You twist your knee, your back flares up, or your joints start aching seemingly for no reason. The first instinct is often to reach for relief, a dose of ibuprofen, or a Google search for turmeric, omega-3s, or ginger. That’s when the questions start piling up: Are natural anti-inflammatories truly safer? Are prescription drugs more effective? Which option is actually right for me?
These questions arise because people want to manage pain and inflammation responsibly. Many are concerned about the side effects of long-term medication use, while others worry that natural remedies may not be strong enough to provide meaningful relief. The reality is less dramatic than the headlines suggest and more practical.
Natural and prescription anti-inflammatories aren’t rivals in a battle of “better or worse.” They work through different mechanisms, target inflammation at different levels, and serve different purposes depending on the situation. Understanding the distinctions between these approaches allows you to make informed choices.
You can effectively treat mild, everyday inflammation with natural options while reserving prescription medications for situations that truly require them, thereby reducing unnecessary exposure to drugs without leaving serious inflammation undertreated. In short, both are tools, and knowing how and when to use each one is the key to safer, more effective inflammation management.
What Inflammation Actually Is and Why Treatment Depends on Severity
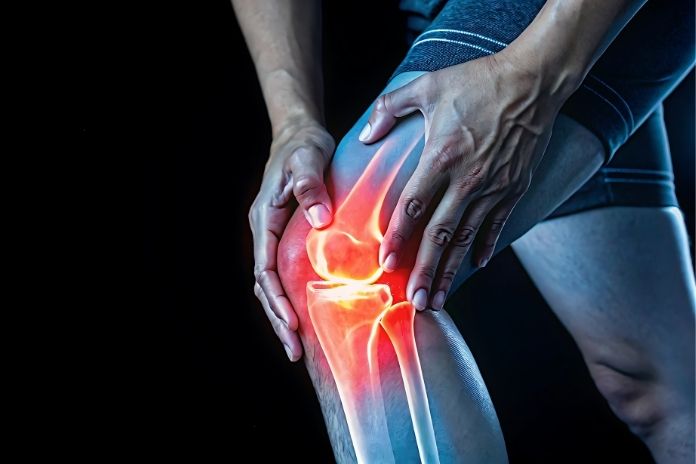
Inflammation is not the enemy. It’s the body’s repair system. When tissue is injured or infected, the immune system sends chemical signals that increase blood flow, bring in immune cells, and start healing. Redness, heat, swelling, and pain are signs that this process is working.
The problem starts when inflammation does not turn off.
Acute vs. Chronic Inflammation
Acute inflammation is short-term and useful. You sprain an ankle, it swells, the injury repairs, and the inflammation fades.
Chronic inflammation stays active even when there is nothing to fix. Instead of healing, it slowly damages healthy tissue and is linked to conditions like heart disease, diabetes, arthritis, autoimmune disorders, and depression.
Inflammation can either heal you or harm you. Time and cause decide which one it becomes.
Pain Is Not Always Inflammation
Some pain is inflammatory, like arthritis or autoimmune flares. Other pain is mechanical or nerve-related, like muscle tightness or disc problems. Anti-inflammatory drugs only help when inflammation is actually driving the pain.
Suppressing helpful inflammation can slow healing. Letting harmful inflammation continue causes lasting damage. The goal is to control the right kind, not eliminate it.
Why Not All Inflammation Needs Medication
Low-grade inflammation from stress, poor sleep, diet, or overuse usually improves with rest, movement, nutrition, and time. Your body can regulate this on its own. But severe, systemic, or autoimmune-driven inflammation cannot. That’s when prescription anti-inflammatories and immune-modulating drugs are needed to prevent tissue damage.
Natural strategies support background inflammation and recovery. Prescription drugs are for inflammation that the body cannot control by itself. The right treatment depends on how severe it is, how long it’s been there, and what’s causing it.
“Many people ask me if they should take something ‘just to lower inflammation.’ The reality is that inflammation itself isn’t always harmful. Acute inflammation helps the body heal. Medications are most useful when inflammation is persistent, damaging tissues, or part of a chronic disease process rather than a short-lived response,” says Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health.
Read More: 6 Everyday Household Items That May Be Triggering Inflammation
What Prescription Anti-Inflammatories Do in the Body
Prescription anti-inflammatories do not just dull pain. They interrupt the chemical systems that create inflammation.
When the immune system detects injury or threat, it releases signals that increase blood flow, activate immune cells, and sensitize nerves. That process creates swelling, heat, stiffness, and pain. Prescription drugs step into that cascade and turn it down or shut parts of it off, which is why they work fast and predictably.
