People with diabetes rarely worry about protein powders because of the fitness culture. They worry because of one simple moment that keeps repeating.
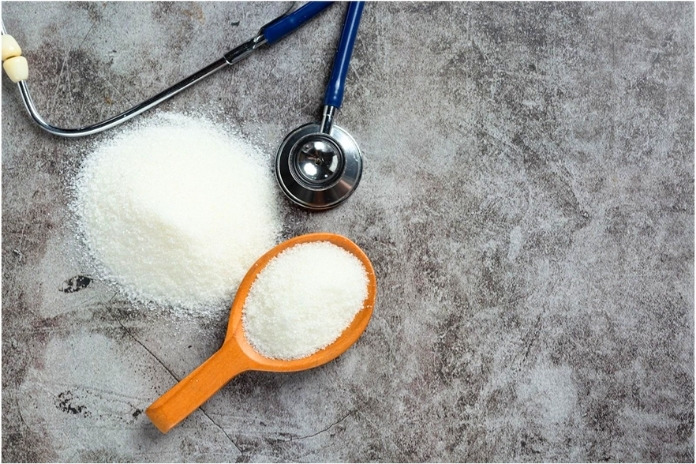
They drink a protein shake. They expect nothing dramatic. Then the glucometer shows a high number that doesn’t make sense. No sugar. No banana. No cookie. Still, the reading is higher than expected.
So the question becomes quieter, more cautious: Is protein powder safe for diabetics… or am I missing something?
This article is not here to sell protein powder or scare you away from it. It’s here to explain why protein powder behaves differently in diabetic bodies than nutrition charts suggest, and why the truth lies somewhat uncomfortably in between.
Protein Powder and Blood Sugar: The Part Everyone Explains, and the Part They Don’t
Yes, protein does not turn directly into glucose the way carbohydrates do. That part is correct. But that explanation is incomplete, and for diabetics, incomplete explanations cause confusion.
Protein triggers insulin. not because it contains sugar, but because the body releases insulin to help move amino acids into cells. In people without insulin resistance, this process is smooth and balanced. In people with type 2 diabetes, however, the response is often delayed, exaggerated, or inconsistent.
Amino acids are the building blocks of protein. After you consume protein, these amino acids enter the bloodstream and are used for muscle repair, hormones, and other essential functions. When more amino acids are present than the body immediately needs, the liver may later convert some of them into glucose to maintain energy balance.
This is why protein powder can look harmless at 1 hour and confusing at 3 hours. Insulin may rise first, followed by a delayed release of glucose as the liver processes excess amino acids. Most people stop testing early, assume protein “did nothing,” and move on. In reality, the body is still processing it.
Protein also slows stomach emptying. That’s generally helpful when protein is part of a solid meal because it blunts rapid glucose spikes. But it becomes less predictable when protein is consumed in liquid form, fast-absorbing, easy to overconsume, and often taken on an empty stomach, which is how most protein shakes are used.
So no, protein powder for diabetes is not neutral. Its effects are subtle, delayed, and highly dependent on form, timing, and insulin sensitivity, which makes them harder to interpret without close monitoring.
Read More: Is Your Morning Smoothie Secretly Spiking Your Blood Sugar?
Why Protein Powder Sometimes Helps People With Diabetes

Protein powder helps when it solves a specific problem. Not when it’s added casually.
One real benefit is predictability. Unlike mixed meals, protein powders have a known and repeatable composition. That makes it easier to track glucose patterns and understand what your body is responding to.
Another benefit is muscle preservation. Losing muscle worsens insulin resistance over time, and many people with diabetes unknowingly eat too little protein, especially when they cut carbohydrates aggressively. Maintaining muscle helps the body handle glucose more efficiently.
Protein powder can also reduce post-meal glucose swings when it replaces refined carbohydrates, not when it’s added on top of them. This effect shows up consistently in continuous glucose monitor (CGM) data, even though it’s rarely discussed in clinic conversations.
When Protein Powder May Be a Problem for Diabetes
Protein powder can become a problem when it bypasses normal appetite regulation.
Liquids don’t activate chewing, stomach stretch, or the usual satiety signals that tell you you’ve eaten enough. That makes it easy to consume more protein than intended without feeling full. Excess protein doesn’t disappear. It increases metabolic load (the extra work the liver and kidneys must do to process and clear nutrients), on the liver and kidneys and may convert to glucose over time.
Another issue is insulin overshoot. Certain proteins stimulate insulin strongly. In people with insulin resistance, this can lead to increased hunger two to three hours later, triggering additional intake that feels disconnected from the original shake.
Clinicians who follow long-term patterns often see this mismatch between short-term glucose stability and later effects. “I don’t recommend using protein powders except in a few instances, and only with supervision,” says registered dietitian Kathy McManus.
