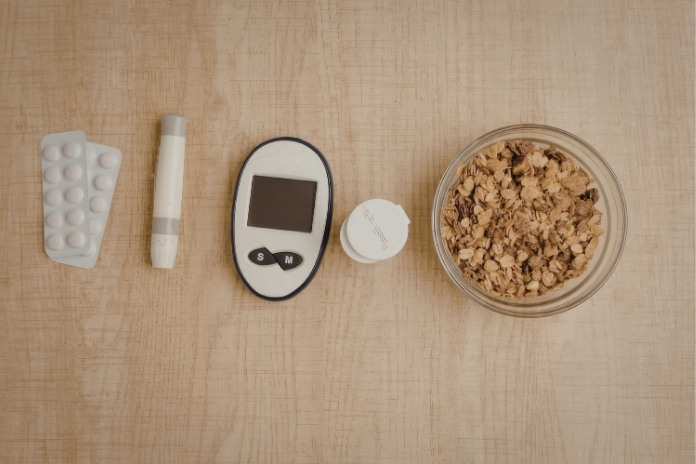
- Eating late at night can raise blood sugar because melatonin reduces glucose tolerance.
- Frequent bedtime snacking may increase the long-term risk of type 2 diabetes, especially for shift workers.
- Finishing dinner 2–3 hours before bedtime helps stabilize blood sugar and improve sleep quality.
The main goal of blood sugar control for those with diabetes or prediabetes is frequently controlling meal choices. But nutrition science is rapidly demonstrating that timing your meals might be just as crucial as what you eat.
Many individuals think that having a little snack before bed is safe; however, studies indicate that the risks of bedtime snacking for diabetes may be greater than previously believed. The connection between sleep hormones and metabolic activities is the cause.
Melatonin, the hormone that tells the brain it’s time to sleep, is produced by the body as night falls. The body’s capacity to metabolize glucose simultaneously alters. Eating late at night can disrupt normal insulin function, as melatonin and blood sugar regulation are closely linked, according to scientific research.
This article discusses the research underlying the connection between metabolism and sleep hormones. We’ll talk about how melatonin and blood sugar interact in the body, why nibbling before bed raises the risk of diabetes at night, and potential interactions between melatonin supplements and glucose.
Read More: Melatonin for Your Gut? The Surprising Role of the Sleep Hormone in Managing IBS Cramping
How Melatonin Affects Metabolism and Blood Sugar
Most people think of melatonin as the hormone that promotes sleep. The pineal gland secretes it and is essential for controlling the circadian rhythm, the biological clock that synchronizes cycles of sleep and wakefulness. But it affects more than sleep.
Recent studies suggest that melatonin and glucose metabolism are closely related, suggesting that melatonin may play a role in controlling blood sugar levels.
Melatonin works by connecting to specific receptors throughout your body. In the pancreas, the gland that makes insulin, there are two key receptors called MT1 and MT2.
To ensure energy processing aligns with regular biological cycles, these receptors help coordinate metabolic activity with the body’s circadian rhythm.
Glucose metabolism depends on a delicate balance between hormones, mainly glucagon and insulin, that keep your blood sugar in check. Melatonin steps in here, too, though not directly.
It tweaks how sensitive your cells are to insulin and affects how much the pancreas releases. At night, when melatonin hits its highest point, your body shifts gears into rest-and-repair mode.
That’s when your glucose tolerance drops.
This nighttime reduction in glucose tolerance explains how meal timing affects blood sugar. When you eat a meal late at night, blood sugar levels may rise more than when you eat it during the day.
Why “Bedtime Snacking” Raises Diabetes Risk

1. Impaired Glucose Tolerance at Night
One of the most important reasons bedtime snacking increases the risk of diabetes at night is reduced glucose tolerance. Eating carbs late at night makes it harder for your body to handle glucose, so your blood sugar and insulin go up.
That’s bad news for fat burning while you sleep, and you’ll probably wake up with higher blood sugar, too. If you’re at risk for diabetes, this really matters, since doctors check your morning numbers to see how well you’re managing your glucose.
Eating late at night messes with the way your body’s supposed to wind down. When you have food right before bed, your body has to kick into gear and start digesting, which actually takes a lot of energy.
Blood rushes to your stomach, your body temperature goes up, and instead of settling down, your system stays busy. It’s no wonder you have a tough time falling into that deep, restful sleep.
2. Genetic Factor — The MTNR1B Gene
Everybody reacts differently to melatonin. Genetic variations can significantly affect how the body uses glucose at night.
