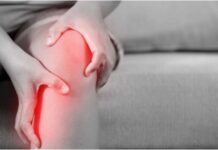
Psoriatic arthritis (PsA) is a chronic autoimmune disorder that doesn’t just affect the skin; it also targets the joints, making it a dual-front battle for those who live with it. While psoriasis is often recognized for its scaly, inflamed skin patches, the impact of PsA runs deeper. Up to one in three people with psoriasis will eventually develop psoriatic arthritis, meaning it’s more common than many realize.
Unlike ordinary aches or joint injuries, PsA stems from the immune system mistakenly attacking healthy joint tissue and skin. This triggers inflammation, causing pain, stiffness, swelling, and, over time, can lead to permanent joint damage. The effects aren’t just physical; PsA can affect mobility, energy levels, and overall quality of life, making daily tasks increasingly challenging.
The good news is that with early detection, accurate diagnosis, and modern treatment options, psoriatic arthritis can be effectively managed. Understanding the condition, recognizing its early warning signs, and learning how it develops are critical first steps toward better control. This article dives into everything you need to know about PsA, from its causes and symptoms to the latest treatment strategies, to help you or your loved ones navigate the condition with confidence and clarity.
What Is Psoriatic Arthritis?
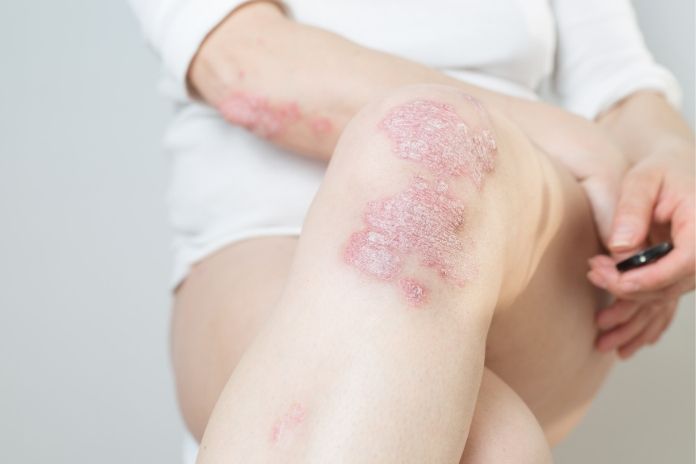
Psoriatic arthritis (PsA) is a chronic autoimmune condition, meaning the immune system mistakenly attacks the body’s own tissues. In this case, it primarily targets the joints and, in many instances, the skin. This dual involvement is what sets PsA apart from other forms of arthritis, like rheumatoid arthritis (RA) or osteoarthritis, which may affect joints differently or not involve the skin at all.
Unlike psoriasis, which primarily affects the skin, PsA causes inflammation inside the joints, leading to swelling, pain, and stiffness. The pattern of joint involvement can also differ from other arthritic conditions.
For example, while rheumatoid arthritis typically affects joints on both sides of the body symmetrically, psoriatic arthritis often appears asymmetrically, impacting one knee, a few fingers, or a single wrist rather than mirrored joints on both sides. This asymmetry can sometimes make diagnosis trickier, especially in the early stages.
PsA can develop at any point in someone’s life, often years after the initial onset of psoriasis. However, in some cases, joint symptoms may precede visible skin changes, adding another layer of complexity to diagnosis. Studies suggest that roughly 30% of people with psoriasis will eventually develop psoriatic arthritis, highlighting the importance of vigilance and early detection.
The condition can vary widely from person to person. Some individuals may experience mild symptoms in just a few joints, while others face widespread inflammation affecting multiple joints and tendons. PsA doesn’t just affect physical health; it can impact daily activities, work, and overall quality of life if left untreated. Understanding the signs, risk factors, and unique characteristics of psoriatic arthritis is crucial for timely diagnosis and effective management, which can help prevent long-term joint damage and maintain mobility.
Symptoms of Psoriatic Arthritis

Recognizing psoriatic arthritis (PsA) early is critical. Untreated inflammation can lead to permanent joint damage, reduced mobility, and long-term disability. While symptoms vary from person to person, several hallmark signs help distinguish PsA from other types of arthritis.
- Joint pain, stiffness, and swelling: PsA commonly affects the fingers, toes, knees, ankles, and lower back. Unlike rheumatoid arthritis, which usually presents symmetrically, PsA often appears asymmetrically, affecting one side more than the other. The inflammation can make simple daily tasks, like buttoning a shirt or walking, painful and difficult.
