-Thyroid Medications
Most newly diagnosed patients begin with medication. The two main drugs are:
- Methimazole (MMI) – first line for most adults.
- Propylthiouracil (PTU) – used in the first trimester of pregnancy or for other conditions.
These medicines block the thyroid’s ability to produce new hormone. Levels usually start improving within weeks. A standard treatment course lasts 12–18 months, and roughly 30–50 percent of patients achieve long-term remission.
Close monitoring matters because antithyroid drugs like methimazole can rarely affect liver function or lower white blood cell counts. According to a long-term review in Endocrine Practice, extended methimazole therapy for 5 or more years is both safe and associated with improved remission rates.
2. Radioactive Iodine Therapy (RAI)
Radioactive iodine (I-131) is a targeted treatment that gradually destroys overactive thyroid cells. It is taken orally and is one of the most common definitive options in the United States.
Advantages include:
- High success rate.
- No surgery required.
- Long-term control of hyperthyroidism.
Most patients develop hypothyroidism afterward, which is expected and easily managed with daily levothyroxine. RAI is avoided during pregnancy or breastfeeding. It can also worsen eye inflammation in people with Graves’ ophthalmopathy. In those cases, doctors often lean toward medication or surgery.
3. Thyroid Surgery (Thyroidectomy)
Surgery provides a rapid and permanent solution. It’s recommended for:
- Very large goiters causing pressure or swallowing issues.
- Severe eye disease, to prevent worsening.
- Patients who cannot tolerate medication.
- Pregnancy, when medications fail or are not tolerated.
After surgery, lifelong levothyroxine replaces natural thyroid hormone. When performed by an experienced surgeon, complication rates are low.
4. Managing Eye and Skin Symptoms
Eye and skin issues sometimes need a separate treatment plan.
For eye symptoms:
- Lubricating drops ease dryness.
- Steroids or immunosuppressive therapy reduce inflammation.
- Prisms or eye surgery may help with double vision.
- Orbital decompression surgery is used in severe cases.
For skin symptoms (pretibial myxedema):
- Topical corticosteroids may reduce thickening.
- Compression stockings can improve comfort.
Across all major endocrine guidelines, one point stands out: quitting smoking is the single most effective lifestyle change for reducing eye disease severity.
Lifestyle Tips for Living Well with Graves’ Disease

Lifestyle changes can’t shut down the autoimmune process, but they make the treatment journey easier and help keep symptoms under control. Think of it as building a steady foundation while your medical treatment does the heavy lifting.
- Balanced Diet: A balanced diet helps counter the strain that hyperthyroidism puts on your bones and metabolism. It gives you steady protein for muscle, calcium-rich foods for bone strength, enough vitamin D, and regular whole-food meals instead of extreme diets.
- Moderate Iodine Intake: Your thyroid uses iodine to make hormones, and Graves’ already pushes that system into overdrive. Avoid high-iodine supplements, kelp tablets, or seaweed-heavy diets unless your doctor says otherwise.
- Stress Management: Stress does not directly cause Graves’, but it can intensify symptoms. Techniques like yoga, mindful breathing, journaling, or guided meditation help calm the nervous system. Many patients also benefit from cognitive behavioral therapy, especially when anxiety or restlessness begins to feel overwhelming.
- Regular Sleep: Sleep becomes tricky because the body feels wired, restless, or overheated. Aim for a consistent bedtime routine, a cooler room, and limited screen time late at night. Short naps can help, but taking them earlier in the day keeps them from making insomnia worse.
- Limit Caffeine and Smoking: Caffeine adds fuel to symptoms like palpitations, tremors, and anxiety. Cutting back, even gradually, can make a noticeable difference. Smoking increases the risk and severity of eye disease in Graves’. Therefore, quitting becomes one of the most impactful choices you can make.
- Consistent Follow-Ups: Thyroid levels can swing quickly, especially in the early phases of treatment. Regular checkups and blood tests help your care team adjust medication before symptoms spike again.
“One thing that we know is stress can bring out Graves’ disease in patients, and traditionally, during wartime in Europe, the incidence of Graves’ disease would go up,” says Andrew Gianoukakis, professor of medicine at UCLA’s David Geffen School of Medicine.
Andrew adds, “Stress on a personal, national, or geographic level can increase the incidence of Graves’ disease. So it’s a combination of environmental factors and genetic factors without them having really been well worked out.”
At the end of the day, healthy habits won’t substitute for proper medical care. Research from Harvard Health notes that patients who commit to supportive routines often stabilize faster, feel more in control, and experience fewer ups and downs while their thyroid levels settle.
Prognosis: Can Graves’ Disease Be Cured?
Graves’ disease can enter remission, especially after a full course of medication. However, recurrence is common, particularly if treatment stops early, smoking continues, or stress remains unmanaged.
Long-term outlook depends on the treatment approach:
- Medication: Remission is possible, but relapse rates vary.
- Radioactive iodine: Permanent solution, though hypothyroidism is expected.
- Surgery: Immediate resolution of hyperthyroidism, with lifelong hormone replacement.
Most people live normal, active lives once their thyroid levels stabilize. The key is ongoing monitoring, because thyroid hormone needs can shift with age, pregnancy, medication changes, and autoimmune activity.
Quick Recap
Graves’ disease is an autoimmune condition where the immune system pushes the thyroid into overdrive, flooding the body with excess hormones. That surge affects almost every major system, which is why symptoms can feel scattered at first; weight loss, heat intolerance, anxiety, tremors, eye changes, and muscle weakness all come from the same hormonal disruption.
Doctors confirm the diagnosis through a clear pattern: low TSH, high T3 and T4, and the presence of TSI antibodies. Imaging tests add clarity when needed. Once identified, treatment is straightforward but personalized.
Some people stabilize on anti-thyroid medications, others opt for radioactive iodine, and a smaller group benefits most from surgery. Each route has its own rhythm and recovery curve.
What this really means is that Graves’ isn’t a lifelong hurdle. With the right treatment, steady follow-ups, and supportive lifestyle habits, most people regain balance and often reach remission. It takes patience because thyroid levels don’t settle overnight, but the outlook is overwhelmingly positive.
The key is staying consistent, listening to your body, and working closely with your healthcare provider, as hormone levels normalize, energy, mood, and quality of life usually follow right behind.
References
- Cleveland Clinic. (n.d.). Graves’ disease
- Mayo Clinic. (n.d.). Graves’ disease – Symptoms & causes
- Wikipedia contributors. (n.d.). Graves’ disease
- National Center for Biotechnology Information
- Apollo Hospitals. (n.d.). Graves’ disease
- Max Healthcare. (n.d.). What is Graves’ disease
- Medscape. (n.d.). Overview of Graves’ disease
- WebMD. (n.d.). Graves’ disease: Basics
- Physio-Pedia. (n.d.). Graves’ disease
- MedlinePlus. (n.d.). Hyperthyroidism. U.S. National Library of Medicine
- CARE Hospitals. (n.d.). Graves’ disease
- PatientsEngage. (n.d.). Graves’ disease: Causes & risk factors
- ADA (American Diabetes Association). (n.d.). Graves’ disease
- Yale Medicine. (n.d.). Graves’ disease
- Manipal Hospitals. (n.d.). Graves’ disease: Symptoms, causes and treatment
In this Article

