The MTNR1B gene and diabetes risk are among the most significant findings in this area. The melatonin receptor type 2 (MT2) present in pancreatic cells is encoded by this gene.
The G-allele is a genetic variation found in certain people. Stronger melatonin signaling in the pancreas may further reduce insulin release in individuals with this variation, according to research.
3. Compounded Risk for Shift Workers and Late Eaters
People who frequently eat at odd hours are another group at higher risk of metabolic problems. People who work shifts, work nights, or have irregular sleep schedules frequently have their biological clocks and daily routines out of sync.
The difference between circadian rhythm and metabolism might affect hormonal control, such as insulin signaling and melatonin synthesis.
Shift work may increase the risk of heart disease, stroke, diabetes, dementia, cardiovascular disease, and cancer-related mortality.
Avoiding nighttime meals can help prevent circadian misalignment, much as avoiding bright lights at night might. Even though we can’t control the lighting at work, we may restrict our food intake overnight, which has been shown to help reduce the adverse metabolic effects of working shifts.
One explanation is that eating during the body’s biological nighttime puts the body in a state where digestion is still ongoing, but melatonin levels are high. A metabolic conflict results from this.
Read More: Can Melatonin Supplements Harm Your Sleep Cycle Long-Term
Melatonin Supplements — Hidden Risks for Diabetic Control
To enhance the quality of their sleep, many people use melatonin tablets. When taken incorrectly, these supplements may harm metabolic health, even if they are beneficial for some sleep disorders.
Researchers are increasingly studying the relationship between melatonin supplements and glucose levels. Higher melatonin doses taken at night may lead to residual hormone levels persisting during the day.
Glycemic variability may increase if circulating melatonin remains elevated during the day or at mealtimes, disrupting normal glucose metabolism. Genetic variables also influence individual reactions to melatonin.
Specifically, melatonin sensitivity has been demonstrated to be influenced by the MTNR1B gene polymorphism rs10830963. The G allele mutation is associated with increased melatonin sensitivity, decreased insulin production, and an increased risk of type 2 diabetes.
Experts advise waiting at least two hours between taking melatonin pills and eating because of this impact. It prevents elevated melatonin levels from interfering with the body’s ability to digest glucose.
Those who need to use extra caution are:
- Individuals who have prediabetes.
- People experiencing melatonin and insulin resistance.
- Those who take insulin.
The Smart Timing Strategy for Stable Blood Sugar
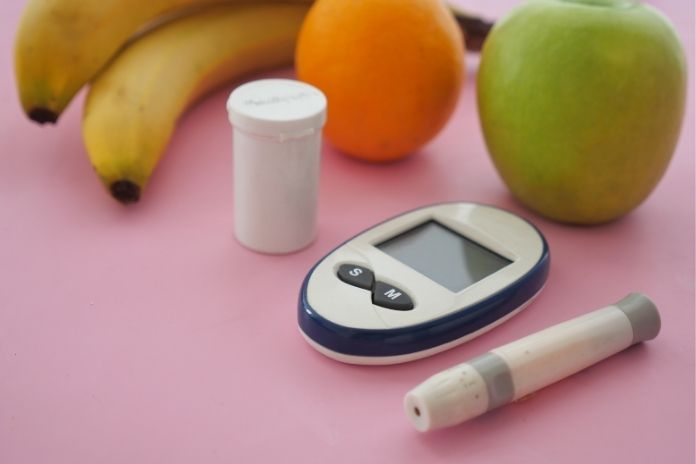
1. The “2–3 Hour Rule” Before Bedtime
Changing meal timing is one of the easiest ways to enhance metabolic health. Eating late might delay sleep. The circadian rhythm, your body’s internal clock, tells you when to go to sleep and get up.
Melatonin release can be delayed by eating too late at night, especially if the meal is substantial or hot.
Meals should be finished 2 to 3 hours before bedtime for optimal digestion and sleep. It allows your body adequate time to digest food without interfering with your sleep. Generally speaking, you should finish your evening meal by 6 or 7 p.m.
The Best Ways to Eat in the Evening:
- Dinner should be balanced, light, and have enough protein and fiber.
- Steer clear of sugary or highly processed foods right before bed.
- Choose a modest, high-protein bedtime snack for diabetics, such as yogurt or nuts, if you’re hungry right before bed.
Adhering to this recommendation reduces the possibility that melatonin–blood sugar interactions interfere with insulin release.
