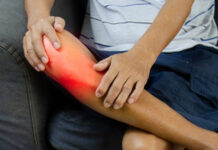
Did you know that nearly 4 million Americans seek medical treatment for tendonitis each year? Whether you’re a weekend warrior pushing through that tennis match or a construction worker dealing with repetitive strain, tendon pain can sideline anyone at any time.
Tendonitis, also known as tendinitis, is a condition that occurs when tendons become inflamed. According to the Mayo Clinic, this injury most commonly happens during physical activities, especially sports, and involves both inflammation and acute injury to the tendon tissue.
This comprehensive guide provides essential information about tendonitis, including its major causes, symptoms, types, and available treatment options backed by current medical research.
Read More: 10 Best Elbow Braces For Tendonitis – Manage The Effects
What is Tendonitis?
Tendonitis is the inflammation of tendons caused by injury or trauma. According to research published in the National Center for Biotechnology Information, it most frequently affects the wrists, thighs, fingers, elbows, and other parts of the body that experience repetitive stress or sudden injury.
A tendon is the flexible tissue that connects muscle to bone. While tendon tissues are fibrous and tough, they’re classified as soft tissue because they’re much softer than bone. Despite their strength, tendons can bear significant tension but are vulnerable to inflammation when overused or injured.
Common names for tendonitis include Achilles tendinitis, tennis elbow, golfer’s elbow, pitcher’s shoulder, and jumper’s knee, depending on the location of the inflammation.
Related Conditions
Sometimes the sheath surrounding the tendon becomes inflamed instead of the tendon itself. This condition is called tenosynovitis, and it often occurs alongside tendonitis.
While tendonitis can affect people of any age, it’s more common in adults who participate in sports or repetitive activities. Older adults are particularly susceptible because tendons lose elasticity and become weaker with age.
The long-term, degenerative form of tendinitis is called tendinosis, which presents similar symptoms but involves tissue breakdown rather than inflammation.
Symptoms and Signs of Tendonitis

Tendonitis symptoms typically occur where the tendon attaches to the bone. The most common signs include:
- Pain and tenderness – Severe pain that worsens with movement
- Swelling, redness, and warmth – Visible inflammation in the affected area
- Lumps or thickening – Development of bumps along the tendon
- Crackling sensation – A grating or crackling feeling during movement
- Stiffness – Reduced range of motion in the affected joint
In severe cases, tendon rupture may occur, creating a noticeable gap along the tendon line and causing significant difficulty with movement. Symptoms can persist anywhere from a few days to several weeks or even months, depending on the severity and treatment approach.
Read More: 9 Best Braces For Achilles Tendonitis – Effective Support!
What Causes Tendonitis?
According to medical experts, tendonitis has two primary causes:
- Repetitive motion over time – Gradual wear and tear from repeated movements
- Sudden injury – Acute trauma to the tendon
“What causes tendinitis to develop, is it’s an inflammatory process to start and then sometimes it can also be a degenerative process,” said Dr. George C. Umeh, MD, a sports medicine physician at Bayhealth Orthopaedics in Milford, Delaware, “similar to what you see with other degenerative things within the body such as disc disease or arthritis.”
“Over time, you keep using that tendon because your tendon is anchored to your muscle and anchored to the bone,” he said. “So, when you put it under a lot of stress with weights or activity or whatever you’re doing, it stretches that tendon.”
Risk Factors
Occupation and Activities: People with jobs or hobbies involving repetitive motions or awkward positions are at higher risk. This includes:
- Construction workers (particularly painters working overhead)
- Athletes in sports requiring repetitive movements (running, basketball, golf, bowling, baseball, swimming, tennis)
- Musicians and office workers with repetitive hand/wrist motions
Age: Older adults face an increased risk as tendons naturally become less flexible and more prone to injury with age.
