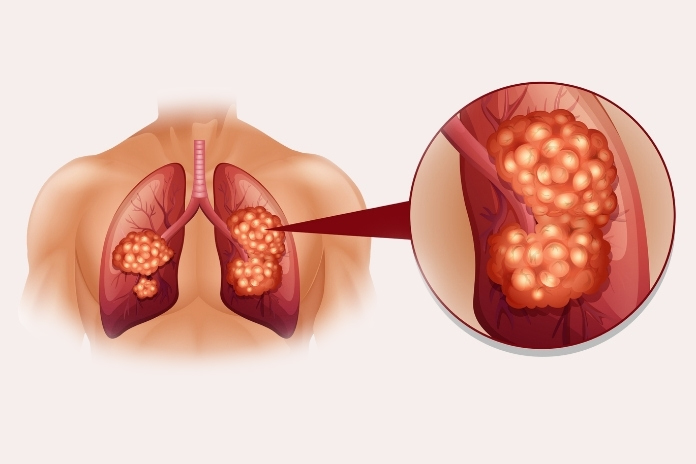
Lung cancer may seem straightforward at first glance, but its complexity extends beyond what is initially apparent. Our lungs—those balloon-like organs in the chest—play a vital role in keeping every cell alive with oxygen.
It is known to be one of the most common forms of cancer. Tobacco smoke mainly causes it. Although these facts are important, there’s still a great deal about lung cancer that the general public doesn’t fully know.
Lung cancer has two significant classifications: small-cell lung cancer and non-small-cell lung cancer.
Understanding the differences between the two forms, equips patients and their families to comprehend the diagnosis, understand the available treatment options, and what to expect in their daily lives.
This article gives a short side-by-side comparison of non-small cell lung cancer or the (NSCLC) and the small cell lung cancer as known as (SCLC) and discusses the different causes of the two cancers, the different symptoms that may occur, stage of the cancer, various diagnostic tests that are available, and treatment options of each variant.
Read More: Diet and Lifestyle Tips After a Pancreatic Cancer Diagnosis
At-a-Glance: SCLC vs NSCLC
Doctors divide the two sponge-like organs in your chest, your lungs, into sections known as lobes. You have three lobes in your right lung. There are two lobes in your left lung. Because the heart occupies more space on the left side of our body, the left lung is smaller.
About SCLC:
The bronchi, or the airways that connect the trachea to the lungs, are frequently where SCLC begins before branching off into ever-tinier structures. SCLC swiftly spreads to other areas of the body, including the lymph nodes, after first affecting the bronchi. Tobacco use usually causes this type, which accounts for less than 20% of lung cancers.
Small cell carcinoma and the combined small cell carcinoma are the other two subtypes of SCLC. Pathologists use these two categories under a microscope to identify the small cells. The most common form of SCLC is called small cell carcinoma, and it appears as oat-like structures under the microscope.
A neoplasm composed of small cell carcinoma cells and a few non-small cell lung cancer cells is known as combined small cell carcinoma.
About NSCLC:
NSCLC accounts for between 80% to 85% of lung cancer cases. Adenocarcinoma, squamous cell carcinoma, and large cell carcinoma are the three primary subtypes of non-small cell lung cancer. Since their prognoses (outcomes) and treatments are frequently comparable, these subtypes—which originate from various kinds of lung cells—are grouped as NSCLC.
- Adenocarcinoma: Lung adenocarcinoma begins in the epithelial cells that produce mucus in the lung. Epithelial cells line the surface of the lungs. The most prevalent kind of non-small cell lung cancer is adenocarcinoma. Although lung adenocarcinoma is the most common form of lung cancer in nonsmokers, it primarily affects those who smoke or have smoked in the past. Compared to other forms of lung cancer, it is more likely to strike younger people and is more prevalent in women than in men.
- Squamous cell carcinoma: This type of cancer originates in squamous cells, which are flat cells that line the internal airways of the lungs. They typically occur in the central region of the lungs, close to a major airway (bronchus), and are frequently associated with a history of smoking.
- Large cell carcinoma (undifferentiated): This type of lung cancer can develop anywhere in the lung. It can be challenging to treat because of its propensity for rapid growth and spread. Large cell neuroendocrine carcinoma (LCNEC) is a rapidly growing subtype of large cell carcinoma that closely resembles small cell lung cancer.
Risk Factors and Causes

According to the National Institutes of Health, 90% of the cases of lung cancer are caused by smoking. Heavy smokers (those who consume at least one pack of cigarettes daily) are more likely to develop SCLC.