How NSAIDs Work
NSAIDs like ibuprofen, naproxen, and diclofenac are used when inflammation becomes painful or function-limiting. They work by blocking COX enzymes, which the body uses to produce prostaglandins, compounds that drive pain, swelling, and fever.
When prostaglandin levels drop, nerve sensitivity decreases, and inflamed tissues calm down. That’s why NSAIDs can quickly reduce pain and stiffness during injuries or inflammatory flare-ups.
But prostaglandins also play protective roles. Some help maintain the stomach lining, support kidney blood flow, and regulate blood vessel function. NSAIDs block these signals as well. Research shows that altering prostaglandin balance can increase cardiovascular risk with certain NSAIDs by affecting blood vessel tone and clotting pathways, which is why doctors factor in heart disease risk, dosage, and duration before prescribing them.
This tradeoff explains why NSAIDs are best suited for short-term or severe inflammation, not low-grade inflammation caused by stress, poor sleep, or overuse. The goal isn’t to eliminate inflammation but to intervene when the body can’t control it without potential tissue damage.
How Corticosteroids Work
Corticosteroids work on a deeper level. Instead of blocking one pathway, they suppress the immune system’s inflammatory response itself.
They reduce cytokines, limit immune cell activity, and prevent fluid and inflammatory cells from flooding tissues. This is why steroids are so effective for autoimmune diseases, asthma attacks, allergic reactions, and severe joint or organ inflammation.
But that power comes with side effects. Long-term use raises infection risk, weakens bones, disrupts hormones, and slows healing, which is why steroids are used carefully and usually for the short term.
What This Means
NSAIDs quiet inflammatory chemicals. Steroids quiet the immune system.
Both are essential when inflammation is causing damage. Neither is meant for everyday aches or mild lifestyle-related inflammation. Used correctly, they protect tissue. Used casually, they create new problems.
Benefits of Prescription Anti-Inflammatory Medications
Prescription anti-inflammatory drugs exist because some inflammation is too aggressive to be left alone.
When the immune system is attacking joints, lining the gut with ulcers, or flooding tissues with inflammatory chemicals, waiting it out is not an option. These drugs are designed for moments when inflammation is actively causing damage.
- They stop dangerous inflammation: When the immune system attacks joints, organs, or tissues, waiting causes real damage. These drugs exist to bring aggressive inflammation under control before it destroys healthy tissue.
- They provide fast relief: NSAIDs and corticosteroids reduce swelling and pain within hours, not weeks. That speed protects movement, breathing, sleep, and the body’s ability to heal.
- They prevent long-term injury: Uncontrolled inflammation leads to joint damage, airway scarring, and organ injury. Prescription anti-inflammatories interrupt that process before it becomes permanent.
- They offer precise, predictable dosing: Doctors know how long these drugs last, how strong they are, and how the body processes them. That allows inflammation to be treated with accuracy instead of guesswork.
- They can be adjusted based on response: If symptoms return or side effects appear, the dose or medication can be changed. This flexibility makes them safe enough for hospital and long-term use.
- They are essential for serious inflammatory diseases: Conditions like rheumatoid arthritis, lupus, severe asthma, and inflammatory bowel disease cannot be controlled with lifestyle changes alone. Medication is what stops the immune system from causing ongoing damage.
Risks and Side Effects of Prescription Anti-Inflammatories
Here’s the tradeoff. When you interfere with inflammation, you are also interfering with systems the body uses to protect itself.
That doesn’t make these drugs bad. It means they need to be used with respect.
- Gastrointestinal irritation and bleeding: NSAIDs block prostaglandins that protect the stomach lining, so that the protective barrier slowly weakens. Over time, this can lead to heartburn, ulcers, or internal bleeding, especially with higher doses, long-term use, alcohol, or older age.
- Cardiovascular risk: Some NSAIDs slightly increase the risk of heart attack and stroke when used long-term or at high doses. This happens because COX-2 inhibition shifts the balance between blood vessel relaxation and clot formation, which matters more in people with existing heart risk.
- Kidney and blood pressure effects: Prostaglandins help maintain healthy blood flow inside the kidneys, and NSAIDs interfere with that process. This can reduce kidney filtration and increase sodium retention, which pushes blood pressure up and can worsen kidney function over time.