Medical Conditions: Certain health conditions increase susceptibility to tendonitis:
- Rheumatoid arthritis
- Diabetes
- Other inflammatory conditions
When to Seek Medical Attention: Contact a healthcare provider immediately if pain suddenly worsens or if joint movement becomes nearly impossible.
Diagnosis of Tendonitis

Healthcare providers typically diagnose tendonitis through:
Physical Examination
- Assessment of symptoms and affected areas
- Listening for creaky sounds when moving the tendon (indicating inflammation and thickening of the tendon sheath)
- Testing for tenderness at specific points along the tendon
Additional Testing
If initial treatment doesn’t improve symptoms, doctors may order:
- X-rays – To identify calcium deposits on tendons
- Ultrasound – To visualize soft tissue inflammation
- MRI – To detect swelling in the tendon sheath and surrounding tissues
Read More: 12 Natural remedies for tendonitis – Find relief the natural way!
Treatment Options for Tendonitis
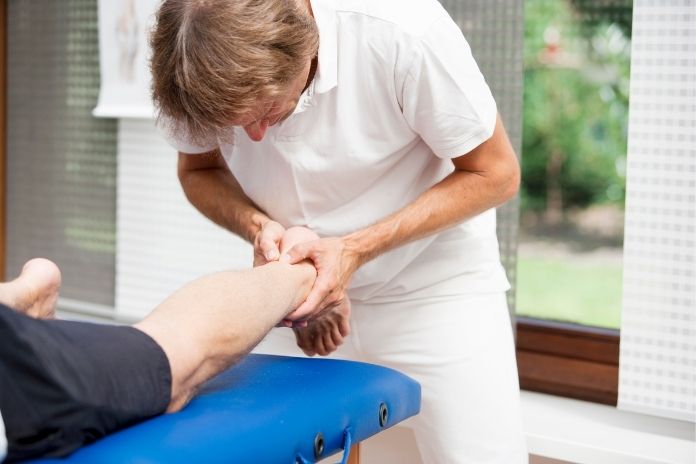
Treatment focuses on reducing inflammation and relieving pain. Most cases respond well to conservative treatment approaches.
Conservative Treatments
Rest and Protection
- Avoid activities that worsen symptoms
- Use splints or braces to protect affected joints
- Modify daily activities to reduce tendon stress
Hot and Cold Therapy
- Apply ice packs for acute injuries (within 48 hours)
- Use warm compresses for chronic pain
- Apply for 10-15 minutes, 2-3 times daily
- Always wrap ice or heat sources in a towel to protect skin
Over-the-Counter Pain Relief
- Ibuprofen and other nonsteroidal anti-inflammatory drugs (NSAIDs) – Studies show these provide short-term relief from tendonitis pain
- Follow package directions and consult with healthcare providers about long-term use
Advanced Treatments
Physical Therapy
- Professional massage to improve healing
- Specific exercises and stretching routines are prescribed by therapists
- Guidance on proper movement techniques
- Gradual return to activities
Corticosteroid Injections
- Effective for reducing inflammation
- Used sparingly due to increased rupture risk with repeated use
- Reserved for cases not responding to conservative treatment
Surgical Options
- Shock wave therapy – Uses sound waves to break up calcium deposits
- Surgery – May be necessary to remove calcium deposits or repair damaged tendons
- Typically considered only when conservative treatments fail
Exercise and Rehabilitation
Specific stretching and strengthening exercises play a crucial role in recovery:
- Improve flexibility and range of motion
- Strengthen surrounding muscles to support the affected tendon
- Prevent future injury through proper conditioning
- Should be performed under professional guidance initially
Read More: How to Protect Your Knees During Workouts: Tips Every Active Person Should Know
Prevention and Outlook

Most cases of tendonitis respond well to treatment when addressed promptly. Recent research from the NIH indicates that both acute and chronic tendinopathy can result in high morbidity if not properly managed. The key to successful recovery is:
- Early intervention
- Proper rest and activity modification
- Consistent adherence to treatment plans
- Gradual return to normal activities
Prevention strategies include proper warm-up before activities, using correct techniques during sports or work, taking regular breaks from repetitive motions, and maintaining overall fitness and flexibility.