- Dactylitis (“sausage digits”): Swelling of an entire finger or toe is a distinctive feature of PsA. Around 40% of patients experience this, and it often signals active inflammation in the joints and surrounding tendons. Dactylitis can be painful, tender to touch, and visually striking.
- Nail changes: Up to 80% of people with PsA experience nail involvement. This can include pitting (small dents), ridging, discoloration, or onycholysis (separation of the nail from the nail bed). Nail changes are more than cosmetic; they often indicate underlying joint inflammation and can serve as an early warning sign of PsA.
- Fatigue: Chronic inflammation takes a toll on the body, leaving many patients feeling constantly exhausted. Fatigue in PsA is often disproportionate to activity level and can interfere with work, social life, and daily routines.
- Eye inflammation (uveitis): Some people develop painful, red, or sensitive eyes. Untreated uveitis can threaten vision, making early detection and prompt ophthalmologic care essential.
- Flare-ups and remissions: PsA is unpredictable. Symptoms often wax and wane, with periods of intense flare-ups followed by times of relative calm. Triggers for flares vary and may include stress, illness, or changes in medication.
- Other systemic symptoms: While PsA primarily affects the skin and joints, it can also contribute to stiffness in the spine (spondylitis), tendon inflammation (enthesitis), and even cardiovascular complications in some patients.
Because PsA can mimic other joint diseases, including rheumatoid arthritis and osteoarthritis, early recognition is key. Paying attention to subtle signs like nail changes, asymmetric joint pain, or sausage digits can help healthcare providers make a timely diagnosis. Early intervention with medications and lifestyle modifications can prevent irreversible joint damage and improve overall quality of life.
Causes and Risk Factors
The exact causes of psoriatic arthritis (PsA) are still not fully understood, but researchers agree that it arises from a complex interplay of genetics, immune system dysfunction, environmental triggers, and lifestyle factors. These elements combine to create the conditions for the immune system to mistakenly attack healthy tissue, leading to inflammation in both the joints and skin.
- Genetics: Family history plays a significant role in PsA risk. Individuals with a parent or sibling who has psoriasis or psoriatic arthritis are more likely to develop the condition themselves. Specific genes, such as HLA-B27, have been strongly linked to PsA, influencing both susceptibility and the pattern of joint involvement. Genetic factors don’t guarantee the disease, but they create a predisposition that can be triggered by other factors.
- Immune system dysfunction: PsA is an autoimmune disease, meaning the body’s immune system mistakenly identifies healthy cells as threats. In PsA, immune cells target joint tissue and skin, triggering inflammation, pain, and tissue damage. This immune overreaction explains why PsA often coexists with psoriasis, as both conditions involve abnormal immune activity.
- Environmental triggers: External factors can activate PsA in genetically predisposed individuals. Infections, such as strep throat, or physical trauma (known as the Koebner phenomenon) can spark disease onset. Chronic stress may also exacerbate inflammation, contributing to flare-ups and symptom progression.
- Lifestyle factors: Obesity, smoking, and sedentary habits have been linked to both a higher risk of developing PsA and worse disease outcomes. Excess weight adds stress to joints, fueling inflammation, while smoking can amplify immune dysfunction. Adopting a healthy lifestyle may reduce disease severity and improve response to treatment.
- Other contributing factors: Age, gender, and the presence of other autoimmune disorders can also influence PsA development. Although anyone can develop the condition, PsA most often appears between the ages of 30 and 50.
“Obesity is one of the stronger risk factors for development of psoriatic arthritis, along with severe psoriasis, history of joint trauma, family history, and general inflammatory bowel disease.” – Dr. Alexis Ogdie, MD, MSCE, Rheumatologist, Perelman School of Medicine, University of Pennsylvania.
Together, these factors create a “perfect storm” for psoriatic arthritis, where genetic susceptibility meets immune dysregulation and environmental stressors. While the exact trigger may differ for each person, understanding these risk factors can help individuals recognize early warning signs, seek timely medical evaluation, and take proactive steps toward management and prevention.