This helps explain why some people report, “protein shakes make me more hungry,” even when their glucose readings initially look stable.
Read More: Top 7 Healthy Snacks on the Go: Portable and Nutrient-Rich Foods and Snack Options
Whey, Plant, Egg: The Conversation That Misses the Point

People often ask which protein is “best” for diabetes. That question assumes there is a single correct answer. There isn’t.
Whey protein acts fast. It stimulates insulin strongly. For some people, this improves post-meal glucose control. For others, it overshoots and leads to later instability.
Plant proteins digest more slowly, especially when blended with fiber. But they vary wildly between brands. Some are clean. Some are carb-heavy with better marketing.
Egg and casein proteins are digested slowly and steadily. They don’t feel impressive. They don’t give a “kick”. But metabolically, they are often easier to manage.
None of these are universally safe or unsafe. The body doesn’t care about protein categories. It cares about absorption speed, total load, and timing.
Read More: Can You Mix Creatine with Coffee? What Happens When You Combine Them
Protein Powders That Impair Blood Sugar

Some protein products should raise immediate red flags.
Meal replacement shakes often contain added sugars disguised as nutrition. They’re formulated for taste and compliance, not for blood sugar control.
Mass gainers are even more straightforward. They are high-carbohydrate supplements marketed as protein, and they reliably raise glucose.
Flavored protein powders can also be problematic, even when labeled “sugar-free.” Sweeteners, fillers, and added starches still affect digestion, insulin response, and appetite. This isn’t accidental.
“A lot of companies use fillers or flavor enhancers designed by food scientists to create flavors beyond the standard vanilla, chocolate, and strawberry,” says registered dietitian Kate Patton.
As a general rule, if one scoop contains nearly as many carbohydrates as protein, it’s not appropriate for regular use in diabetes — regardless of branding or health claims.
Read More: Food Allergy vs. Intolerance: How to Tell the Difference and Why It Matters
Using Protein Powder Without Fighting Your Blood Sugar
Protein powder works best when it behaves like food, not a beverage. That means:
- Taking it with meals, not instead of them
- Pairing it with fiber or fat
- Avoiding sweet liquids
- Slowing consumption rather than gulping
Timing matters. Protein taken after physical activity is more likely to be directed toward muscle repair and replenishment when muscles are more insulin-sensitive. In this context, amino acids are used efficiently, and delayed glucose rises are often smaller or absent.
Protein taken late at night, especially after a sedentary day, behaves differently. With lower energy demand and reduced insulin sensitivity, excess amino acids are more likely to be processed by the liver and gradually converted into glucose, which can raise fasting or early-morning blood sugar levels.
Context matters as well. A protein shake for diabetes consumed with a balanced meal tends to digest more slowly and produce a flatter glucose curve. The same shake taken after skipping a meal or on an empty stomach is absorbed faster, triggers a stronger insulin response, and is more likely to produce a delayed glucose rise hours later.
This is why how protein powder is used matters as much as how much is used:
- With meals: Fiber and fat slow digestion, spreading amino acid absorption over time, and reducing delayed glucose release.
- Not gulped: Drinking protein quickly delivers a large amino acid load at once, increasing the chance that excess will later be converted to glucose.
- Paired with food: Protein alone behaves more like a metabolic stressor; protein with food behaves more like nutrition.
On a glucometer, this often shows up as normal or slightly lower readings in the first hour, followed by a gradual rise 2-4 hours later, especially when protein is taken alone, late in the day, or in large liquid doses.
These differences don’t show up in studies easily, but they show up clearly on glucometers.
Read More: How to Make Oatmeal Diabetes-Friendly: Toppings and Recipes That Work
How Much Is Too Much?
More protein does not always mean better blood sugar control.
For most adults with diabetes, 15–25 grams per serving is sufficient. That’s roughly ½ to 1 standard scoop of protein powder, or about the same protein you’d get from 2-3 eggs, a cup of Greek yogurt, or a palm-sized portion of chicken. Beyond this, benefits plateau while metabolic cost increases.
Total daily protein intake matters more than per-scoop numbers. For most adults with diabetes, this usually falls around 0.8-1.2 grams of protein per kilogram of body weight per day, depending on age, activity level, and kidney health. A person already eating adequate protein does not gain much by adding powder daily.
Read More: How to Lower Cholesterol During Menopause: Effective Strategies for Cardio Health
Protein Powder and Kidney Health in Diabetes
Diabetes changes kidney risk over time. Even mild kidney changes alter how protein waste is handled. High protein intake increases filtration pressure (the extra strain placed on the kidneys as they filter waste from the blood). Over the years, this may accelerate the decline of kidney health in susceptible individuals.