Small cell lung cancer (SCLC) and non-small cell lung cancer (NSCLC) share numerous risk factors that highlight genetic and environmental influences on lung health.
Tobacco smoke: The most significant risk factor for lung cancer is smoking. Researchers estimate that smoking causes about 80% of lung cancer deaths, and it likely accounts for an even higher percentage of small-cell lung cancer (SCLC) cases. SCLC is uncommon in people who have never smoked. Compared to nonsmokers, smokers have a significantly increased risk of developing lung cancer. Your risk increases with the length of time you smoke and the number of packs you smoke each day.
Secondhand smoke: If you don’t smoke, inhaling other people’s smoke, also known as environmental tobacco smoke, can raise your risk of lung cancer. In the US, secondhand smoke ranks as the third most frequent cause of lung cancer.
Radon exposure: Radon is a naturally occurring radioactive gas that is produced when uranium breaks down in rocks and soil. It is not visible, palatable, or odorous. Radon is the second most common cause of lung cancer in the US and the most common reason among nonsmokers, according to the US Environmental Protection Agency (EPA).
Asbestos exposure: The risk of dying from lung cancer is increased several times for those who work with asbestos, such as in shipyards, mills, textile factories, mines, and locations that use insulation. Smoking workers exposed to asbestos face a significantly higher risk of developing lung cancer.
The extent to which short-term or low-level asbestos exposure may increase risk of lung cancer is unknown. Additionally, high levels of asbestos exposure make people more likely to develop mesothelioma, a form of cancer that begins in the pleura (the lining surrounding the lungs).
Read More: 8 Pancreatic Cancer Symptoms You Shouldn’t Ignore
Symptoms of SCLC vs NSCLC

Lung cancer symptoms include a persistent or worsening cough, shortness of breath, wheezing, coughing up blood, chest pain, fatigue, and weight loss that has no apparent cause. Lung cancer frequently doesn’t show symptoms until it has advanced to a later stage.
People with SCLC may experience a sudden onset or a rapid worsening of symptoms because the disease tends to grow more quickly.
The following symptoms are common in patients with either type of lung cancer:
- Discomfort or pain in the chest
- A persistent cough that worsens with time
- Breathing problems
- Wheezing
- Having a hoarse voice
- Difficulty in swallowing
- Coughing up blood
- Appetite loss
- Inexplicable loss of weight
- Swelling of the face
- Enlarged veins in the neck
However, small-cell lung cancer can also cause symptoms like bone pain, confusion, seizures, and paralysis because it usually grows and spreads to other parts of the body more quickly than non-small cell lung cancer.
Staging Systems: Limited/Extensive vs TNM
To determine the cancer stage, the TNM staging system combines letters and numbers to classify the disease. A number ranging from 0 to 4 follows each letter to indicate the stage. The letter ‘T’ represents tumor size and extent. Doctors use the letter ‘N’ to indicate whether the tumor has spread to the lymph nodes. They use the letter ‘M’ for metastasis when cancer has reached distant organs. Although doctors can treat both NSCLC and SCLC this way, NSCLC benefits more from the approach.
Stages of non-small cell lung cancer
Stage 1: There is only one lung with the tumor, and it has not migrated to any other organ or lymph nodes. Radiation therapy, surgery, or a combination of both are available as treatment options. In specific instances, a doctor may recommend adjuvant therapy that may include:
- Targeted therapy
- Brachytherapy
- Chemotherapy
- Radiation therapy
Stage 2: The cancer measures more than three centimeters (cm) in diameter. It might have reached the lung’s internal lymph nodes, but not any other organs.
Surgery and radiation therapy, with or without adjuvant therapies, are the usual treatment choices. These may include:
- Targeted therapy
- Chemotherapy
- Immunotherapy
- Radiation therapy
Stage 3: The malignancy measures more than 7 cm in diameter. Although it did not spread to any distant organs, it might have reached the lymph nodes in the middle of the chest. There are two subtypes of stage 3 NSCLC:
3A: There is no evidence of the malignancy spreading to the other side of the chest.
3B: The malignancy has spread to lymph nodes close to the collarbone or in the lung on the other side.
Depending on where the tumor is located, treatment options may involve one or more of the following:
- Surgery
- Radiation therapy
- Chemotherapy
Stage 4: NSCLC has expanded to distant lymph nodes or organs, the other lung, or the fluid surrounding the lung or heart.
Options for treatment could involve combinations of:
- Combination chemotherapy
- Targeted therapies
- Monoclonal antibodies
- Radiation therapy for obstructive tumor growth
Stages of small-cell lung cancer
About 10–15% of all instances of lung cancer are SCLC.