- Corticosteroid-specific risks: Steroids suppress the immune system and disrupt normal hormone signaling, not just inflammation. With long-term use, they can raise blood sugar, weaken bones, thin skin, slow healing, and increase infection risk, which is why they are used in short courses or carefully tapered schedules.
Why Long-Term Use Requires Medical Supervision
Prescription anti-inflammatory drugs are not wellness tools. They are medical interventions designed to stop tissue damage when the immune system is no longer regulating inflammation on its own.
Used correctly, these medications protect organs, preserve function, and prevent long-term complications. Used casually or without monitoring, they can suppress normal immune defenses and create serious risks over time.
As rheumatologist Dr. Jessica K. Gordon, MD, explains, disease-modifying anti-rheumatic drugs and other prescription anti-inflammatory therapies can be lifesaving in chronic autoimmune conditions, but they require careful monitoring because they suppress the immune system and can have serious side effects if not managed over time.
That’s the balance. When inflammation is severe, persistent, or autoimmune-driven, these drugs are essential. When inflammation is mild or self-limited, they’re often unnecessary. Knowing the difference is what makes treatment effective instead of risky.
What Natural Anti-Inflammatories Actually Do

Natural anti-inflammatory remedies don’t try to overpower the immune system. They work by nudging it back toward balance.
Instead of blocking inflammation outright, they influence the signals that tell your body how much inflammation to produce and how long it should last. That makes them slower, gentler, and far better suited for long-term use.
Foods and Compounds With Real Anti-Inflammatory Effects
A few natural compounds have a strong scientific backing behind them.
- Omega-3 fatty acids: Found in fatty fish like salmon and sardines, omega-3s reduce the production of inflammatory eicosanoids and cytokines. They also help stabilize cell membranes, which makes immune reactions less explosive.
- Curcumin from turmeric: Curcumin inhibits NF-κB, one of the main switches that turns inflammatory genes on. It doesn’t shut inflammation off. It turns the volume down.
- Gingerols from ginger: These compounds reduce prostaglandin formation and oxidative stress, which is why ginger can ease joint pain, muscle soreness, and digestive inflammation.
- Polyphenols: Found in berries, olive oil, tea, cocoa, herbs, and vegetables, polyphenols regulate immune signaling and protect cells from oxidative damage that keeps inflammation smoldering.
These compounds don’t behave like drugs. They don’t force inflammation to stop. They reshape how the immune system reacts to stress, food, microbes, and injury.
Read More: Best Foods to Eat with Omega-3 Supplements: How to Boost Absorption and Maximize Benefits
How Natural Options Modulate Inflammatory Pathways
Natural anti-inflammatories don’t shut inflammation off. They help the body regulate itself more effectively.
A systematic review found that plant-based dietary patterns, like the Mediterranean or DASH diet, are associated with lower levels of oxidative stress and inflammation biomarkers compared with Western or processed diets.
These diets are rich in antioxidants and anti-inflammatory nutrients, which reduce oxidative stress and the overproduction of pro-inflammatory cytokines such as IL-6 and TNF-α.
What this really means is that natural strategies make the inflammatory response more controlled and less destructive, rather than eliminating it entirely. The immune system still responds to threats, but with less unnecessary amplification.
Unlike corticosteroids, these natural approaches don’t suppress immune defense. You can still fight infections, you just do it without the collateral damage that comes from broad immune suppression.
That’s why dietary and lifestyle-based anti-inflammatory strategies are valuable for prevention and long-term management, not for medical emergencies where inflammation is already causing active tissue damage.
Benefits of Natural Anti-Inflammatories
Natural anti-inflammatories are built for steady, long-term support rather than quick symptom shutdown.
- Lower risk when used correctly: When these compounds come from food or well-made supplements, the risk of serious side effects is low. You are supporting pathways the body already uses, which makes them safe for long-term, daily use.
- They support long-term inflammation control: Chronic low-grade inflammation from stress, poor sleep, blood sugar swings, gut issues, and aging responds best to steady, gentle regulation. Natural anti-inflammatories help keep the immune system from staying stuck in a mildly inflamed state.
- They improve more than just inflammation: Most anti-inflammatory foods also improve insulin sensitivity, cholesterol balance, blood vessel function, and gut microbiome health. That means you are not just calming inflammation but strengthening the systems that regulate it.
Limitations of Natural Anti-Inflammatories
This is where social media often gets it wrong.
- They Work Slowly: You do not feel turmeric, ginger, or omega-3s in an hour. Their effects build over weeks as cell membranes change, oxidative stress drops, and immune signaling recalibrates. They are not painkillers. They are long-term regulators.