Once kidney disease is established, protein intake from all sources needs to be adjusted. Not complete elimination, but moderation and planning.
Avoiding protein powder blindly doesn’t protect the kidneys. Monitoring total protein intake does.
This is where individual medical advice matters.
Read More: Protein Powder in Coffee: How to Do It, Why It Works, and What to…
Signs Protein Powder Isn’t Working for You
The body usually gives quiet feedback before things go obviously wrong. With protein powder, the signals are often subtle and delayed, which is why they’re easy to dismiss.
A consistent rise in blood sugar 2-4 hours after a protein shake, especially when the initial reading looks normal, suggests that either the dose is too high, the protein is absorbing too quickly, or the timing doesn’t match your insulin sensitivity. This is one of the most common patterns people overlook because it doesn’t show up in short testing windows.
Persistent or unexpected hunger a few hours later is another clue. Some proteins stimulate insulin strongly. In insulin-resistant individuals, this can lead to a drop in cellular energy, triggering hunger even when glucose readings appear acceptable. This often leads to extra snacking that feels unrelated but is metabolically connected.
Digestive discomfort, such as bloating, heaviness, reflux, or irregular bowel movements, can signal poor tolerance to certain proteins, sweeteners, or fillers. These symptoms don’t always mean the protein is “bad,” but they often indicate that the formulation isn’t well-suited for regular use.
If weight increases over time without improvement in glucose control, protein powder may be adding calories without improving metabolic efficiency. This is common when shakes are used in addition to meals rather than replacing a specific nutritional gap.
Finally, if managing blood sugar feels more complicated after adding protein powder, more testing, more guessing, more adjustments, that’s feedback too. Protein powder should reduce variability, not introduce new uncertainty.
When these patterns appear, the solution isn’t always elimination. Often, small changes in portion size, timing, protein type, or pairing with food are enough. But ignoring the signals usually leads to frustration rather than benefit.
Read More: Why More Parents Are Switching to Organic Baby Formula: Is It the Healthier Choice?
When a Healthcare Conversation Is Necessary
If blood sugar patterns change after adding protein powder, don’t guess. If kidney function is compromised, don’t experiment. If medications affect appetite or digestion, protein intake needs alignment.
This is where a doctor or registered dietitian can help fine-tune protein type, timing, and portion size based on lab values, medications, and glucose patterns, not generic advice.
Protein powder is not a supplement you “try and see” forever. It’s something you adjust, measure, and sometimes remove.
Read More: Top PCOS-Friendly Protein Powders for Energy & Metabolism Support
Final Thoughts
Protein powder is not dangerous for people with diabetes. It is also not automatically harmless. It behaves quietly, slowly, and contextually, which makes it easy to misunderstand.
Used carefully, it can support stability. Used casually, it can complicate an already complex system.
The goal is not to avoid protein powder. The goal is to use it without working against blood sugar control. That requires attention, not fear.
- Protein powder doesn’t spike sugar loudly; it does it quietly. It means blood sugar may stay normal at first, then rise slowly a few hours later instead of jumping up right away.
- Most research doesn’t match how diabetics actually use protein powder
- The body reacts more to the speed of digestion and absorption than to protein “type”
- Food labels don’t reflect glucose behaviour
- There is limited long-term research on the long-term effects of daily protein powder use in diabetics.
FAQs
1. Does protein powder increase blood sugar in diabetics?
Sometimes yes, sometimes no, and often later than expected. The effect is usually delayed, not immediate.
2. Why does my sugar rise hours after a protein shake?
Because protein triggers insulin and slows digestion. In insulin resistance, this can lead to late glucose release.
3. Is whey protein bad for type 2 diabetes?
Not bad by default. It’s fast-acting and insulin-stimulating, which helps some people and destabilises others.
4. Does “diabetic-friendly” labelling mean it is safe?
No. Labels do not reflect delayed glucose effects.
5. Should diabetics stop using protein powder?
No. But it should be used deliberately, not casually, and not treated like a harmless drink.
References
- Beaudry, K. M., & Devries, M. C. (2019). Nutritional Strategies to Combat Type 2 Diabetes in Aging Adults: The Importance of Protein. Frontiers in Nutrition, 6.
- Kim, J. (2020). Pre-sleep casein protein ingestion: new paradigm in post-exercise recovery nutrition. Physical Activity and Nutrition, 24(2), 6–10.
- Ma, J., Stevens, J. E., Cukier, K., Maddox, A. F., Wishart, J. M., Jones, K. L., Clifton, P. M., Horowitz, M., & Rayner, C. K. (2009). Effects of a Protein Preload on Gastric Emptying, Glycemia, and Gut Hormones After a Carbohydrate Meal in Diet-Controlled Type 2 Diabetes. Diabetes Care, 32(9), 1600–1602.
In this Article