Read More: Causative Gene Behind Rheumatoid Arthritis – Study Shows Evidence
Diagnosis: How Doctors Confirm PsA
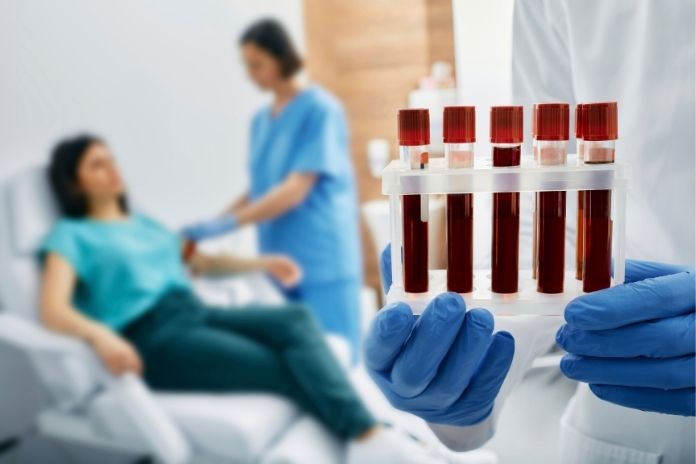
Diagnosing psoriatic arthritis (PsA) can be challenging because no single test definitively confirms the condition. Instead, doctors rely on a combination of patient history, physical examination, laboratory tests, and imaging studies to reach an accurate diagnosis. Early detection is critical, as untreated inflammation can lead to permanent joint damage and reduced mobility.
- Symptom review and physical exam: Physicians carefully assess joint pain, stiffness, swelling, and tenderness. They also examine fingers and toes for dactylitis (“sausage digits”), check nails for pitting or separation, and inspect the skin for psoriasis plaques. Observing patterns of joint involvement, whether symmetrical or asymmetrical, helps distinguish PsA from other forms of arthritis.
- Blood tests: While there is no blood test that definitively diagnoses PsA, certain tests help rule out other conditions. Patients with PsA typically test negative for rheumatoid factor (RF), which differentiates it from rheumatoid arthritis. Additional markers of inflammation, such as C-reactive protein (CRP) or erythrocyte sedimentation rate (ESR), may be elevated during active disease.
- Imaging: X-rays, ultrasound, and MRI scans can reveal characteristic changes in joints affected by PsA, including swelling, bone erosion, new bone formation, or enthesitis (inflammation at tendon and ligament attachment sites). Advanced imaging techniques are particularly useful for detecting early joint changes that aren’t visible on X-rays alone.
- Specialist collaboration: Because PsA affects both the skin and joints, dermatologists and rheumatologists often work together to confirm the diagnosis. Coordinated care ensures that both skin and joint symptoms are properly evaluated, which can improve treatment outcomes.
- Early and accurate diagnosis: Prompt recognition of PsA allows doctors to start treatment before significant joint damage occurs. This may include disease-modifying medications, biologics, and lifestyle interventions. Early intervention not only preserves joint function but also improves overall quality of life, reduces pain, and minimizes long-term disability.
PsA diagnosis is a careful balance of clinical observation, laboratory data, and imaging. Patients experiencing persistent joint pain, swelling, or unusual nail and skin changes should seek evaluation promptly. Accurate diagnosis is the first step toward controlling the disease, preventing complications, and maintaining mobility and function over the long term.
Read More: The Ultimate Arthritis Toolkit: 12 Products That Provide Comfort
Treatment Options for Psoriatic Arthritis

The goal of psoriatic arthritis (PsA) treatment is to reduce inflammation, relieve pain, prevent joint damage, and improve quality of life. Because PsA varies widely among individuals, treatment is highly personalized, taking into account disease severity, affected joints, skin involvement, lifestyle, and other medical conditions.
A. Medications
Medications are the cornerstone of PsA management. They range from symptom-relief options to advanced therapies that slow disease progression and target immune dysfunction.
- NSAIDs (Nonsteroidal Anti-Inflammatory Drugs): Over-the-counter NSAIDs, such as ibuprofen or naproxen, help alleviate joint pain, swelling, and stiffness. While they don’t modify disease progression, they provide effective short-term symptom relief and improve daily functioning.
- DMARDs (Disease-Modifying Antirheumatic Drugs): Medications like methotrexate, leflunomide, and sulfasalazine reduce immune system activity, helping to slow joint damage and disease progression. DMARDs are often used when NSAIDs alone are insufficient.
- Biologics: These targeted therapies block specific immune system proteins driving PsA inflammation. Common categories include:
- TNF inhibitors: adalimumab, etanercept, infliximab.
- IL-17 inhibitors: secukinumab, ixekizumab.
- IL-23 inhibitors: guselkumab, risankizumab
Biologics have revolutionized PsA treatment and are often prescribed for moderate-to-severe cases. A 2020 review in Rheumatology confirmed their effectiveness in reducing joint damage and skin symptoms.
- JAK inhibitors: Newer oral medications, such as tofacitinib and upadacitinib, block Janus kinase pathways involved in inflammation. These are typically used for patients who do not respond adequately to biologics.
Read More: 9 Essential Supplements for Joint Health and Arthritis Relief
B. Lifestyle and Home-Based Strategies
Lifestyle interventions complement medical treatment and can have a meaningful impact on symptom management and disease progression.