- They Are Too Weak for Severe Inflammation: Autoimmune flares, surgical inflammation, major injuries, or inflammatory bowel disease are not problems you can fix with tea and spices. In those situations, the immune system is causing active tissue damage. You need medical anti-inflammatories to stop that.
- Supplement Quality Matters: A high-quality curcumin extract with good absorption is not the same as a random capsule off the internet. Many supplements are underdosed, poorly absorbed, or contaminated. When people say natural remedies don’t work, they are often using products that barely contain the active compounds.
- They Do Not Replace Medical Care: Natural anti-inflammatories are supportive tools. They are not treatments for serious diseases. They help control background inflammation and support recovery. Not only that, but they do not stop aggressive immune attacks. Confusing the two delays real treatment and makes outcomes worse.
What this all comes down to is simple. Natural anti-inflammatories are built for balance. Prescription anti-inflammatories are built for battle. Knowing which situation you are in makes all the difference.
Natural vs. Prescription Anti-Inflammatories
Here’s the thing. Most people treat this like a good vs. bad debate. It isn’t.
Natural and prescription anti-inflammatories are built for different jobs. One is designed to manage long-term background inflammation. The other is designed to stop active, damaging inflammation fast. When you understand that, the whole comparison becomes clear.
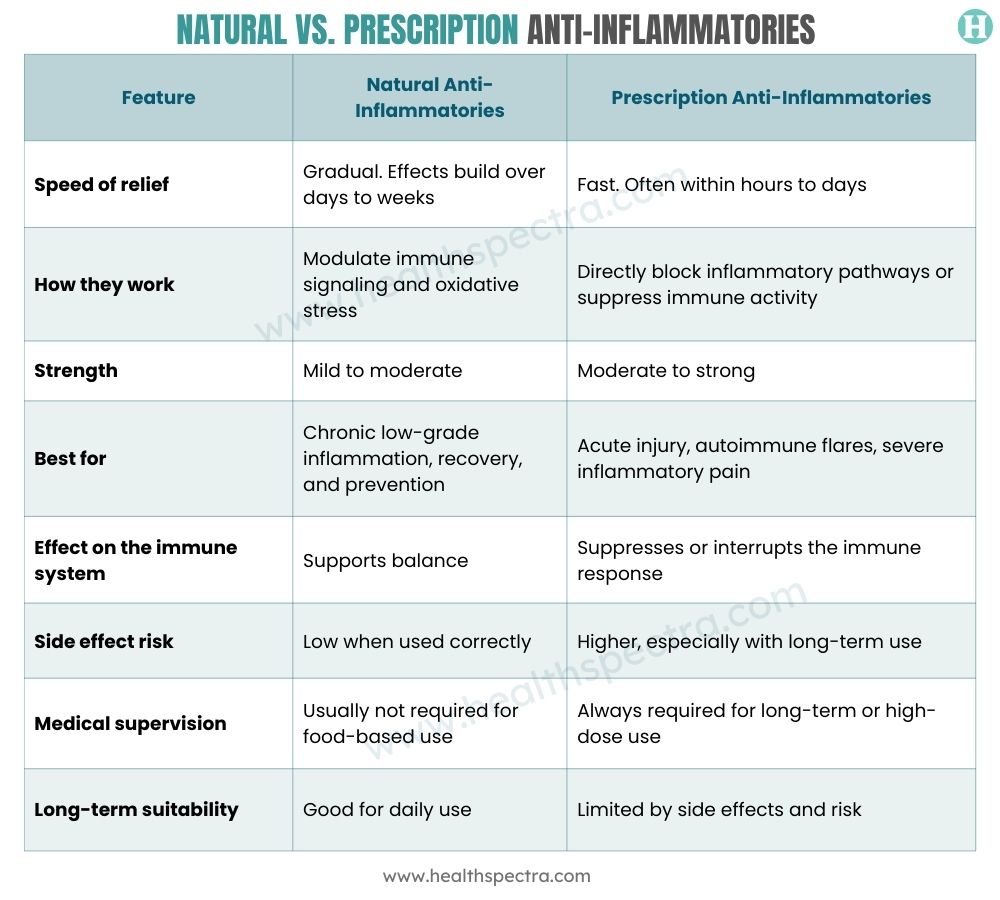 Natural anti-inflammatories help keep the immune system steady over time. Prescription anti-inflammatories step in when inflammation is actively causing damage. One manages the background. The other handles the emergency. Knowing which situation you’re in is what makes treatment work.