2. Best Nighttime Snack Options (When Needed)
Snacking at night may be medically required in certain circumstances. For instance, a light snack may be necessary for people taking insulin or other diabetes medications to avoid hypoglycemia overnight.
Selecting the appropriate cuisine becomes crucial when snacks are required. A high-protein bedtime snack for diabetics can help stabilize blood sugar levels without causing significant spikes in blood sugar.
Examples include:
- Almond butter and banana.
- Oatmeal.
- Fruit.
- Hard-boiled eggs.
- A tiny amount of seeds and nuts.
- Cheese that is low in fat and carbs.
These foods minimize rapid spikes in blood sugar while providing protein and healthy fats.
Read More: Beyond Weight Loss: GLP-1 Benefits for Heart Disease and Diabetes Prevention
3. Aligning Meal Timing With Circadian Rhythms
Chrononutrition examines how our eating patterns and body clocks interact. These days, life moves fast, and it’s easy to grab whatever’s quick, not what’s healthiest. Most people barely think about what they eat or how much they eat.
But studies show that syncing meal times with your natural daily rhythms can significantly affect your health. Turns out, timing matters a lot more than we thought.
Our bodies run better when we eat at times that match our natural daily rhythms.
Here’s how you can sync your meals with your circadian cycle:
Start your Day with a Hearty Breakfast: Seriously, don’t skimp in the morning; your metabolism kicks into gear early, so give it plenty to work with. As the day goes on, try to eat a little less at each meal, and keep dinner on the lighter side.
Stick to Regular Mealtimes: Eating at the same times each day helps keep your internal clock steady, so your body knows what to expect. It’s a simple move, but it really helps you feel more balanced.
Mindful Eating: Observe signs of hunger and fullness as you eat. Eating comfortably and enjoying your food improves digestion.
Prevent Late-Night Snacking: To promote restful sleep, avoid consuming large or sugary snacks right before bed.
For individuals with irregular sleep schedules, maintaining consistent eating windows may help reduce the negative effects of shift work and diabetes control.
Long-Term Impacts — From Elevated Glucose to Metabolic Syndrome

Frequent nighttime glucose surges may not seem like much at first, but they can have detrimental effects on metabolism over time.
Insulin sensitivity may progressively deteriorate if melatonin and blood sugar regulation are chronically out of sync. Melatonin and insulin resistance are developed as a result of this process, making glucose regulation more challenging.
This metabolic disturbance increases the risk of metabolic syndrome when paired with inadequate sleep, erratic eating habits, and sedentary lifestyles.
Several illnesses are included in metabolic syndrome, including:
- Elevated blood sugar.
- Increased fat in the abdomen.
- Elevated blood pressure.
Read More: Diabetes Diet: How Plant-Based Eating Can Transform Your Health
Conclusion
Managing diabetes isn’t just about counting the calories or carbs. In fact, it is more than that. Emerging research shows that meal timing affects blood sugar levels, playing a crucial role in overall glucose control.
Eating late at night can disrupt insulin release and raise blood sugar levels because melatonin levels naturally rise at this time. Over time, bedtime snacking may subtly disrupt metabolic balance through the interplay between melatonin and blood sugar.
If you’re aiming for steadier blood sugar and deeper sleep, have dinner earlier. Let your meals line up with your body’s natural rhythm. When you focus on what you eat and when you eat it, you set yourself up for healthier days ahead, and it’s a smart, lasting way to manage diabetes and protect your overall health.
References
- Heather Grey. (November 30, 2023). How does melatonin affect insulin sensitivity and metabolic health with diabetes?
- Hong, S. H., & Kim, J. (June 27, 2024). Melatonin and metabolic disorders: Unraveling the interplay with glucose and lipid metabolism, adipose tissue, and inflammation.
- ImArabic. How does melatonin affect blood sugar levels?
- National Health Service. (2023, February 13). How and when to take melatonin.
- American Heart Association. (2025, November 3). Long-term use of melatonin supplements to support sleep may have negative health effects.
- Mendez, E. Eating before bed: How late-night snacks affect sleep and digestive health.
- Gillaspy, B. (2020, September 22). Bedtime snacking: Here’s what happens inside you.
- Natalie Dragon. (November 8, 2024). Meal timing crucial for night shift worker health.
- Aggarwal, B. (2024, February 22). Count down—not sheep—to a good night’s sleep.
- Eating for you. (2025, March 10). Food and sleep: The hidden connection you need to know.
- Danielle Pacheco. (July 16, 2025). Healthy Bedtime Snacks to Eat Before Sleep.
In this Article