- Regular exercise: Low-impact activities like swimming, yoga, walking, or cycling maintain joint mobility, improve muscle strength, and reduce stiffness.
- Anti-inflammatory diet: Diets rich in omega-3 fatty acids, fruits, vegetables, and whole grains may reduce systemic inflammation and improve overall health.
- Stress management: Stress is a common trigger for PsA flares. Techniques such as mindfulness, meditation, and deep breathing exercises can help control flare intensity.
- Weight management: Maintaining a healthy weight reduces stress on joints, decreasing pain and potentially slowing disease progression.
“Lifestyle modification is one of the recommended strategies to improve outcomes in psoriatic arthritis, alongside treating comorbidities and addressing fatigue and pain.” – Adapted from Dr. Christopher T. Ritchlin et al., “Strategies to Improve Outcomes in Psoriatic Arthritis”.
Read More: 13 Lifestyle Changes For Arthritis – Lead A Healthier Life
C. Physical and Occupational Therapy
Targeted therapies support joint function, prevent disability, and make daily life easier.
- Physical therapy: Personalized exercise plans improve flexibility, strengthen muscles around affected joints, and maintain mobility.
- Occupational therapy: Therapists provide joint protection strategies, adaptive tools, and ergonomic advice to reduce strain in daily activities.
- Assistive devices: Splints, braces, or modified utensils can help manage pain and reduce stress on inflamed joints.
D. Surgery (For Advanced Cases)
Surgery is generally considered a last resort, but it can dramatically improve the quality of life for patients with severe joint damage.
- Joint replacement: In cases where inflammation has caused irreversible joint destruction, replacement surgeries restore function and reduce pain.
- Other surgical interventions: Tendon repair or joint fusion may be considered depending on the specific joints affected.
Managing psoriatic arthritis requires a multifaceted approach that combines medications, lifestyle adjustments, therapy, and sometimes surgery. Early intervention, consistent medical follow-up, and patient engagement in lifestyle choices are crucial for controlling symptoms, protecting joints, and maintaining quality of life.
Read More: 10 Tips for Managing Arthritis Pain Without Medication
Conclusion
Psoriatic arthritis is a chronic autoimmune condition, but it is far from a life sentence. While it can cause persistent pain, stiffness, swelling, fatigue, and, if left untreated, permanent joint damage, early recognition and intervention dramatically improve outcomes. Modern treatments, ranging from DMARDs and biologics to JAK inhibitors, have transformed the way PsA is managed, giving patients the ability to lead active, fulfilling lives despite the disease.
The key takeaway is this: if you have psoriasis and start experiencing joint pain, swelling, or unexplained fatigue, take it seriously. Early evaluation by a healthcare professional can prevent irreversible joint damage, reduce flare-ups, and preserve mobility.
Beyond medications, integrating lifestyle strategies, including regular low-impact exercise, a balanced anti-inflammatory diet, stress management, and maintaining a healthy weight, amplifies the effectiveness of treatment and supports long-term joint and overall health.
Living with PsA doesn’t mean resigning yourself to pain or limitation. With the right combination of medical care, proactive lifestyle choices, and ongoing monitoring, patients can regain control, protect their joints, and enjoy a higher quality of life. Awareness, early action, and consistent management are the strongest tools for overcoming the challenges of psoriatic arthritis and staying active, healthy, and resilient.
References
- https://www.mayoclinic.org/diseases-conditions/psoriatic-arthritis/symptoms-causes/syc-20354076
- https://my.clevelandclinic.org/health/diseases/13286-psoriatic-arthritis
- https://www.ncbi.nlm.nih.gov/books/NBK547710
- https://en.wikipedia.org/wiki/Psoriatic_arthritis
- https://versusarthritis.org/about-arthritis/conditions/psoriatic-arthritis
- https://www.goodrx.com/conditions/psoriatic-arthritis
- https://www.arthritis.org/diseases/psoriatic-arthritis
- https://www.archivesofmedicalscience.com/Psoriatic-arthritis-new-perspectives,93614,0,2.html
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3596149
- https://www.nhs.uk/conditions/psoriatic-arthritis
- https://www.physio-pedia.com/Psoriatic_Arthritis
- https://www.psoriasis.org/our-spot-psoriatic-arthritis
- https://medlineplus.gov/genetics/condition/psoriatic-arthritis
- https://www.webmd.com/arthritis/psoriatic-arthritis/psoriatic-arthritis-the-basics
- https://emedicine.medscape.com/article/2196539-overview
- https://rheumatology.org/patients/psoriatic-arthritis
In this Article