Natural anti-inflammatories help keep the immune system steady over time. Prescription anti-inflammatories step in when inflammation is actively causing damage. One manages the background. The other handles the emergency. Knowing which situation you’re in is what makes treatment work.
Which Is Better for Different Types of Inflammation?
Not all inflammation requires the same approach. Cause, intensity, and duration matter.
- Acute Injury or Severe Pain: When you twist a knee, have surgery, or face a sudden flare-up, fast action is key. Prescription anti-inflammatories work best when pain is severe, swelling limits movement, or tissue is at risk.
NSAIDs reduce swelling and pain quickly, while corticosteroids handle extreme inflammation that threatens nerves, joints, or organs. This is not the time for slow, nutritional strategies.
- Chronic Low-Grade Inflammation: Low-grade inflammation from stress, poor sleep, insulin resistance, gut issues, or aging rarely causes sharp pain but raises long-term health risks.
Diet, movement, omega-3s, polyphenols, turmeric, and sleep quality are far more effective here than medication. Prescription drugs only mask symptoms; natural strategies address root causes and are better for long-term management.
- Autoimmune and Inflammatory Diseases: When the immune system attacks the body, medical intervention is essential. Conditions like rheumatoid arthritis, lupus, IBD, severe asthma, and psoriasis require prescription anti-inflammatory or immune-modulating therapy. Natural approaches can support recovery but cannot prevent tissue damage on their own.
Can Natural and Prescription Approaches Be Combined?
Yes. Short-term NSAIDs or steroids can control acute flares, while long-term dietary and lifestyle strategies prevent recurrence. Coordination matters, though; high-dose omega-3s may increase bleeding risk with NSAIDs, and turmeric can affect drug metabolism. Always let your doctor know what you’re taking.
How to Choose the Right Approach?
Ask yourself three questions: How severe is the inflammation? How long has it been present? What’s causing it? Escalate care if pain persists or interferes with daily life. For chronic, manageable inflammation, focus on lifestyle and natural strategies. Relief matters, but long-term health matters more.
Read More: How to Build an Anti-Inflammatory Morning Routine
Key Takeaway
Prescription anti-inflammatories exist because some inflammation is dangerous. When swelling, pain, or immune activity is actively damaging tissue, these drugs step in fast and stop the process. They are precise, powerful, and medically necessary in those moments.
Natural anti-inflammatories serve a different purpose. They help the body stay out of that danger zone in the first place. By lowering oxidative stress, calming immune signaling, and improving metabolic health, they reduce the background inflammation that quietly builds toward bigger problems.
What this really means is that you do not have to choose sides.
Short-term medication can put out the fire. Long-term nutrition, movement, and targeted natural compounds keep the conditions that start the fire from returning. The smartest approach is not natural versus prescription. It is using the right tool for the level of inflammation you are dealing with and knowing when to shift from crisis control to long-term balance.
References
- Cleveland Clinic. (n.d.). Inflammation.
- StatPearls Publishing. (2023). Inflammation. In StatPearls. National Center for Biotechnology Information.
- Siloam Hospitals. (n.d.). What is inflammation?
- Wikipedia contributors. (n.d.). Inflammation.
- Physio-pedia. (n.d.). Inflammation: Acute and chronic.
- Netmeds. (n.d.). Inflammation: Types, causes, symptoms, and treatment.
- González-Gallego, J., García-Mediavilla, M. V., Sánchez-Campos, S., & Tuñón, M. J. (2022). Anti-inflammatory properties of dietary polyphenols. International Journal of Molecular Sciences, 23(23), 14905.
- Sparsh Hospital. (n.d.). Inflammation.
- OSF HealthCare. (n.d.). What you should know about inflammation.
- WebMD. (n.d.). Inflammation.
- Aditya Birla Capital. (2024, August 27). Inflammation: Causes, symptoms, and treatment.
- Barbaresko, J., Koch, M., Schulze, M. B., & Nöthlings, U. (2021). Dietary patterns and biomarkers of oxidative stress and inflammation: A systematic review. Redox Biology, 42, 101933.
- Hospital for Special Surgery. (n.d.). DMARDs for rheumatic disease.
- Bally, M., et al. (2017). Risk of acute myocardial infarction with NSAIDs. BMJ, 357, j1909.
- Harvard Health Publishing. (n.d.). Can medication tame chronic inflammation?
In this Article
