With appropriate treatment, most people with tendonitis can expect full recovery and return to their normal activities.
Take Action Against Tendon Pain Today
Don’t let tendonitis keep you on the sidelines. If you’re experiencing persistent tendon pain, swelling, or difficulty moving a joint, it’s time to take action. Early intervention can prevent a minor issue from becoming a chronic problem that sidelines you for months.
Your next steps:
- Schedule a consultation with a healthcare provider or sports medicine specialist
- Document your symptoms – when they started, what makes them better or worse
- Consider physical therapy even for mild symptoms to learn proper techniques
- Modify activities that may be contributing to your pain
Remember, tendonitis is highly treatable when caught early. The sooner you address it, the faster you’ll get back to doing what you love.
Read More: How to Prevent DOMS (Delayed Onset Muscle Soreness) Without Skipping Gains
Frequently Asked Questions (FAQ)
How long does tendonitis take to heal?
Recovery time varies depending on severity and location, but most cases of tendonitis heal within 2-6 weeks with proper treatment. Chronic cases may take several months. According to Mayo Clinic research, early intervention significantly improves healing time.
Can tendonitis become permanent?
While tendonitis itself isn’t permanent, untreated cases can lead to tendinosis – a degenerative condition that’s more difficult to treat. Chronic tendinopathy can result in long-term complications, making early treatment crucial.
What’s the difference between tendonitis and tendinosis?
Tendonitis involves inflammation of the tendon, while tendinosis is a degenerative condition without significant inflammation. Medical literature shows that tendinosis often develops from chronic, untreated tendonitis.
Should I use ice or heat for tendonitis?
Use ice for acute injuries (first 48 hours) to reduce inflammation. After 48 hours, heat can help improve blood flow and healing. Both should be applied for 10-15 minutes at a time, wrapped in a towel to protect your skin.
Can I exercise with tendonitis?
You should modify or avoid activities that worsen your pain. However, complete rest isn’t always recommended. Research indicates that appropriate exercise and stretching, guided by a healthcare provider, can actually help healing.
When should I see a doctor for tendonitis?
Seek medical attention if:
- Pain suddenly worsens or becomes severe
- You can’t move the affected joint
- Symptoms don’t improve after a few days of rest and home treatment
- You develop numbness or tingling
- The area becomes red, hot, or shows signs of infection
Are steroid injections safe for tendonitis?
Corticosteroid injections can be effective for reducing inflammation, but they come with risks. Medical studies show that repeated injections may increase the risk of tendon rupture, so they’re used sparingly and only when conservative treatments haven’t worked.
Can certain medical conditions make tendonitis worse?
Yes, conditions like rheumatoid arthritis and diabetes can increase your risk of developing tendonitis and may slow healing. People with these conditions should work closely with their healthcare providers to manage tendon health.
Is surgery ever necessary for tendonitis?
Surgery is rarely needed for tendonitis and is typically reserved for severe cases that don’t respond to months of conservative treatment. Most people recover fully with non-surgical approaches.
References
- https://www.mayoclinic.org/diseases-conditions/tendinitis/symptoms-causes/syc-20378243
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3761855/
- https://www.mayoclinic.org/diseases-conditions/patellar-tendinitis/diagnosis-treatment/drc-20376118
- https://www.mayoclinic.org/diseases-conditions/achilles-tendinitis/diagnosis-treatment/drc-20369025
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5865563/
- https://www.mayoclinic.org/diseases-conditions/tendinitis/diagnosis-treatment/drc-20378248
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7886058/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2505250/
- https://medlineplus.gov/tendinitis.html
- https://www.ama-assn.org/delivering-care/prevention-wellness/what-doctors-wish-patients-knew-about-tendinitis
- https://find-doctor.ama-assn.org/doctor/george-chinedum-umeh-md/49648985
In this Article