Doctors divide SCLC into two groups according to the most widely used staging system:
Limited stage: The lung, lymph nodes, or both may be affected, and the cancer has only spread to one side of the chest.
At this point, treatment options include:
- Combined radiation and chemotherapy
- Combination with the chemotherapy
- Chemotherapy or chemoradiation therapy after surgery
Extensive stage: The cancer has either spread outside of the chest or to the other side.
At this point, the treatment options include:
- Modulation of immune checkpoints and combination chemotherapy
- Radiation treatment
- Chemotherapy in combination
Read More: 7 Comfort Items for Cancer Patients Undergoing Chemotherapy
Diagnosis and Testing — What Doctors Order and Why

If your healthcare provider suspects lung cancer, they can perform numerous tests to check for malignant cells and rule out other disorders.
Tests could consist of:
Imaging testing: Imaging exams create images of the body. These tests can show the location and the spread of lung cancer. Doctors may perform X-rays, MRIs, CT scans, and positron emission tomography (PET) scans.
Cytology of sputum: Doctors call the mucus coughed out from the lungs sputum. They can examine the sputum under a microscope.
A biopsy is the process of taking a tissue sample for laboratory analysis.
A lung cancer biopsy is done in several ways by your medical team. Bronchoscopy is one method. A lighted tube equipped with a camera is inserted through your throat and into your lungs by a medical specialist during a bronchoscopy to evaluate the area. To obtain a tissue sample, specialized instruments can be inserted via the tube.
There is also the possibility of mediastinoscopy. A base of neck incision is made during a mediastinoscopy. After that, surgical instruments are placed below your breastbone to remove the tissue samples from the lymph nodes.
Conclusion
Both small cell lung cancer (SCLC) and non-small cell lung cancer (NSCLC) grow rapidly, spread easily, and doctors classify them as limited or extensive within either their class or TNM groupings. SCLC is treated primarily with radiation and chemotherapy.
When patients and family members understand the fundamental differences in cause, symptoms, stage, diagnostic tests, and treatment options for these diseases, they can interpret complex medical information and participate in treatment decisions with greater confidence. Our article provides an overall picture, but your own healthcare team will develop specific treatment plans tailored to you, and individual treatment plans will vary.
Read More: Ovarian Cancer Stages Explained: What You Need to Know
FAQs
Which is more aggressive—SCLC or NSCLC?
Doctors regard SCLC as a worse form of lung cancer because it is more aggressive, grows and spreads faster, and has a poorer survival rate than NSCLC. In contrast, NSCLC occurs more frequently, and doctors can often treat it with surgery.
Can a cancer change type?
To adapt to their surroundings and become more resistant to therapy, cancer cells can undergo a process known as transdifferentiation or histological metamorphosis, which causes them to change their type.
Is screening different for SCLC vs NSCLC?
Doctors derive their names from the appearance of their cells under the microscope. Comparing SCLC cells to NSCLC cells, the former appear spherical and smaller in size. However, their level of aggression is where they differ the most. Compared to NSCLC, SCLC is more aggressive and tends to spread to other areas of the body more frequently.
Are targeted therapies only for NSCLC?
Targeted therapy isn’t always appropriate for everyone, though. Factors such as the type of cancer, genetic alterations, overall health, and treatment history influence whether this therapy is appropriate.
References
- https://www.cancer.org/cancer/types/lung-cancer/about/what-is.html
- https://www.moffitt.org/cancers/lung-cancer/faqs/what-is-the-difference-between-small-cell-lung-cancer-non-small-cell-lung-cancer
- https://phelpshealth.org/news/latest-news/small-and-non-small-cell-lung-cancer-whats-difference
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4080902
- https://www.cancer.org/cancer/types/lung-cancer/causes-risks-prevention/risk-factors.html
- https://www.mdanderson.org/cancer-types/lung-cancer.html
- https://www.mayoclinic.org/diseases-conditions/lung-cancer/symptoms-causes/syc-20374620
- https://www.cancer.org/cancer/types/lung-cancer/detection-diagnosis-staging/signs-symptoms.html
- https://www.jtcvs.org/article/S0022-5223(17)32136-0/pdf
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3351680/
- https://www.thoracic.org/patients/patient-resources/resources/lung-cancer-staging.pdf
- https://www.medicalnewstoday.com/articles/316198#stages
- https://www.aafp.org/pubs/afp/issues/2022/0500/p487.html
- https://www.mayoclinic.org/diseases-conditions/lung-cancer/diagnosis-treatment/drc-20374627
In this Article